Artificial Blood The blood of the future JongHwan

Artificial Blood The blood of the future Jong-Hwan Lee, M. D. Dept. of Anesthesiology & Pain Medicine Dong-A Univ.

Synonym Artificial Blood ¡ Synthetic Blood ¡ Blood Substitute ¡ Oxygen Carrier ¡ ¡ More exactly. . . Oxygen therapoutics Red Blood cell substitutes Cell-free oxygen carreirs

The History of Artificial Blood ¡ Milk was one of the first substances used as a blood substitute in order to treat patients with Asiatic cholera. ¡ After several patients died by receiving milk transfusions, other substances were discovered as potentials: l Salt or saline solutions: used primarily as a plasma volume expander, rather than as artificial blood l Hemoglobin isolated from red blood cells l Animal plasma could be used as a substitute for human blood ¡ However, since many of the materials in animal plasma are toxic to humans, this posed a problem to using it as a substitute ¡ The problem of not having a workable substitute led to Ringer’s Solution…

History 1628: William Harvey describes the circulatory system 1600 s: Sheep's blood suggested for wounded soldiers 1795: first successful human-to-human transfusion mid 1870’s: experiments with alternatives to human blood - milk from cows, goats, humans; severe reactions. 1884: 0. 9% normal saline transfused 1901: Karl Landsteiner discovers A, B, O blood groups 1907: typing/crossmatching of donors and recipients utilized 1937: Amberson experiments with bovine hemoglobin in saline solution transfusion to animals 1939: Rh blood group discovered 1943: first recorded case of transfusion-transmitted hepatitis 1949: Amberson used experimental hemoglobin-saline solution to treat severe postpartum hemorrhage after supplies of compatible banked blood were exhausted; patient died of renal failure

History 1959: molecular structure of hemoglobin determined by Max Perutz 1966: report of mice immersed in a perfluorocarbon liquid saturated with oxygen; mice survived up to 10 minutes 1978: first clinical trial of HBOCs: Savitsky infuses stroma-free hemoglobin solution to normal human volunteers, resulting in significant systemic toxicity 1985: risk of HIV infection from 1 unit of transfused blood is 1 in 2, 500 in the US 1985: US Army and Baxter begin program to develop red blood cell substitute, eventually called Hem. Assist 1989: Fluosol-DA (Green Cross Corp. , Japan) FDA approved for use during angioplasty 1994: Fluosol-DA withdrawn from market 1996: Perftoran (Perftoran, Russia) approved in Russia for use in severe anemia, hemorrhagic/traumatic shock, cerebral ischemia, cardiac surgery

History 1998: Hem. Assist (Baxter) Phase III trial suspended for use in traumatic/hemorrhagic shock, elective surgery 1998: Oxyglobin approved by US FDA for anaemia in dogs 1999: Oxyglobin approved by EU EMEA for anaemia in dogs 2001: Hemopure (Biopure) approved in South Africa for acutely anemic adult surgical patients 2001: Oxygent (Alliance Corp. ) Phase III cardiac surgery study terminated early 2001: Oxygent (Alliance Corp. ) Phase III European study completed for use in acute normovolemic hemodilution in elective noncardiac surgery

