Assessment Detection and Management of Malnutrition in Children




![Magnitude of malnutrition Globally, 9% of pre-school children are wasted[1] In developing countries, however, Magnitude of malnutrition Globally, 9% of pre-school children are wasted[1] In developing countries, however,](https://slidetodoc.com/presentation_image_h/7922524b981bd096f74462973fc918f8/image-5.jpg)
![Malnutrition contributes to 54% of under-5 mortality[3] A malnourished child suffers from multitude Malnutrition contributes to 54% of under-5 mortality[3] A malnourished child suffers from multitude](https://slidetodoc.com/presentation_image_h/7922524b981bd096f74462973fc918f8/image-6.jpg)

























- Slides: 34

Assessment, Detection and Management of Malnutrition in Children BY Sampson Antwi (Dr) FWACP, FGCP Senior Lecturer: SMS-KNUST/KATH

Outline Learning Expectations Magnitude of malnutrition Methods of nutritional assessment Management of acute complications Feeding, discharge & follow-up Recipe for Re. So. Mal, F-75 & F-100

Learning Expectations By the end of presentation, participants should • • • appreciate the magnitude of malnutrition and its contribution to childhood morbidity and mortality be familiar with the various methods of assessing the nutritional status of a child. be able to recognise a child with malnutrition be able to identify and manage common complications associated with the acute presentation of a child with malnutrition be familiar with appropriate diet formulation for a child with malnutrition

Preamble Malnutrition could be nutritional excess or nutritional deficiency In this presentation, malnutrition only refers to nutritional deficiencies.
![Magnitude of malnutrition Globally 9 of preschool children are wasted1 In developing countries however Magnitude of malnutrition Globally, 9% of pre-school children are wasted[1] In developing countries, however,](https://slidetodoc.com/presentation_image_h/7922524b981bd096f74462973fc918f8/image-5.jpg)
Magnitude of malnutrition Globally, 9% of pre-school children are wasted[1] In developing countries, however, under-5 malnutrition prevalence is estimated at 27%[2] Worrying is the fact that as the global trend is decreasing, trend in Africa is increasing. (WHO Dept of nutrition 2010)
![Malnutrition contributes to 54 of under5 mortality3 A malnourished child suffers from multitude Malnutrition contributes to 54% of under-5 mortality[3] A malnourished child suffers from multitude](https://slidetodoc.com/presentation_image_h/7922524b981bd096f74462973fc918f8/image-6.jpg)
Malnutrition contributes to 54% of under-5 mortality[3] A malnourished child suffers from multitude of problems including mental deficiency S/he also has close to 50% chance of dying if not correctly identified and properly treated[4] It is important therefore that children are properly assessed for evidence of malnutrition

Significance in clinical practice Children constitute >50% of most outpatients clinical consultations in most hospitals in Africa These children are seen mostly by General and Family Practitioners and even Specialist non-Paediatricians (locum Drs) Paediatric practice should therefore be of interest to most Medical Practitioners in Africa

Under-diagnosis of malnutrition • • • Despite its high prevalence in developing countries, malnutrition is often underdiagnosed Antwi S found only 5. 9% of wasted children to be so identified by the attending Physicians in a tertiary hospital in Ghana. [5] It is important therefore that all Practitioners attending to children properly assess for malnutrition and familiarise themselves with its treatment.

Methods of Nutritional assessment in children Four (4) basic methods: § § Nutritional and other relevant history Clinical examination Anthropometric measurements Laboratory tests

1. History • • Dietary history may reveal deficiency in the quantity and quality of food intake. A child at risk of malnutrition may have a history of one or more of the following: – Premature birth or LBW – Lack of breastfeeding in poor social circumstance – Twin birth – Prolonged or recurrent diarrhoea, TB or other infectious dx – Affectation or infection by HIV – Cancer or chronic dx

History cont. ◦ Lost a parent by death or desertation ◦ Large family size with poor social circumstances ◦ Lives in a home without pipe-borne water or other source of clean water

