Assessing the burden of NCDs in populations Pascal

Assessing the burden of NCDs in populations Pascal Bovet, MD, MPH Institute of Preventive Medicine (IUMSP), University of Lausanne 9 th WHO-IUMSP International Seminar on the Public Health Aspects of NCDs Lausanne, 4 -8 May 2015
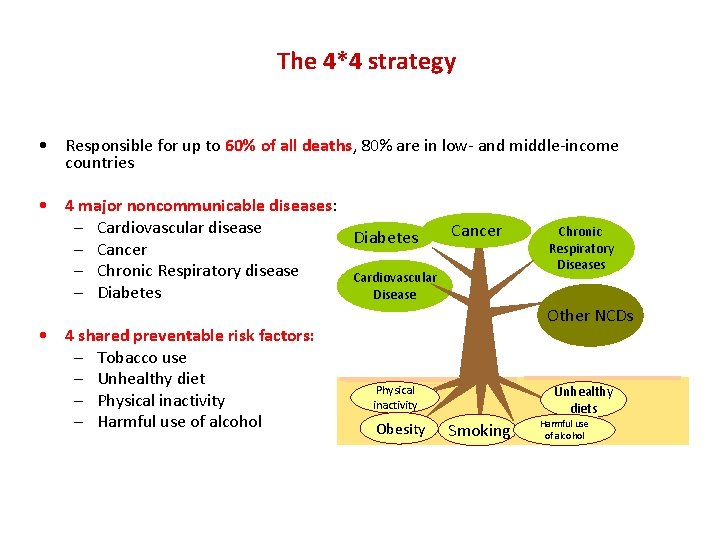
The 4*4 strategy • Responsible for up to 60% of all deaths, 80% are in low- and middle-income countries • 4 major noncommunicable diseases: – Cardiovascular disease Cancer Diabetes – Cancer – Chronic Respiratory disease Cardiovascular – Diabetes Disease • 4 shared preventable risk factors: – Tobacco use – Unhealthy diet – Physical inactivity – Harmful use of alcohol Chronic Respiratory Diseases Other NCDs Physical inactivity Obesity Unhealthy diets Smoking Harmful use of alcohol
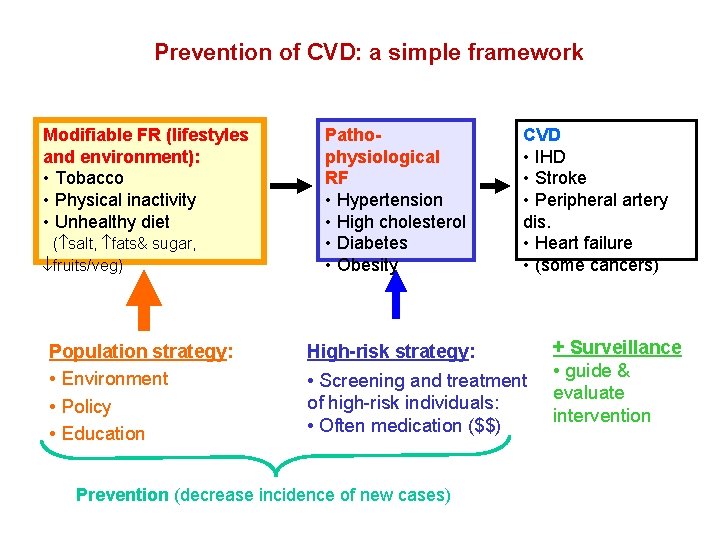
Prevention of CVD: a simple framework Modifiable FR (lifestyles and environment): • Tobacco • Physical inactivity • Unhealthy diet ( salt, fats& sugar, fruits/veg) Population strategy: • Environment • Policy • Education Pathophysiological RF • Hypertension • High cholesterol • Diabetes • Obesity CVD • IHD • Stroke • Peripheral artery dis. • Heart failure • (some cancers) High-risk strategy: • Screening and treatment of high risk individuals: • Often medication ($$) Prevention (decrease incidence of new cases) + Surveillance • guide & evaluate intervention

