Assessing and Managing Back pain in the Workplace

Assessing and Managing Back pain in the Workplace Jonathan Daniel MCSP HCPC Occupational Health Physiotherapist (Director) Copyright Fit. Back 2015

What does the next hour look like? • Explore your current process of assessment • Common types of back pain • Assessment and diagnosis of back pain • Identifying red flags- When to refer on • Initial management and advice for back pain Copyright Fit. Back 2015

Your current processes? • How do you currently assess and manage your patients with back pain? • What are the aims of your assessment? • What are you hoping to use the findings from your assessment for? • Do you have any frustrations with your current processes? Copyright Fit. Back 2015

Government initiative ‘Improving Working Lives’ 2008 • Recommendations of the Black Report • Early intervention is the key to successfully managing common health problems in the workplace. • Employers should recognise the importance of maintaining health at work as it produces considerable economic benefits • There should be closer liaison between employers and G. P. s to facilitate earlier return to work. Copyright Fit. Back 2015

But there is a problem- waiting times • Average waiting times to see G. P. - Up to 3 weeks • Average waiting times for physiotherapy 11. 8 weeks. (CSP 2011) • Waiting times for non urgent consultant referral –up to 18 weeks. Copyright Fit. Back 2015

Back Pain In The Workplace • • Lifting Bending Twisting Stooping Poor Posture (driving, PC`s) Prolonged Seated Position (driving) Whole Body Vibrations (Driving HGV`s) Copyright Fit. Back 2015

Common Problems • • Neck (Cervical) Midback (Thoracic) Lower Back (Lumbar) Sacroiliac ( sacrum) – Disc ( Prolapses, Degeneration) – Joint Dysfunction: facet joints, instability – Muscular/ Ligament strains, tears, pulls – Nerve root irritation – Arthritis Copyright Fit. Back 2015

A review of the anatomy of the spine Copyright Fit. Back 2015
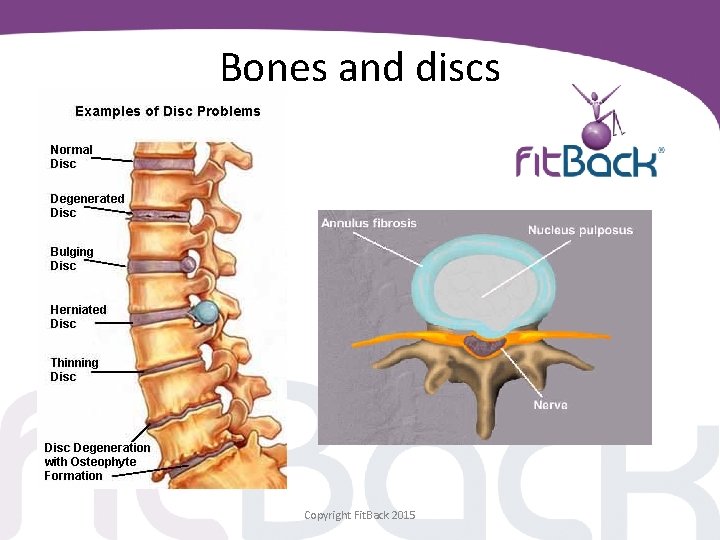
Bones and discs Copyright Fit. Back 2015
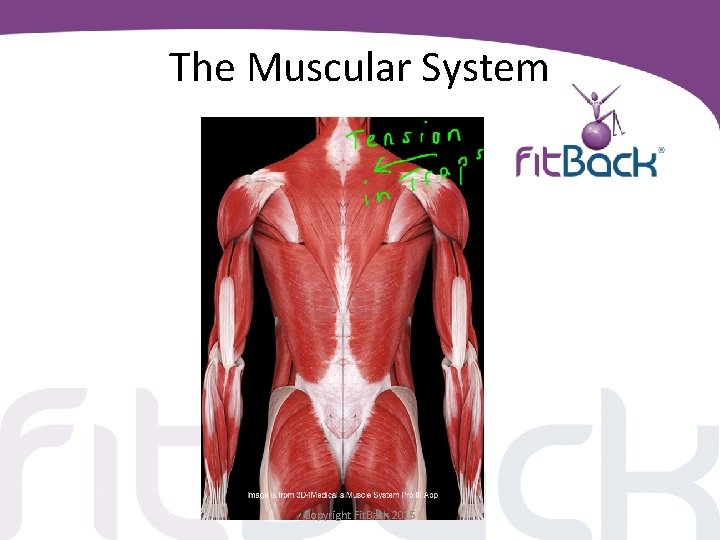
The Muscular System Copyright Fit. Back 2015

Primary care givers • Given the current lengths of waiting lists, as occupational health professionals in the workplace we are often the primary care givers. • Therefore it is vital that we are give the right type of care and advise at the earliest possible opportunity. • This will help to prevent common health problems resulting in chronic disability. Copyright Fit. Back 2015

The role of OH in back pain • What do you see your role as? • Give advice • To help facilitate return to work if an employee is absent • To recommend amendments to duties to help keep an employee in work • To liaise with other health care professionals and make onward referrals where appropriate Copyright Fit. Back 2015