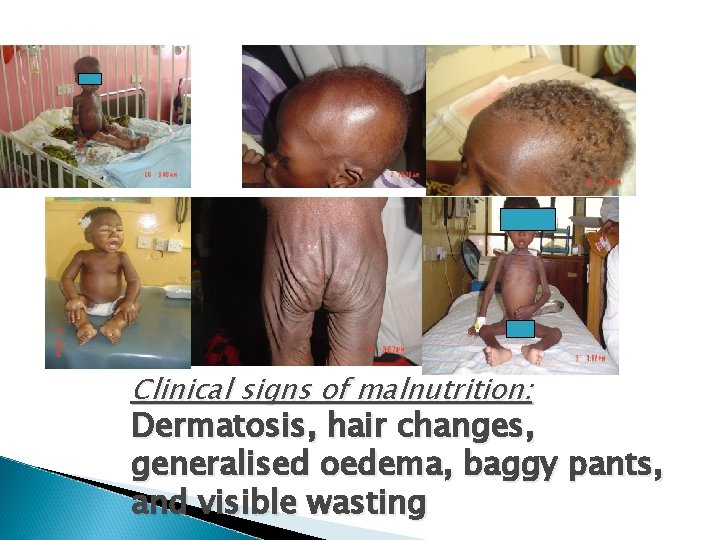
2. Clinical signs of malnutrition • Hair changes: • • • silkiness, curliness or straightness, lightly coloured to shades of brown/red sparsely distributed thin and easily pluckable

• Dermatosis: commoner in oedematous type. Manifest as: • • • hypo-/hyper-pigmentation, rough patches, shedding in scales, cracks and fissures. Extensive desquamation that may resemble burns.

Visible signs of wasting: most visible in ◦ ◦ chest as prominent ribs, arms and thighs as loose skin and flabby muscle, back as prominent scapula and spine, buttocks as loss of fat and muscles with overlying skin hanging loose in a typical “baggy pants” fashion.

Peripheral oedema: § Suspect malnutrition in any child with bi-pedal oedema, particularly in presence of other physical signs of malnutrition § May mimic nephrotic syndrome and may sometimes be difficult to differentiate especially in presence of abnormal urinalysis from UTI Note: presence of significant ascites discriminates against oedematous malnutrition

Other signs of malnutrition: § § § Pallor moon face with drooping cheeks angular stomatitis and glossitis with loss of papilla distended abdomen irritability and apathy

Clinical signs of malnutrition: Dermatosis, hair changes, generalised oedema, baggy pants, and visible wasting

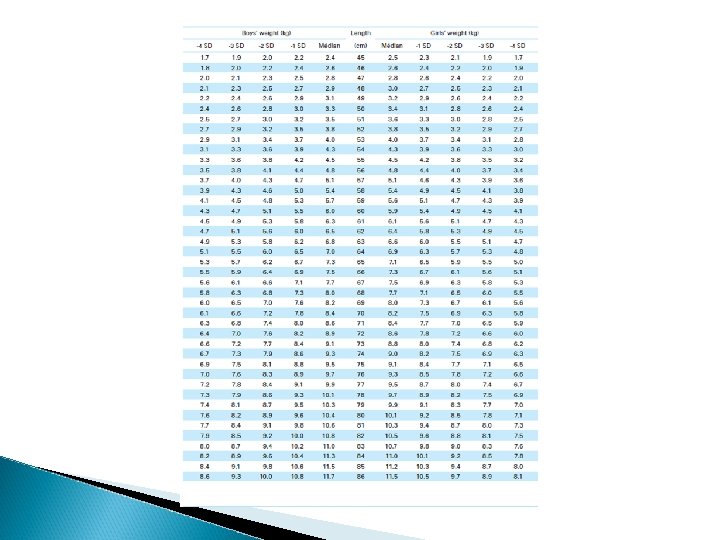
3. Anthropometric measurements May not accurately diagnose oedematous malnutrition due to added weight of oedema fluid. Anthropometric measurements include: ◦ ◦ ◦ Wt-for-age ht-for-age wt-for-ht MUAC head circumference skinfold thickness.

Ht-for-age < 90% centile (2 SD)→stunted and implies chronic malnutrition. (severe if <85% or -3 SD) Wt-for-age < 80% (2 SD)→malnourished (If <60% →marasmus [Wellcome criteria]) § difficult to accurately diagnose acute malnutrition wt-for-ht (age independent) ◦ Accurately assesses for acute wasting ◦ <80% (<2 SD)=moderate ◦ <70% (<-3 SD)=severe MUAC ◦ Has been used as proxy for wt-for-ht for children <5 yrs ◦ If <12. 5 cm, then severe wasting

Anthropometry cont. Head circumference § Malnutrition in the first 2 yrs of life may result in faltering HC § Rarely useful after 2 years Skinfold thickness • Assesses for the thickness of skin and subcutaneous fat and thus the nutritional store • Nutritional deficiency →loose and overhanging skin fold

