APPROACH TO FETAL ANOMALIES Presented By Tamara shawabkeh

APPROACH TO FETAL ANOMALIES Presented By : Tamara shawabkeh 1

Congenital anomalies Is a term that describe structural, behavioral, functional, and metabolic disorders present at birth or develops later in life. 2

Epidemiology • Congenital malformations are a major cause of infant morbidity and mortality in the world. • Major congenital abnormality occur in 2 - 3% of live births. • Minor congenital abnormality occur in 15% of live born infants. • This incidence increases in pre-term and small for gestational age infants. • Birth defects are the leading cause of infant mortality, accounting for approximately 21% of the infant deaths. 3

Definitions • Malformation: • It`s a primary error results in complete or partial absence of a structure or alterations of its normal configuration. • Occur during organogenesis. • Mostly during the first 8 weeks of gestation. 4

Deformation: • Late change in previously normal structure. • It results from mechanical forces on the fetus which is either extrinsic or intrinsic causes. • Examples: • Extrinsic causes small maternal stature, oligohydramnios, uterine malformation. • Intrinsic factors neuromuscular disease. (club-feet) 5

Why prenatal diagnosis is important? • May treat in utero • To transfer certain cases in utero to deliver in a tertiary care center • The option of termination • To anticipate mechanical obstruction in labor • To avoid unnecessary operative delivery • To prevent maternal psychological trauma

Etiology of Congenital Malformations Unknown - 60% Multifactorial - 20% Single-gene - 7. 5% Chromosomal - 6% Infections - 2 -3% Maternal medical disorders - 1. 5% Maternal medication - 1 -2% 7

Systems commonly involved “over all: 30/1000” • • • CNS => 10/1000 CVS => 8/1000 Renal => 4/1000 Limbs => 2/1000 Others => 6/1000 8

Multifactorial • NTD. • Abdominal wall defect • Uropathy • Cleft lip & palate. • Congenital heart disease 9

Single gene disorders Autosomal Dominant • Only one abnormal gene is necessary for disease manifestation. • E. g. Neurofibromatosis, tuberous sclerosis, Marfan syndrome, Achondroplasia. Autosomal Recessive • Two affected genes must be present for the disease to manifest. • Consanguinity increases the chance. • E. g. sickle cell anemia, cystic fibrosis, congenital adrenal hyperplasia, wilson disease, Tay-Sachs disease. X - linked Recessive • Carried on X chromosomes • Inherited through the mother. • Cannot have male to male transmission. • e. g. fragile X (the 2 nd most common form of mental retardation after Down syndrome) also G 6 PD, Duchenne muscular dystrophy. 10

Chromosomal Disorders • Defect is either in : Number: non disjunction. Structure: translocation Down syndrome is the most common of the chromosomal disorders and the commonest cause of mental retardation in children. 11

CLINICAL APPROACH When to suspect congenital abnormalities? 12

History 1. Maternal age if above 35 years. 2. Previous history of child with birth defect or mental retardation. 3. Previous history of child died in the neonatal period. 4. Recurrent abortion in the first trimester. 5. Parental consanguinity. 6. Exposure to infections or excessive medications. 7. Medical disorders such as DM, epilepsy. 8. Family history of birth defect, chromosomal abnormality, or single gene defect. 13

Obstetric examination: • Fundal height (normal, SGA, …). • Fetal malpresentations. • Abnormal fetal heart. 14

• INDICATIONS FOR GENETIC COUNSELING AND PRENATAL DIAGNOSIS OTHER THAN AGE • 1. A previous child with or a family history of birth defects, chromosomal abnormality, or known genetic disorder • 2. A previous child with undiagnosed mental retardation • 3. A previous baby who died in the neonatal period • 4. Multiple fetal losses • 5. Abnormal serum marker screening results • 6. Consanguinity • 7. Maternal conditions predisposing the fetus to congenital abnormalities • 8. A current pregnancy history of teratogenic exposure • 9. A fetus with suspected abnormal ultrasonic findings • 10. A parent who is a known carrier of a genetic disorder 15

