Are DCBs a Game Changer Kenneth Rosenfield MD

Are DCB’s a Game Changer Kenneth Rosenfield, MD, MHCDS, MSCAI Mass General Hospital, Boston

Kenneth Rosenfield, MD, MHCDS Conflicts of Interest • Consultant: Abbott Vascular, Cardinal Health; Sur. Modics; Cruzar Systems; Capture Vascular; Endospan; Micell; Silk Road; Valcare; Proteon; Univ. of Maryland • Grants/Contracts: Abbott Vascular; Atrium; Lutonix/BARD; NIH • Equity: Access Closure, Inc. ; Angio. Dynamics/Vortex; Jana. Care, Inc; PQ Bypass, Inc. ; Primacea; MD Insider • Personal Compensation: Cook • Board Member: VIVA Physicians, a not for profit 501 c 3 organization dedicated to advancing the field of vascular medicine and intervention through education and research (www. vivapvd. com)

What is a “Game-Changer”? Definition: • event, idea, or procedure that effects a significant shift in the current manner of doing or thinking about something

What does it take to be a “Game-Changer”? Vascular Intervention • PTA (Dotter) and PTCA (Greuntzig) • Fixed GW Coaxial GW motion monorail • Stent DES • Rotational atherectomy Imaging • IVUS, Cardiac CTA, Fractional Flow Structural • TAVR Healthcare Delivery models • ACA • AUC

Do DCB’s Qualify as a “Game-Changer”? 1. Fill unmet clinical need…accomplish something important that other technology cannot? 2. Good scientific basis 3. Results different from otherapies? How much improvement? 4. Impact important enough for patients? 5. Is effect long-lasting? 6. Lead to altered MD behavior?