History 2002: Biopure filed biologic license application (BLA) with the FDA to market Hemopure in the US 2003: Hemolink (Hemosol) Phase IIb cardiac surgery trial suspended 2004: PHP (Curacyte) Phase IIc clinical trial completed for treatment of distributive shock 2005: Poly. Heme (Northfield Laboratories) is in Phase III trial for prehospital treatment of severely injured bleeding trauma patients
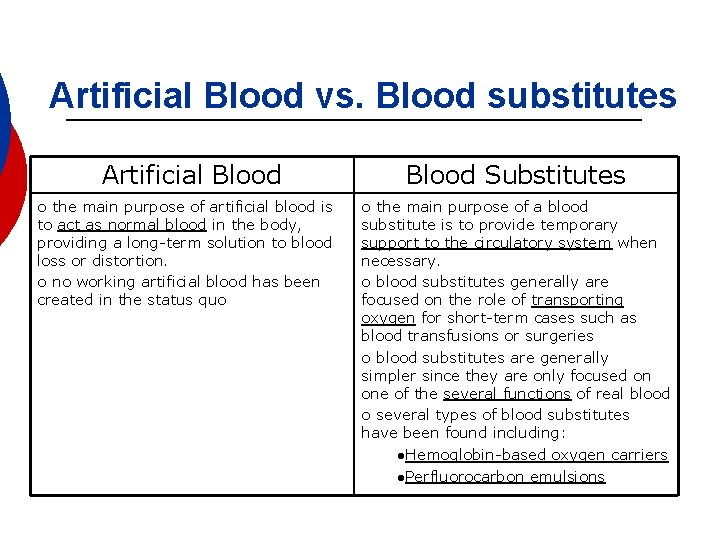
Artificial Blood vs. Blood substitutes Artificial Blood ¡ the main purpose of artificial blood is to act as normal blood in the body, providing a long-term solution to blood loss or distortion. ¡ no working artificial blood has been created in the status quo Blood Substitutes ¡ the main purpose of a blood substitute is to provide temporary support to the circulatory system when necessary. ¡ blood substitutes generally are focused on the role of transporting oxygen for short-term cases such as blood transfusions or surgeries ¡ blood substitutes are generally simpler since they are only focused on one of the several functions of real blood ¡ several types of blood substitutes have been found including: l. Hemoglobin-based oxygen carriers l. Perfluorocarbon emulsions
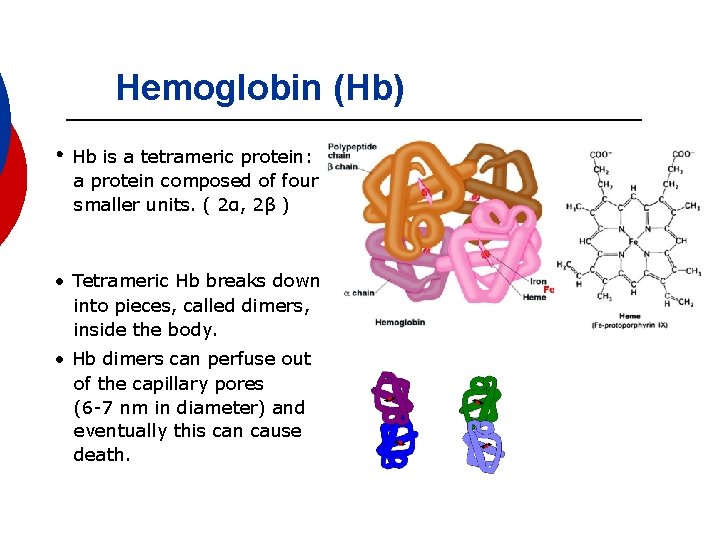
Hemoglobin (Hb) • Hb is a tetrameric protein: a protein composed of four smaller units. ( 2α, 2β ) • Tetrameric Hb breaks down into pieces, called dimers, inside the body. • Hb dimers can perfuse out of the capillary pores (6 -7 nm in diameter) and eventually this can cause death.
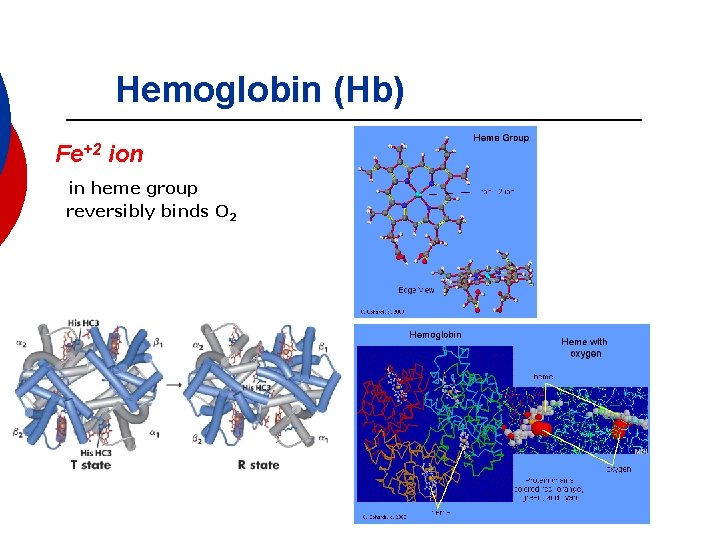
Hemoglobin (Hb) Fe+2 ion in heme group reversibly binds O 2
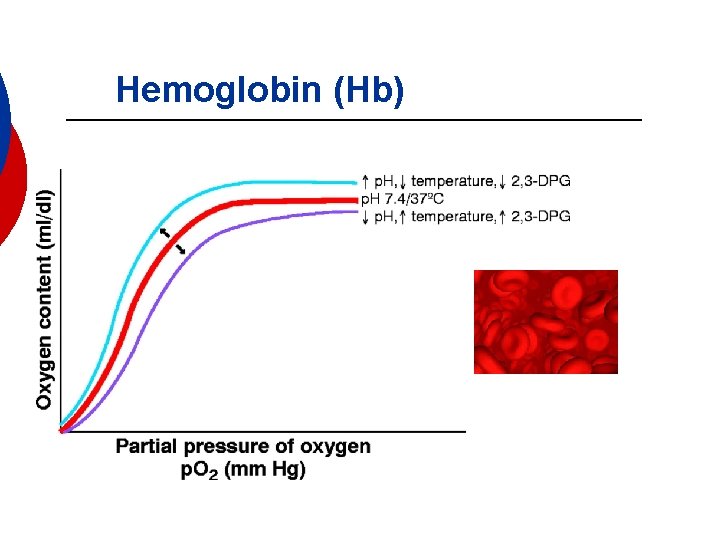
Hemoglobin (Hb)

What substitures are we developing? Approach Biomimetic Abiotic Theme of research Basis for substitute development Substitute type Mimicking nature's way of delivering Producing injectable fluids oxygen to based on chemically-modified the body's products of Haemoglobin (Hb) tissues Hb-based Substitute Use of totally synthetic Producing injectable emulsions chemicals to of compounds known as deliver perfluorochemicals (PFCs) oxygen to the tissues PFC-based Substitute

What constitutes a suitable substitute? 1. Adequate oxygen uptake in the lungs 2. Adequate oxygen delivery to the tissues 3. Long circulation time 4. Non-toxic 5. Rapidly excreted without causing harm 6. Stable at room temperature and readily available for use 7. Easily sterelisable (i. e. easy to ensure absence of pathogens such as viruses) 8. Cheap to manufacture 9. Long shelf life and easy to store 10. Widely applicable (i. e. no need for crossmatching or compatibility testing) 11. Free of any side effects

Types of Blood Substitutes ¡ Perfluorocarbon(PFC)-based oxygen carriers ¡ Hemoglobin-based oxygen-carrying solutions(HBOC’s) 1. Polymerization 2. stabilization 3. conjugation 4. hybridization 5. encapsulation
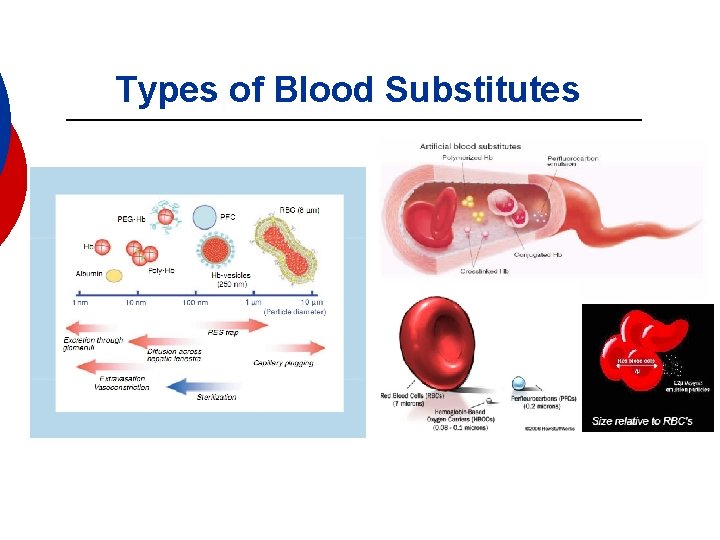
Types of Blood Substitutes