Investigations: • Screening Tests: 1. Biochemical screening tests. 2. Detailed anomaly scan (19 -22 weeks) • Diagnostic Tests: 1. Amniocentesis. 2. Chorionic villus sampling. 3. Cordocentesis 16

Serum screen marker test 1. Alpha fetoprotein: § § 2. 3. 4. It is a glycoprotein produced by the fetal yolk sac and fetal liver (16 -18 GA). Elevated level found in: wrong dating, multiple gestation, fetal demise, liver tumor. NTD, ventral wall defect. HCG Inhibin A Pregnancy specific proteins (e. g. PAPP-A) 17
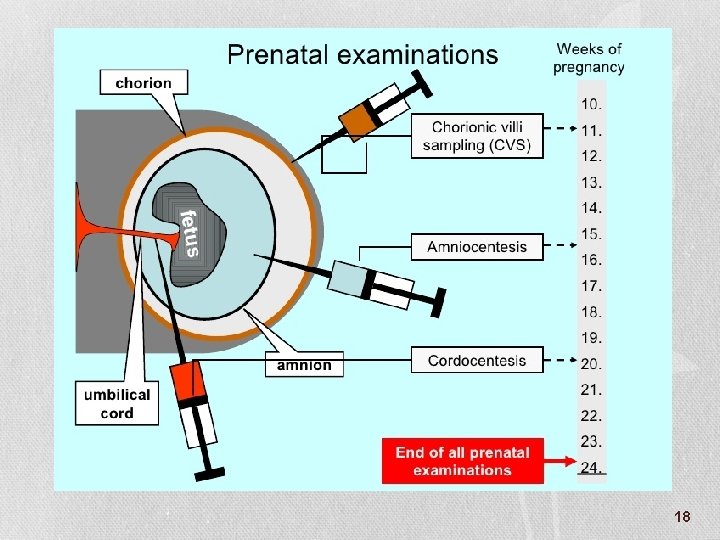
18
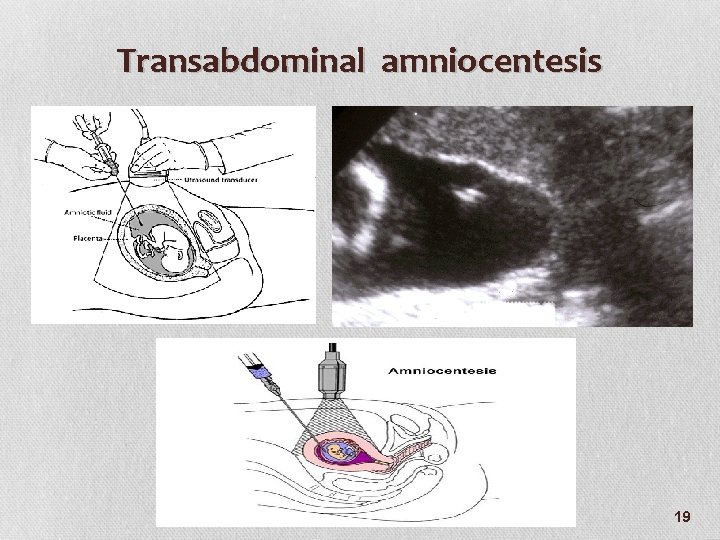
Transabdominal amniocentesis 19
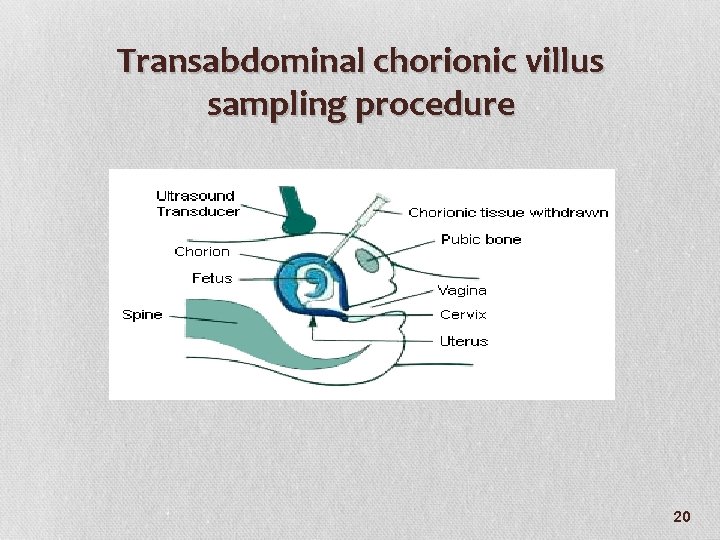
Transabdominal chorionic villus sampling procedure 20