1. Unmet clinical need… • 86 year-old female with AS status post TAVI, COPD, CHF and intermittent claudication. • Now reports left leg pain that occurs at night and is relieved by sitting up/dangling leg over side of bed (new rest pain/CLI) • No wounds/ulcers Rutherford category 4 6
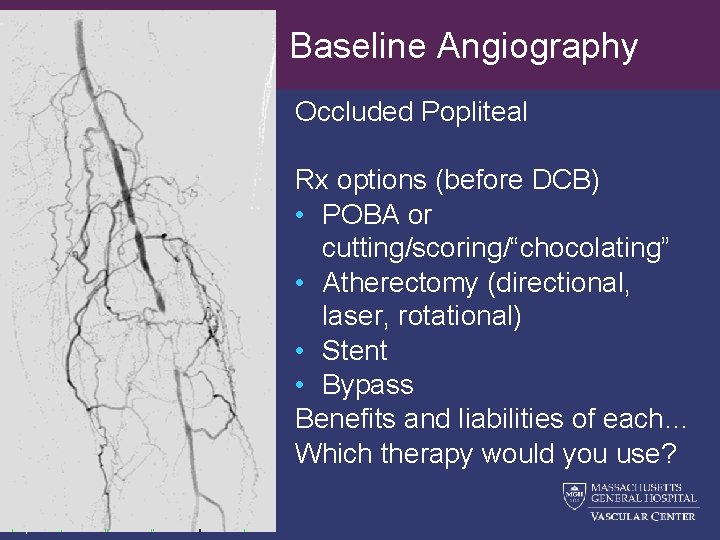
Baseline Angiography Occluded Popliteal Rx options (before DCB) • POBA or cutting/scoring/“chocolating” • Atherectomy (directional, laser, rotational) • Stent • Bypass Benefits and liabilities of each… Which therapy would you use? 7
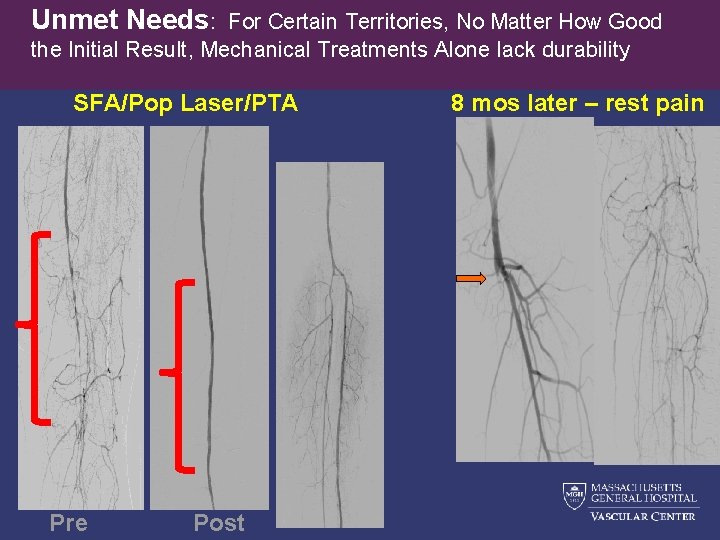
Unmet Needs: For Certain Territories, No Matter How Good the Initial Result, Mechanical Treatments Alone lack durability SFA/Pop Laser/PTA Pre Post 8 mos later – rest pain
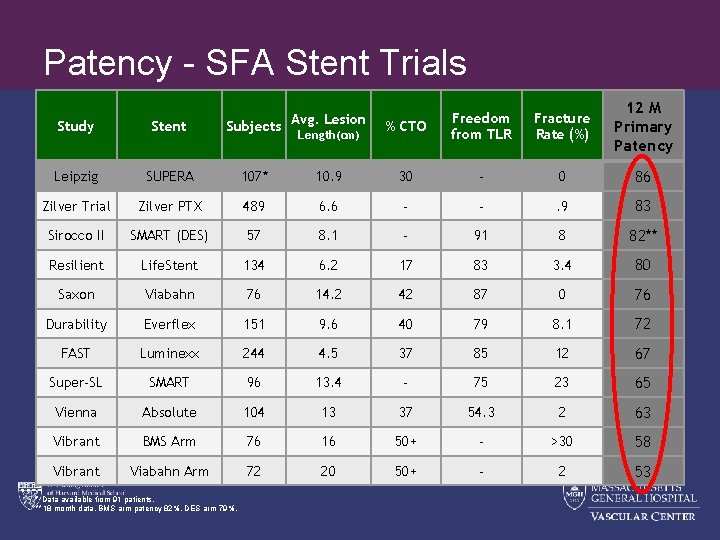
Patency - SFA Stent Trials Avg. Lesion % CTO Freedom from TLR Fracture Rate (%) 12 M Primary Patency Study Stent Subjects Leipzig SUPERA 107* 10. 9 30 - 0 86 Zilver Trial Zilver PTX 489 6. 6 - - . 9 83 Sirocco II SMART (DES) 57 8. 1 - 91 8 82** Resilient Life. Stent 134 6. 2 17 83 3. 4 80 Saxon Viabahn 76 14. 2 42 87 0 76 Durability Everflex 151 9. 6 40 79 8. 1 72 FAST Luminexx 244 4. 5 37 85 12 67 Super-SL SMART 96 13. 4 - 75 23 65 Vienna Absolute 104 13 37 54. 3 2 63 Vibrant BMS Arm 76 16 50+ - >30 58 Vibrant Viabahn Arm 72 20 50+ - 2 53 * Data available from 91 patients. **18 month data. BMS arm patency 82%, DES arm 79%. Length(cm)
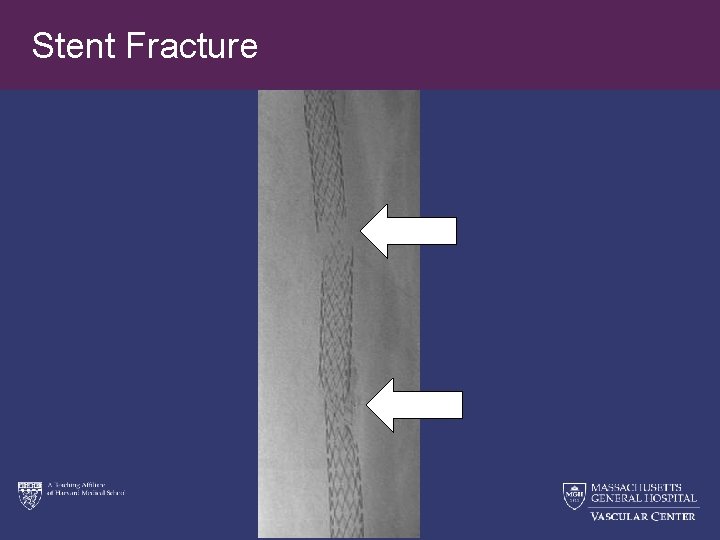
Stent Fracture

