Asymptomatic Carotid Surgery Trial ACST2 Collaborators Meeting 2014

Asymptomatic Carotid Surgery Trial ACST-2 Collaborators Meeting 2014 Pembroke College, Oxford Is recent coronary stenting a problem (or an opportunity) for enrolling the patient in the trial? Valerio Tolva MD, Ph. D Istituto Auxologico Italiano IRCCS Deparment of Surgery Vascular Surgery (Head: Renato Casana MD) Milan, Italy

Handling a patient with recent coronary stenting and carotid stenosis is like a sailing race: • You can head straight forcing the upwind : with double therapy perform CAS • You can run on a beam wind and then upwind : stop double therapy and perform CEA Crews have guidelines for the right approach to a race… can we create guidelines using the data of the Trial?

“the prevalence of severe carotid disease (>80%% stenosis of ICA) among patients undergoing Percutaneous Coronary Intervention (PCI)/Open Heart Surgery (OHS) is estimated to be 6% to 12%. ” “…optimal treatment of patients with concurrent carotid and coronary artery disease remains unresolved despite >110 publications during the last 30 years reporting results in 9, 000 patients. ” Overview of the Nationwide Inpatient Sample (NIS) of the Healthcare Cost and Utilization Project (HCUP), from Timaran et al. J Vasc Surg 2009