What is the Perfluorocarbons?
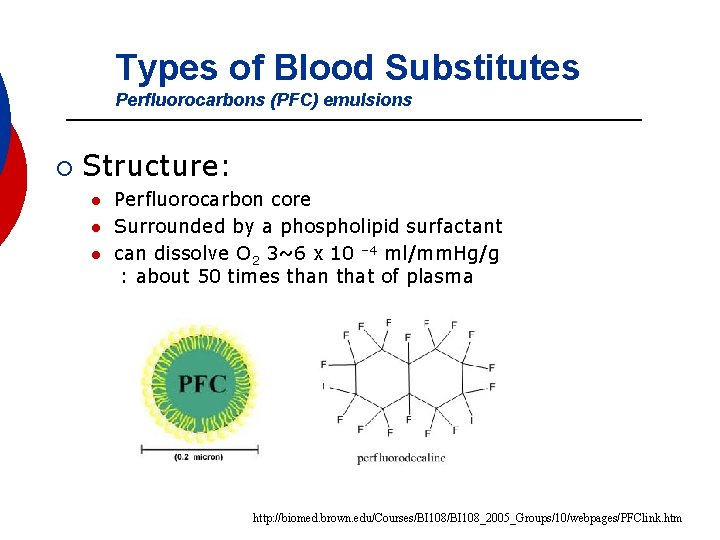
Types of Blood Substitutes Perfluorocarbons (PFC) emulsions ¡ Structure: l l l Perfluorocarbon core Surrounded by a phospholipid surfactant can dissolve O 2 3~6 x 10 – 4 ml/mm. Hg/g : about 50 times than that of plasma http: //biomed. brown. edu/Courses/BI 108_2005_Groups/10/webpages/PFClink. htm

Types of Blood Substitutes Perfluorocarbons (PFC) emulsions ¡ ¡ Perfluorocarbons are derived from a group of hydrocarbons in which the hydrogen atoms are replaced by fluorine atoms. l PFCs are chemically inert due to the strength of the carbon-fluorine bonds Used to create artificial blood during surgeries Process of production: l Water, salts, and phospholipids surfactant are added and emulsified through high-pressure homogenization l Purified through high temperatures of steam. Common PFCs: l Perfluorodecalin(C 10 F 18) : Fluosol, Perftoran l Perfluorooctyl bromide (C 8 F 17 Br) : Perflubron l Perfluorodichorotane (C 8 F 16 C 12)
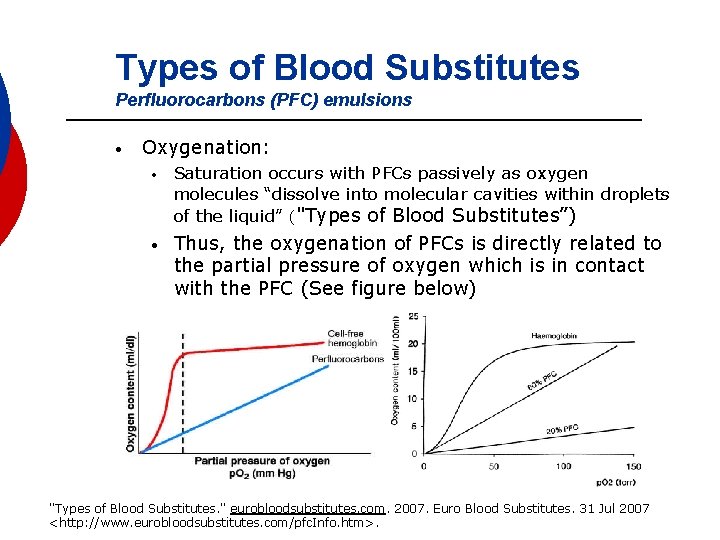
Types of Blood Substitutes Perfluorocarbons (PFC) emulsions • Oxygenation: • Saturation occurs with PFCs passively as oxygen molecules “dissolve into molecular cavities within droplets of the liquid” ("Types of Blood Substitutes”) • Thus, the oxygenation of PFCs is directly related to the partial pressure of oxygen which is in contact with the PFC (See figure below) "Types of Blood Substitutes. " eurobloodsubstitutes. com. 2007. Euro Blood Substitutes. 31 Jul 2007 <http: //www. eurobloodsubstitutes. com/pfc. Info. htm>.
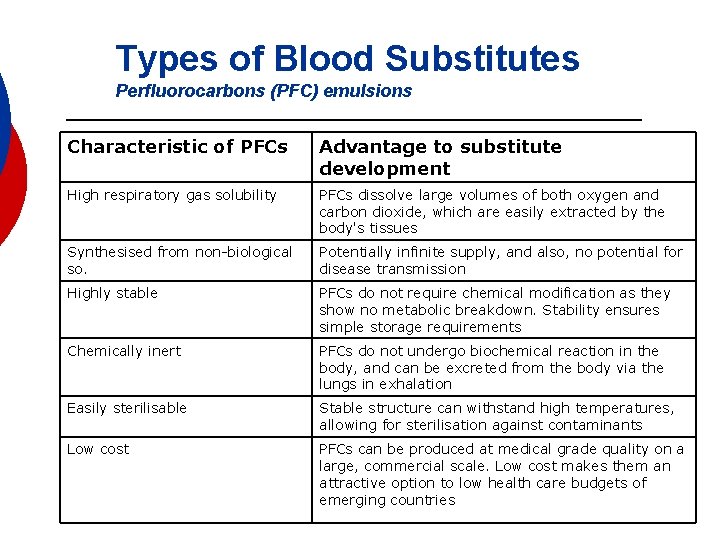
Types of Blood Substitutes Perfluorocarbons (PFC) emulsions Characteristic of PFCs Advantage to substitute development High respiratory gas solubility PFCs dissolve large volumes of both oxygen and carbon dioxide, which are easily extracted by the body's tissues Synthesised from non-biological so. Potentially infinite supply, and also, no potential for disease transmission Highly stable PFCs do not require chemical modification as they show no metabolic breakdown. Stability ensures simple storage requirements Chemically inert PFCs do not undergo biochemical reaction in the body, and can be excreted from the body via the lungs in exhalation Easily sterilisable Stable structure can withstand high temperatures, allowing for sterilisation against contaminants Low cost PFCs can be produced at medical grade quality on a large, commercial scale. Low cost makes them an attractive option to low health care budgets of emerging countries

