ARRHYTHMIAS Jamil Mayet Arrhythmias learning objectives Mechanisms of

ARRHYTHMIAS Jamil Mayet

Arrhythmias - learning objectives – Mechanisms of action of antiarrhythmic drugs – Diagnosis • To differentiate the different types of SVTs on the ECG • To diagnose ventricular tachyarrhythmias from the ECG • To differentiate different bradyarrhythmias from the ECG – Treatment • Understand different options; drugs versus ablation; pacing • Importance of anticoagulation in atrial fibrillation • Appreciate increasing use of ICDs

Tachyarrhythmias • Antiarrhythmic drugs – Vaughn-Williams Classification – Drugs divided according to EP effects on cells – All are negatively inotropic – Can also be pro-arrhythmic

Tachyarrhythmias • Class I – Impede Na transport across cell membrane – Ia increase AP duration eg quinidine, disopyramide, procainamide – Ib shorten AP duration eg lignocaine, mexilitene, propafenone – Ic little effect on AP eg flecainide

Tachyarrhythmias • Class II – Interfere with effects of SNS on the heart eg beta blockers • Class III – Prolong AP duration but do not effect initial Na dependent phase eg sotalol, amiodarone • Class IV – Antagonise Ca transport across cell membrane – SA and AV node particularly susceptible eg verapamil, diltiazem

Supraventricular arrhythmias • Atrial fibrillation – Rapid atrial discharge (350 -600/min) – AV node cannot conduct all impulses – Cardioversion (electrical or drugs) can restore SR – Class Ia, Ic, III drugs may maintain SR – Px often rate control and stroke prevention – Rate control with digoxin, class II, IV drugs – Anticoagulation with warfarin in most cases – Causes include ht, ischaemia, rheumatic hd, alcohol, thyrotoxicosis, cardiomyopathy, PTE, thoracotomy, idiopathic (“lone”)
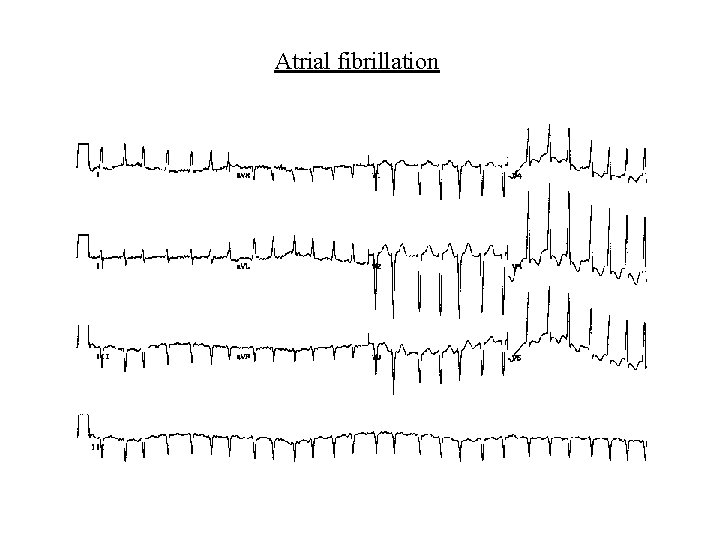
Atrial fibrillation

