ARTTB Initiation Counseling Patientcentered ART Initiation and Adherence

ART/TB Initiation Counseling Patient-centered ART Initiation and Adherence counseling model

Objectives At the end of the training you will be able to: – Know the structure of the adapted ART/TB Initiation counseling model – Know what all the tools are, and use them appropriately – Understand the importance of the Adherence Plan and how to complete it with the client – Apply the 14 steps to assist the client to complete the counseling sessions – Perform ART/TB initiation counseling and PMTCT counseling

How many squares do you see?

Rationale for a adapted counseling model Think about your counseling at the moment: • What counseling support do your patients need? - Post-initiation support Challenging social circumstances Problem-solving Co infection with HIV/TB (or other conditions) • What do you think are the qualities of a good counselor?
Overview of adapted model with a new approach toward patients, putting them at centre in order to find solutions to their problems Structure Approach Tools Training Mentoring
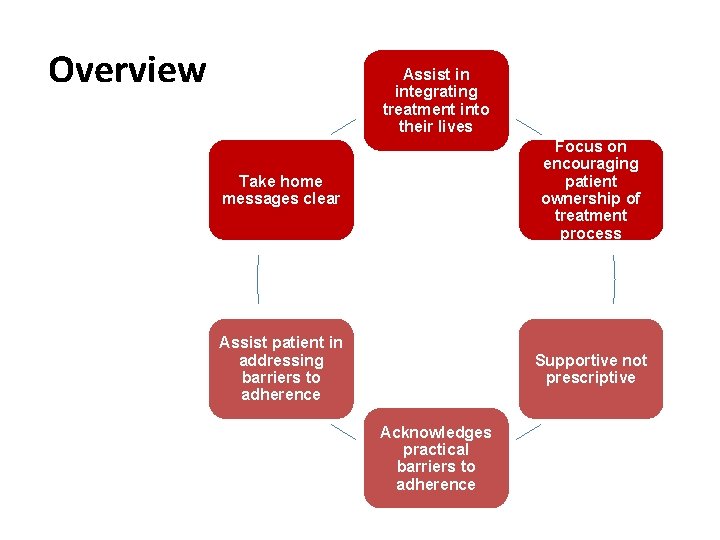
Overview Assist in integrating treatment into their lives Take home messages clear Focus on encouraging patient ownership of treatment process Assist patient in addressing barriers to adherence Supportive not prescriptive Acknowledges practical barriers to adherence
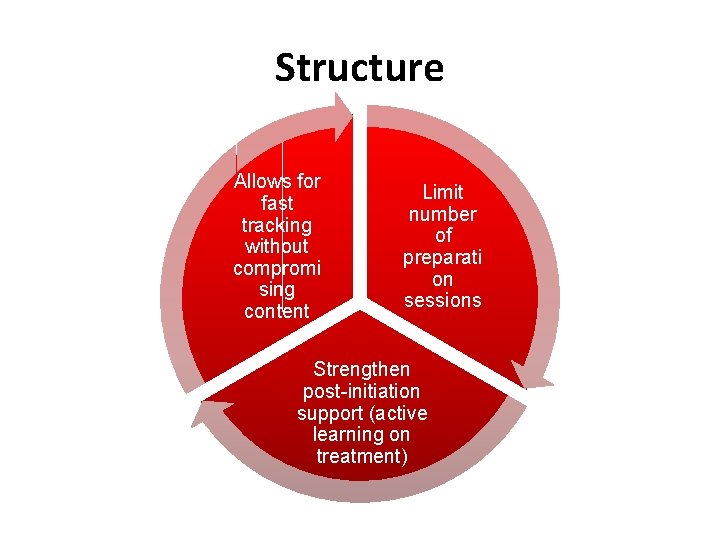
Structure Allows for fast tracking without compromi sing content Limit number of preparati on sessions Strengthen post-initiation support (active learning on treatment)
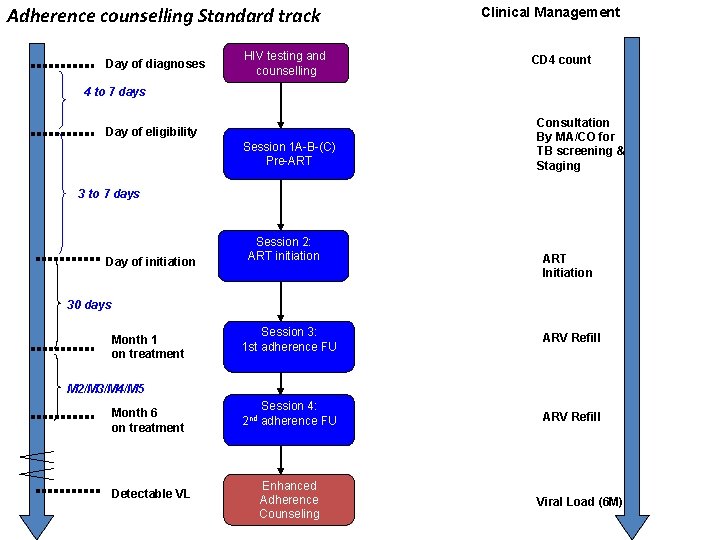
Adherence counselling Standard track Day of diagnoses HIV testing and counselling Clinical Management CD 4 count 4 to 7 days Day of eligibility Session 1 A-B-(C) Pre-ART Consultation By MA/CO for TB screening & Staging 3 to 7 days Day of initiation Session 2: ART initiation ART Initiation 30 days Month 1 on treatment Session 3: 1 st adherence FU ARV Refill Session 4: adherence FU ARV Refill M 2/M 3/M 4/M 5 Month 6 on treatment Detectable VL 2 nd Enhanced Adherence Counseling Viral Load (6 M)
Approach 14 simple specific adherence support steps to address Limit time spent on repeated treatment literacy Patient centered readiness to initiate
Approach: ABC’s of adherence Identify the GOAL Identify the BARRIERS to achieving the goal Work on making a PLAN to overcome the barriers

