Asthma SCE Qs Bea Downie Q 1 You

Asthma SCE Qs Bea Downie

Q 1. You see a 28 yr old man in clinic for review of his chronic asthma. He has had 2 asthma attacks in the last year. PMHx: Asthma, Obesity, Fibromyalgia, Depression. He works as a secretary, lives alone and smokes 10/day. Spirometry reveals an obstructive picture with reversibility. In this patient, which of the following is not considered to be a marker of an increased risk of future asthma attacks? • A) Previous asthma attacks • B) Male gender • C) Reduced lung function • D) Obesity • E) Smoking • F) Depression

Q 1. You see a 28 yr old man in clinic for review of his chronic asthma. He has had 2 asthma attacks in the last year. PMHx: Asthma, Obesity, Fibromyalgia, Depression. He works as a secretary, lives alone and smokes 10/day. Spirometry reveals an obstructive picture with reversibility. In this patient, which of the following is not considered to be a marker of an increased risk of future asthma attacks? • A) Previous asthma attacks • B) Male gender • C) Reduced lung function • D) Obesity • E) Smoking • F) Depression
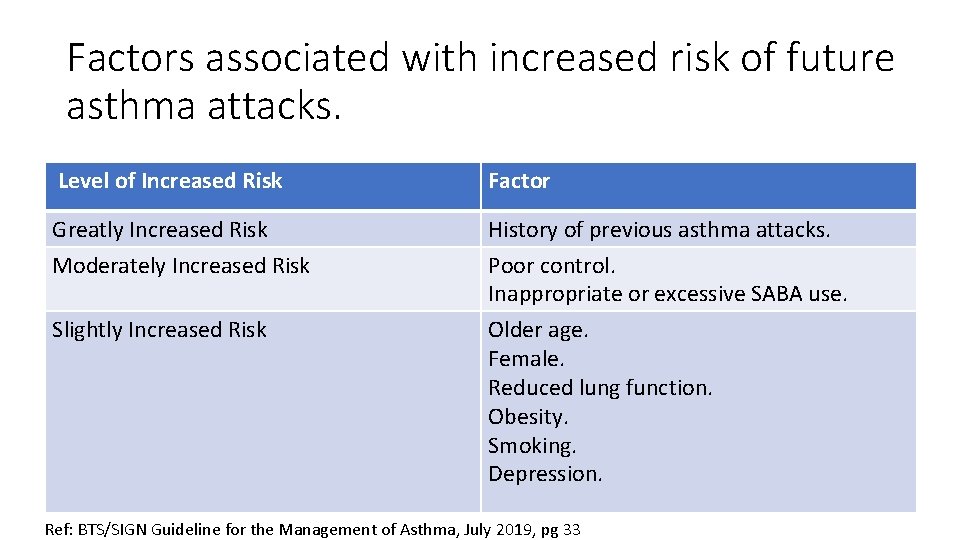
Factors associated with increased risk of future asthma attacks. Level of Increased Risk Factor Greatly Increased Risk Moderately Increased Risk History of previous asthma attacks. Poor control. Inappropriate or excessive SABA use. Slightly Increased Risk Older age. Female. Reduced lung function. Obesity. Smoking. Depression. Ref: BTS/SIGN Guideline for the Management of Asthma, July 2019, pg 33

Q 2 A 45 yr old asthmatic patient presents with 24 hrs of breathlessness, wheeze and chest tightness. RR 26, Sats 93%, HR 115, BP 89/45. You note she is in AF. Her PEF is 150 L/min. Her usual best PEF is 300 L/min. Which two of the following are indications to perform an Arterial Blood Gas? • A) Sats of 93% • B) Arrhythmia • C) PEF of 150 L/min. • D) Hypotension

Q 2 A 45 yr old asthmatic patient presents with 24 hrs of breathlessness, wheeze and chest tightness. RR 26, Sats 93%, HR 115, BP 89/45. You note she is in AF. Her PEF is 150 L/min. Her usual best PEF is 300 L/min. Which two of the following are indications to perform an Arterial Blood Gas? • A) Sats of 93% • B) Arrhythmia • C) PEF of 150 L/min. • D) Hypotension "Patients with Sp. O₂ <92% or other features of lifethreatening asthma require ABG measurement. " BTS/SIGN Guideline for the Management of Asthma, July 2019

Patients with Sp. O₂ <92% or other features of life-threatening asthma require ABG measurement.

Q 3 You see a 35 yr old pregnant woman in asthma clinic. She asks if there is any special advice for managing asthma in pregnancy/labour. Regarding asthma in pregnancy, which of the following is false. . ? • A) If anaesthesia is required, regional blockade is preferred to GA due to the risk of some inhaled anaesthetic agents causing bronchospasm. • C) Prostaglandin F 2α should be used with extreme caution in women with asthma because of the risk of inducing bronchoconstriction. • D) Continuous fetal monitoring is recommended for women presenting with acute severe asthma whilst pregnant. • E) Those taking > 5 mg/day of prednisolone for >2 weeks prior to delivery should receive hydrocortisone 100 mg IV 6– 8 hourly during labour.