DOWN SYNDROME 21

It is the most common chromosomal disorder. It is the most common cause of congenital mental retardation. The overall risk is 1: 650 for all maternal ages. 22
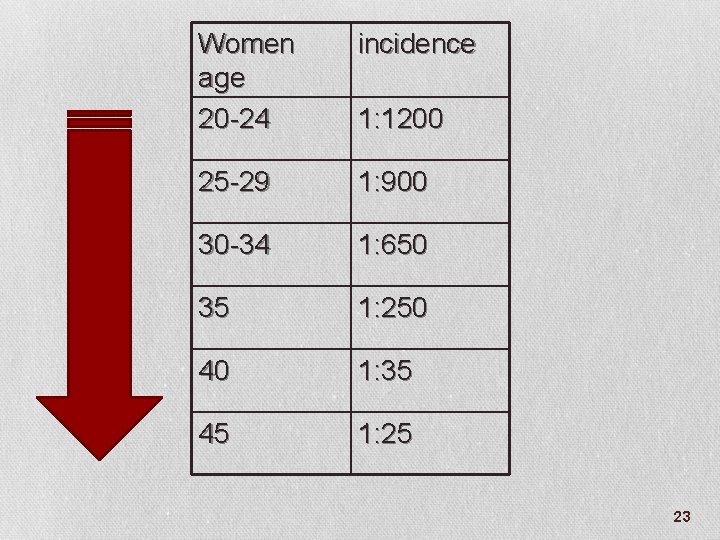
Women age 20 -24 incidence 25 -29 1: 900 30 -34 1: 650 35 1: 250 40 1: 35 45 1: 25 1: 1200 23
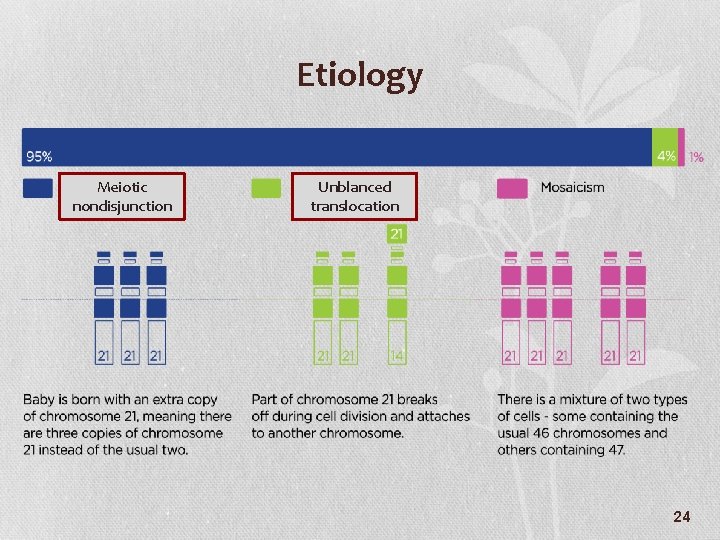
Etiology Meiotic nondisjunction Unblanced translocation 24
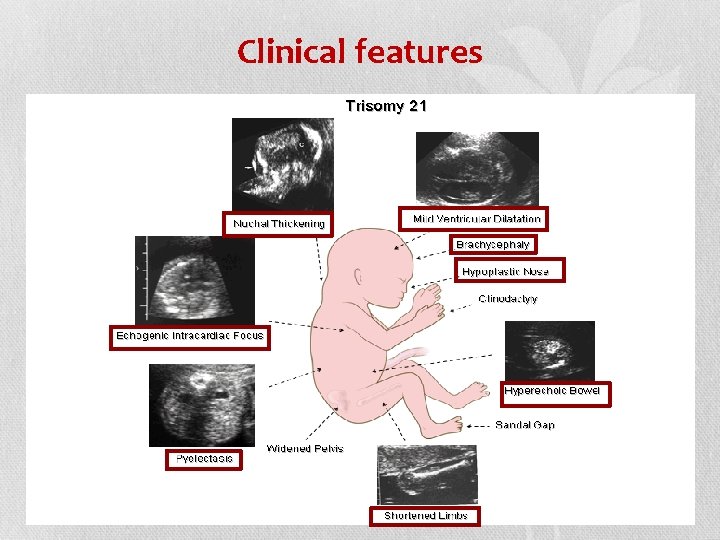
Clinical features 25