Supraventricular arrhythmias • Atrial flutter – Rapid atrial discharge (250 -350/min) – Occasional 1: 1 conduction – More often 2: 1, 3: 1, 4: 1 conduction – Diagnosis aided by increasing block eg CSM, adenosine – Cardioversion (electrical or drugs) can restore SR – Class Ia, Ic, III drugs may maintain SR – Rate control with digoxin, class II, IV drugs – ? Anticoagulation – Similar causes to atrial fibrillation
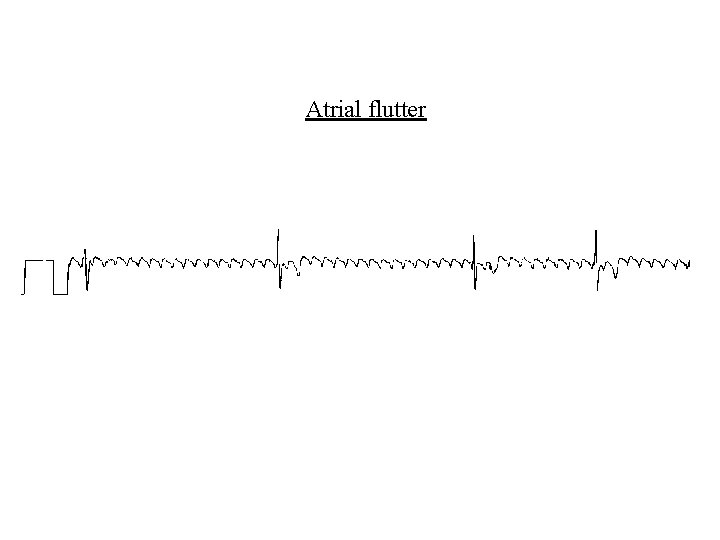
Atrial flutter
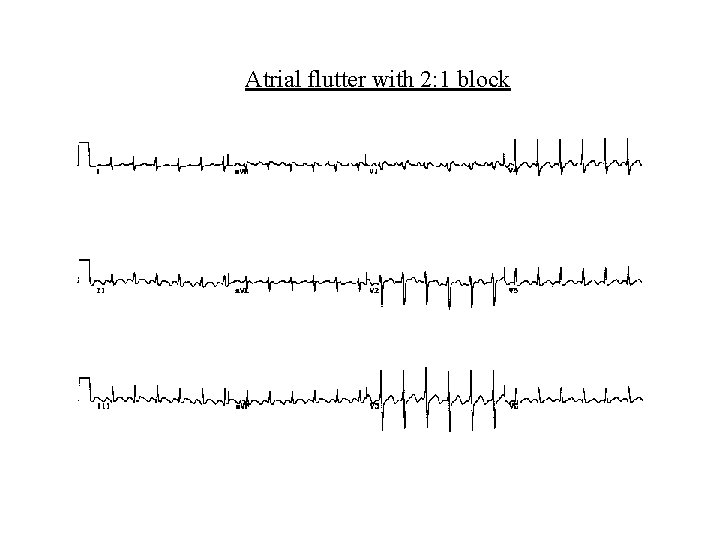
Atrial flutter with 2: 1 block

Supraventricular arrhythmias • Atrial tachycardia – Atrial discharge slower (120 -250/min) – Occasional 1: 1 AV node conduction – More usually 2: 1 conduction – With AV block often due to digitoxicity – Cardioversion (electrical or drug) can restore SR – Overdrive pacing is an alternative
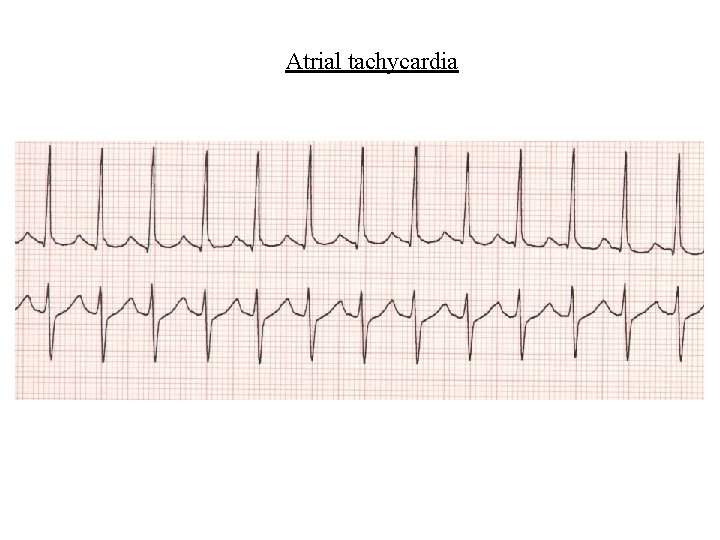
Atrial tachycardia