Q 3 Regarding asthma in pregnancy, which of the following is false. . ? • A) If anaesthesia is required, regional blockade is preferred to GA due to the risk of some inhaled anaesthetic agents causing bronchospasm. • C) Prostaglandin F 2α should be used with extreme caution in women with asthma because of the risk of inducing bronchoconstriction. • D) Continuous fetal monitoring is recommended for pregnant women presenting with acute severe asthma. • E) Those taking > 5 mg/day of prednisolone for >2 weeks prior to delivery should receive hydrocortisone 100 mg IV 6– 8 hourly during labour. - FALSE (it is those receiving >7. 5 mg/day)
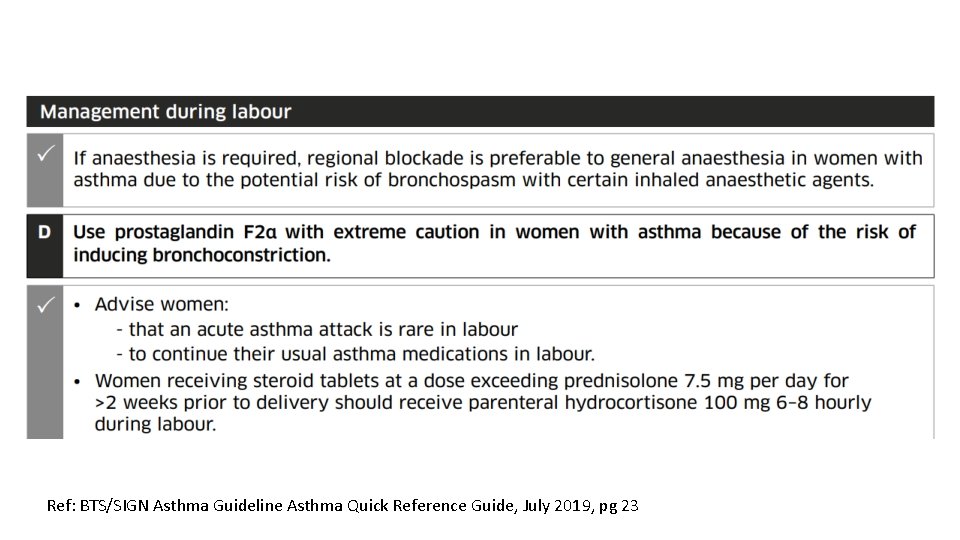
Ref: BTS/SIGN Asthma Guideline Asthma Quick Reference Guide, July 2019, pg 23

Q 4 Regarding diagnostic tests for asthma, which of the following is false. . . • A) In adults with obstructive spirometry, an improvement in FEV 1 of ≥ 12% in response to either β 2 agonists or corticosteroid treatment trials, together with an increase in volume of ≥ 200 ml, is regarded as a positive test. • B) Wheeze heard by a healthcare professional on auscultation increases the probability of asthma. • C) When doing 'best of 3' peak flows (PEF), further blows should be done if the largest two PEF are not within 40 L/min of each other. • D) PEF should be measured at least 2 x/day if occupational asthma is suspected.

Q 4 Regarding diagnostic tests for asthma, which of the following is false. . . • A) In adults with obstructive spirometry, an improvement in FEV 1 of ≥ 12% in response to either β 2 agonists or corticosteroid treatment trials, together with an increase in volume of ≥ 200 ml, is regarded as a positive test. • B) Wheeze heard by a healthcare professional on auscultation increases the probability of asthma. • C) When doing 'best of 3' peak flows (PEF), further blows should be done if the largest two PEF are not within 40 L/min of each other. • D) PEF should be measured at least 2 x/day if occupational asthma is suspected. - FALSE (should be 4 x/day)

Q 5 – Regarding 'direct challenge tests', which of the following is false? • A) A Provocation Concentration (PC) of 8 mg/ml or less is regarded as positive. • B) The provocative concentration (PC) or dose (PD) is the dose of bronchoconstrictor required to cause a 10% fall in FEV 1. • C) Two thirds, or more, of adults with a positive methacholine challenge have asthma. • D) The false negative rate is less than 10%.