Prenatal Diagnosis 26

Prenatal Diagnosis History : Mother age. Previous history of down. Recurrent abortion. Family history. Examination: Small sized fetus. Investigation: Abnormal serum markes. § Ultrasound findings § Amniocenteses, Chorionic villous sampling. § 27
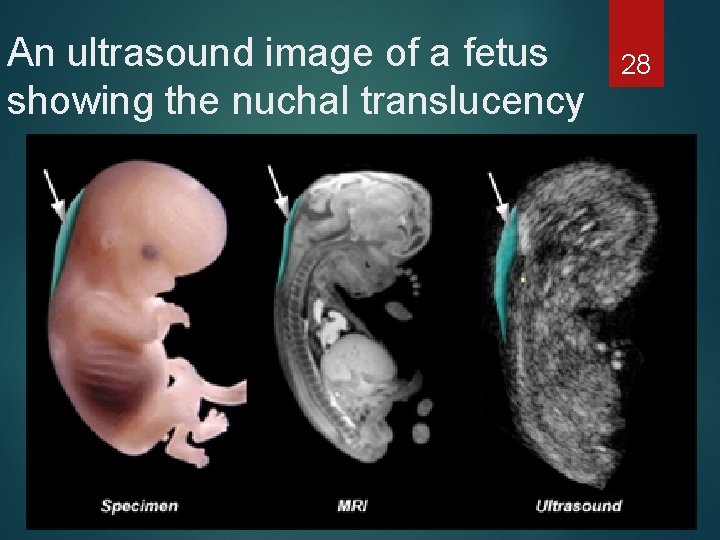
An ultrasound image of a fetus showing the nuchal translucency 28
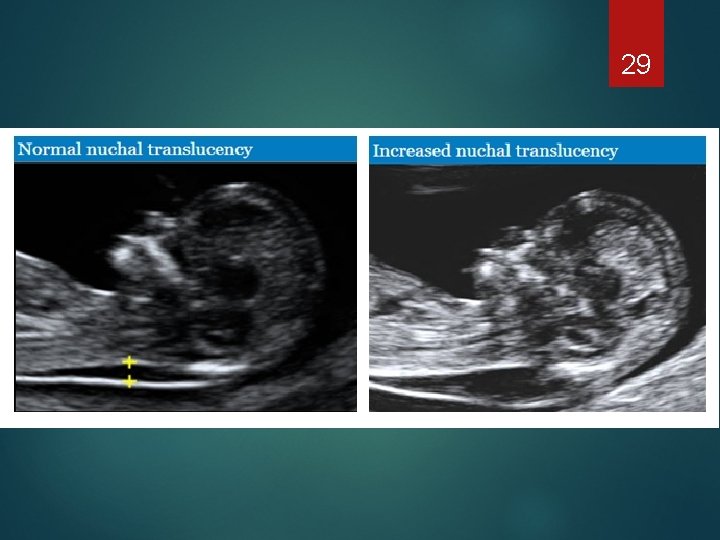
29
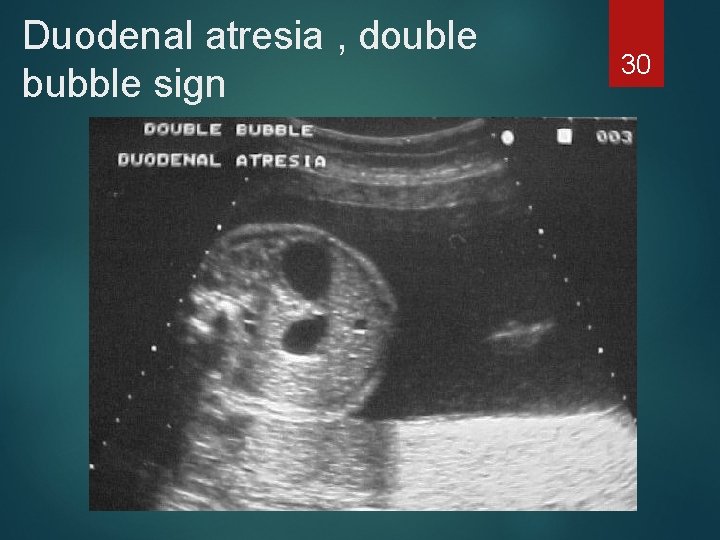
Duodenal atresia , double bubble sign 30