Supraventricular arrhythmias • AV nodal re-entry tachycardia – Re-entry circuit within AV node – Rate usually 130 -250/min – CSM or adenosine may terminate arrhythmia – Alternatives include cardioversion (electrical or drug) and overdrive pacing – Prophylaxis with class II, IV, III, Ia, Ic drugs
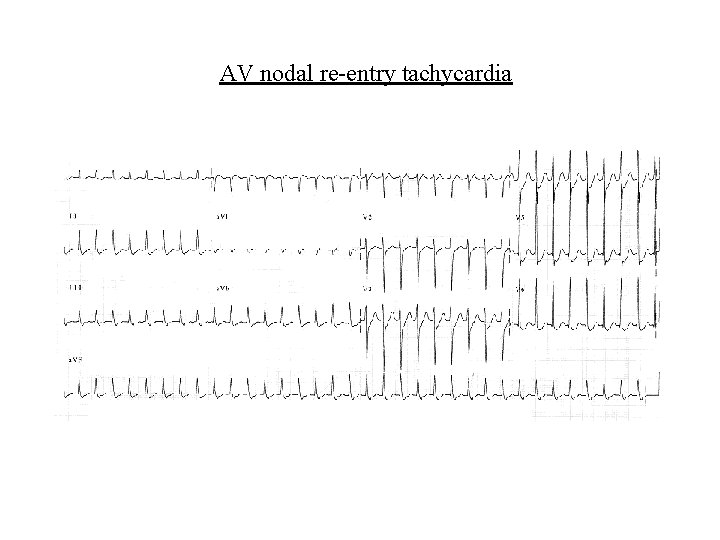
AV nodal re-entry tachycardia

Supraventricular arrhythmias • Pre-excitation syndromes – WPW syndrome due to accessory pathway (bundle of Kent) – 0. 15% of population – Accessory pathway allows rapid conduction – Resting ECG shows short PR and delta wave – May cause AV re-entry tachycardia – A fib may be dangerous due to rapid conduction

Supraventricular arrhythmias • Pre-excitation syndromes – Digoxin/verapamil may increase conduction in bundle of Kent and should be avoided – Class Ia, Ic and III drugs slow ventricular rate and may cardiovert to SR – Electrical cardioversion especially in fast A fib – Lown-Ganong-Levine syndrome: connection between atria and His bundle; short PR; no delta wave
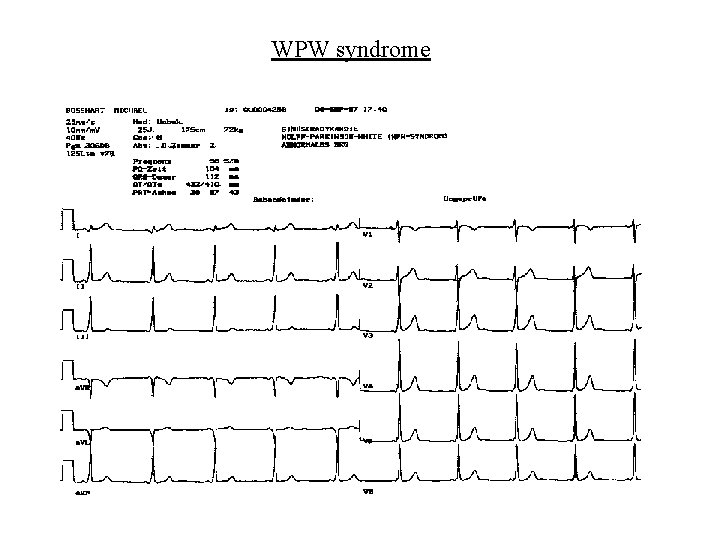
WPW syndrome

