Assistive Devices or Mobility Assistive Equipment for Gait

“Assistive Devices” or “Mobility Assistive Equipment for Gait Disorders in the Elderly” Steve Swedlund, MD Assistant Professor, Dept of Geriatrics April 4, 2011

Objectives (1 of 2) The learner shall: – Identify different types of canes, walkers, wheelchairs, and a power scooter. – Outline a plan for matching a cane, walker, or wheelchair to a patient’s needs. – Describe how to assess the fit of a cane, walker, or wheelchair for a patient. – List components of a prescription for ‘Mobility Assistive Equipment (MAE). ’

Objectives (2 of 2) • The learner shall: – Describe the process of the ‘Certificate of Medical Necessity (CMN), ’ relative to the prescription of MAE. – Identify the CMS website as a resource for webbased learning regarding completion of the CMN. – List common mistakes in prescribing MAE.

Pre-Quiz The following 5 slides are to challenge your knowledge about mobility assistive equipment. Let’s take a Quiz!

Can you name it?

Can you name it?
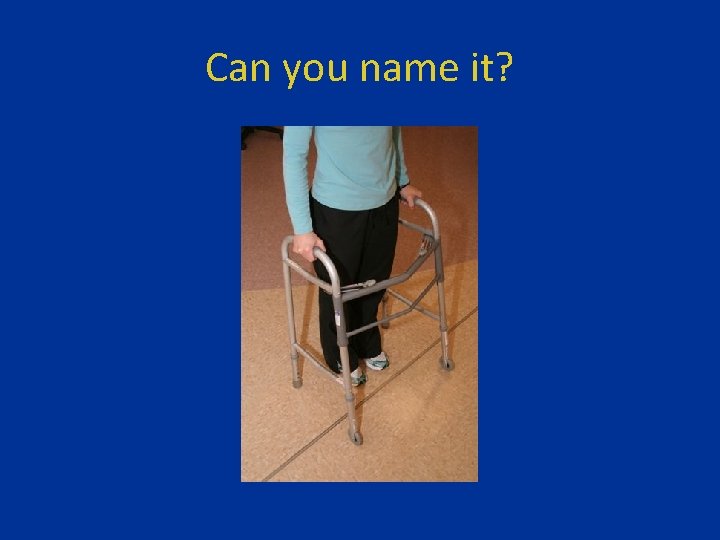
Can you name it?

True or False • When using a cane properly, the patient should use the cane in the hand on the same side as the deficient leg.

True or False • When advancing up stairs with a cane, the patient should advance the deficient leg first for each step, in tandem with the cane.

Pre-Quiz answers 1. Powered Scooter 2. Powered, or motorized wheelchair 3. Forward wheeled walker 4. False. Use the cane on the opposite side from deficient leg. • 5. False. Advance upward with the functional leg, each step. Descend with the deficient leg first with each step. • •

Mobility Assistive Equipment (MAE) • The Center for Medicare and Medicaid Services (CMS) has defined MAE (in 2005) as: – Canes – Crutches (de-emphasized in elderly) – Walkers – Manual Wheelchairs – Power Scooters

Activities of Daily Living (ADLs) • ADLs are commonly defined as the patient’s ability to do: – Ambulation, including transferring – Toileting, including continence – Bathing – Dressing – Feeding (definitions of ADLs can vary, by author)

Mobility Related Activities of Daily Living (MRADLs) • Mobility Related ADLs (MRADLs) are: • those activities of daily living that require mobility, and occur within the residence of the patient. • The Medicare program does not cover mobility assistive equipment that is only needed for activities outside of the patient’s residence (also known as ‘Community Related ADLs. ’)

Instrumental Activities of Daily Living (IADLs) • IADLs are commonly defined as the patient’s ability to: – – – – Use the telephone. Go shopping. Prepare food for meals. Do housekeeping chores. Do laundry. Be responsible for taking own medications. Manage finances. Drive a car, or manage transportation.

Centers for Medicare and Medicaid Services (CMS) • The CMS is: – a federal agency, – within the Department of Health and Human Services, – which manages the Medicare and Medicaid programs, and is – responsible for distribution of covered services. • Medicare is a federal program, funded by income taxation. • Medicaid is a joint federal and state program.