Serum Markers B-hcg : inhibin-A : PAPP-A : Maternal a. FP : 31
32

33 Neural Tube Defects
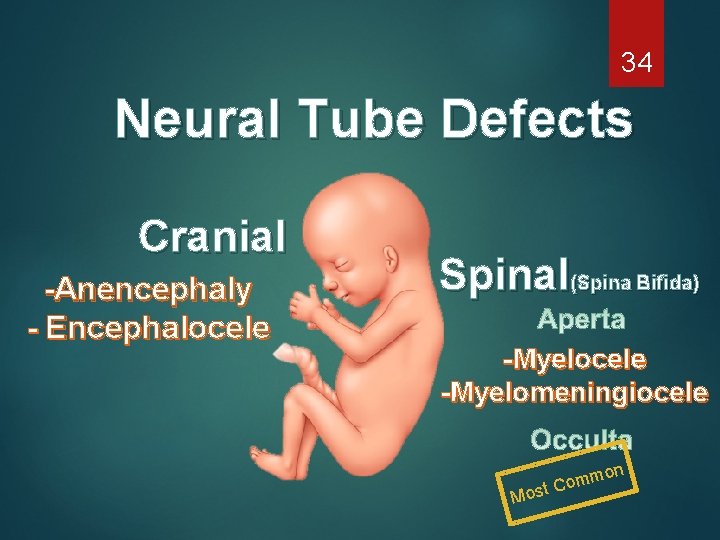
34 Neural Tube Defects Cranial -Anencephaly - Encephalocele Spinal(Spina Bifida) -Myelocele -Myelomeningiocele on Mo mm o C t s
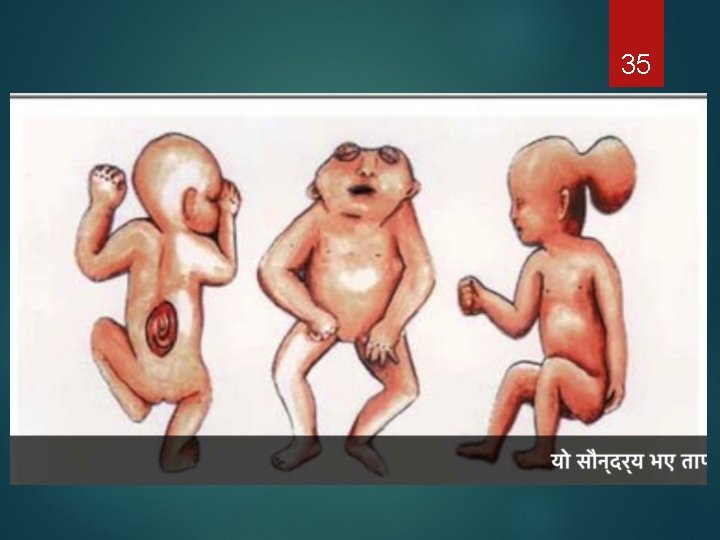
35
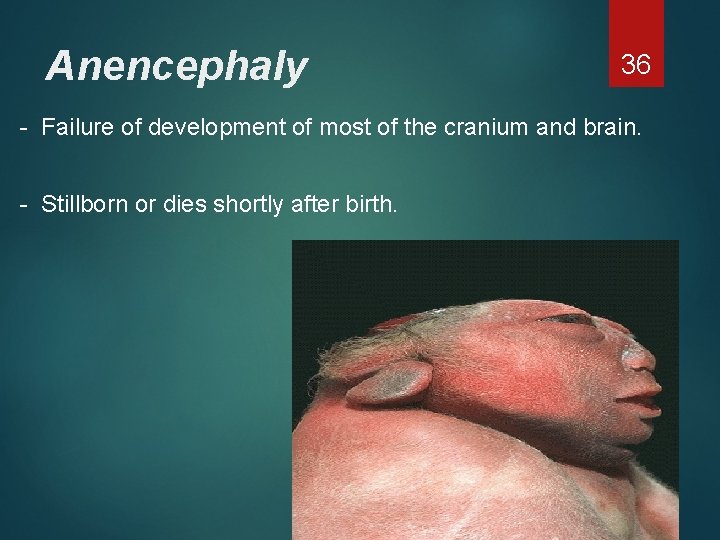
Anencephaly 36 - Failure of development of most of the cranium and brain. - Stillborn or dies shortly after birth.