Ventricular arrhythmias • Ventricular tachycardia – Broad complex tachycardia – Independent atrial activity – Capture/fusion beats – Risk of degeneration to ventricular fibrillation – Cardioversion (electrical or drug) can restore SR – Overdrive pacing is an alternative – Idioventricular tachycardia; rate<120/min; often related to reperfusion in AMI; Px often unnecessary
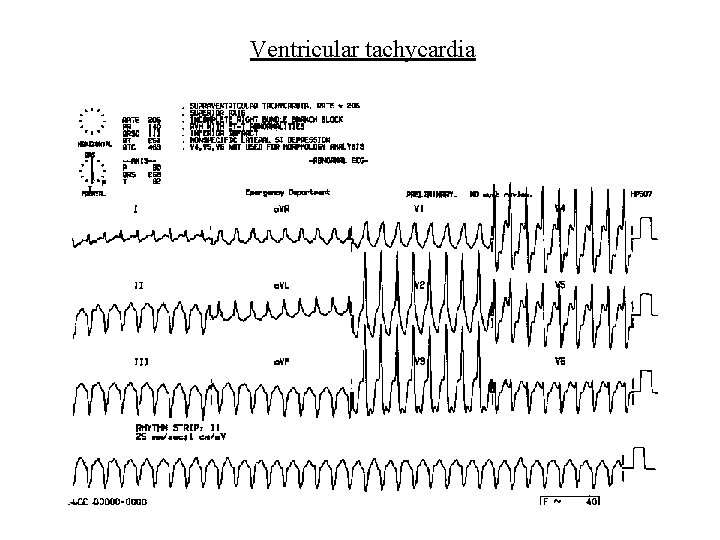
Ventricular tachycardia
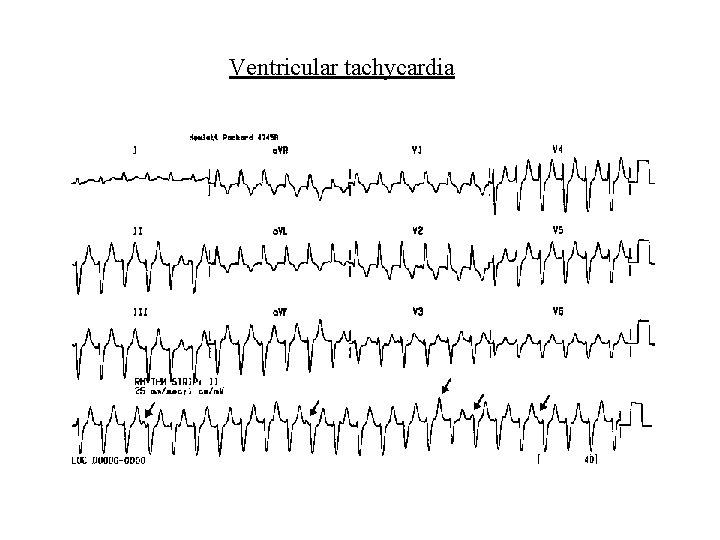
Ventricular tachycardia