Prescription for MAE—”Know your patient” (1 of 4) • Meet the patient, get history, examine, diagnose, assess, and plan goals. – You must know: mobility needs of patient, home environment, ADLs, IADLs, Past Medical History, Family Medical History, Social History, Surgical History, level of cognition, upper limb function, lower limb function, functional mobility, community mobility, diagnoses, medications, short and long-term goals.

Prescription for MAE (2 of 4) • CMS requires this documentation about your evaluation process to be in the medical record. • ‘Medical record’ can include hospital, nursing home, home visit, or consultation visits recorded by you or others. • Generally, it is standard to include family or caregiver(s), in evaluation and goal setting process.

Prescription for MAE (3 of 4) • A typical prescription includes: – Medical condition related to the need for MAE, – Prognosis, – Functional limitations, in regards to ADLs, – Previously prescribed interventions and why failed, – Justification for the MAE, particularly related to ADLs, – Signature, credentials and date.

Prescription for MAE (4 of 4) • This prescription will be routed to the durable medical equipment (DME) supplier, and if a ‘certificate of medical necessity’ (CMN) is required by CMS, then the supplier will forward a CMN to the prescriber, with sections A (demographic data) and C (equipment description, Medicare allowed rate, and cost quoted from supplier) completed. • The prescriber will then need to complete CMN sections B (documentation of medical necessity) and D (attestation, signature, credentials, and date).

Certificate of Medical Necessity (CMN) (1 of 2) • A CMN is a form developed by CMS, which is utilized to determine medical necessity of the patient, for distribution of MAE, or other durable medical equipment (DME), prostheses, orthotics, oxygen, or supplies. • A CMN is not required of all DME and supplies, and CMS defines which DME and supplies require CMNs.

Certificate of Medical Necessity (CMN) (2 of 2) • CMS has developed a web-based training course for prescribers of CMNs, which is available at: www. cms. gov--select ‘Outreach and Education, ’ then find ‘Medicare Learning Network’ (MLN), then select ‘MLN products, ’ and ‘Web-based Training Modules, ’ then select ‘Certificate of Medical Necessity. ’ This activity requires about an hour of time, and is accredited for continuing education, until 2012.

Certificate of Medical Necessity— common mistakes • Common prescriber mistakes are: – not performing a face-to-face evaluation of patient, – not demonstrating medical necessity, – not listing failed prescriptions for less technical MAE, such as canes, walkers, manual wheelchairs, – not limiting the MAE prescription to ADLs within the home (ie. writing a prescription for community related ADLs).
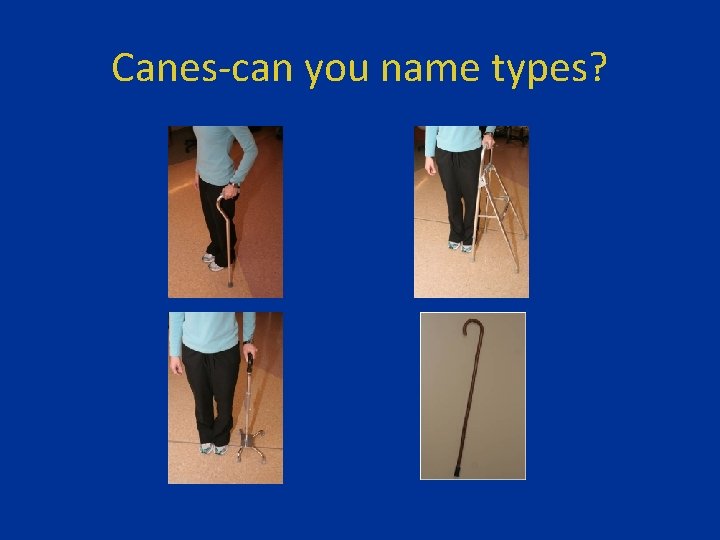
Canes-can you name types?
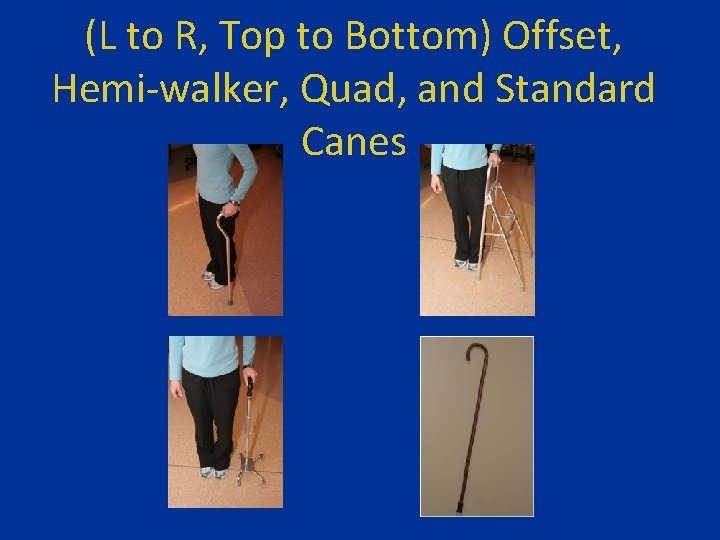
(L to R, Top to Bottom) Offset, Hemi-walker, Quad, and Standard Canes