Origins of risk factors Proximal risk factors • Lifestyle: exercise, obesity, diet, stress, smoking • Treatments: blood pressure, cholesterol, diabetes Distal risk factors (distal) • • • Agricultural policy/food availability Social deprivation Climate change Fiscal policy eg tobacco Industrialisation/urbanisation
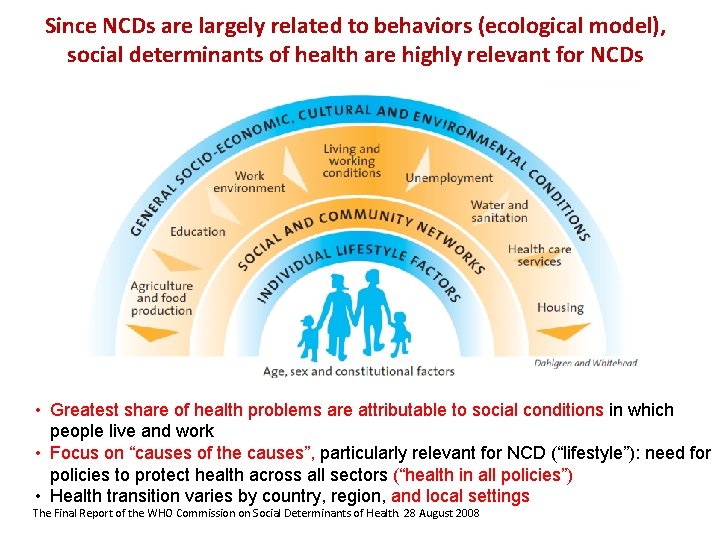
Since NCDs are largely related to behaviors (ecological model), social determinants of health are highly relevant for NCDs • Greatest share of health problems are attributable to social conditions in which people live and work • Focus on “causes of the causes”, particularly relevant for NCD (“lifestyle”): need for policies to protect health across all sectors (“health in all policies”) • Health transition varies by country, region, and local settings The Final Report of the WHO Commission on Social Determinants of Health. 28 August 2008
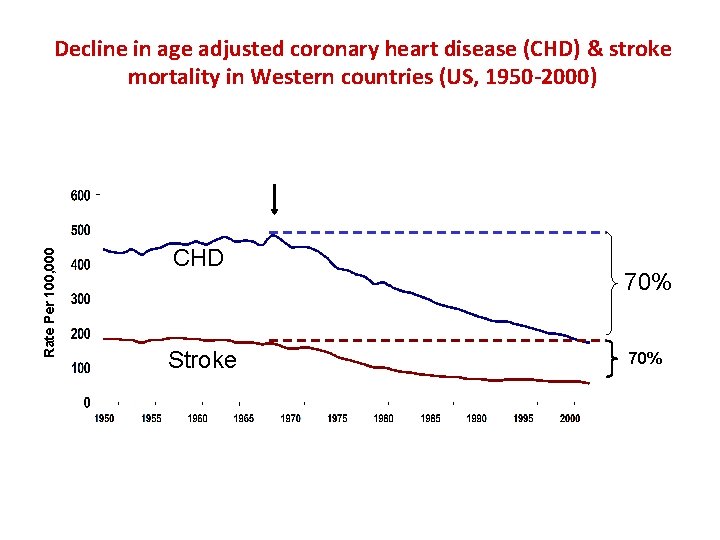
Rate Per 100, 000 Decline in age adjusted coronary heart disease (CHD) & stroke mortality in Western countries (US, 1950 -2000) CHD Stroke 70%
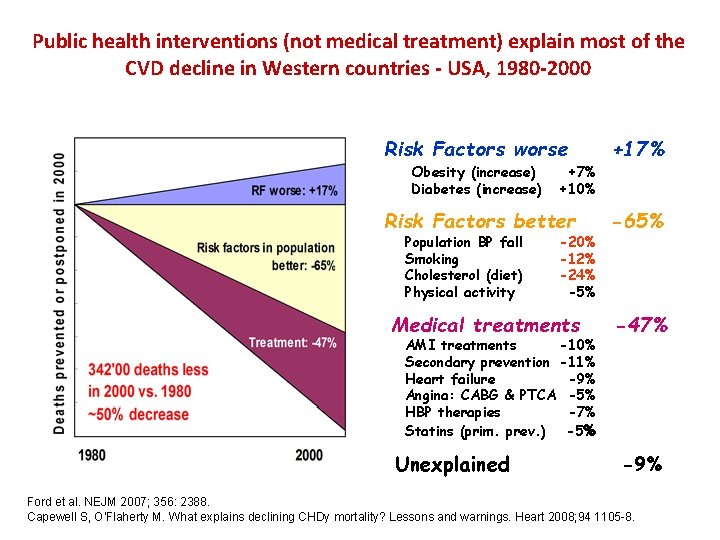
Public health interventions (not medical treatment) explain most of the CVD decline in Western countries - USA, 1980 -2000 Risk Factors worse +17% Risk Factors better -65% Medical treatments -47% Obesity (increase) Diabetes (increase) Population BP fall Smoking Cholesterol (diet) Physical activity +7% +10% -20% -12% -24% -5% AMI treatments -10% Secondary prevention -11% Heart failure -9% Angina: CABG & PTCA -5% HBP therapies -7% Statins (prim. prev. ) -5% Unexplained -9% Ford et al. NEJM 2007; 356: 2388. Capewell S, O'Flaherty M. What explains declining CHDy mortality? Lessons and warnings. Heart 2008; 94 1105 8.
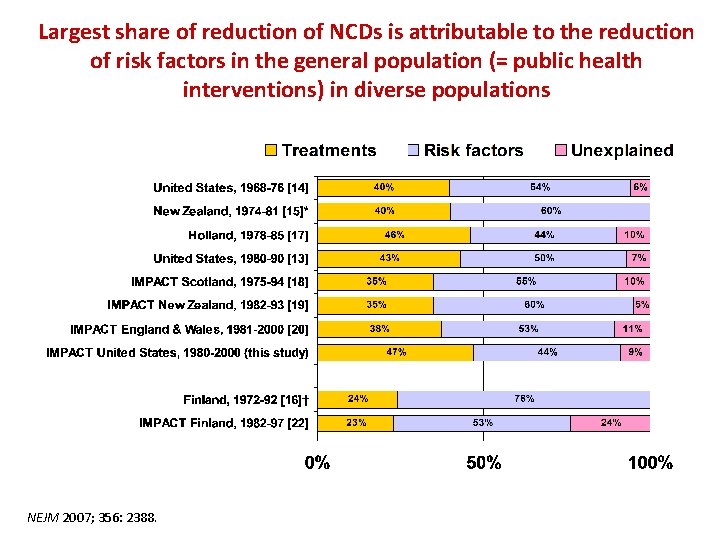