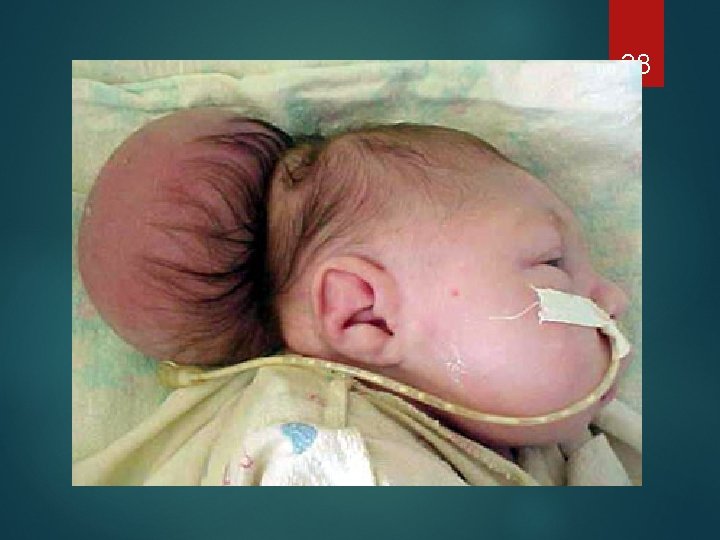
Encephalocele 37 - Extrusion of brain and meninges through a midline skull defect. Prognosis : Can be corrected surgically but often associated cerebral malformations exist.
38
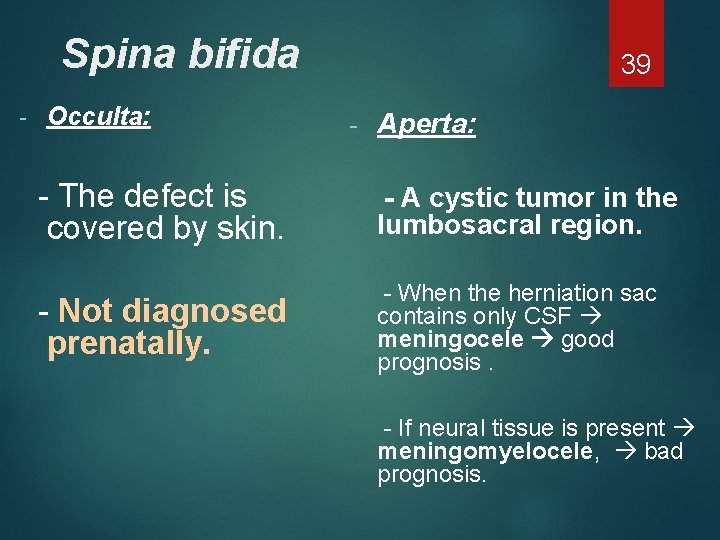
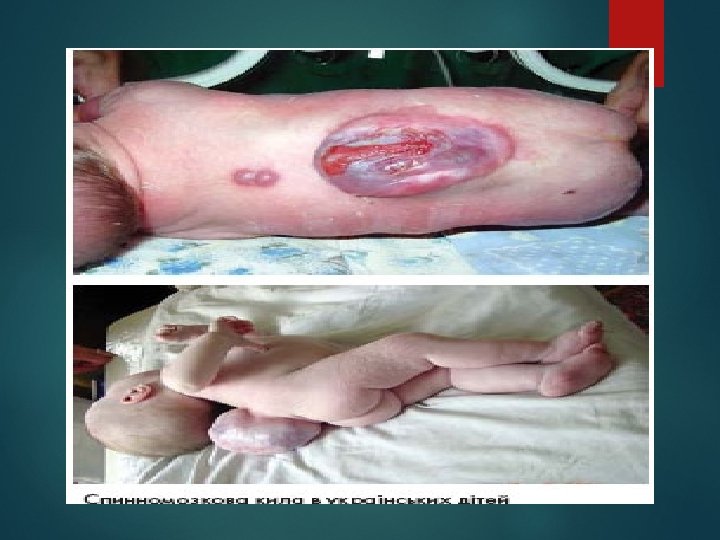
Spina bifida - Occulta: 39 - Aperta: - The defect is covered by skin. - A cystic tumor in the lumbosacral region. - Not diagnosed prenatally. - When the herniation sac contains only CSF meningocele good prognosis. - If neural tissue is present meningomyelocele, bad prognosis.
40