Back Pain • How can OHNs/advisors differentiate between the different types of back pain? • Subjective history and basic assessment. Copyright Fit. Back 2015

History Taking is Key • Careful questioning is vital to help diagnose • Patients can be poor historians! • Very often there is no one incident or recollection of injury • Often there is a slow progression of symptoms • Symptoms don`t always tie in with the pathology or results of Xray/ MRI……. ! Copyright Fit. Back 2015
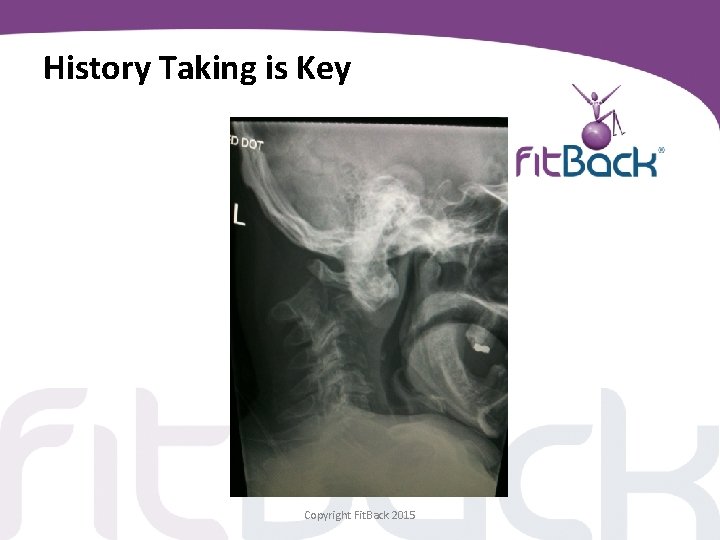
History Taking is Key Copyright Fit. Back 2015

Back Pain Clinical Standards Advisory Group diagnostic triage: • Simple backache ( mechanical LBP) (95% of patients); • Nerve root pain (<5% of patients); • Possible serious spinal pathology (<1% of patients). • Clinical Standards Advisory Group. Back pain. HMSO; 1994. Copyright Fit. Back 2015

Simple mechanical back pain • Presentation between ages 20 -55 • Lumbosacral region, buttocks and thighs • Pain "mechanical" in nature i. e. – varies with physical activity – varies with time • Patient well • Prognosis good Copyright Fit. Back 2015

Acute back pain • • • Sudden onset Pain ++ often from muscle spasm Restricted movements Difficulty getting comfortable Very often will settle in a few days/ week Copyright Fit. Back 2015

Chronic low back pain • • • Back pain > 12 weeks Often very longstanding Source of pain not clearly defined Lots of previous interventions Possible psychosocial issues. • EUROPEAN GUIDELINE FOR THE MANAGEMENT OF CHRONIC NON-SPECIFIC LOW BACK PAIN November 2004 Copyright Fit. Back 2015
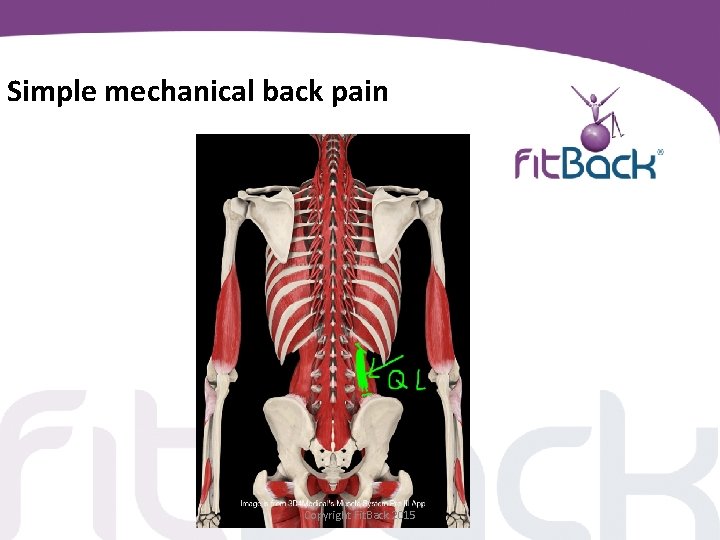
Simple mechanical back pain Copyright Fit. Back 2015

Back pain with radiculopathy ( nerve root involvement) • Unilateral leg pain worse than low back pain • Pain++ ( often constant) generally radiates to foot or toes • Numbness and parasthesia in the same distribution • Prognosis reasonable – 50% recover from acute attack within 6 -8 weeks Copyright Fit. Back 2015

Serious spinal pathologies • Infection, Tumor, Osteoporosis, Ankylosing Spondylitis ( inflammatory arthritis), Fracture, Inflammatory conditions, radicular syndromes or cauda equina syndrome • (EUROPEAN GUIDELINES FOR THE MANAGEMENT OF ACUTE NONSPECIFIC LOW BACK PAIN IN PRIMARY CARE 2004) Copyright Fit. Back 2015