ABC’s of adherence in practice Adherence Step 7 - Storing medication and extra doses Review adherence goal “It is important to identify a convenient place to store medication so that you have easy access and are easily reminded” Identify barriers “Where could you keep your medication at home? ” “How could you carry your medication when you go out? ” Make a concrete plan Identify safe and convenient place to store drugs at home or at place where patient usually takes his/her drugs Identify a place to carry extra doses of drugs, what to keep them in - in case patient does not make it in time to usual storage place (e. g. envelope in pocket of woman’s bag, plastic bag in man’s backpack or jacket he usually wears)

Tools • Simplified flipchart (HIV/ART, TB, PMTCT) • Session guide (for lay counselors) • Adherence plan (put in patient file)

ARV Patient Education Flipchart • Simplified flipchart for group/individual educational session • Limited to treatment literacy for Session 1 A only

TB Flipchart

Flipchart for PMTCT ART Initiation • Covers general PMTCT information in addition to routine ART adherence messages • For group/individual educational session

Adherence Plan • For patient file

Session guide for counselors • Step by step guide • Structured in ABC approach (goal, barrier, plan)
Adherence steps • Adherence steps are associated with 3 reasons to stay healthy and alive • Move away from treatment focus, but rather on why… 1. 2. 3. I want to be alive for my children I need to be able to earn I want to see my children grow older

Mentoring tools Counselor observation tool • Who is responsible for this? – MSF Patient Support Officers are responsible for providing mentorship to the lay counselors at the facilities • How is this completed? – Observation of sessions – Feedback on sessions – Develop goals with counselor to strengthen/improve counseling

Overview complete!

Building Session 1 A ART/TB Initiation and Adherence Counseling Model

Brainstorm! What is the most important information a patient should learn and know about HIV?

Session 1 • 3 parts to session 1 (A + B + C - All done on same day) • Education session (A) • Individual session (B) • Non readiness session (C) • Content covers: Adherence Steps 1 -4

Review flipchart • In pairs read through Flipchart together

End of Building Session 1 A Next time to Role Play Session 1 A

Session 1 A: Review • When do we do Session 1 A? – As soon as eligible patient referred to counseling • What tools are needed? – Flipchart • Remember to start from the cover page. • Start with overview of the colours/images and what they stand for – this is your first introduction to the components of the flipchart AND the patient’s learning

Role play Session 1 A: – What tools do you need? – Introduction (intro facilitator, explain objectives, confidentiality) – Work through flipchart

End of Role Play Session 1 A Next Building Session 1 B

Building Session 1 B ART/TB Initiation and Adherence Counseling Model

Brainstorm! What should a patient know or learn about their treatment journey? What are the most common challenges that a patients faces when learning to take their treatment?

Overview of Adherence Plan

End of Building Session 1 B Next time to Role Play Session 1 B

Session 1 B Role Play – When do we do Session 1 B? • Immediately after 1 A – What tools do you need? • Adherence Plan, guide – Introduction (intro facilitator, explain objectives, confidentiality) – Work through session with your partner (each person has a turn at being the counselor) – Use your manual -READ, READ !!

End of Role Play Session 1 B Next Session 1 C Discussion

Session 1 C • How soon after patient says ‘they are not ready to start ART’ do we do Session 1 C? üImmediately • Why do we need session 1 C? üGive the patients time and space to share the reasons why they are not ready to start treatment üAllows us to better understand their reasons for non -readiness

Session 1 C • How do we do this? – Allow the patient to share – Give a listening ear to the patient – Share other patients stories (testimonies) of having overcome barriers to starting treatment – Work together to make a plan to overcome their reasons for non-readiness

Session 1 C • GROUP or INDIVIDUAL : why? • Tools: session guide, testimonies, • Overview of session: – – Invite the patient to share why they don’t feel ready Choose the testimony that best fits their needs/reasons Read the testimony Discuss the way forward to overcoming these reasons

Day 1 complete!