Largest share of reduction of NCDs is attributable to the reduction of risk factors in the general population (= public health interventions) in diverse populations NEJM 2007; 356: 2388.
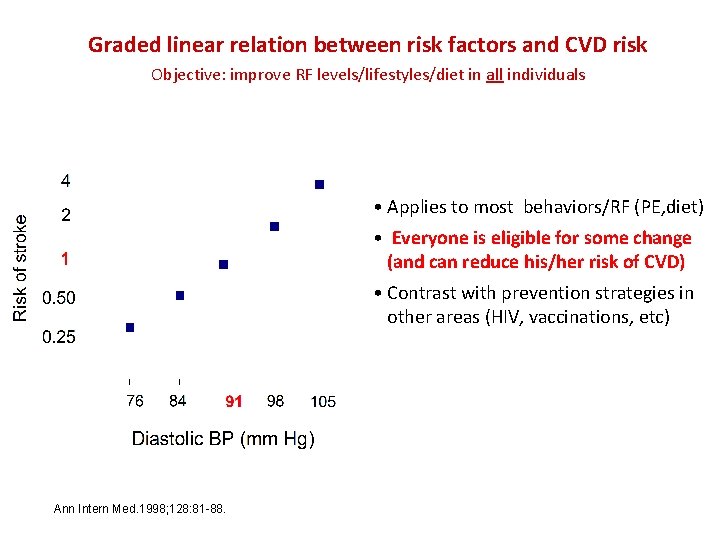
Graded linear relation between risk factors and CVD risk Objective: improve RF levels/lifestyles/diet in all individuals • Applies to most behaviors/RF (PE, diet) • Everyone is eligible for some change (and can reduce his/her risk of CVD) • Contrast with prevention strategies in other areas (HIV, vaccinations, etc) Ann Intern Med. 1998; 128: 81 88.
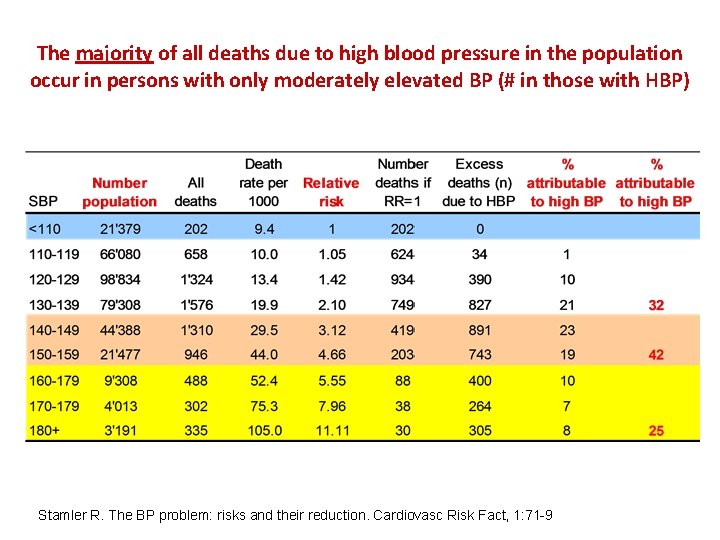
The majority of all deaths due to high blood pressure in the population occur in persons with only moderately elevated BP (# in those with HBP) Stamler R. The BP problem: risks and their reduction. Cardiovasc Risk Fact, 1: 71 9
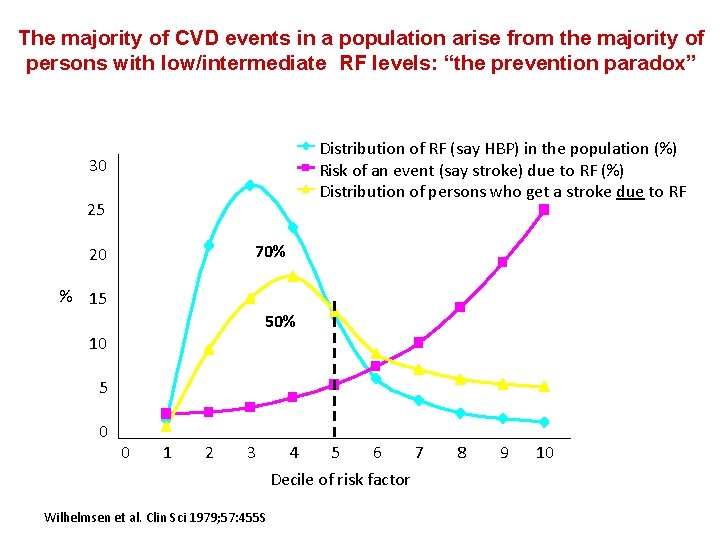
The majority of CVD events in a population arise from the majority of persons with low/intermediate RF levels: “the prevention paradox” Distribution of RF (say HBP) in the population (%) Risk of an event (say stroke) due to RF (%) Distribution of persons who get a stroke due to RF 30 25 70% 20 % 15 50% 10 5 0 0 1 2 3 4 5 6 Decile of risk factor Wilhelmsen et al. Clin Sci 1979; 57: 455 S 7 8 9 10
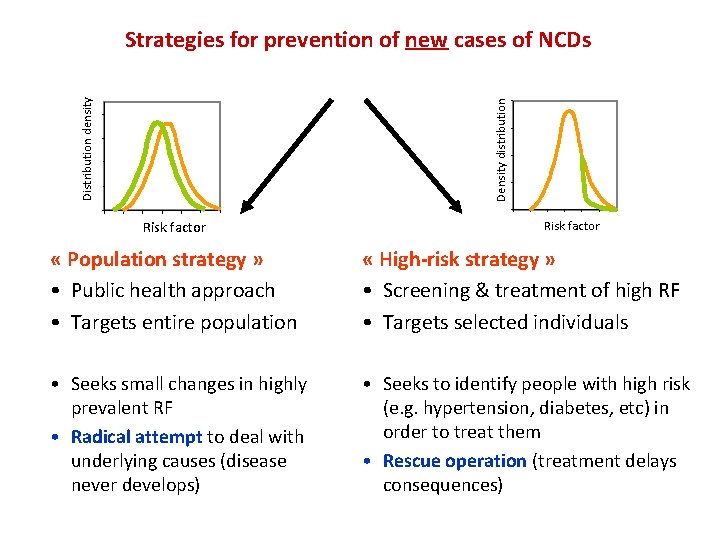
Density distribution Distribution density Strategies for prevention of new cases of NCDs Risk factor « Population strategy » • Public health approach • Targets entire population « High-risk strategy » • Screening & treatment of high RF • Targets selected individuals • Seeks small changes in highly prevalent RF • Radical attempt to deal with underlying causes (disease never develops) • Seeks to identify people with high risk (e. g. hypertension, diabetes, etc) in order to treat them • Rescue operation (treatment delays consequences)

