Aseptic loosening of Hip Prostheses Ernesto Pintore Istituto






























- Slides: 34

Aseptic loosening of Hip Prostheses Ernesto Pintore Istituto Clinico Mediterraneo Agropoli (Salerno) - Italy

Prosthetic Surgery = Life quality

AIM OF REVISION SURGERY • GOOD FUNCTION • QUALITY OF LIFE

TECHNICALLY DIFFICULT VARIETY OF IMPLANTS LEARNING CURVE INSTRUMENTS

RECENT PROGRESS: -BIOMATERIALS -DESIGNS -IMPROVED CEMENTING TECHNIQUE -MODULAR PROSTHESES

• SEPTIC LOOSENING • ASEPTIC LOOSENING

SEPTIC LOOSENING • CLINIC • LABORATORY • X-RAY • SCINTIGRAPHY

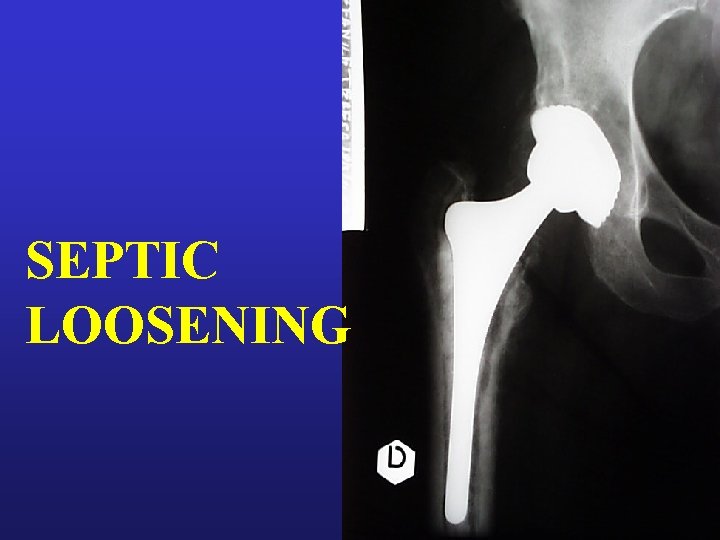
SEPTIC LOOSENING

ASEPTIC LOOSENING MECHANICAL FAILURE: “Aseptic loosening of one or both components, fracture of a component, recurrent dislocation of the hip, fracture of the femoral shaft. ” Callaghan JJ; Salvati E. A. et al. JBJS 1985

ASEPTIC LOOSENING OF THE FEMUR • • • MALPOSITION OF THE STEM FRACTURE OF THE IMPLANT FRACTURE OF THE FEMUR RECURRENT DISLOCATION INADEQUATE STEM DESIGN INADEQUATE CEMENTING TECHNIQUE • INADEQUATE CEMENT LAYER

ASEPTIC LOOSENING OF THE CUP • • POOR BONE COVERAGE MALORIENTATION too vertical, >60° POLYETHYLENE FAILURE EXCESSIVE HIGHT OF THE CUP >35 mm compared to the contralateral • INADEQUATE CEMENT TECHNIQUE fixation holes and thickness of cement layer • SMOOTH CUPS and RE-CEMENTED • THREATED CUPS

X-RAY FEMUR • • • VARUS-VALGUS OF THE STEM VERTICAL SUBSIDENCE HORIZONTAL MIGRATION RADIOLUCENCY OSTEOLYSIS FRACTURE OF THE CEMENT

X-RAY ACETABULUM • • VERTICAL MIGRATION HORIZONTAL MIGRATION CUP HIGHT CUP ANGLE RADIOLUCENCY OSTEOLYSIS POLYETHYLENE FAILURE

FEMORAL BONE STOCK Poor: if the thickness of either aspect of the cortex on the AP x -ray had decreased by 50%, along a 10 cm segment of femoral stem, compared with the original arthroplasty, or if the thickness of both aspect of the cortex had decreased this amount along a 5 cm segment