Types of Blood Substitutes Perfluorocarbons (PFC) emulsions Advantages Disadvantages ¡ PFCs do not react with oxygen ¡ often causes flu-like symptoms. This is often caused by phagocytosis of the perfluorocarbon emulsion by the recipient the oxygen to the body they allow organism’s immune system increased solubility of oxygen in ¡ unable to remain mixed as aqueous plasma solutions – thus, they must be prepared ¡PFCs minimize the effects of factors as emulsions for use in patients ¡a decrease in blood platelet count like p. H and temperature in blood ¡ PFC products cannot be used by the circulation human body, and must be discarded this takes approximately 18 -24 months ¡ because PFCs absorb oxygen passively, patients must breathe at a linear rate to ensure oxygenation of tissues (Euro blood substitutes). ¡PFCs allow easy transportation of
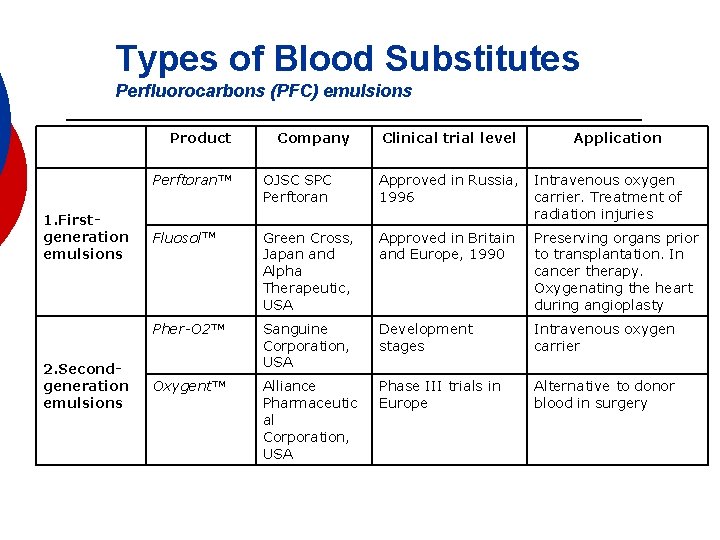
Types of Blood Substitutes Perfluorocarbons (PFC) emulsions Product 1. Firstgeneration emulsions 2. Secondgeneration emulsions Company Clinical trial level Application Perftoran. TM OJSC SPC Perftoran Approved in Russia, Intravenous oxygen 1996 carrier. Treatment of radiation injuries Fluosol. TM Green Cross, Japan and Alpha Therapeutic, USA Approved in Britain and Europe, 1990 Preserving organs prior to transplantation. In cancer therapy. Oxygenating the heart during angioplasty Pher-O 2 TM Sanguine Corporation, USA Development stages Intravenous oxygen carrier Oxygent. TM Alliance Pharmaceutic al Corporation, USA Phase III trials in Europe Alternative to donor blood in surgery
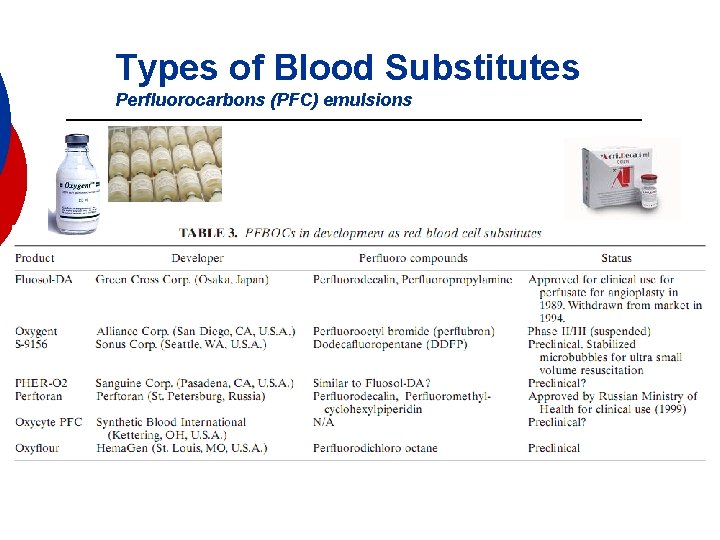
Types of Blood Substitutes Perfluorocarbons (PFC) emulsions

Dying for Lack of Blood ¡ ¡ ¡ ¡ Emily Gruszka was dying for lack of blood in 1999 despite 45 days of continuous RBC transfusion Kidneys stopped working; on the verge of multi organ failure But blood couldn’t save her because of severe autoimmune hemolytic anemia Her doctor read about Oxyglobin in a pet magazine, then requested Biopure for 11 units of Hemopure Hours after first transfusion, she stabilized and was maintained for 8 days until immune system was controlled She survived at a hematocrit of 3%+ New Engl J Med. 2000; 342(22): 1638 -1643
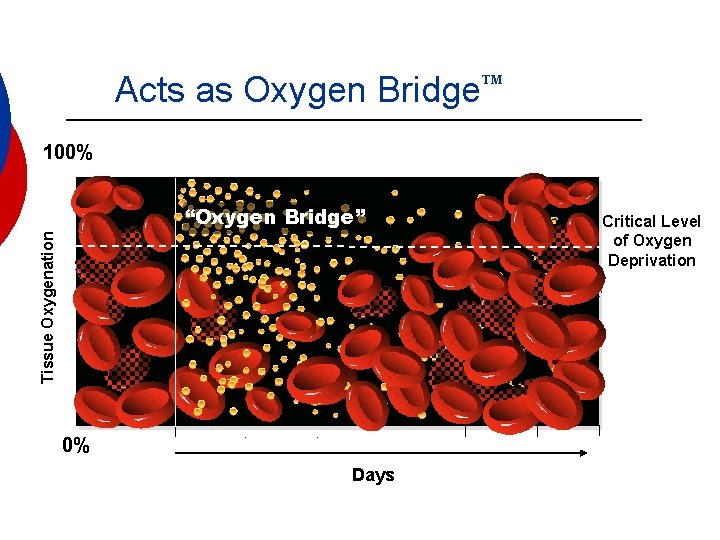
Acts as Oxygen Bridge 100% Tissue Oxygenation “Oxygen Bridge” 0% Days Critical Level of Oxygen Deprivation



What is the HBOC?