4. Laboratory evaluation Not routinely employed in nutritional assessment Can sometimes be valuable. May also be useful in monitoring Rx response Lab abnormalities include: § § § ↓serum pre-albumin & albumin, ↓urea, ↓cholesterol, profoundly low K+, low Hb & MCV Low transferin


Management -1: Acute complications Actively looked for the following and treat: 1. 2. 3. 4. 5. Hypoglycaemia Hypothermia D and/or V (dehydration) Shock very severe anaemia 6. 7. 8. 9. heart failure severe dermatosis Xerophthalmia focus of specific infection

1. Hypoglycaemia: (RBS < 3 mmol/l) 50 mls of 10% dextrose or sucrose per os or NG tube. Alternatively, 5 ml/kg of 10% dextrose IV (if unconscious) Then start feed with F-75 q 30 min for next 2 hours plus monitor RBS 2. Hypothermia: (T<35⁰C axillary) Active warming – ◦ kangaroo technique, ◦ provide bulbs Passive warming- ◦ keep room temp at 250 C, ◦ don’t leave child uncovered or close to open window, ◦ promptly change wet nappies, ◦ warm hands during physical exams, ◦ wrap baby in clothes and cover head too

3. Diarrhoea/vomiting: Re. So. Mal 5 mls/kg q 30 min for 2 hrs then: alternate Re. So. Mal with F-75 qhourly 4. Shock: IVF (1/2 Darrows in 5%DW or R/lactate with added KCl [20 mmol/l] in 5% Dextrose) ◦ 15 ml/kg for 1 hour. ◦ Repeat x 1 if improving. O 2, IV antibiotics 5. V. Severe anaemia: (Hb <4 g/dl or PCV < 12%) Transfuse PRBCs 57 ml/kg or 10 ml/kg over 3 hours with IV lasix 6. Xerophthalmia: Vitamin A on days 1, 2, 15 plus: § treat eye infection if present. § Bandage eye after atropine and antibiotic eye drops if corneal ulceration

7. Severe dermatosis: Dilute potassium permanganate dabbing or GV painting 8. Heart failure: Iv lasix, restrict all fluids including feeds till out of failure 9. Specific focus of infection: Appropriate IV antibiotics. If no focus of infection and child has no acute complication, then oral antibiotics (cotrimoxazole or amox)

Management -2: Feeding + mineral supplement If no complications on presentation; ◦ out-patient mx in a feeding center with RUTF may be instituted For all SAM with complications, in-patient mx should be instituted Here, 2 types of milk feeds are prescribed: § F-75 during the acute stabilisation phase § F-100 in the subsequent rehabilitation phase

The feeds are prepared with added mineralmix or CMV In addition, all SAM should receive ◦ Folic acid (5 mg stat then 1 mg daily) ◦ Vit A on day 1 Where no mineral-mix, § Give analytical grade KCl or slow K (1/2 tab/kg/day) Iron should only be given in rehabilitation phase Stimulative play activity should be introduced

Important things not to do Do not use diuretics to treat oedema Do not use IV fluids for rehydration if not in shock Do not give iron during initial stabilisation Do not give high sodium diet Do not give high protein diet > 1. 5 g/kg/day or high calories >100 kcal/kg/day during the initial stabilisation phase Be careful with transfusion for anaemia that occurred after admission

Discharge & Follow-up Discharge preferably if wt-for-ht is > -2 SD or by linking up to out-patient feeding center after all acute complications have been treated Follow-up should be arranged Home visit may be arranged before and during discharge

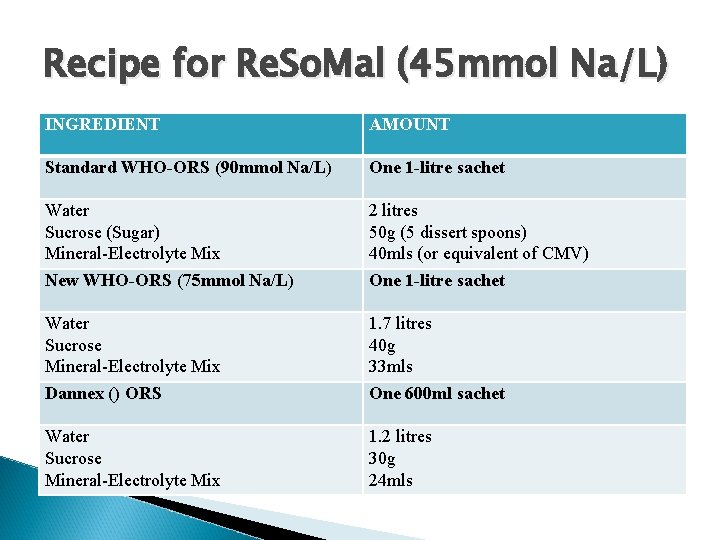
Recipe for Re. So. Mal (45 mmol Na/L) INGREDIENT AMOUNT Standard WHO-ORS (90 mmol Na/L) One 1 -litre sachet Water Sucrose (Sugar) Mineral-Electrolyte Mix New WHO-ORS (75 mmol Na/L) 2 litres 50 g (5 dissert spoons) 40 mls (or equivalent of CMV) One 1 -litre sachet Water Sucrose Mineral-Electrolyte Mix Dannex () ORS 1. 7 litres 40 g 33 mls One 600 ml sachet Water Sucrose Mineral-Electrolyte Mix 1. 2 litres 30 g 24 mls