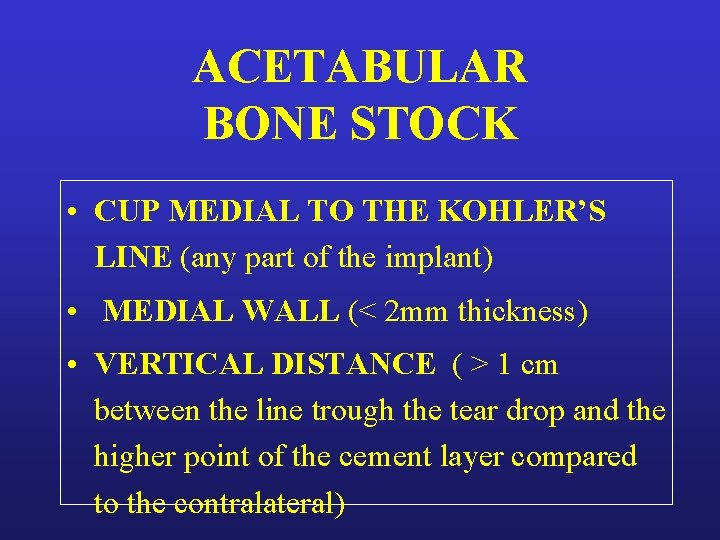
ACETABULAR BONE STOCK • CUP MEDIAL TO THE KOHLER’S LINE (any part of the implant) • MEDIAL WALL (< 2 mm thickness) • VERTICAL DISTANCE ( > 1 cm between the line trough the tear drop and the higher point of the cement layer compared to the contralateral)

A. A. O. S. Classification for bone stock damage • MILD • MODERATE • SEVERE

CLINIC - PAIN - START UP HECITANCY

DEFINITION OF ACETABULAR LOOSENING (Harris and Mc Gunn JBJS 1986) DEFINITE LOOSENING: • change of position of the implant, or cement. • fracture of the cement • radiolucency at the cement-implant interface PROBABLE LOOSENING: • no migration or change of position • continuous radiolucency (100%) at cement-bone interface POSSIBLE LOOSENING: • radiolucency 50%-99% at the cement-bone interface

WEAR DEBRIS The wear debris is responsible of a local inflammatory reaction with histyocytes an mast cells proliferation, that leads to osteolysis and loosening of the implant.

OPERATIVE TECHNIQUE • • CHOICE OF THE APPROACH POSTERO-LATERAL APPROACH OSTEOTOMY OF THE TROCHANTER FEMORAL “WINDOW” WAGNER TECHNIQUE REMOVAL OF THE CEMENT IMPLANTS

IMPLANTS • • • STANDARD STEM LONG STEM SURFACE MODULAR PROSTHESES “LOCKING NAIL” PROSTHESES

BONE GRAFT • AUTOGRAFT • HOMOGRAFT • ALLOGRAFT Only an accurate reconstruction of the anatomy can allow a good result in the revision surgery ( Bone bank)

CEMENT OR NOT CEMENT?

ALTHOUGH MODIFICATION AND IMPROVING OF CEMENTING TECHNIQUE HAVE DECREASED THE INCIDENCE OF FEMORAL AND ACETABULAR LOOSENING IN THR, THRE IS NO EVIDENCE DEMONSTRATING BENEFITS IN REVISION SURGERY WITH THE CEMENT. Engh C. ; Glassman A. (Instructional course lecture 1991)

CRITERIA FOR DETERMINING BIOLOGIC FIXATION • BONE INGROWTH • STABLE BONE-FIBROUS TISSUE • UNSTABLE IMPLANT

BONE INGROWTH • NO IMPLANT MIGRATION • ADAPTIVE REMODELING OF THE SURROUNDING BONE

CAUSES OF SUCCESS IN FEMORAL REVISION • • • FRESHENING THE BONE RESTORE THE BONE STOCK IMPROVED TROCHANTERIC FIX. TREATEMENT OF PERFORATIONS ADEQUATE STEM: -Extensevely porous coated -Design (filling)