Strategies to prevent NCDs in the population “Primary prevention: avoid occurrence of new cases” • Reduce RF levels in all individuals: population strategy – – – Create conducive environment enabling adoption of healthy lifestyle e. g. legislation, tax, financial incentives by government Small effect in individuals but large impact at entire population level Does not require behavior change, can be rapidly effective Often very cost effective (can even generate revenue: tobacco tax) “Good for all” • Detect and treat high-risk individuals : high-risk strategy – – – Screening (e. g. HBP, diabetes) and treat before complications occur Large effect in few people but small impact at population level Requires behavior change at individual level (compliance to drugs) Often costly (drugs for years for lots of patients) “Good for some”

Types of interventions for primary prevention of NCDs 1) Educational interventions • Media, school, workplace 2) Transportation policies (change environment) • Limit role of automobile (and increase use of buses): promote walking/cycling • Health promoting cities and environments 3) Improve food supply (change environment) • Improve process and manufacturing (salt, trans fat, saturated fats, etc) • Increasing availability and reducing cost of healthy foods • Promoting healthy food choices and limiting marketing to children 4) Economic policies: incentives and disincentives • Tax on tobacco • Differential taxes for energy dense foods/fruits-vegetables 5) Initiatives at the community level • Most effective when multifaceted, involving community • Dose of intervention and duration must be large enough Prevention of chronic diseases by means of diet and lifestyles changes. Disease Control Priorities in Developing Countries (DCPC 2), World Bank & WHO, 2006
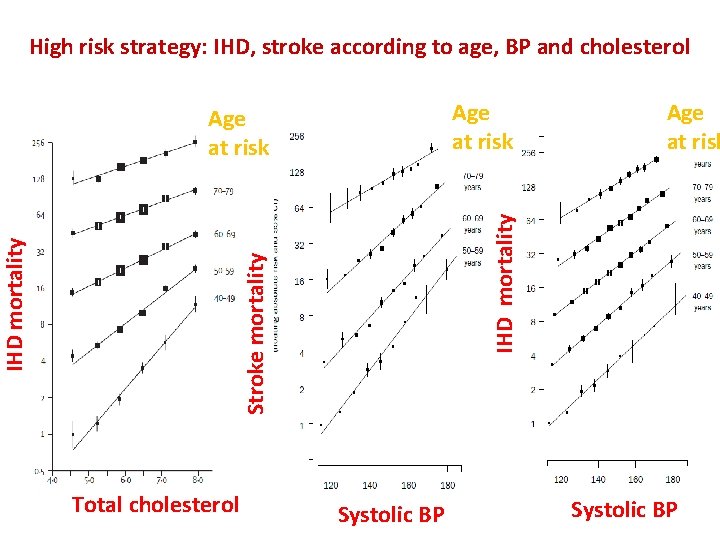
High risk strategy: IHD, stroke according to age, BP and cholesterol Age at risk Total cholesterol Age at risk IHD mortality Stroke mortality IHD mortality Age at risk Systolic BP
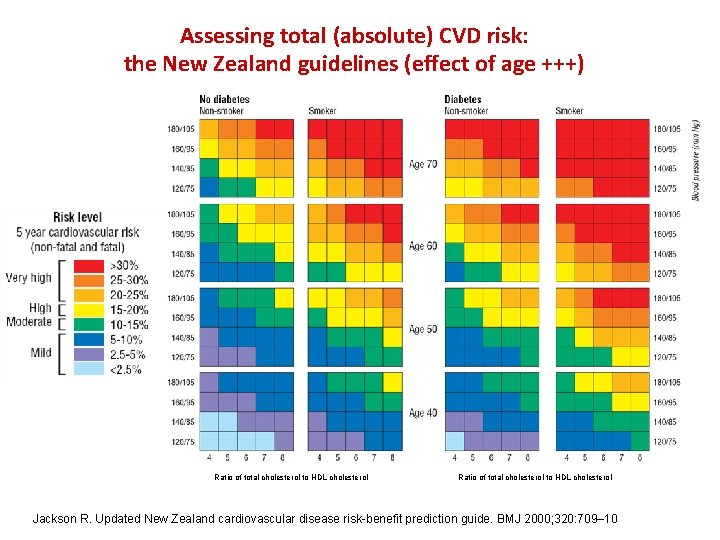
Assessing total (absolute) CVD risk: the New Zealand guidelines (effect of age +++) Ratio of total cholesterol to HDL cholesterol Jackson R. Updated New Zealand cardiovascular disease risk benefit prediction guide. BMJ 2000; 320: 709– 10

The “polypill”: a strategy to reduce CVD by >80% Polypill proposed for secondary prevention by Yusuf (Lancet 2002: 60: 2 -3) Wald & Law (BMJ 2003): a single “polypill” per day composed of six active ingredients could reduce CVD by 80% if taken by anyone aged >55 ACE-inhibitor (half-dose) Beta-blocker (half-dose) Diuretic (half-dose) Statin (standard dose) Aspirin (low dose) (in secondary prev) 20 cent per day (generic, LMICs) Wald & Law. BMJ 2003 Jun 28; 326(7404): 1419. Targeted several risk factors: • Blood pressure • LDL cholesterol • Platelet function • Vascular function

Prescribing treatment is no guarantee of result… Barriers for treatment approaches emphasize crucial role of public health measures (tax on tobacco, food regulations, etc)