Q 5 – Regarding 'direct challenge tests', which of the following is false? • A) A Provocation Concentration (PC) of 8 mg/ml or less is regarded as positive. • B) The provocative concentration (PC) or dose (PD) is the dose of bronchoconstrictor required to cause a 10% fall in FEV 1. - FALSE • C) Two thirds, or more, of adults with a positive methacholine challenge have asthma. • D) The false negative rate is less than 10%. Ref: BTS/SIGN Guidelines for the management of Asthma , July 2019, pg 14

Direct challenge tests • A measure of airway responsiveness. • Usually use methacholine or histamine. • The provocative concentration (PC 20) or dose (PD 20) of bronchoconstrictor required to cause a 20% fall in FEV 1.

Q 6 – Regarding Fractional exhaled nitric oxide (Fe. NO) levels, which of the following are false? • A) Fe. No levels are increased in men. • B) Fe. No levels are reduced in cigarette smokers. • C) Fe. No levels are reduced by inhaled or oral steroids. • D) Fe. No levels are increased in allergic rhinitis. • E) In steroid-naive adults, a Fe. NO level of 40 parts per billion (ppb) or more is regarded as positive. • F) A negative test excludes asthma

Q 6 – Regarding Fractional exhaled nitric oxide (Fe. NO) levels, which of the following are false? A) Fe. No levels are increased in men. B) Fe. No levels are reduced in cigarette smokers. C) Fe. No levels are reduced by inhaled or oral steroids. D) Fe. No levels are increased in allergic rhinitis. E) In steroid-naive adults, a Fe. NO level of 40 parts per billion (ppb) or more is regarded as positive. • F) A negative test excludes asthma - FALSE • • •

Fractional exhaled nitric oxide (Fe. NO) Testing • Can be used to find evidence of eosinophilic inflammation. • A positive test increases the probability of asthma. • A negative test does not exclude asthma. • In steroid-naive adults, a Fe. NO level of 40 parts per billion (ppb) or more is regarded as positive.

Ref: BTS/SIGN Guideline for the Management of Asthma, July 2019, pg 15

Q 7 – 38 yr old pregnant woman presents to A&E with 2 days of wheeze and increased SOB. Two hours after treatment with nebulisers and steroids her RR is 18, Sats 95% on air, HR 84, BP 120/70. PEFR is 320 L/min but she states that she does not feel better. Her 'best' recorded PEF is 400 L/min. Which of the following is not a reason to consider hospital admission? A) A history of poor compliance with treatment. B) Presentation at night. C) Asthma attack despite adequate dose of oral corticosteroid prior to presentation. D) She still has significant symptoms E) Her PEFR post-treatment. F) Pregnancy.

Q 7 – 38 yr old pregnant woman presents to A&E with 2 days of wheeze and increased SOB. Two hours after treatment with nebulisers and steroids her RR is 18, Sats 95% on air, HR 84, BP 120/70. PEFR is 320 but she states that she does not feel better. Her 'best' recorded PEF is 400. Which of the following is not a reason to consider hospital admission? A) A history of poor compliance with treatment. B) Presentation at night. C) Asthma attack despite adequate dose of oral corticosteroid prior to presentation. D) She still has significant symptoms E) Her PEFR post-treatment. (which is 80% of 'best') F) Pregnancy.

Criteria for admission

Q 8 – Regarding treatment of asthma with Omalizumab, which of the following is false? • A) Omalizumab can be used to treat severe persistent confirmed allergic Ig. E‑mediated asthma. • B) It is used in those with continuous or frequent oral corticosteroid use, defined as >2 courses in the previous year. • C) Patients must have stopped smoking. • D) The dosage is determined by the concentration of serum Ig. E before the start of treatment and body weight. • E) Response should be evaluated at 16 wks, and treatment should be stopped if there is no improvement.

Q 8 – Regarding treatment of asthma with Omalizumab, which of the following is incorrect? • A) Omalizumab can be used to treat severe persistent confirmed allergic Ig. E‑mediated asthma. • B) It is used in those with continuous or frequent oral corticosteroid use, defined as >2 courses in the previous year. - Incorrect. • C) Patients must have stopped smoking. • D)The dosage is determined by the concentration of serum Ig. E before the start of treatment and body weight. • E) Response should be evaluated at 16 wks, and treatment should be stopped if there is no improvement.

NICE Guidance on Omalizumab 1. 1 Omalizumab is recommended as an option for treating severe persistent confirmed allergic Ig. E‑mediated asthma as an add‑on to optimised standard therapy: • who need continuous or frequent treatment with oral corticosteroids (defined as 4 or more courses in the previous year) • 1. 2 Optimised standard therapy is defined as a full trial of and, if tolerated, documented compliance with: Ø inhaled high‑dose corticosteroids Ø long‑acting beta 2 agonists Ø leukotriene receptor antagonists Ø theophyllines Ø oral corticosteroids Ø smoking cessation if clinically appropriate Ref: Omalizumab for treating severe persistent allergic asthma. NICE Technology appraisal guidance [TA 278] April 2013
- Slides: 25