CAUSES OF FAILURE • • BAD BONE STOCK TROCHANTERIC PROBLEMS MISDIAGNOSED PERFORATIONS INADEQUATE DESIGN OF THE IMPLANTS DYSPLASIC AND NECROTIC HIPS INFECTION CURVE OF LEARNING

RESULTS OF UNCEMENTED REVISIONS (C. Engh - A. Glassman) • 163 hips • 80, 7% of bone ingrowth • 12, 3% of stable fibrous tissue • 3, 5% unstable implants re-revised

COMPLICATIONS SYSTEMIC COMPLICATIONS • Urinary infections • Cardiac problems • DVT • Pulmonary embolism • Blood loss (1000 -1500 ml)

LOCAL COMPLICATIONS • • Superficial and deep infections Trochanteric nonunion (10%) Trochanteric problems Fracture of the femur Perforation of the femur Fracture of the pelvis Recurrent dislocations (9 -12%) Ectopic bone

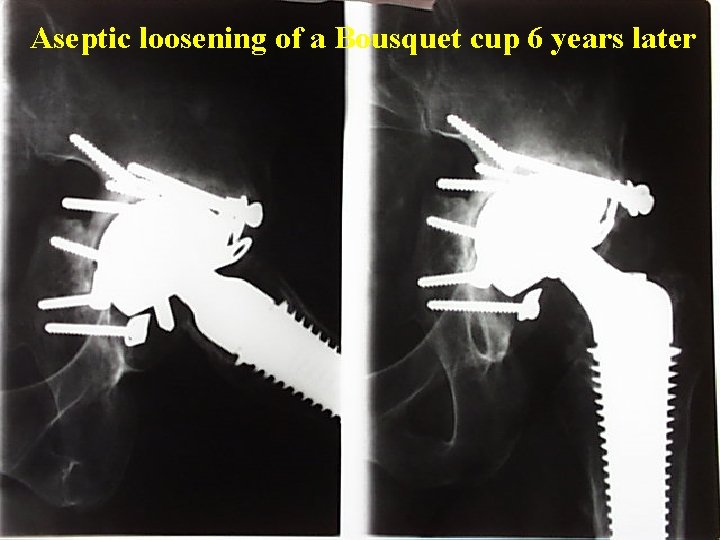
Aseptic loosening of a Bousquet cup 6 years later

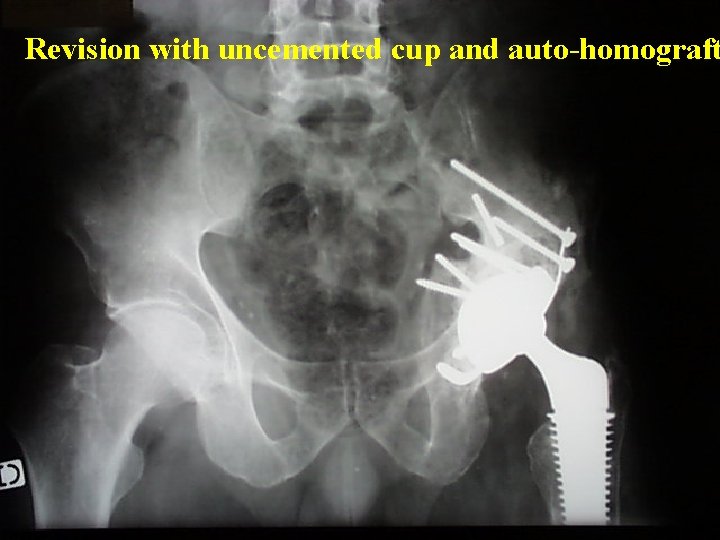
Revision with uncemented cup and auto-homograft

Revision surgery is technically difficult and requires an experienced surgeon and economic means to achieve the most performant devices. There are many complications and the results are not always good. The learning curve is long but despite this we beleave that this is the surgery wich we have to develop in the future.