Shaping the environment: improvement in street design
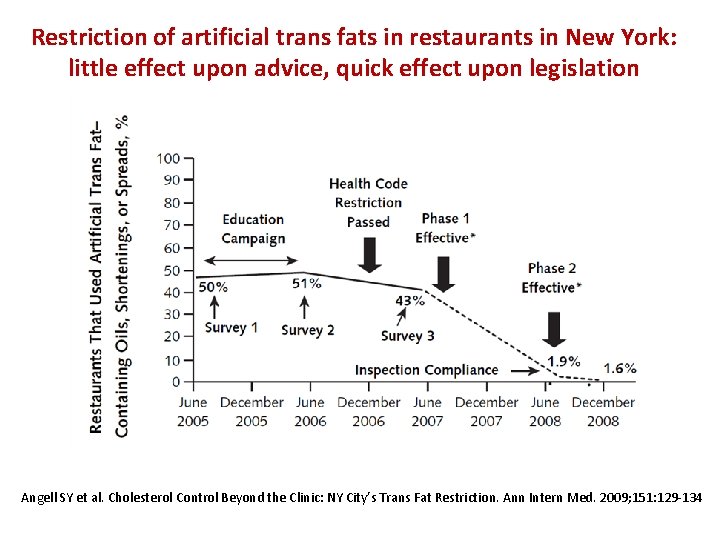
Restriction of artificial trans fats in restaurants in New York: little effect upon advice, quick effect upon legislation Angell SY et al. Cholesterol Control Beyond the Clinic: NY City’s Trans Fat Restriction. Ann Intern Med. 2009; 151: 129 -134
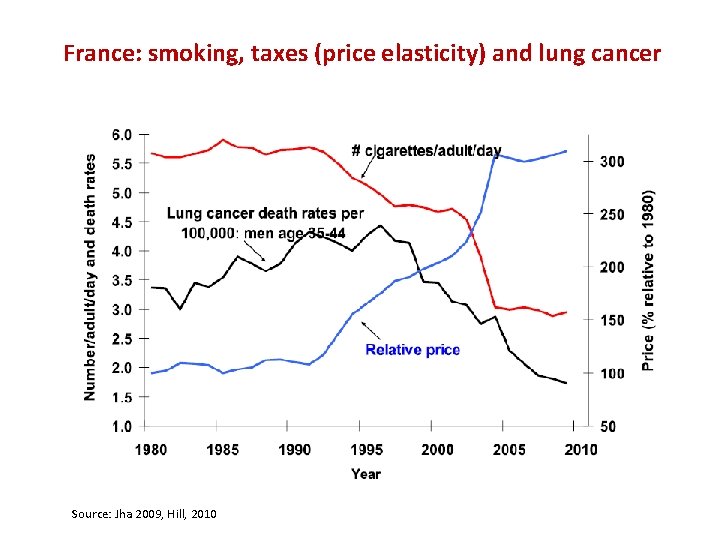
France: smoking, taxes (price elasticity) and lung cancer Source: Jha 2009, Hill, 2010
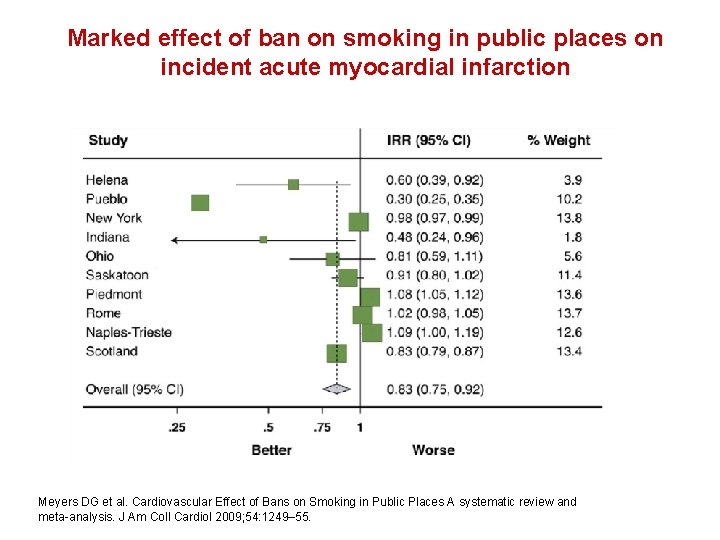
Marked effect of ban on smoking in public places on incident acute myocardial infarction Meyers DG et al. Cardiovascular Effect of Bans on Smoking in Public Places A systematic review and meta analysis. J Am Coll Cardiol 2009; 54: 1249– 55.

Why are the poorest people in low- and middle-income countries affected the most? WHO Framework Convention on Tobacco Control (WHO FCTC) • First global health legally binding treaty negotiated under auspices of WHO/UN • >180 parties (=countries that have ratified treaty) • Entered into force on 27 Feb 2005 • Creates international laws to: – Establish tobacco control as a priority on the public health agenda – Provide an evidence-based tool for adoption of sound tobacco control measures – Introduce a mechanism for firm country commitment, monitoring and accountability
![Main provisions of FCTC (1/2) • Prominence of public health [over trade] (Preamble) – Main provisions of FCTC (1/2) • Prominence of public health [over trade] (Preamble) –](http://slidetodoc.com/presentation_image_h2/777b259d9610ee715de9003bd0932c4e/image-24.jpg)
Main provisions of FCTC (1/2) • Prominence of public health [over trade] (Preamble) – “(Parties) determined to give priority to their right to protect public health” • Tax & price policies (Art 6) – Prohibition or restriction of duty free sales – Parties encourage to adopt high taxes • Protection from secondhand smoke (Art 8) – • Prohibit smoking in indoor workplaces/public places, and public transports Packaging and labeling (within 3 years) (Art 11) – Ensure that labeling is not "false, misleading, deceptive " (e. g. low tar, light, etc) – Health warnings for 50% but at least 30% & rotating • Advertising, promotion and sponsorship (within 5 years) (Art 13) – Comprehensive ban of all tobacco advertising, promotion and sponsorship – Parties have the right to ban cross border tobacco APS entering their territory