Canes--discussion • Canes widen a person’s base of support, and thus balance. • Modified designs of canes permit degrees of weight bearing. • Usually used when only one upper extremity is needed for balance, and/or to off-load a painful lower extremity joint.

Canes—How to fit?

Cane—How to fit? • Top of the cane should be at the flexural crease of the wrist, or at the greater trochanter, with a 15 to 30 degree of flexion at the elbow.

Canes-how to use? • The patient uses the cane in the hand opposite of the leg with the most severe deficit; the cane is then advanced with the opposite (deficient) leg. • Climbing or descending the stairs: “up with the good, and down with the bad”

Cane-standard type

Canes--Standard • Wooden—inexpensive, but must be custom fitted. • Aluminum—more expensive, but usually adjustable. • Indicated for patients who need one more contact point for balance, and need little or no upper extremity weight bearing (such as poor sense of balance, or mild arthralgia in lower extremity).
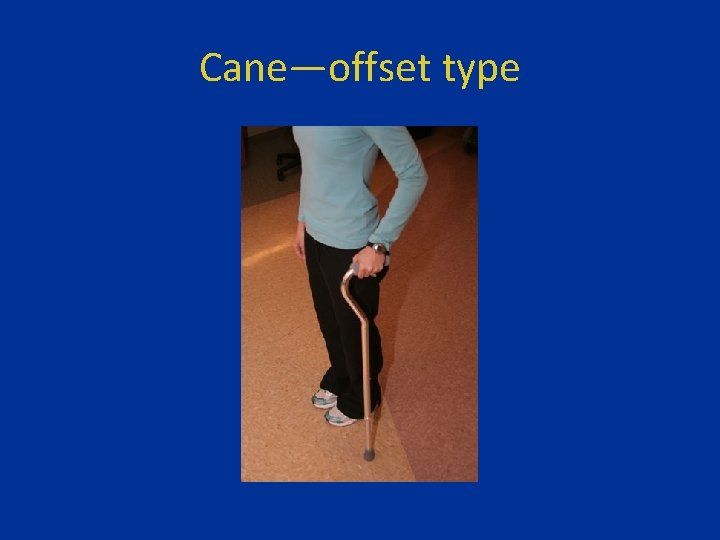
Cane—offset type

Canes—offset type • Allow weight to be placed over the shaft of the cane; usually aluminum and adjustable. • Indicated for patients with mildly to moderately painful gait, due to hip or knee arthralgia.
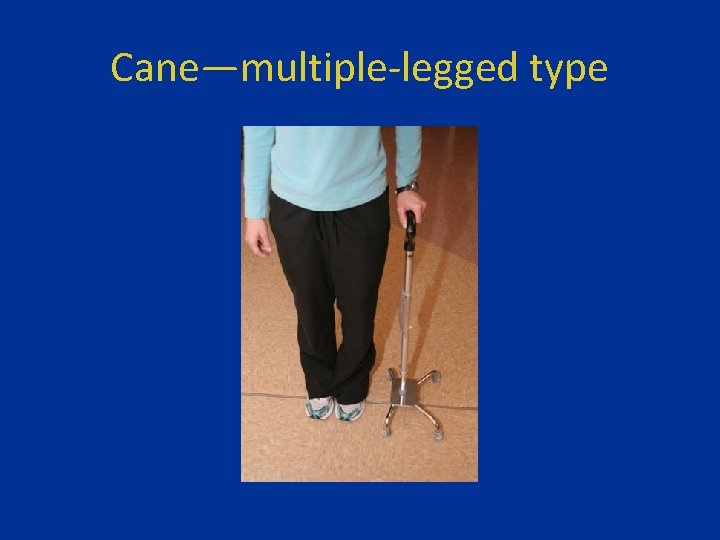
Cane—multiple-legged type