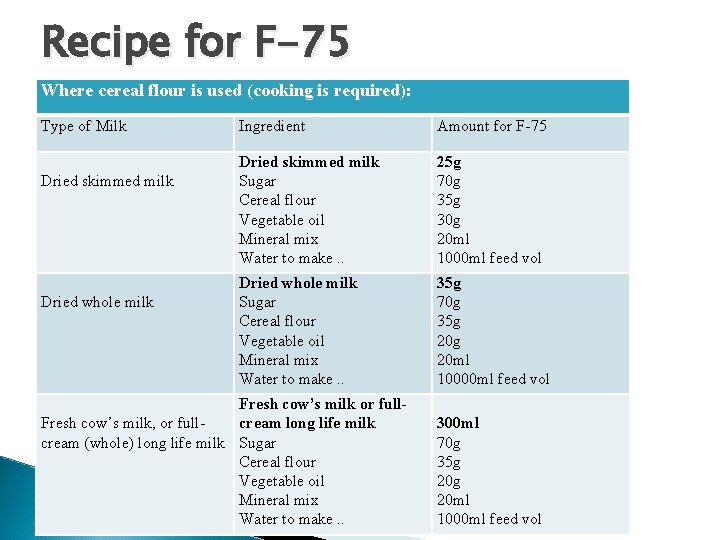
Recipe for F-75 Where cereal flour is used (cooking is required): Type of Milk Dried skimmed milk Dried whole milk Ingredient Amount for F-75 Dried skimmed milk Sugar Cereal flour Vegetable oil Mineral mix Water to make. . 25 g 70 g 35 g 30 g 20 ml 1000 ml feed vol Dried whole milk Sugar Cereal flour Vegetable oil Mineral mix Water to make. . 35 g 70 g 35 g 20 ml 10000 ml feed vol Fresh cow’s milk or full. Fresh cow’s milk, or fullcream long life milk cream (whole) long life milk Sugar Cereal flour Vegetable oil Mineral mix Water to make. . 300 ml 70 g 35 g 20 ml 1000 ml feed vol

Recipe for F-75 & F-100 cont. Where no cooking facility available, or cereal flour not used: (No cooking or cereal floor required for F-100) Type of milk Dried skimmed milk Dried whole milk Fresh cow’s milk, or full-cream (whole) long life milk Ingredient Amount for F-75 Amount for F-100 Dried skimmed milk Sugar Vegetable oil Mineral mix Water to make. . 25 g 100 g 30 g 20 ml 1000 ml feed vol 80 g 50 g 60 g 20 ml 1000 ml Dried whole milk Sugar Vegetable oil Mineral mix Water to make. . 35 g 100 g 20 ml 1000 ml feed vol 110 g 50 g 30 g 20 ml 1000 ml Fresh cow’s milk/fullcream long life milk Sugar Vegetable oil Mineral mix Water to make. . 300 ml 100 g 20 ml 1000 ml feed vol 880 ml 75 g 20 ml 1000 ml

References 1. 2. World Health Organization (1999). Management of severe malnutrition: manual for physicians and other senior health care workers. Geneva: WHO. United Nations Children’s Fund (2006). Malnutrition –the challenge. Available on line at: URL: http: //www. childonfo. org/areas/malnutrition/index/php 3. World Health Organisation (2005). Handbook: IMCI Integrated Management of Childhood Illness. Geneva. WHO. 4. World Health Organization (2000). Management of the child with a serious infection or severe malnutrition: guidelines for care at the first-referral level in developing countries. Geneva: WHO. 5. Antwi S. Malnutrition: missed opportunities for diagnosis. Ghana Med J. 2008 Sep; 42(3): 101 -4.