Main provisions of FCTC (2/2) • Education (Art 12) – Promote and strengthen public awareness of tobacco hazards & control issues • Treatment of tobacco dependence (Art 14) – Promote cessation of tobacco use and adequate treatment for tobacco dependence • Smuggling (Art 15) – Packets clearly marked for origin and final destination – Develop tracking and tracing regime and monitoring to investigate illicit trade • Sales to minors (Art 16) – Ban sales to minors – Restrict/ban vending machines • Liability (Art 19) – Consider legislation to deal with criminal and civil liability, incl. compensation • Surveillance of tobacco use and research (Art 20) – Establish programs for the surveillance of tobacco use • No reservation may be made to the Convention (Art 30)
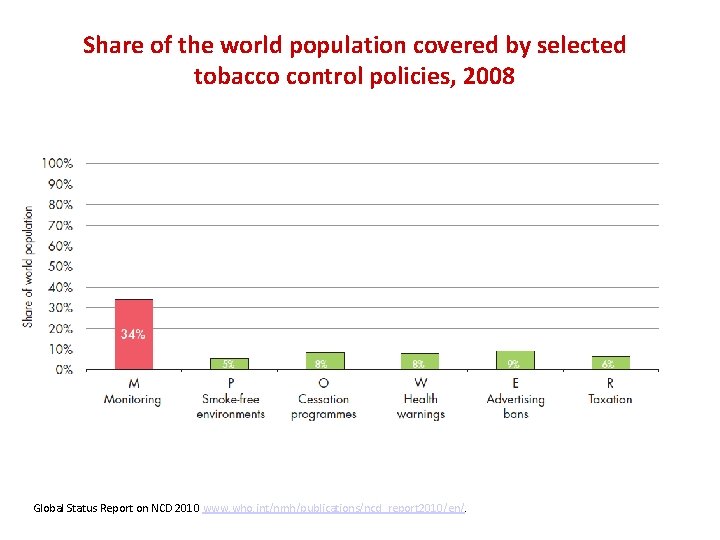
Share of the world population covered by selected tobacco control policies, 2008 Global Status Report on NCD 2010 www. who. int/nmh/publications/ncd_report 2010/en/.

Processes influencing the population prevalence of obesity: proximal vs distal determinants (individual level vs. societal approaches) Kumanyika S et al. Public Health Approaches to the Prevention of Obesity (PHAPO) Working Group of the International Obesity Task Force (IOTF). Obesity prevention: the case for action. IJO 2002; 26: 425– 436.

Examples of societal measures that can improve the environment of food choices • Small taxes on junk foods and soft drinks – reduces consumption & raise funds on anti obesity campaigns • Restrictions on food marketing to children – e. g. ban on vending machines in schools and on TV • Calorie labels on all foods (including fast foods) • Changes in farm subsidies and trade taxes to promote production / consumption of fruits and vegetables • Reformulation of foods (cooperation with food industry/regulation) – Ban trans fats, reduce sugar/salt/saturated fats Nestle M. Science 2003; 299: 781 Nestle M. Food politics: How the food industry influences nutrition and health

Examples of population strategies for primary prevention of obesity (and CVD) • Environment shaping – Sidewalks, safe public green areas, cycling lanes, pedestrian zones • Improving available diet – Alter food content (salt, sugar, saturated fats, trans-fatty acids) • Regulations – Labeling food content – Fiscal measures for production/trade of healthy/unhealthy foods – Advertising of junk foods, vending machines in schools
26 Jul 2008
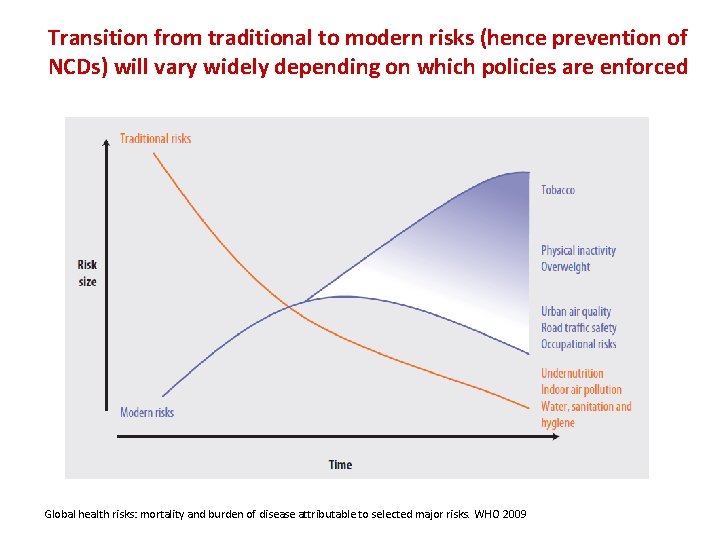
Transition from traditional to modern risks (hence prevention of NCDs) will vary widely depending on which policies are enforced Global health risks: mortality and burden of disease attributable to selected major risks. WHO 2009

Series of seminal policy documents to address NCDs 2000 Global Strategy for the Prevention and Control of Noncommunicable Diseases Global Strategy on Infant and Young Child Feeding 2002 2003 WHO Framework Convention on Tobacco Control Global Strategy on Diet, Physical Activity and Health WHA resolution on cancer prevention and control 2004 Action Plan on the Global Strategy for the Prevention and Control of NCDs 2005 Set of recommendations on the marketing of foods and non-alcoholic beverages to children 2008 2010 2011 Global Strategy to Reduce the Harmful Use of Alcohol High-level Meeting on NCDs (New York, 19 -20 September 2011)

“Best buys” for NCD prevention and control *Prevention* Reducing the level of exposure to risk factors *Management* Strengthen health care for people with NCDs Risk factor / disease "Best buy" Interventions Raise taxes on tobacco Protect people from tobacco smoke Warn about the dangers of tobacco Enforce bans on tobacco advertising Tobacco use - Harmful use of alcohol - Raise taxes on alcohol - Restrict access to retailed alcohol - Enforce bans on alcohol advertising Unhealthy diet and physical inactivity - Reduce salt intake in food - Replace trans fat with polyunsaturated fat - Promote public awareness about diet and physical activity Cardiovascular disease and diabetes - Provide counselling and multi-drug therapy for people with medium-high risk of developing heart attacks and strokes - Treat heart attacks with aspirin Cancer - Hepatitis B immunization to prevent liver cancer - Screening and treatment of pre-cancerous lesions to prevent cervical cancer UN General Assembly. Political declaration of the high-level meeting of the General Assembly on the prevention and control of noncommunicable diseases. A/66/L. 1. 16 September 2011. http: //www. un. org/ga/search/view_doc. asp? symbol=A/66/L. 1