Canes—multiple-legged • Also known as a 4 pronged cane, or ‘quad cane. ’ • Provides increased base of support and can permit greater weight bearing. • Indicated for patient with moderately to severely painful gait from arthralgia of hip or knee, or perhaps for a patient with a ‘frontal gait pattern. ’

Canes—multiple-legged • Advantage—can stand upright on floor, when not in use, while patient uses hands. • Disadvantage—all legs need to be in simultaneous contact with the ground; many patients find this awkward (can cause patient to walk slower).

Canes—Walk Cane

Canes—Walk Cane • Also known as “hemi-walker. ” • Is usually broad-based, aluminum, with a handle and two legs, and another component of two legs that are angled away from the patient.

Walk Cane-pros and cons • Provides more support than standard, offset, or multiple-legged canes. • Because of size and 4 contact points, speed of gait is sacrificed for support.

Walk Cane-Indication • Can be used for patients needing continuous weight bearing with only one arm, such as a stroke patient with hemiparesis and moderate to severe loss of lower extremity function.
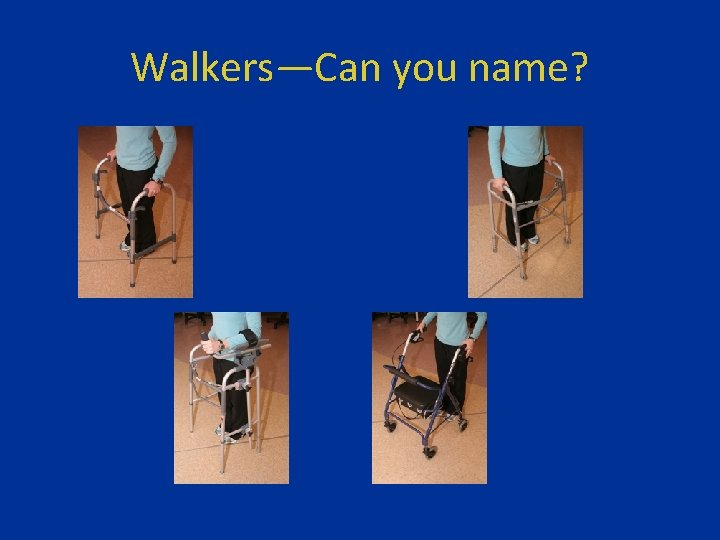
Walkers—Can you name?

(L to R) Standard, Platform, 4 - Wheeled, and Forward Wheeled Walkers

Walkers--advantages • Improve balance – by increasing the patient’s base of support, – by enhancing lateral stability, – and by supporting the patient’s weight.

Walkers--disadvantages • Requires more space to maneuver. • Reduced arm swing. • Changed posture, with abnormal flexion of the back while walking. • In general, not used on stairs.

Walkers—How to fit • The handgrips of the walker should be at the flexural crease of the wrist, or at the greater trochanter, with a 15 to 30 degree of flexion at the elbow.

Standard Walker

Standard Walkers • 4 legs with rubber tips that come in contact with the floor simultaneously. • Most stable of walker types. • But needs slower, controlled gait pattern. • Requires more ‘attention demand’ (a higher level of awareness) than canes.

Standard Walkers-indications • Are useful for patients with moderate to severe cerebellar ataxia, hip and knee replacement rehabilitation. • But the need for attention (attention demand) makes them less desirable for cognitively impaired patients.

Walkers—forward-wheeled

Walkers—forward-wheeled pros and cons • Permits more normal gait pattern than the standard walker. • Requires less lifting than the standard type. • Less stable than the standard walker. • Less suitable for the more cognitively impaired, as the patient requires more ‘attention demand. ’

Walkers—forward-wheeled indications • For example, can be used in patients with frontal lobe-related gait disorders, moderateto-severe Parkinson’s disease, or moderate ataxia.