NTD Screening 41 - MSAFP (Maternal Serum Alpha-fetoprotein ) is primarily used from 16 -18 weeks. - Elevated MSAFP levels are highly sensitive and specific for these cases. if elevated ultrasound (to make sure it’s not because of multiple gestationfetal demisewrong date) if truly high amniocentesis is recommended to determine the amniotic fluid AFP level and to measure acetylcholinesterase (ACh. E). Acetylcholinesterase is a protein that is present only if there is an open neural tube defect.

NTD Presentation - IUGR. - Malpresentation - Polyhydramnios - Post-term pregnancy - Decreased fetal movements 42

Abdominal wall defect 43 Gastroschisis and omphalocele are the two most common types of ventral wall defect. Reported with nearly equal frequency in 1 in 4000 live birth.

Types of ventral wall defects include Gastroschisis. Omphalocele 1. 2. • • 3. 4. 5. 6. With extracorporeal liver. With intracorporeal liver. Cleft or absent sternum. Ectopia cordis. Bladder exstrophy. Cloacal exstrophy. 44
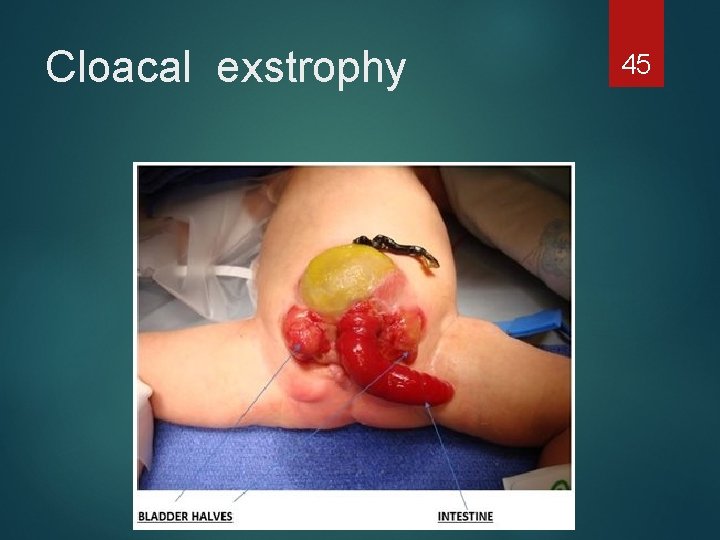
Cloacal exstrophy 45