Ventricular arrhythmias • Torsades de pointes – Twisting pattern – Precipitated by prolonged QT – May be congenital, metabolic or drug induced • Ventricular fibrillation – Death – Electrical cardioversion
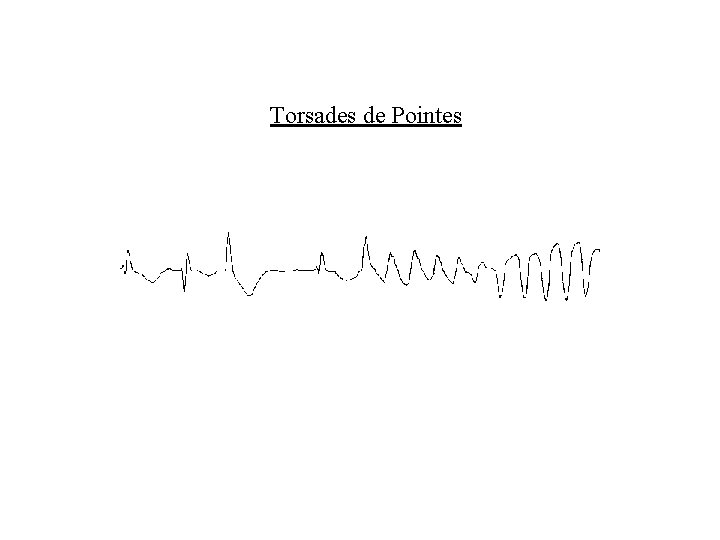
Torsades de Pointes
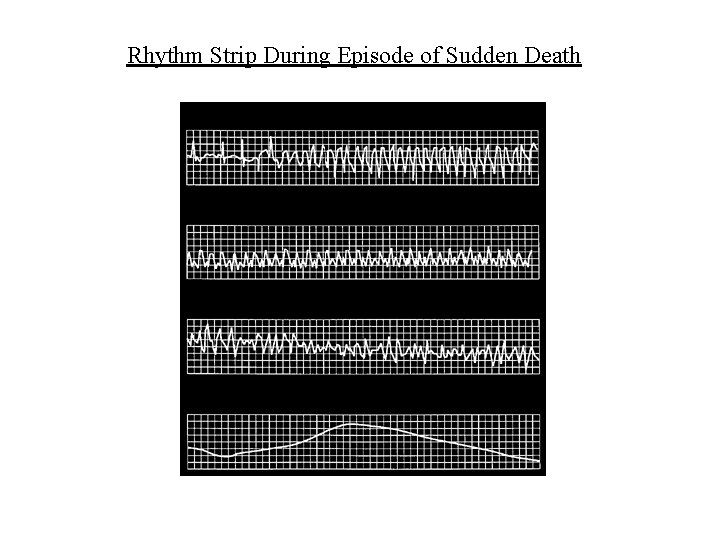
Rhythm Strip During Episode of Sudden Death

VT versus SVT with aberrant conduction • • History of IHD (VT) Age>60 (VT) Independent P wave activity (VT) Very broad QRS (>140 ms) (VT) Resting BBB of same morphology (SVT) Concordant QRS direction (V 1 -V 6) (VT) If in doubt assume VT

EP studies and ablation therapy • Diagnosis and curative treatment of AVNRT, AVRT (eg WPW) atrial tachy and atrial flutter • Potential curative treatment of VT • Stratification of risk in patients with VT – Guide need for implantable defibrillator insertion – Guide antiarrhythmic drug treatment • Potential for treatment of A fib

Implanatable defibrillators
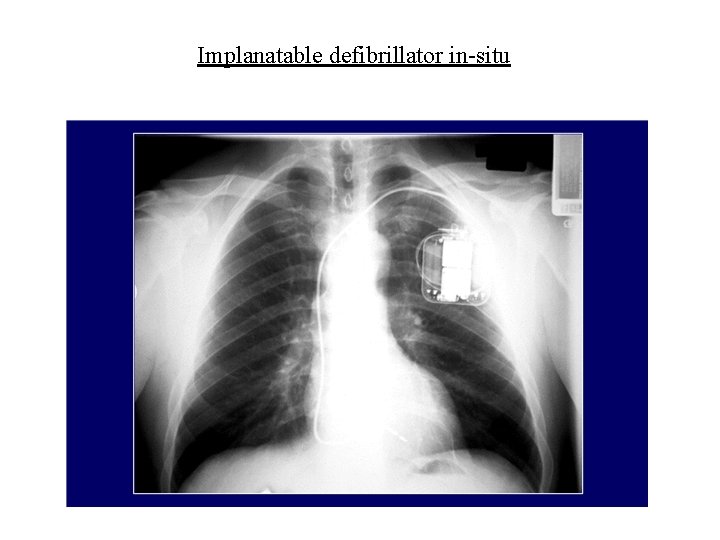
Implanatable defibrillator in-situ

