Association between presence of advanced airway and hyperventilation

Association between presence of advanced airway and hyperventilation during pediatric CPR: a report from the VIPER Collaborative Karen O’Connell, MD, MEd; Children’s National Hospital, Washington, DC Sage Myers, MD MSCE; Children’s Hospital of Philadelphia, PA Benjamin Kerrey, MD; CCHMC, Cincinnati, OH Alexis Sandler, BS; Children’s National Hospital, Washington, DC Ryan Keane, MD; Duke University School of Medicine, Durham, NC Benjamin Parrish, BS; Children’s National Hospital, Washington, DC Ichiro Watanabe, MD; Children’s Hospital of Philadelphia, PA Aaron Donoghue, MD, MSCE; Children’s Hospital of Philadelphia, PA Abstract: 204

FINANCIAL DISCLOSURE All authors report no financial disclosures or conflicts of interest Presenter: Karen O’Connell, MD, MEd Co-authors: • Sage Myers, MD, MSCE • Benjamin Kerrey, MD • Alexis Sandler, BS • Ryan Keane, MD • Benjamin Parrish, BS • Ichiro Watanabe, MD • Aaron Donoghue, MD, MSCE

BACKGROUND & OBJECTIVE Background: • Hyperventilation is common during pediatric CPR and has known deleterious hemodynamic consequences. • Our research collaborative has previously reported that hyperventilation is more prevalent in the presence of an advanced airway (AA) compared to CPR with a natural airway (NA). • It is not known whether the presence of an AA is independently associated with hyperventilation when controlling for within-patient variability. Objective: • To determine the independent association between the presence of an AA and hyperventilation during pediatric CPR in a collaborative of PEDs using video review during resuscitations.

METHODS • We present a report from the Videography in Pediatric Emergency Resuscitation (VIPER) Collaborative, a prospective observational database from three tertiary PEDs. • Study design: Retrospective, multicenter, video-based cohort study Example of 4 -Frame View Utilized for Video Review (CNH: On. SSI Ocularis IS 3. 5; CHOP, CCHMC, CHC: Live. Capture, B Line Medical)

METHODS Inclusion Criteria: • Birth to 18 years of age • Events where CPR was performed and ventilations could be counted for at least 30 sec • Video available from July 2016 to June 2019

METHODS Data collection: • • All study sites are established within the VIPER infrastructure All sites video record and review resuscitations for quality, safety and IRB approved research; validity, feasibility and inter-rater reliability have been established in previous studies. CPR and ventilation event data was collected using video review. Ventilation rates were counted and expressed in segments corresponding to individual providers performing CPR (‘compressor segments’) and extrapolated to breaths per minute (bpm) where applicable. – Segments during which tracheal intubation was being performed were excluded from analysis • Hyperventilation was defined as a ventilation rate greater than 12 bpm, in accordance with American Heart Association 2015 recommendations.

METHODS Data Analysis: • Ventilation rates were compared between CPR segments with a natural airway (bag-valve mask device; NA) versus an advanced airway (endotracheal tube, supraglottic airway, or tracheostomy; AA). • Univariate analysis was done by two sided t-testing. • Repeated measures logistic regression with random effects modeling (patient as intercept) was performed to determine the independent association of the presence of an AA with hyperventilation.
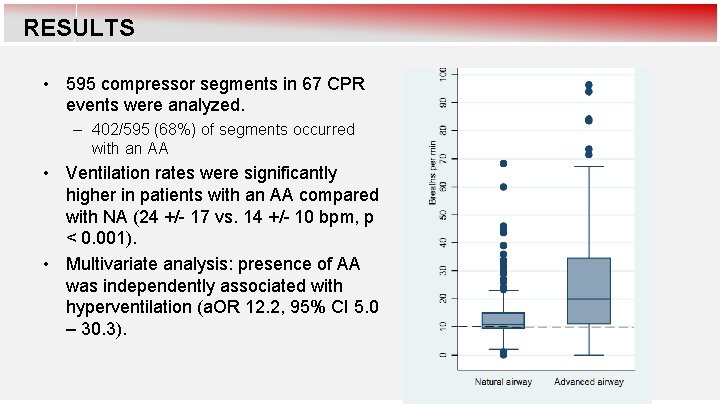
RESULTS • 595 compressor segments in 67 CPR events were analyzed. – 402/595 (68%) of segments occurred with an AA • Ventilation rates were significantly higher in patients with an AA compared with NA (24 +/- 17 vs. 14 +/- 10 bpm, p < 0. 001). • Multivariate analysis: presence of AA was independently associated with hyperventilation (a. OR 12. 2, 95% CI 5. 0 – 30. 3).

CONCLUSION • The presence of an advanced airway is associated with higher ventilation rates during pediatric CPR. • In light of 2020 PBLS recommendations for intubated patients, more data is needed to examine the 15: 2 C: V ratio, as well as optimal means of AA placement during pediatric CPR. • Future studies should examine methods of limiting manual hyperventilation during pediatric CPR, as well as impact of ventilation rates during CPR on patient outcomes. Questions: Karen O’Connell, MD, MEd Children’s National Hospital koconnel@childrensnational. org
- Slides: 9