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ ¡ Hemoglobin-based Oxygen Carriers were created as a mechanism to mimic the oxygen-carrying role of hemoglobin in the body, while still reducing the need for real human hemoglobin. Hemoglobin is a tetramer with two alpha and two beta polypeptide chains; each is bound to an iron heme group which successively binds to an oxygen molecule • Hemoglobin’s heme bond allows it to have a higher affinity for oxygen, thus making it an excellent source of blood substitutes. (Goorha et al 46). Advantages Disadvantages ¡Available in much larger quantities ¡ reduced circulation half-life ¡Can be stored for long durations ¡Can be administered rapidly without typing or cross-matching blood types ¡Can be sterilized via pasteurization ¡ disrupts certain physiological structures, especially the gastrointestinal tract and normal red blood cell hemoglobin. ¡ the release of free radicals into the body
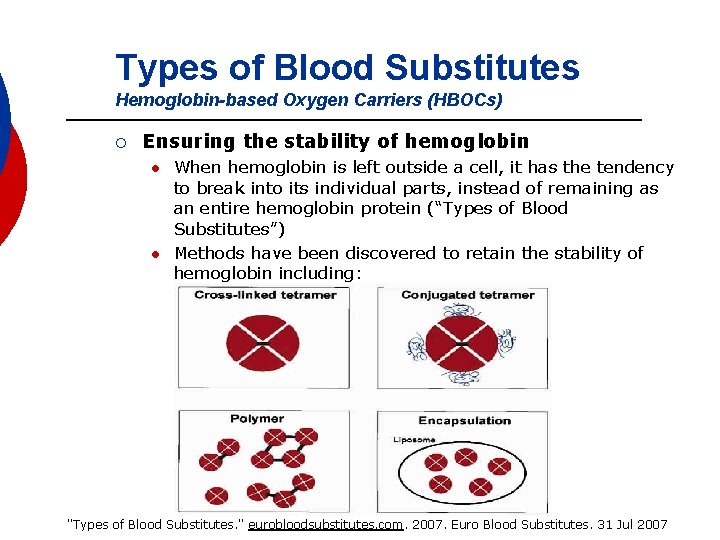
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ Ensuring the stability of hemoglobin l l When hemoglobin is left outside a cell, it has the tendency to break into its individual parts, instead of remaining as an entire hemoglobin protein (“Types of Blood Substitutes”) Methods have been discovered to retain the stability of hemoglobin including: "Types of Blood Substitutes. " eurobloodsubstitutes. com. 2007. Euro Blood Substitutes. 31 Jul 2007
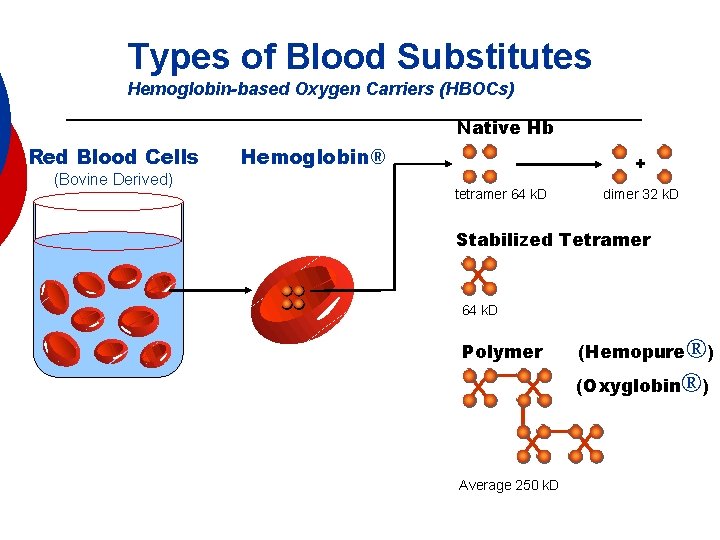
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) Native Hb Red Blood Cells (Bovine Derived) Hemoglobin® + tetramer 64 k. D dimer 32 k. D Stabilized Tetramer 64 k. D Polymer (Hemopure®) (Oxyglobin®) Average 250 k. D
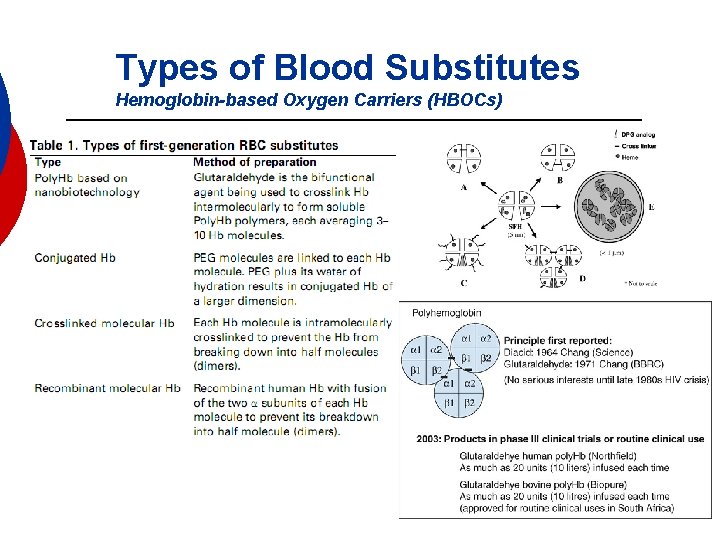
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs)
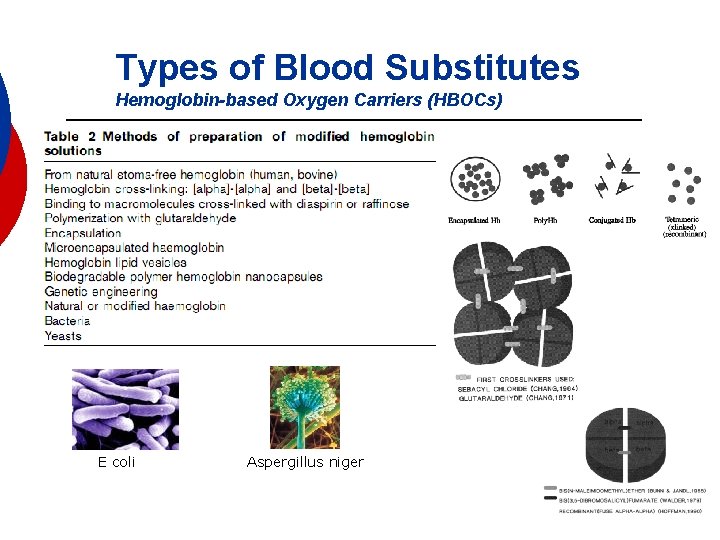
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) E coli Aspergillus niger