Walkers—four-wheeled

Four-wheeled walker • Is indicated for the patient that needs a large base of support, but does not need to use it for much weight bearing. • Best for higher cognitively functioning patients who walk longer distances and need minimal weight bearing.

Four-wheeled walker • For example, can be used for patients with mild to moderate Parkinson’s disease, mild “cautious” gait, or mild ataxia.
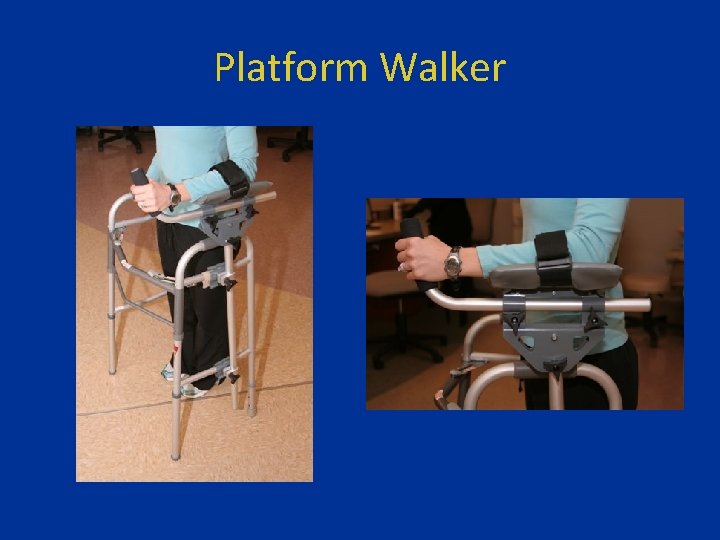
Platform Walker

Platform walker • Platform walker is fitted to redistribute the weight—to offload the stress on the wrist and forearm--for example, in cases of arthritis, or injury of the upper extremity.

Wheelchairs—Can you name?

(L to R) Standard, Hemi, Motorized, and Hemi Wheelchairs

Wheelchair-Standard

Wheelchair-Hemi type

Wheelchair—motorized type

Wheelchair—general assessment for fit • Discuss 90 -90 -90 rule—when patient sitting properly in the WC, the elbows, hips, and knees should be flexed to 90 degrees (exception 60 -90 degrees for knees, if to ambulate in WC); soles should be flat on floor. • Seat depth: the knees should not be advanced more than 2 to 3 inches beyond the front edge of the seat, or a seat extension may be needed.

Wheelchair fit— 90/90/90 rule

Wheelchair—general fit • Seat width is about one inch more than the distance between the lateral aspects of the greater trochanters, when patient is seated. • Seat back height is about 1 inch below the inferior angle of the scapula.

Wheelchair—general fit

Motorized Scooter

Motorized Scooter • Takes more room to maneuver than a motorized wheelchair. • May demand two hands to control. • The seating is less supportive, and less adaptable for patients, as compared to the motorized wheelchair. • Less expensive than motorized wheelchair. • Easier to transport.

Medicare Guidelines for MAE (overview) • A face-to-face exam must be performed by treating physician in order to initiate and determine medical necessity. • Canes, crutches, walkers, manual wheelchairs, power wheelchairs and scooters are all now termed ‘MAE. ’

Medicare Guidelines for MAE (overview) • Basis for prescription must be logical; documentation of why less expensive and less technical equipment is not appropriate must be included. • MAE can only be ordered to enhance Mobility Related ADLs in the home, and cannot be prescribed for community needs. (Mobility outside of home is not considered a medical necessity. )

Summary • You can now: – identify types of Mobility Assistive Equipment. – select patients who may benefit from MAE. – assess general fit for MAE. – recite components of a prescription for MAE, which are derived from a face-to-face evaluation. – describe the general process of completing a Certificate of Medical Necessity, and find a webbased training module to learn more about CMNs.

Post-Quiz Let’s evaluate the application of your new knowledge!

Can you name it?

Quad Cane

True or False • When using a cane properly, the patient should use the cane in the hand on the same side as the deficient leg.

True or False • When using a cane properly, the patient should use the cane in the hand on the same side as the deficient leg. • False. Patient should use the cane in the hand opposite the impaired side.

True or False • When advancing up stairs with a cane, the patient should advance the deficient leg first for each step, in tandem with the cane.

