Assessing and Treating People with Brain injury in

Assessing and Treating People with Brain injury in the Mental Health Diversion Program: A Collaboration with Fred Victor Toronto, September 13, 2018 Robin Green, Ph. D, CPsych (Clinical Neuropsychology) Canada Research Chair (II) in Traumatic Brain Injury Clinical-Research Director, Telerehab Centre for ABI Mary Boulos, MSc Candidate, U of T Cognitive Neurorehabilitation Sciences Lab Toronto Rehab

Overview ● Traumatic Brain Injury - General Background ● Traumatic Brain Injury & the Criminal Justice System ● New program for TBI with Fred Victor and Mental Health Diversion Program
Neurological Disorders Congenital/Developmental/ Degenerative Disorders e. g. , Cerebral Palsy, Down’s Syndrome, Multiple Sclerosis, Lupus, Dementia
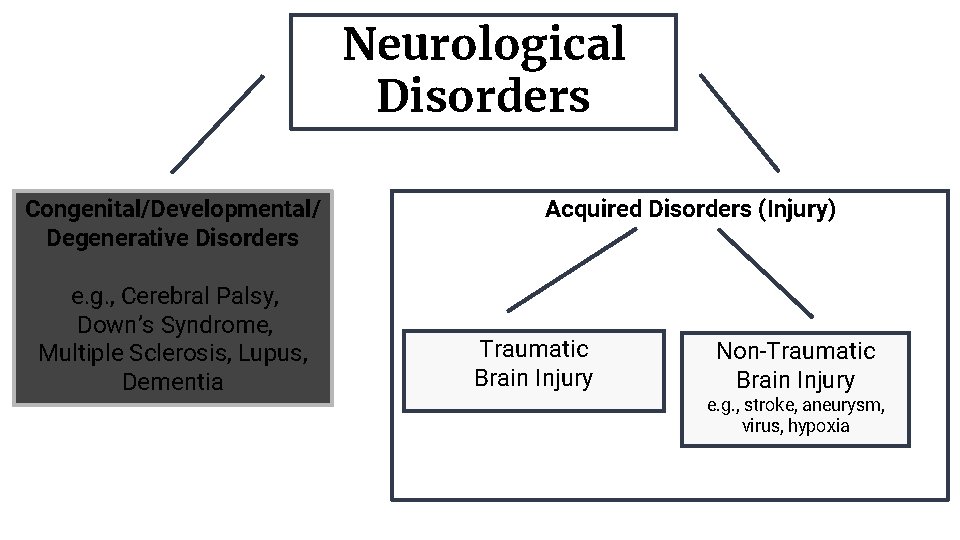
Neurological Disorders Congenital/Developmental/ Degenerative Disorders e. g. , Cerebral Palsy, Down’s Syndrome, Multiple Sclerosis, Lupus, Dementia Acquired Disorders (Injury) Traumatic Brain Injury Non-Traumatic Brain Injury e. g. , stroke, aneurysm, virus, hypoxia

Neurological Disorders Congenital/Developmental/ Degenerative Disorders e. g. , Cerebral Palsy, Down’s Syndrome, Multiple Sclerosis, Lupus, Dementia Acquired Disorders (Injury) Traumatic Brain Injury Non-Traumatic Brain Injury e. g. , stroke, aneurysm, virus, hypoxia

What is Traumatic Brain Injury (TBI) ● A TBI occurs when there is an external force exerted on the brain ● Major causes: ○ falls ○ sports injuries ○ motor vehicle accidents ○ assault ● Can occur with or without a direct blow to the head ● Injury severity: Mild (concussion) to severe

Concussion ● Traumatically induced temporary disturbance of brain function (alteration in consciousness) ● Event sets in motion complex physiological processes Adapted from: American Medical Society for Sports Medicine position statement: concussion in sport and from Ontario Neurotrauma Foundation concussion guidelines

Concussion Recovery ● Approximately 85% of people: rapid recovery - week to a month ● Approximately 15% of people have persisting symptoms of 1 month or longer ● Multiple concussions – slower recovery

Moderate to Severe TBI ● Permanent brain damage: ○ focal injuries (contusions, bleeds, hematomas) ○ diffuse injuries (axonal stretching/shearing; microbleeds; edema) ● While some neurological effects of moderate to severe TBI resolve (e. g. , swelling), others are permanent (e. g. , scar tissue, and possibly neuroinflammation)

Moderate to Severe TBI: Persistent Deficits ● Cognitive impairments: attention, memory, executive function. . . ● “Behavioural” impairments: impulsivity, inappropriateness. . . ● Emotional dysfunction: depression, anxiety, anger, suicidality… ● Personality changes: apathy, dependence, aggression… ● Motor Impairments: weakness, incoordination… ● Psychosocial consequences: unemployment, failure to return to school, broken relationships, social isolation

Moderate to Severe TBI: Recovery ● Most brain recovery occurs in the first days and weeks of TBI ● Cognitive recovery occurs for years, and is maximal in the first weeks and months ● Brain and cognitive effects are chronic; they may also be progressive (i. e. , worsen with time)