Why HBOCs? Preoperative EPO • Repeated office visits • Failure rate @ 5% • Iron Preoperative Autologous Donation (PAD) • Collection • Transport • Risk of errors • Old RBCs (>15 Days) • Certain conditions precluded; HIV, hep. C • 45% wasted General Benefits of HBOCs Intraoperative Cell Salvage • Equipment • Disposable • Technician • Small recovery vol. Acute Normovolemic Hemodilution (ANH) • Extra time • Risk of anemia • • • No prior planning Faster & better O 2 Del Ready to use No waste No equipment Long shelf life No refrigeration Universally compatible No clerical errors Immediately offloads oxygen (No 2, 3 -DPG) • Can use Jehovah’s patients

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ First-generation RBC substitutes : simply an oxygen-carrier based on the use of modified Hb without the presence of RBC enzymes or membrane ¡ Second-generation RBC substitutes : more than an oxygen carrier : incorporate modified Hb with RBC antioxidant enzymes ¡ Third-generation RBC substitutes : closer to RBCs : contain Hb and all of the enzymes of RBCs

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs)
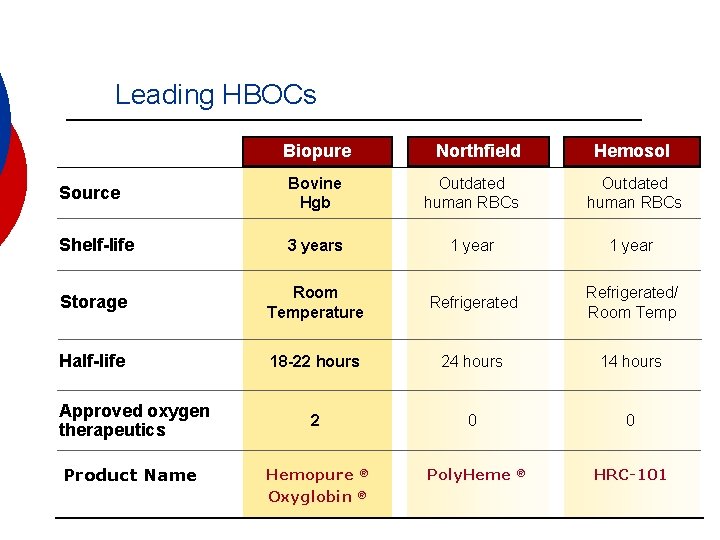
Leading HBOCs Biopure Northfield Hemosol Source Bovine Hgb Outdated human RBCs Shelf-life 3 years 1 year Storage Room Temperature Refrigerated/ Room Temp Half-life 18 -22 hours 24 hours 14 hours 2 0 0 Hemopure ® Oxyglobin ® Poly. Heme ® HRC-101 Approved oxygen therapeutics Product Name
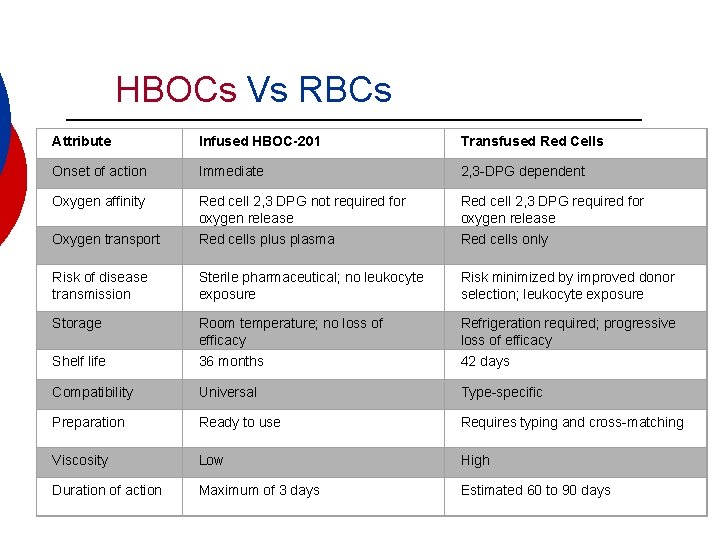
HBOCs Vs RBCs Attribute Infused HBOC-201 Transfused Red Cells Onset of action Immediate 2, 3 -DPG dependent Oxygen affinity Red cell 2, 3 DPG not required for oxygen release Red cell 2, 3 DPG required for oxygen release Oxygen transport Red cells plus plasma Red cells only Risk of disease transmission Sterile pharmaceutical; no leukocyte exposure Risk minimized by improved donor selection; leukocyte exposure Storage Room temperature; no loss of efficacy Refrigeration required; progressive loss of efficacy Shelf life 36 months 42 days Compatibility Universal Type-specific Preparation Ready to use Requires typing and cross-matching Viscosity Low High Duration of action Maximum of 3 days Estimated 60 to 90 days

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) Goorha, Brig, and Maj Deb. "Artificial Blood. " MJAFI 59(2003): 45 -49.