Bradyarrhythmias • Sinus node disease – Bradycardias usually caused by idiopathic fibrosis, ischaemia or drugs • Tachy-brady syndrome – Combination of tachycardic and bradycardic episodes
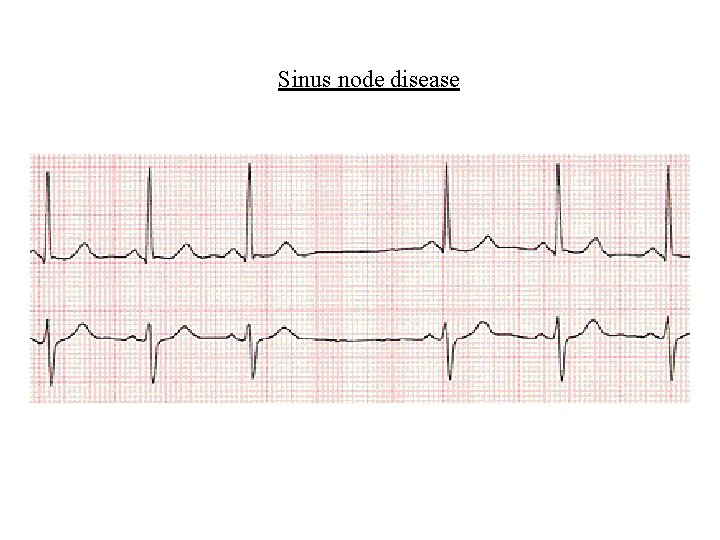
Sinus node disease

Bradyarrhythmias • AV node disease – 1 st degree; prolonged PR interval – 2 nd degree; Mobitz type I (Wenckebach); increasing PR interval then non-conducted P wave – 2 nd degree; Mobitz type II; non-conducted P waves – 2 nd degree; 2: 1 or 3: 1 AV node block – 3 rd degree; complete heart block • AV block usually caused by idiopathic fibrosis; other causes include MI, drugs and congenital block

AV node disease 1 st degree heart block 2 nd degree heart block (2: 1)
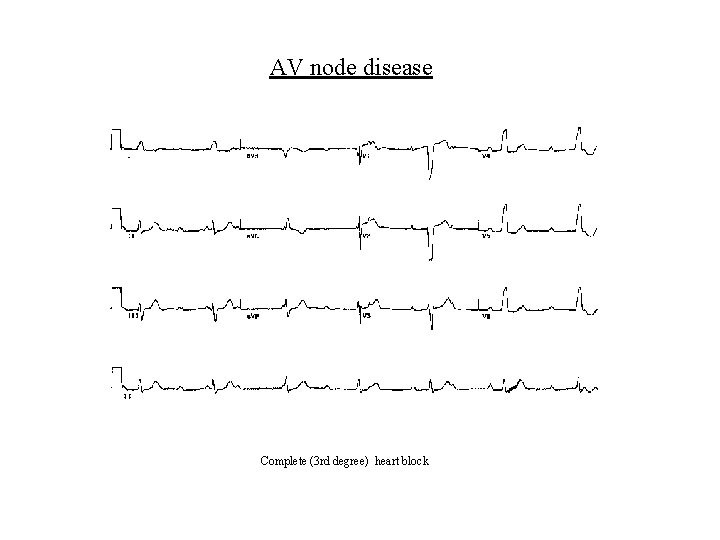
AV node disease Complete (3 rd degree) heart block

Bradyarrhythmias • Treatment of symptomatic bradyarrhythmias often consists of pacing • In the short-term drugs may be used to augment conduction eg atropine, isoprenaline
- Slides: 33