Limitations of Current Endovascular Treatments for Femoropopliteal Artery Endovascular Procedures PTA • restenosis rates of 3060% at 1 year 1 • TLR rates of 17. 5% to as high as 54. 9% at 1 year 3, 4 Stents • restenosis rates of 20 -40% at 1 year 2 • ongoing stimulus for restenosis • “no stent zones” segments limit use in femoropopliteal artery • concerns of stent fracture • permanent implants limit future treatment options Reference: (1) Dick et al. ; Laird et al. (2) Laird et al. ; Armstrong et al 3. Dake M et al; 4. Laird JR et al. . 11

Significant Unmet Clinical Need • Significant clinical need remains for a therapy that – Achieves more durable patency by reducing restenosis – Reduces rates of repeat interventions – Does not require a permanent implant – Preserves future treatment options 12
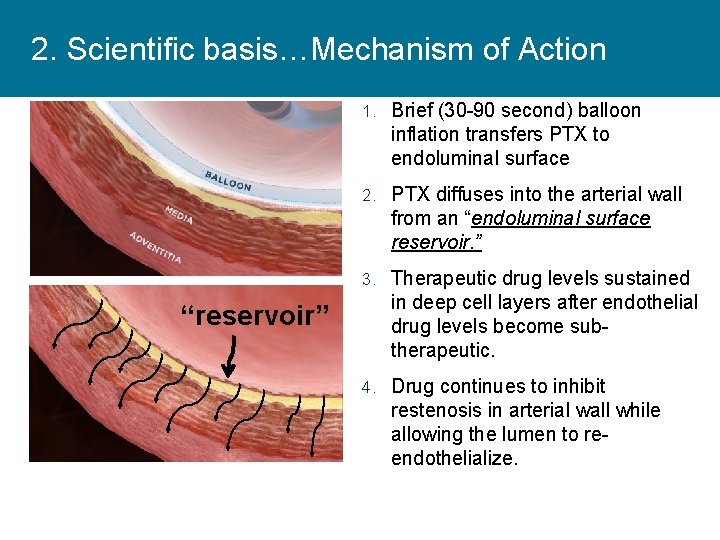
2. Scientific basis…Mechanism of Action 1. Brief (30 -90 second) balloon inflation transfers PTX to endoluminal surface 2. PTX diffuses into the arterial wall from an “endoluminal surface reservoir. ” 3. Therapeutic drug levels sustained “reservoir” in deep cell layers after endothelial drug levels become subtherapeutic. 4. Drug continues to inhibit restenosis in arterial wall while allowing the lumen to reendothelialize.
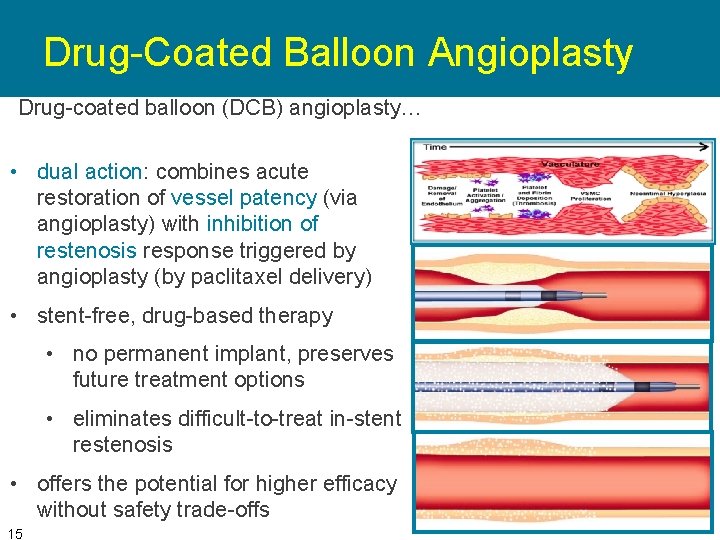
Drug-Coated Balloon Angioplasty Drug-coated balloon (DCB) angioplasty… • dual action: combines acute restoration of vessel patency (via angioplasty) with inhibition of restenosis response triggered by angioplasty (by paclitaxel delivery) • stent-free, drug-based therapy • no permanent implant, preserves future treatment options • eliminates difficult-to-treat in-stent restenosis • offers the potential for higher efficacy without safety trade-offs 15
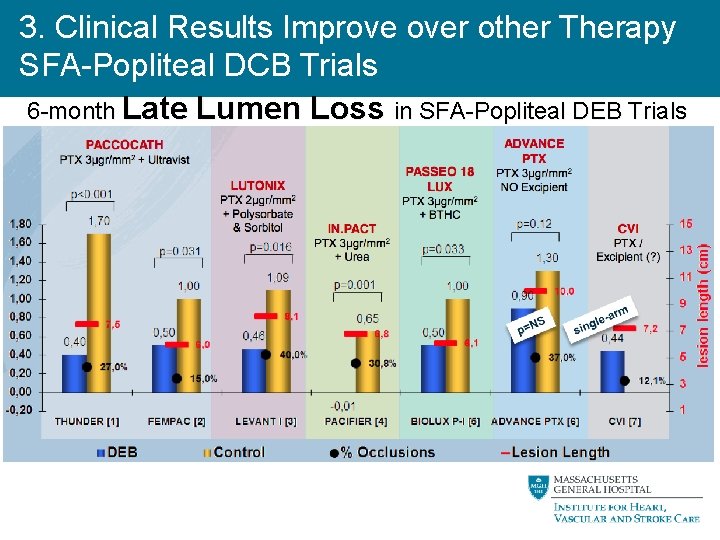
3. Clinical Results Improve over other Therapy SFA-Popliteal DCB Trials 6 -month Late Lumen Loss in SFA-Popliteal DEB Trials J Lammer LINC 2014