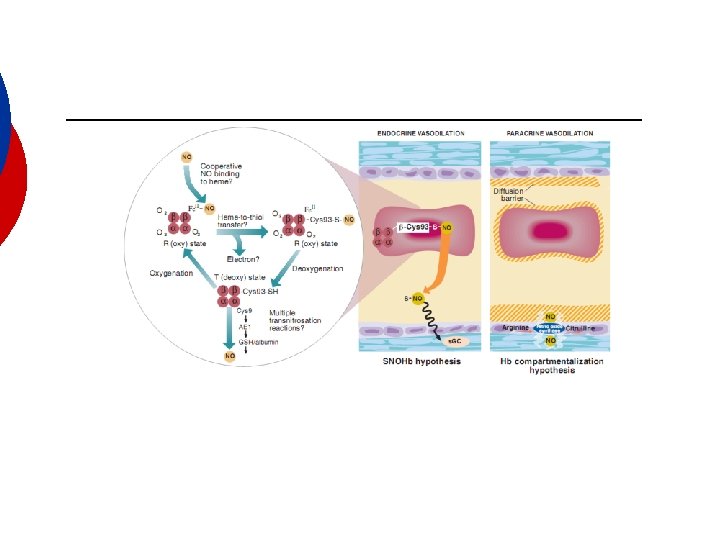
HBOC Associated Clinical Side Effects: 1. Vasoactivity – vasoconstriction effects. As nitric oxide bind to hemoglobin, nitric oxide becomes less available to cause vascular smooth muscle relaxation. Hence vasoconstricition occurs. 2. Hemostasis – Studies have shown an increased hemostatic effect in HBOCs due to reversal of the inhibition effect of nitric oxide on platelet aggregation. 3. Gastrointestinal side effects – Studies have observed gastrointestinal side effects such as nausea, vomiting, diarrhea, and bloating. The binding of nitrous oxide to gastrointestinal intestine tissues is the proposed cause.
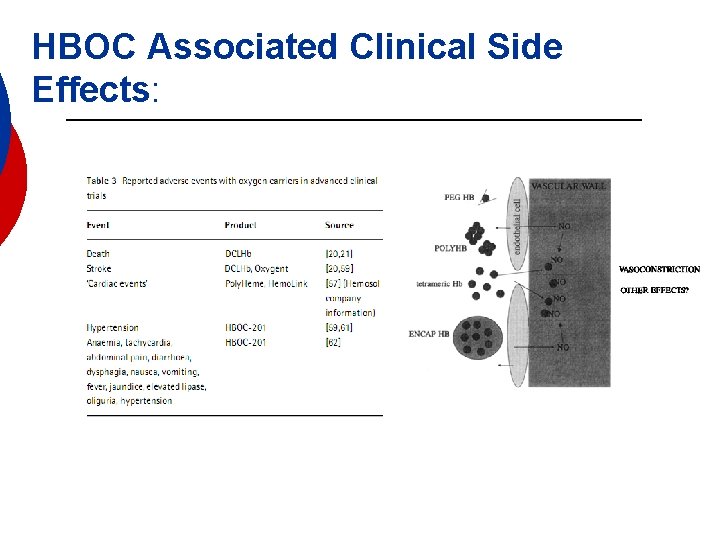
HBOC Associated Clinical Side Effects:
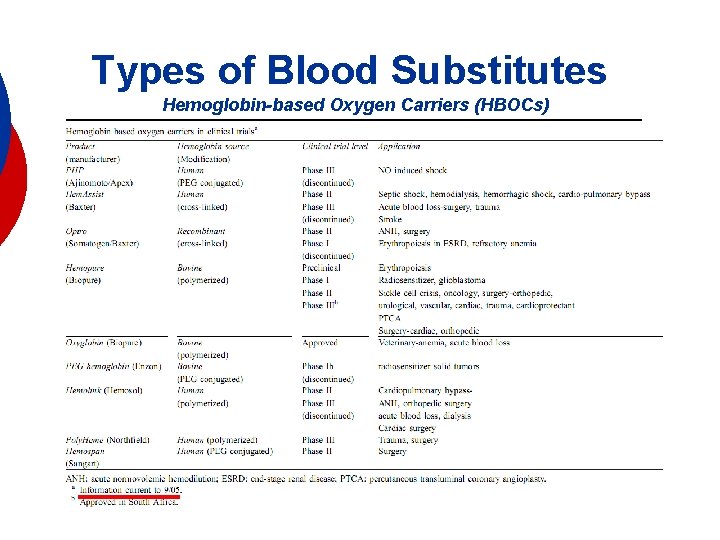

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs)
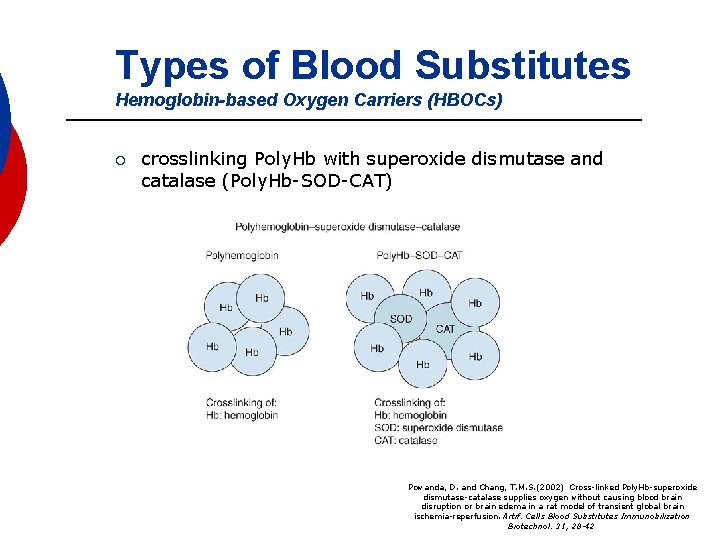
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ crosslinking Poly. Hb with superoxide dismutase and catalase (Poly. Hb-SOD-CAT) Powanda, D. and Chang, T. M. S. (2002) Cross-linked Poly. Hb-superoxide dismutase-catalase supplies oxygen without causing blood brain disruption or brain edema in a rat model of transient global brain ischemia-reperfusion. Artif. Cells Blood Substitutes Immunobilization Biotechnol. 31, 28 -42

Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ ¡ Currently, experimentation is occurring to develop vesicles which carry the Hemoglobin before inserting it into the body as an HBOC There are several advantages to HBOC carrier vesicles • • ¡ Prevents the denaturation of the Hemoglobin The vesicles themselves are made of purified Hb and lipids, making them compatible with the human immune system Current Setbacks with Hb Vesicle Technology • • • Materials such as nylon, gelatin, and gum arabic have been tried but the human immune system, specifically the reticuloendothelial system, removed the vesicle promptly as a natural bodily response. Later, theory of phospholipid vessels was used to create a vesicle using phospholipids Researchers are trying to develop a way to create liposome sacks to carry the HBOCs (Goorha et al)
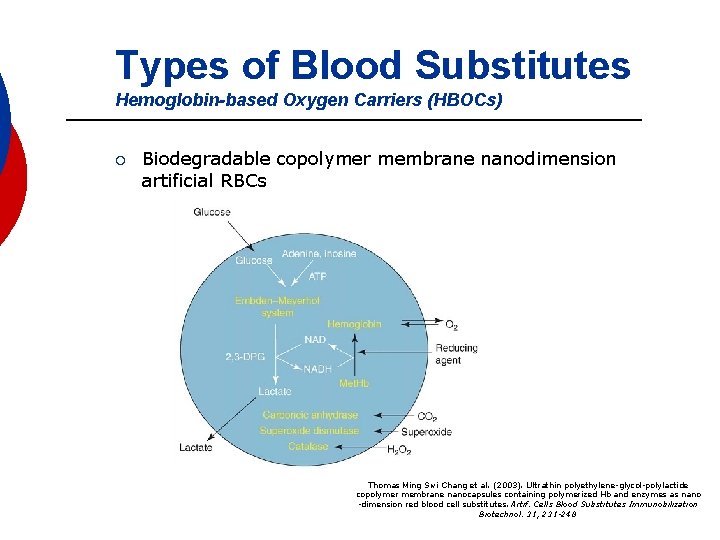
Types of Blood Substitutes Hemoglobin-based Oxygen Carriers (HBOCs) ¡ Biodegradable copolymer membrane nanodimension artificial RBCs Thomas Ming Swi Chang et al. (2003). Ultrathin polyethylene-glycol-polylactide copolymer membrane nanocapsules containing polymerized Hb and enzymes as nano -dimension red blood cell substitutes. Artif. Cells Blood Substitutes Immunobilization Biotechnol. 31, 231 -248
Types of Blood Substitutes ¡ Hemo. Bio Tech : Hemo. Tech blood : reduce the clotting and narrowing of the artery
Types of Blood Substitutes ¡ Dendritech Corporation : water-soluble dendrimers : highly fluorinated water soluble nano-polymers

Artificial Plastic Blood ¡ Dr. Lance Twyman (2007. 5. 12) : combing a porphyrin with monomers that build together in a hyper-branching or tree-like structure : Polymer-porphyrin system : Hyperbranched polymer based on 3, 5 -diacetoxybenzoic acid, starting with tetrakis(4 -acetoxyphenyl) porphyrin as the core : porphyrin core for iron to bind and release oxygen : similar to Hb in size and shape : a dark red water-soluble paste with consistency of honey ¡ The advantage of this system over a dendritic system with similar structure is that the polymer can be made in one step.
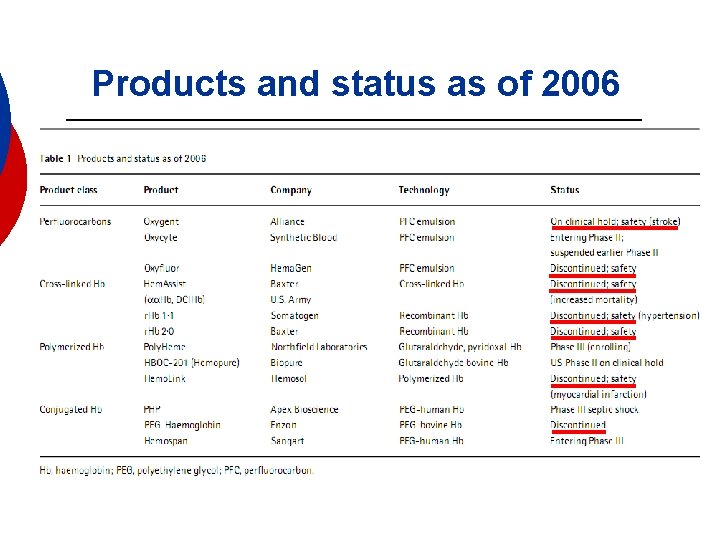
Products and status as of 2006

Products and status as of 2006 ¡ Poly. Heme Lawsuit (Fabruary 22, 2006) : Northfield Laboratories, Inc : Heart attacks within 7 days in 10 of 81 patients


Potential clinical applications of oxygen carrying solutions 1. Thearpy (a) Blood substitutes : hemorrhagic shoc; hemorrhage; anemia (b) Whole-body rinse out : acute drug intoxication; acute hepatic failure (c) Local ischemia : acute MI; evolving MI; cardiac failure; brain infarction; acute arterial thrombosis and embolism; PTCA of coronary artery (d) General ischemia : gas embolism; CO intoxication; HAPO; HACO (e) Aid for organ recovery : acute renal failure; acute hepatic failure; acute pancreatitis (f) Infectious disease : anaerobic and aerobic disease (g) Adjuvant therapy : tumor radiotherapy; chemotherapy 2. Perfusional protection of organs during surgery – cardiopulmonary bypass, deep hypothermia, circulatory arrest, cardioplegia 3. Preservation of donor organ 4. Drug carrier – drug-conjugated haemoglobin and perfluorochemicals 5. Contrast agent – (Perfluoro-octylbromide) Non-Clinical Applications 1. Culture medium 2. Chemical examination – oxygen sensor, standard solution for oxygen calibrator 3. Bioreactor Paradoxical Utilisations (of high-oxygen affinity) 1. Oxygen absorbent 2. Oxygen pulse therapy for malignant tumors in combination with radiotherapy or chemotherapy


2008년 SABM annual meeting

The End
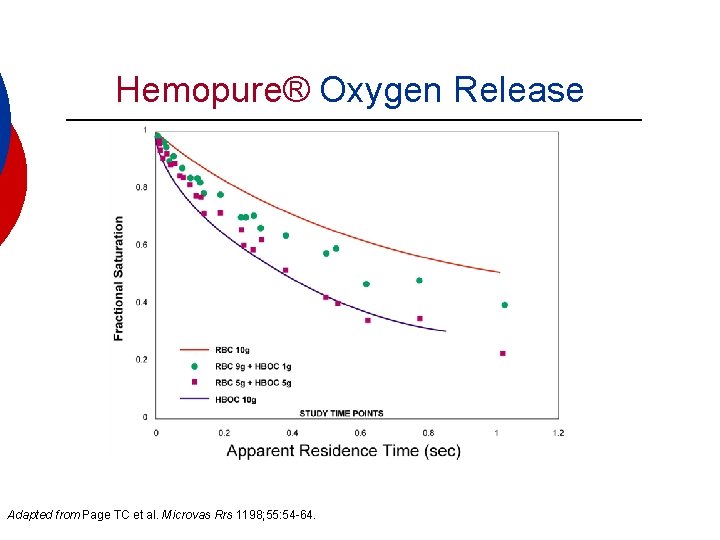
Hemopure® Oxygen Release Adapted from Page TC et al. Microvas Rrs 1198; 55: 54 -64.
- Slides: 58