Welcome to Day 2

Recap of Day 1 • How many sessions are in the model? • What is the order of the sessions? • Name 4 adherence steps • What are the ABCs of Adherence? • Name tools!

Recap of Day 1 ART/ TB Treatment Counseling Model contains: • Sessions: 4 sessions - 1 education session, 1 day initiation, 2 post initiation follow-up • Tools: flipchart (2), counselor session guide, adherence plan • Approach: patient-centered, supportive, address the common adherence challenges, focus on reasons to be healthy and alive • ABCs of Adherence: Goals, Barriers, Plans

Building Session 2 ART/TB Initiation and Adherence Counseling Model

Session 2 • When do we do Session 2? - On the day of treatment initiation • Which tools are needed? – Session guide, Adherence Plan • Review all content covered in: Adherence Steps 5 -9 - Medication schedule - Managing missed doses - Reminder strategies - Storing medication - Dealing with side effects

Session 2 Role Play • Introducing Observation and Feedback (discussion) • In groups of 3 role-play the session: • 1 counselor • 1 patient • 1 observer – Observer asks counselor: how did the session go? What went well, what could improve? – Observer report back: give your own feedback, make goals with the counselor to work on progress.

End of Role Play Session 2 Next Building Session 3

Session 3 • When is session 3 completed? – First adherence follow-up appt. • Which tools are used? – Session guide, Adherence Plan • Content covered in: Adherence Steps 10 -12 • Planning for trips • Dealing with substance use • Communicating with Treatment Team

Session 3 Role play • Go into pairs • Different pairs from those in Day 1 • Each person should get a chance to be the counselor – Session 3 lasts approx. 20 mins

Day 2 Feedback • What are your overall thoughts on the sessions practiced today (session 2 and 3)? • Did you like the structured session plan? • What would you do differently?

Day 2 complete!

Welcome to Day 3

Recap of Day 2

Session 4 • When is session 4 completed? – Final adherence follow-up appt. • Which tools are required? – Session guide, Adherence Plan, Flipchart • Content covered in: Adherence Steps 13 -14 • Preventing any future problems with taking treatment • Education on Viral Load • Continuation Phase (TB)

Session 4 Role play • Go into pairs • Different pairs from those in Day 1 • Each person should get a chance to be the counselor – Session 4 lasts approx. 20 mins

Feedback • What are your overall thoughts on the sessions practiced today (session 4) ? • Did you like the structured session plan? • What would you do differently?

Recap! • How many sessions are in the model? • What is the order of the sessions? • Name 4 adherence steps • What are the ABCs of Adherence? • Name tools!
Recap: patient flow How are they referred to counseling What can we do to make sure they come to counseling? How do patients move in your facility? Counseling is IMPORTANT
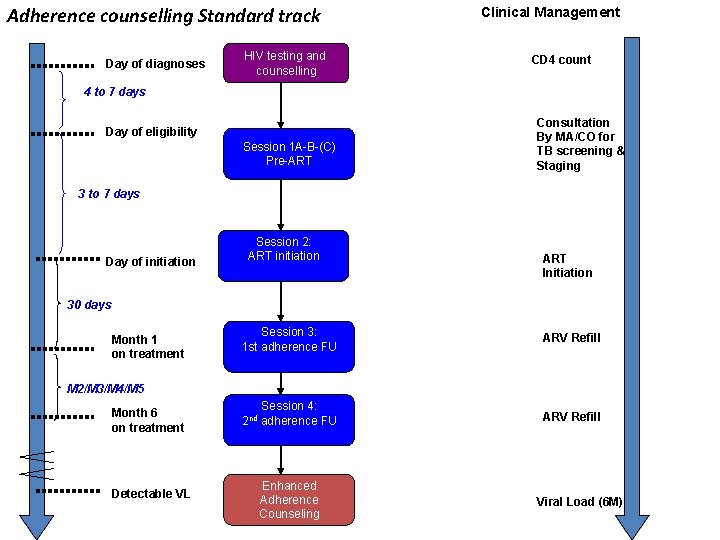
Adherence counselling Standard track Day of diagnoses HIV testing and counselling Clinical Management CD 4 count 4 to 7 days Day of eligibility Session 1 A-B-(C) Pre-ART Consultation By MA/CO for TB screening & Staging 3 to 7 days Day of initiation Session 2: ART initiation ART Initiation 30 days Month 1 on treatment Session 3: 1 st adherence FU ARV Refill Session 4: adherence FU ARV Refill M 2/M 3/M 4/M 5 Month 6 on treatment Detectable VL 2 nd Enhanced Adherence Counseling Viral Load (6 M)

Role Play Session 1 to 4

Day 3 complete!

Welcome to Day 4!

Brainstorm! What is the most important information a pregnant patient should learn and know about HIV?

Review our PMTCT Guidelines

Key messages for PMTCT • Start ART early! • Breast is still best! Exclusive breastfeeding for first 6 months • Give your baby ARVs after birth • Deliver in a health facility • Stay on ART for life to protect mom, baby and partner!

Questions?
- Slides: 64