• Coronary revascularization before non cardiac surgery is believed to decrease the peri- and post-operative risk in selected patients Fleisher LA et al. ACC/AHA 2007 Guidelines on perioperative cardiovascular evaluation. J Am Coll Cardiol 2007 • The frequency of major non cardiac surgery in the year after Drug Eluting Stent placement is >4 -5% Berger et al. Pre-Operative DES in EVENT Registry. J Am Coll Cardiol Intv. 2010 Van Kuijk et al. Timing of non cardiac surgery after coronary artery stenting. Am J Cardiol 2009
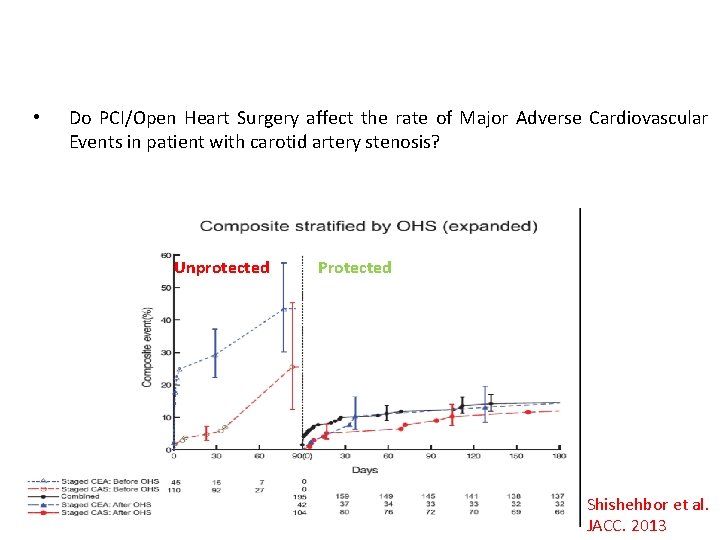
• Do PCI/Open Heart Surgery affect the rate of Major Adverse Cardiovascular Events in patient with carotid artery stenosis? Unprotected Protected Shishehbor et al. JACC. 2013
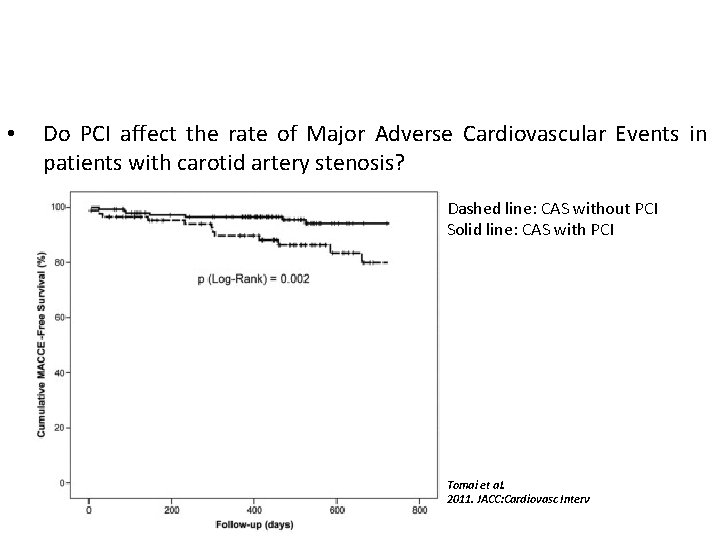
• Do PCI affect the rate of Major Adverse Cardiovascular Events in patients with carotid artery stenosis? Dashed line: CAS without PCI Solid line: CAS with PCI Tomai et al. 2011. JACC: Cardiovasc Interv
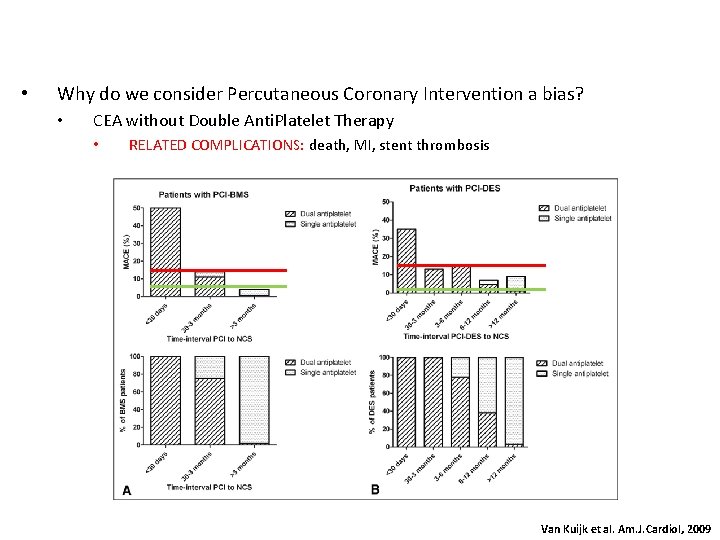
• Why do we consider Percutaneous Coronary Intervention a bias? • CEA without Double Anti. Platelet Therapy • RELATED COMPLICATIONS: death, MI, stent thrombosis Van Kuijk et al. Am. J. Cardiol, 2009