True or False • When advancing up stairs with a cane, the patient should advance the deficient leg first for each step, in tandem with the cane. • False. The patient should advance up stairs with the leg which is not impaired.

Can you name it?
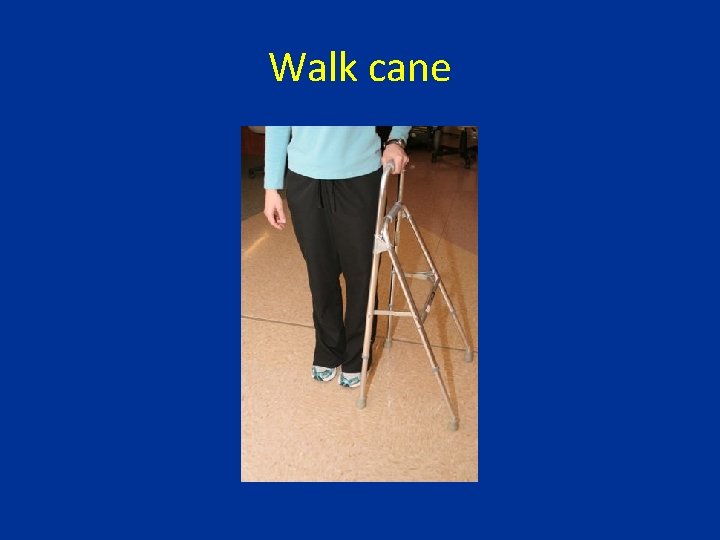
Walk cane
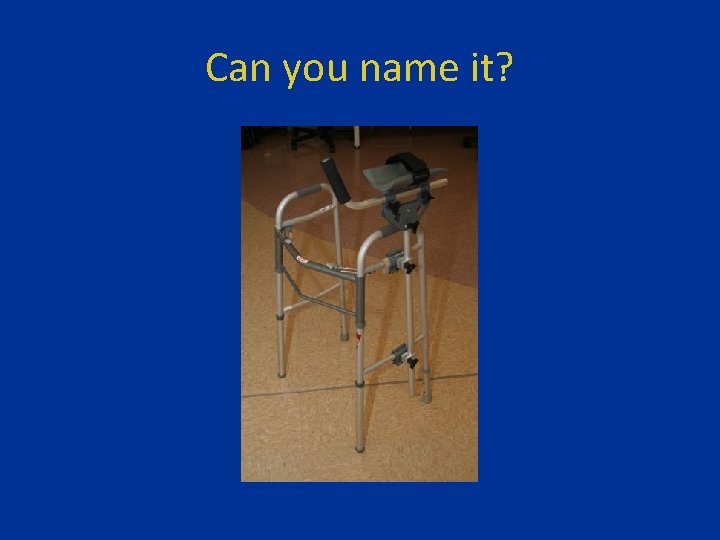
Can you name it?

Standard walker, with platform attachment, or ‘platform walker’

Can you name it?

Four wheeled walker, also known as a rollator
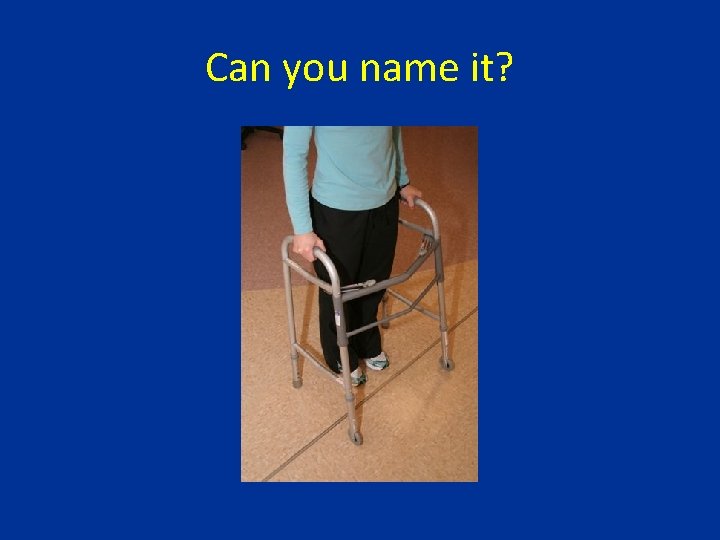
Can you name it?