17

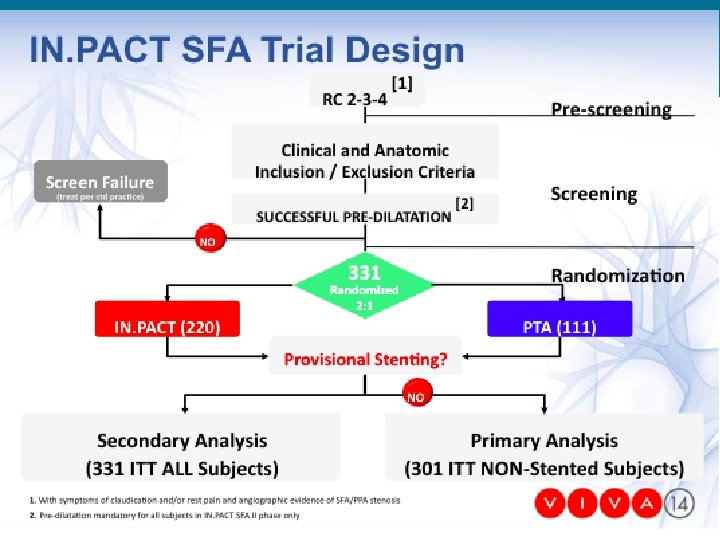
LEVANT 2 Study Flow Pre-Dilatation With Undersized Uncoated Balloon Successful Pre-Dilatation Randomized 2: 1 Test Arm Control Arm Dilatation with Lutonix Drug Coated Balloon Dilatation with Standard PTA 12 Month Follow-up Suboptimal PTA Major flow limiting dissection OR >70% residual stenosis Treat per standard practice 30 day follow-up for safety
19
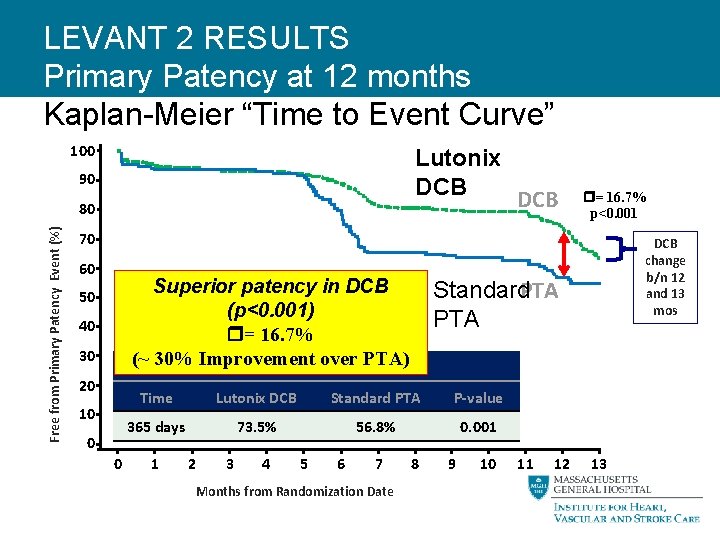
LEVANT 2 RESULTS Primary Patency at 12 months Kaplan-Meier “Time to Event Curve” 100 Lutonix DCB 90 Free from Primary Patency Event (%) 80 = 16. 7% p<0. 001 70 60 Superior patency in DCB (p<0. 001) = 16. 7% (~ 30% Improvement over PTA) Survival % 50 40 30 20 10 0 0 Standard. PTA Time Lutonix DCB Standard PTA P-value 365 days 73. 5% 56. 8% 0. 001 1 2 3 4 5 6 7 Months from Randomization Date DCB change b/n 12 and 13 mos 8 9 10 11 12 13
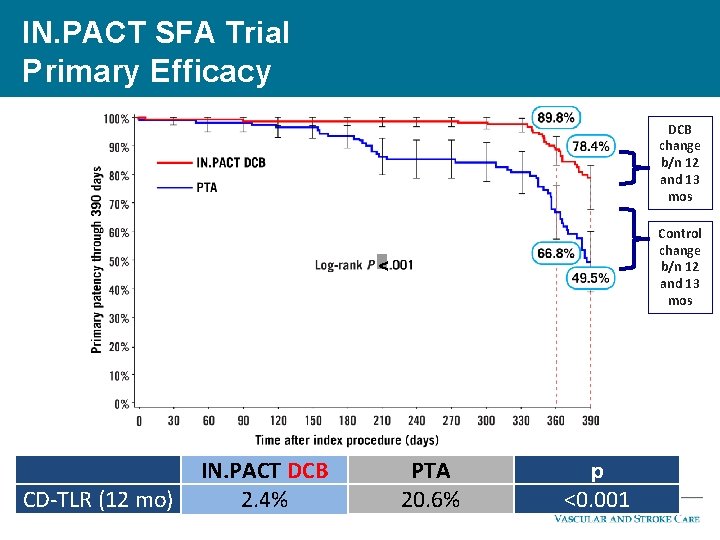
IN. PACT SFA Trial Primary Efficacy DCB change b/n 12 and 13 mos Control change b/n 12 and 13 mos < CD-TLR (12 mo) IN. PACT DCB 2. 4% PTA 20. 6% p <0. 001