• Suspension of Double Anti. Platelet Therapy after Percutaneous Coronary Intervention (PCI) is associated with the risk of perioperative Major Adverse Cardiovascular Events due to stent thrombosis • Stent thrombosis is a multifactorial process • • • Surface coating: Drug Eluting Stents (DES), Bare Metal Stents (BMS) Stent diameter Stent length Vessel diameter Left ventricular ejection fraction Metabolic syndrome

• Stent-related decision making: • PCI with BMS: • PCI with DES: The European Society of Cardiology + ACC/AHA recommends DAPT for a minimum of 6 weeks after PCI The European Society of Cardiology + ACC/AHA recommends DAPT for a minimum of 1 year • • Always consider the time interval in patients with coronary and carotid lesions Avoiding DES in patients scheduled for carotid or aortic surgery can save 6 -9 months. The cardiovascular crew
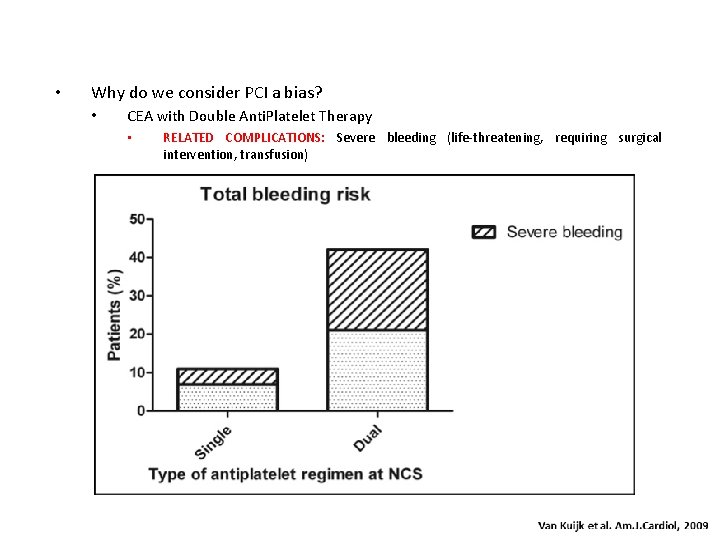
• Why do we consider PCI a bias? • CEA with Double Anti. Platelet Therapy • RELATED COMPLICATIONS: Severe bleeding (life-threatening, requiring surgical intervention, transfusion)
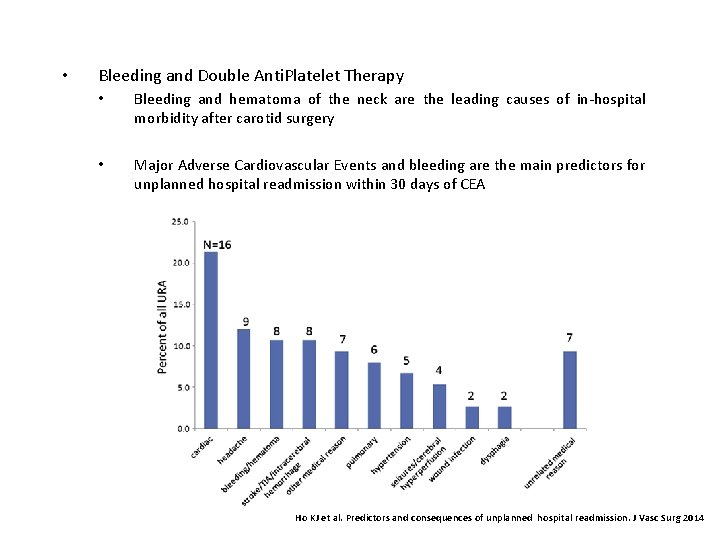
• Bleeding and Double Anti. Platelet Therapy • Bleeding and hematoma of the neck are the leading causes of in-hospital morbidity after carotid surgery • Major Adverse Cardiovascular Events and bleeding are the main predictors for unplanned hospital readmission within 30 days of CEA Ho KJ et al. Predictors and consequences of unplanned hospital readmission. J Vasc Surg 2014
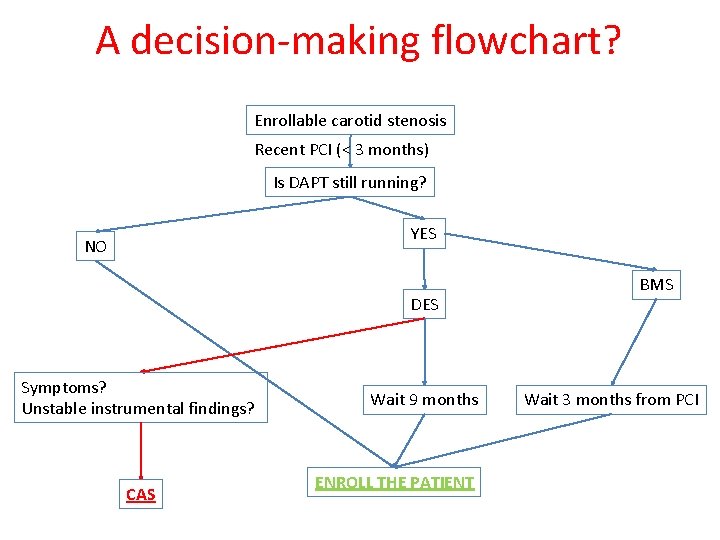
A decision-making flowchart? Enrollable carotid stenosis Recent PCI (< 3 months) Is DAPT still running? YES NO DES Symptoms? Unstable instrumental findings? CAS Wait 9 months ENROLL THE PATIENT BMS Wait 3 months from PCI

Key points • The cut off for enrolling the patient is 3 months. • In asymptomatic patients, cardiac timing is the leading priority regarding carotid stenosis • Carotid endarterectomy is the bias for enrollment if the patient is taking double therapy • As DES and BMS have different safety periods, a tailored stenting in patients with tandem lesions (coronary and carotid) must be considered. • Recruitment Centers with Cath. Lab can enroll 6 -12% of patients after PCI (30 -60 pts/year) Should we look at this subgroup or will the trial give the answers?

Before making a mistake… …Join the Trial and choose the best route
- Slides: 14