Forward wheeled walker

Can you name it?

Motorized wheel chair

True or False • The national rate for prescribing motorized wheelchairs increased 33 times between 1994 and 2001.

True or False • The national rate for prescribing motorized wheelchairs increased 33 times between 1994 and 2001. • True, based on investigation of the Office of the Investigator General. Surveys of the beneficiaries revealed that many prescriptions were inappropriate, such as no face-to-face evaluation by prescriber, --or the prescription was for Community Related ADLs, and not for ADLs within the residence.
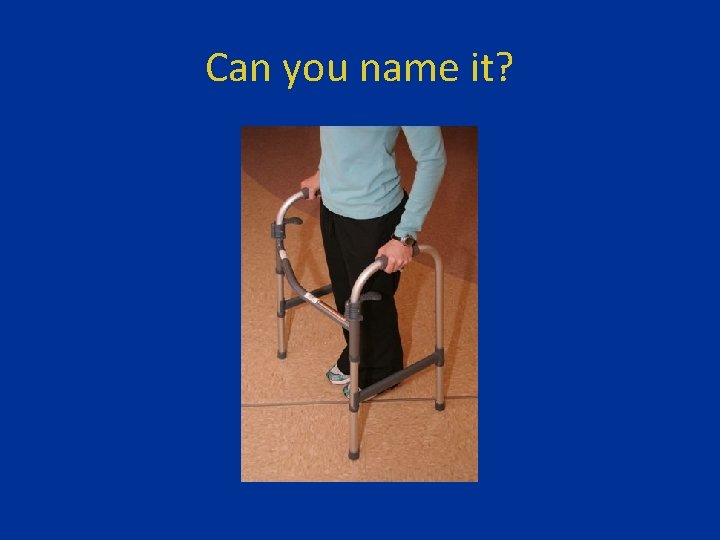
Can you name it?

Standard Walker

Can you name it?

Hemi-wheel chair, with seat extension

Can you name it?

Standard Cane

Can you name it?

Motorized scooter

True or False • Prescribing a motorized scooter for community function is within CMS guidelines.

True or False • Prescribing a motorized scooter for community function is within CMS guidelines. False. Mobility-related ADLs in the community are not qualifications for prescribing motorized scooters or wheelchairs.

Can you name it?

Anti-tippers

Bibliography • Ambulatory Devices for Chronic Gait Disorders in the Elderly, Van Hook, FW, et. al, Am Fam Physician 2003; 67: 1717 -24. • Canes, Crutches and Walkers, Joyce BM, Kirby RL, Am Fam Physician 1991; 43: 535 -42.

Bibliography • “Special Communication--Power Mobility Device Provision: Understanding Medicare Guidelines and Advocating for the Clients, ” Dicianno, BE, et. al, Arch Phys Rehabil 2007; 88: 807 -816. • “Seating Evaluation and Wheelchair Prescription, ” Wilson, PE, et. al, as accessed on e. Medicine website on 4. 2. 2011.

Bibliography • “Wheelchair Evaluation for the Older Adult, ” Sabol, TP, et. al, Clin Geriatr Med 22(2006)355375. • “Epidemiology of Medicare Abuse: The Example of Power Wheelchairs, ” Goodwin, JS, et. al, J Am Geriatr Soc 55: 221 -226, 2007.

Bibliography • “Seating and Mobility Considerations for People With Spinal Cord Injury, ” Minkel, JL, Phys Ther 2000; 80: 701 -709. • “Assistive Devices for Gait in Parkinson’s Disease, ” Constantinescu, R, et. al, Parkinsonism and Related Disorders 13(2007)133 -138.

Bibliography • ‘Certificate of Medical Necessity, ’ web-based training module, in the Medicare Learning Network, linked within the CMS website, www. cms. gov, as accessed on 4/2/2011. • The Wheelchair Evaluation: A Clinician’s Guide. Mitchell Batavia, Ph. D, PT. Second Edition. Jones and Bartlett, Publishers. 2010. —this reference includes a CD with short videos of wheelchairs and accessories.

Bibliography • ‘Power Mobility Device Evaluation, ’ as accessed at www. tafp. org, on 4/2/2011. The Texas Academy of Family Physicians has developed and made available an evaluation form for use in evaluating a patient with impaired mobility.
- Slides: 106