Further cost-effective and low-cost population-wide interventions that can reduce risk factors for NCDs • Nicotine dependence treatment; • Promoting adequate breastfeeding and complementary feeding; • Enforcing drink driving laws; • Restrictions on marketing of foods/drinks high in salt/fats/sugar, esp. to kids; • Food taxes and subsidies to promote healthy diets. Strong evidence, but shortage of cost effectiveness research, for following : • Healthy nutrition environments in schools; • Nutrition information and counseling in health care; • National physical activity guidelines; • School based physical activity programs for children; • Workplace programs for physical activity and healthy diets; • Community programs for physical activity and healthy diets; • Designing the built environment to promote physical activity Global Status Report on NCD 2010 www. who. int/nmh/publications/ncd_report 2010/en/.
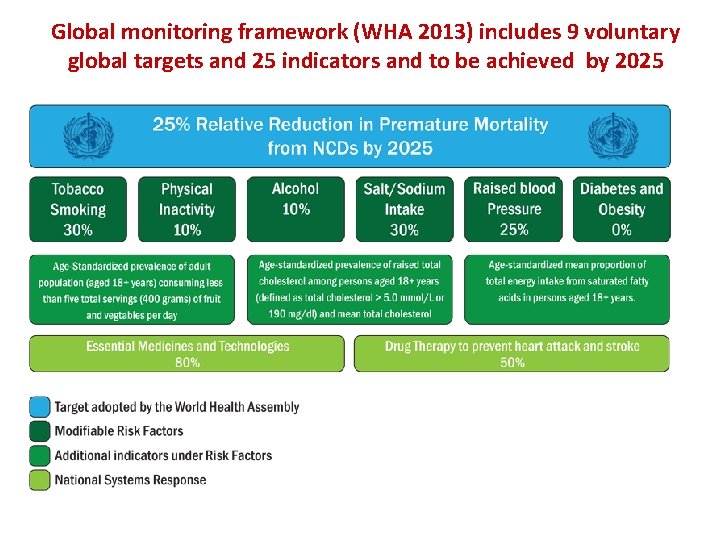
Global monitoring framework (WHA 2013) includes 9 voluntary global targets and 25 indicators and to be achieved by 2025