TBI & The Criminal Justice System

Outcomes of TBI that have been Associated with Criminality ● ● ● ● Impulsivity Emotional lability Aggression Irritability Substance abuse Memory impairment Concentration impairments Reduced rule-abiding behaviour Mauss-Clum & Ryan 1981; Leon-Carrion & Ramos 2003; Slaughter et al. 2003; Daniel 2007; Beckworth 2010; Williams 2010

TBI & The Criminal Justice System • Individuals with a history of TBI are 2. 5 times more likely to engage in criminal activity 1 • ~40% of Ontario prison population has sustained a TBI 2 • Offenders with TBI have 69% increased risk of recidivism 3 • TBI linked to earlier, more violent, more persistent offending 4 1. Mc. Isaac et al. 2016; 2. Colantonio et al. 2014; 3. Ray et al. 2017; 4. Williams 2012

TBI & The Criminal Justice System • Individuals in prison with TBI have ↑ history of felony convictions and misdemeanors 1 • Violent offenders have more lesions in frontal lobes 3 • Young offenders with history of TBI at greater risk of self-harm & suicide 4 1. Piccolino 2014; 2. Timonen et al. 2002; 3. Schiltz et al. 2013; 4. Chitsabsan 2015

Impact of TBI on Prison Health Services Previous research has demonstrated individuals with a history of TBI in prisons have: • Increased use of psychological/medical services • Increased crisis intervention • Less successful substance abuse treatment Piccolino & Solberg 2014

Needs in 1 CJS regarding TBI • Reduction of brain injuries • Earlier and more effective assessment and management • Increased awareness of TBI throughout criminal justice system to enable consideration of brain injury for: Sentencing, Rehabilitation, Resettlement Williams 2012

Collaborative Program for TBI with Fred Victor

Overarching Aims ● Improve functioning and well-being of highly vulnerable individuals ● Reduce recidivism ● Increase safety of communities

Objectives Assessment & Treatment ● Identify individuals in CJS with TBI ● Assess associated cognitive/mood impairments ● Provide treatment through remote delivery (via our telehealth centre)

Objectives Assessment & Treatment ● Identify individuals in CJS with TBI ● Assess associated cognitive/mood impairments ● Provide treatment through remote delivery (our telehealth centre) Education ● Raise awareness of prevalence of TBI in CJS ● Provide education about sequelae of TBI

Objectives Assessment & Treatment ● Identify individuals in CJS with TBI ● Assess associated cognitive/mood impairments ● Provide treatment through remote delivery (our telehealth centre) Education ● Raise awareness of prevalence of TBI in CJS ● Provide education about sequelae of TBI Influence policy/guidelines ● Ensure identification of TBI and access to intervention

Traumatic Brain Injury Program ● Partnership between Fred Victor and Toronto Rehabilitation Institute’s Cognitive Neurorehabilitation Sciences Lab – Dr. Green ● Providing services to individuals with TBI in mental health diversion program ● 2 primary services planned: ○ Neuropsychological assessment ○ Psychological and cognitive therapies
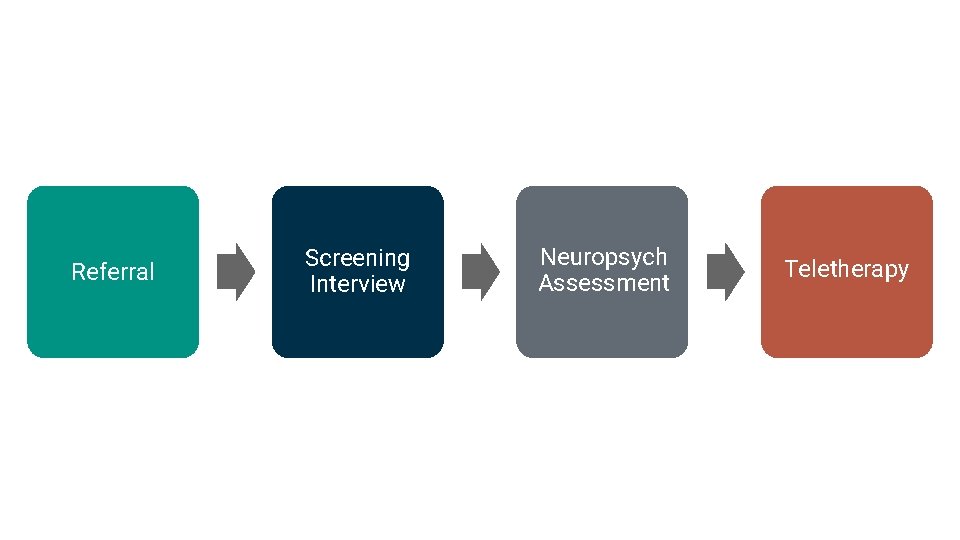
Referral Screening Interview Neuropsych Assessment Teletherapy

Referral

Referral Criteria ● Clients with TBI living in Toronto with history of mild to severe traumatic brain injury ● > 6 months post-injury ● Have insight (i. e. , awareness of challenges/difficulties) ● No active psychosis or severe substance abuse ● At least semi-fluent in English
Referral Screening Interview