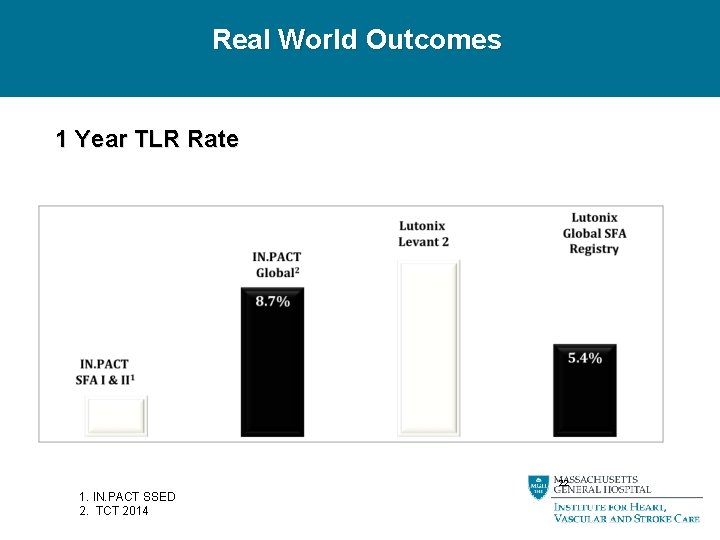
Real World Outcomes 1 Year TLR Rate 22 1. IN. PACT SSED 2. TCT 2014

DCB Conclusions • Proven “class” effect – Drug delivery to deep layers after single contact (dependent on good carrier) • Acceptable safety profile • Many potential advantages – Reduce restenosis; no stent; avoid DAPT, etc. • Initial results promising • Cost unknown • Much more comparative data required

GAME CHANGER? ? . . . NO QUESTION!! • Ubiquitous use in Europe, US, and wherever available • Accepted as Game-Changing • Exact role and indications still being defined…both stand -alone and in conjunction with otherapies – Stents – primary and ISR – Atherectomy – BTK/CLI

Current Unknowns with DCB’s • Unknown interaction with stents, atherectomy, etc. • Unknown effect in heavy calcification • Question of coating uniformity and durability • Opportunity to improve with second generation and beyond…
- Slides: 24