Priority actions recommended for Member States Accelerating progress at country level o Set national targets for 2025 in 2013, taking into account the 9 global targets o Develop national multisectoral NCD policies and plans to attain national targets for 2025 Implement interventions identified by WHO as "best buys" into the basic primary health care Implement interventions identified by WHO as "best buys" using WHO tools: o Tobacco use o Harmful use of alcohol o Unhealthy diet and physical inactivity o Strengthen national NCD surveillance systems o Integrate NCD surveillance systems into the national health information systems o Contribute information on trends in NCDs
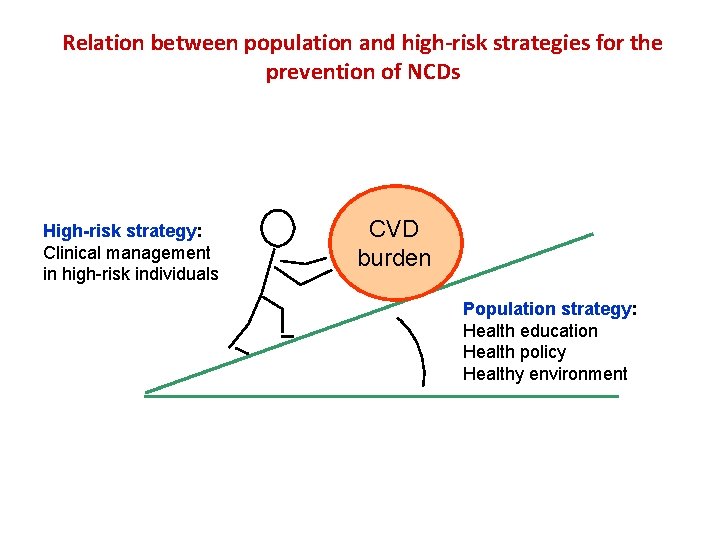
Relation between population and high-risk strategies for the prevention of NCDs High-risk strategy: Clinical management in high risk individuals CVD burden Population strategy: Health education Health policy Healthy environment
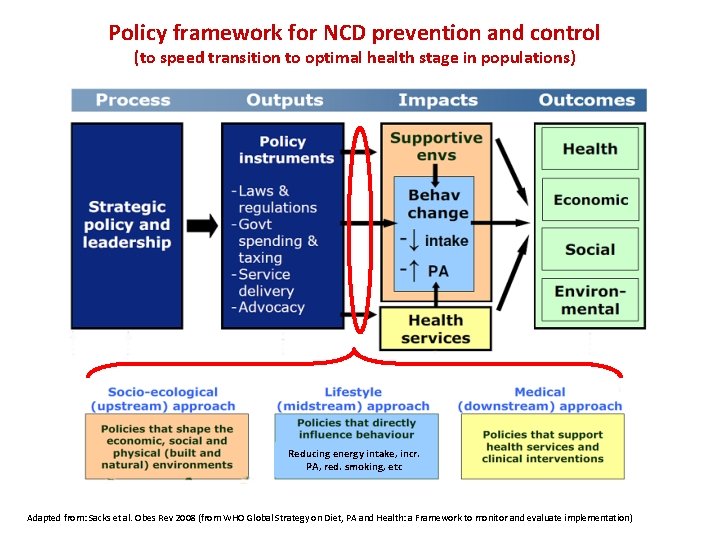
Policy framework for NCD prevention and control (to speed transition to optimal health stage in populations) Reducing energy intake, incr. PA, red. smoking, etc Adapted from: Sacks et al. Obes Rev 2008 (from WHO Global Strategy on Diet, PA and Health: a Framework to monitor and evaluate implementation)
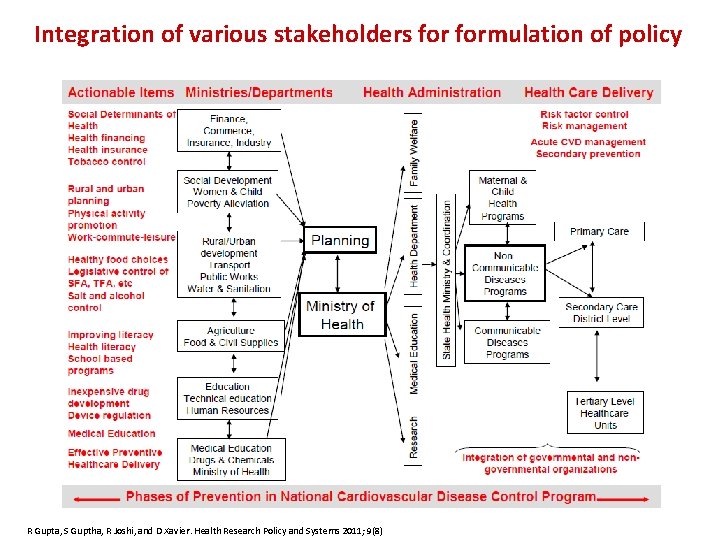
Integration of various stakeholders formulation of policy R Gupta, S Guptha, R Joshi, and D Xavier. Health Research Policy and Systems 2011; 9(8)
How to establish a multisectoral strategy/plan? (1/3) Development of national multisectoral action plans to attain national targets A national multisectoral NCD action plan with national targets provides the framework for addressing NCDs through a coherent public health approach Multisectoral action is central to the success of national NCD efforts and attainment of national targets Strategic planning requires concrete national targets Chapter 10
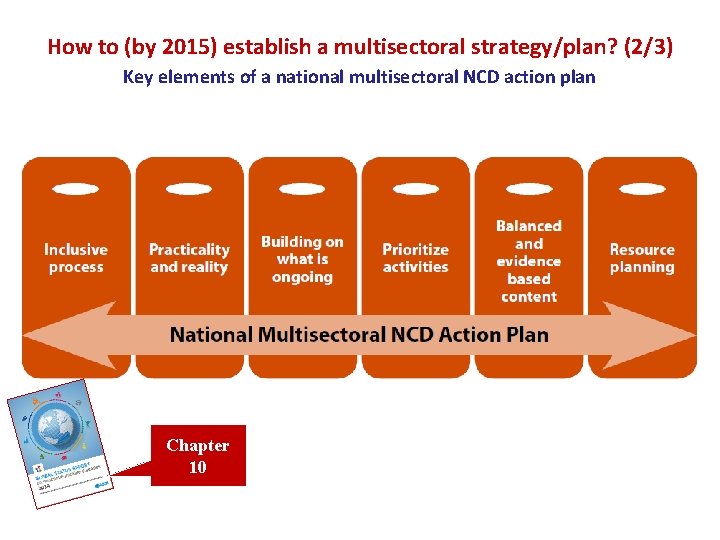
How to (by 2015) establish a multisectoral strategy/plan? (2/3) Key elements of a national multisectoral NCD action plan Chapter 10
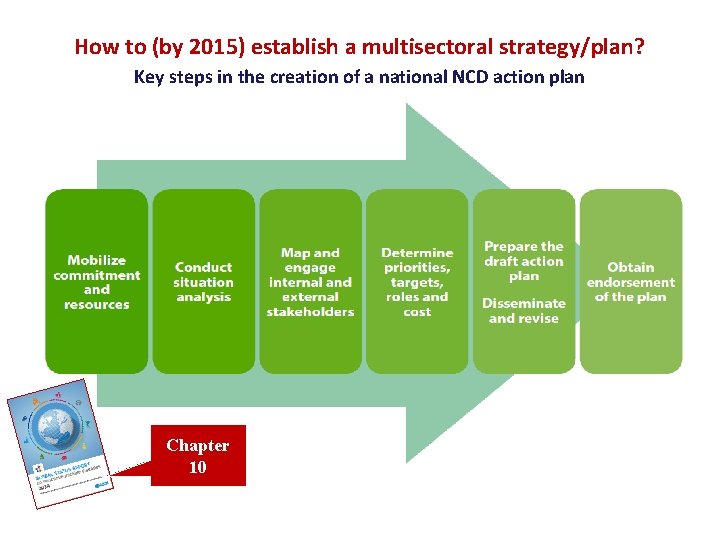
How to (by 2015) establish a multisectoral strategy/plan? Key steps in the creation of a national NCD action plan Chapter 10

Conclusions Ø Modifiable RF of NCD are known as well as effective interventions Ø Apply the knowledge Ø Multifactorial nature of NCDs underlie need for multisectoral action, coordination & partnerships Ø Emphasis on population approaches (high impact, potentially low cost) Ø Majority of NCD cases arise from persons with fairly low risk Ø Focus on population-wide interventions (radical, affordable) Ø Most effective PH interventions are outside the health sector Ø Need for selected high-risk approaches (screen & treat) Ø High cost, limited efficacy, commercial interests: careful selection Ø Can be good entry points for other programs/policy

Thank you for your attention! Selected references • Political Declaration of the High-Level Meeting of the General Assembly on the Prevention and Control of Non-communicable Diseases (WHO web site). • Plan of Action for the Prevention and Control of Noncommunicable Diseases 2013 -2013, WHO (A 66/A/CONF. /1 Rev. 1 ). • Global Status Report on NCDs 2014, WHO, Geneva 2015 • Lloyd-Jones DM et al. Defining and setting national goals for cardiovascular health promotion and disease reduction. The American Heart Association’s strategic impact goal through 2020 and beyond. Circulation 2010; 121: 586 -613. • Ezzati M, Riboli E. Can Noncommunicable Diseases Be Prevented? Lessons from Studies of Populations and Individuals. Science 2012 ; 337, 1482.
- Slides: 44