Screening Interview ● Conducted at Old City Hall or College Park ● Gather more detailed info about client to confirm eligibility for program ● Ask about demographics, injury history, areas of difficulty, client’s needs ● Determine which services client is interested in
Referral Screening Interview Neuropsych Assessment

Neuropsychological Assessment Purpose: Develop profile of cognitive and neuropsychiatric strengths and weaknesses ● Clinical recommendations provided to client ● Results provided to the client/family members/caregivers ● Results used to triage client to determine eligibility for therapy
Referral Screening Interview Neuropsych Assessment Teletherapy

Teletherapy @ Telerehab Centre for ABI • Therapy provided remotely (i. e. , over webcam or telephone) • Three therapy modules available: • Cognitive behaviour therapy • Goal management training • Mindfulness meditation • Each module is approx. 8 -11 weeks long, 2 hours per week • Client assigned to modules depending on individual needs

Mindfulness Meditation ● Paying attention in a particular way – on purpose, in the present moment, and nonjudgmentally ● Demonstrated efficacy for cognitive functioning (especially attention) depression, anxiety, stress, aggression, physical pain, quality of life ● Can lead to structural and functional brain change Kabat-Zinn, 1994 Davidson, Johannsen et al. , 2012; For review of brain benefits see Green and Turner, 2008

Cognitive Behaviour Therapy ● Psychotherapy involving a problem-solving approach for changing unhelpful thinking and behaviours ● Problem focused“: tied to specific therapeutic goals/problems ● “Action oriented“: active identification of strategies for goals ● Demonstrated efficacy for depression, anxiety, aggression Greenberger & Padesky, 1995, 2015; Arundine et al, 2012; Bradbury et al, 2008; Fann et al, 2015; Hsieh et al. , 2012

Goal Management Training • Rehabilitation of higher-order cognitive skills such as executive functioning abilities – E. g. , managing time, paying attention, and remembering details • Improves planning and implementation of goals

Therapeutic benefits for TBI sequelae that have been associated with criminality ● ● ● Reduced: Impulsivity/disinhibition Emotional lability Aggression Irritability Substance abuse Attention/concentration impairments Mauss-Clum & Ryan 1981; Leon-Carrion & Ramos 2003; Slaughter et al. 2003; Daniel 2007; Beckworth 2010; Williams 2010

Therapeutic benefits for everyday life? • Improved follow through on plans/goals (e. g. , attending court dates, parole meetings, etc. )? • Decreased combativeness/violence? • Improved personal and professional relationships?

Progress So Far • Increased TBI education/awareness in CJS • Collaborative partnership with Fred Victor & community organizations established • Referral procedure established • Neuropsychological assessments underway

Expert Consensus Panel Recommendations from Schofield et al (2016) Following a consensus meeting in 2016, a series of recommendations were made for TBI and criminal justice system. Of these, we have accomplished the following: ✔ Educate criminal justice system stakeholders about TBI ✔ Develop different models for responding to people with TBI ✔Develop pathways for people with a TBI ✔ Develop a person-centred approach encompassing a communitybased prison model Schofield et al. 2016

Challenges Impediments to diagnosis and treatment – Lack of available health records, permanent address, social supports – Comorbid substance abuse – Comorbid neuropsychiatric deficits (unrelated to TBI, e. g. , psychosis); our services developed for TBI-related deficits Identifying TBI patients with more “invisible injuries” of TBI that may contribute to criminality (e. g. , impulsivity, poor judgement, anger), but who are not in mental health diversion program

Solutions • Greater focus on neuropsychological assessment with clinical recommendations; less focus on “therapies” from which patients are unlikely to benefit • Improve identification and management of TBI by focusing on multiple time points and contexts (e. g. , at arrest, sentencing, , post-release) • Continue to develop partnerships with justice community organizations

THANK YOU Questions? Ideas?

Lab Members Robin Green Brenda Colella Liesel-Ann Meusel Lily Miguel-Jaimes Marika Dabek Mary Boulos Tom Worthington Michelle Panozo Alana Changoor Joanna Glazer Greg Noack Lesley Ruttan Bhanu Sharma Pavel Tselichtchev Tuck Voon-How Sally Abudiab Collaborators Priyanka Prince Taha Arshad Jenkin Mok Eliyas Jeffay Rochelle Chauhan Adina Levi Zorry Belchev Julia Rybinka Kadeen Johns Walter & Maria Schroeder Institute for Brain Innovation and Recovery Fred Victor Organization Natasha Bartlett Vesna Milinkovic MHCSWs at Old City Hall & College Park

Upcoming Event Concussion Symposium for Lawyers, Insurers, Judges, and Clinicians When: Thursday, December 6 th, 2018 Where: Donald Lamont Learning Centre, 130 Queen Street West Held by: The Canadian Concussion Centre in collaboration with the Law Society of Ontario Registration: https: //store. lsuc. on. ca/concussion-symposiumfor-lawyers-judges-and-clinicians

For more information, presentation requests, or opportunities for collaboration: Please contact 416 -597 -3422 x 7332 or mary. boulos@uhn. ca
- Slides: 45