What are red flags? Copyright Fit. Back 2015
What are the Red Flags associated with back pain? • Previous history of Ca (38%) Breast Prostate, Lung, Ovarian • Systematically unwell. Fever malaise (6%) • Cauda Equina ( Bladder and bowel dysfuction) • Thoracic Pain (13%) • Unexplained weight loss (38%) • Unable to lie supine (13%) • Recent Major accidents • Constant progressive pain (57%) • Progressive neurological deficit gait disturbance (6%) Copyright Fit. Back 2015

Cauda Equina lesions – Difficulty with controlling urination – Loss of anal sphincter tone or fecal incontinence – Saddle anesthesia about the anus, perineum or genitals Patient’s with these symptoms require urgent onward referral with a covering letter Copyright Fit. Back 2015

Why do we need to know about red flags? • Health professionals in an occupational health setting are working in a primary care setting • We may be the first health contact • Waiting lists are long and red flags need to be identified and acted upon early. Copyright Fit. Back 2015

Subjective/ objective assessment Back pain assessment form Copyright Fit. Back 2015

Objective Examination • • Patients expect to be touched and examined! Don’t be afraid to carry out a basic assessment Observe their standing posture Bending forward, backwards, to the side – Are the movements restricted / painful? – Note range of movement and any pain and region of pain • Straight leg raise (SLR) (Positive test indicates nerve involvement) Copyright Fit. Back 2015
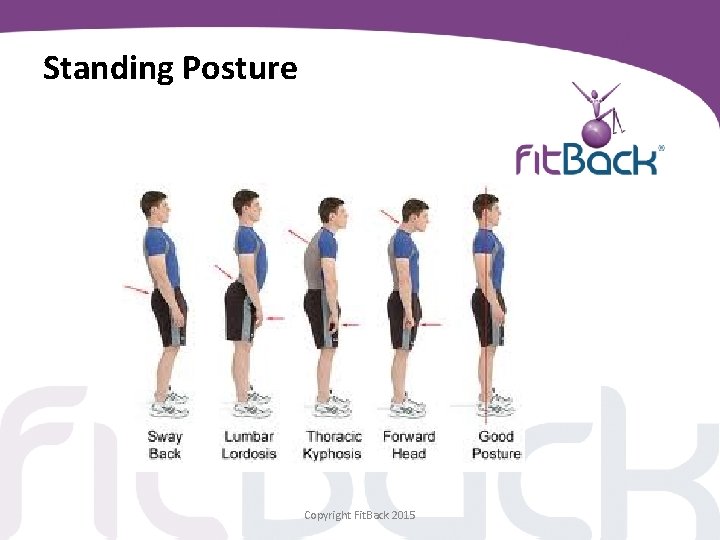
Standing Posture Copyright Fit. Back 2015

What can you do to assess this back pain? • Careful questioning will indicate how serious the pathology is and if there any psychosocial issues present. • It can indicate the type of back pain • Once you have decided what type of pain it could be then you can take action Copyright Fit. Back 2015

What might the patient tell you? . . . Flags • I`m terrified I`m going to end up in a wheel chair (Yellow flag) • Work is going to make my pain worse (Yellow/Blue flag) • My manger isn`t interested (Blue flag) • My manager doesn`t want me coming back to work until I`m 100% fit ( Black/ Blue flag) • There are no light duties at work so I may never get back to work ( Black/ Yellow Flag) Copyright Fit. Back 2015

Pathway for the care of low back pain. • Initial assessment Initial assess ment and diagn ostic triage • Red flags suspected- refer with urgency to G. P. With covering letter. • Radicular pain -refer for physiotherapy assessment and treatment • Simple mechanical back pain- reassurance and baseline advice: DSE assessment, refer for physiotherapy. • If sickness absence anticipated - refer for physiotherapy. Copyright Fit. Back 2015

Copyright Fit. Back 2015

What`s a good DSE set up? Move the chair close to the desk and sit back on the seat. Adjust the chair back so that the upper body is relaxed and supported. Raise the chair seat so that, with the upper arms vertical, the elbows are level with or just above the desk. 90 DEGREE RULE www. ergo. info

What`s a good DSE set up? Raise the monitor so that the visible screen top is just below eye level. www. ergo. info

Baseline Advice for acute low back pain • Hand out leaflet on managing back pain • The advice you give at your first meeting with the patient is crucial. • “Low back pain is common and is rarely due to a serious problem” • “From what you have told me there is no indication of a serious problem. ” • Use basic pain relief (can include ice or heat) • Relative rest for 1 or 2 days only • Keep active Copyright Fit. Back 2015

“Fit. Back For Life” Mobilise and Stretch • Back pain prevention workshop • Education and exercises • Conditions and strengthens the spine • Effective for both chronic and acute back pain.

Summary • Most back pain isn`t serious • With careful questioning and listening you can identify the serious pathologies and those needing urgent assessment • Proving the right advice and timely onward referral is key Copyright Fit. Back 2015

- Slides: 39