Ectopia Cordis 46
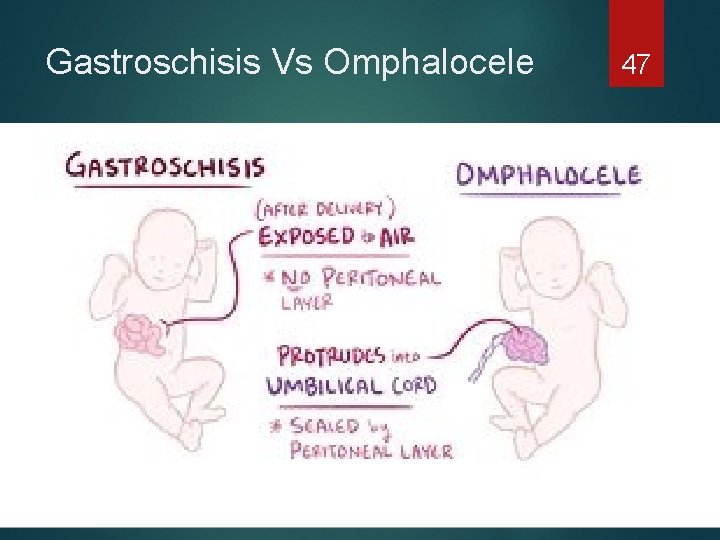
Gastroschisis Vs Omphalocele 47
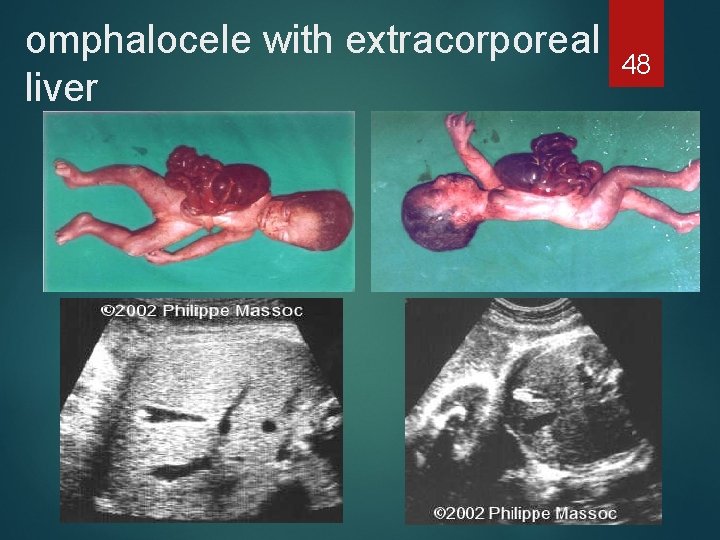
omphalocele with extracorporeal liver 48
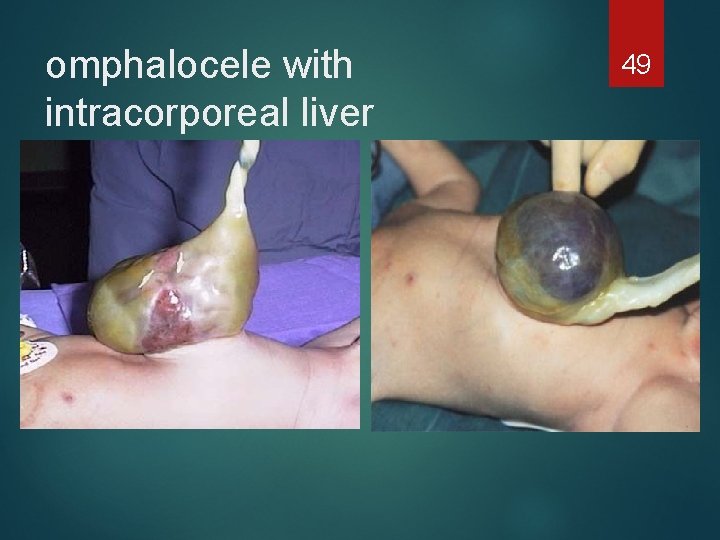
omphalocele with intracorporeal liver 49
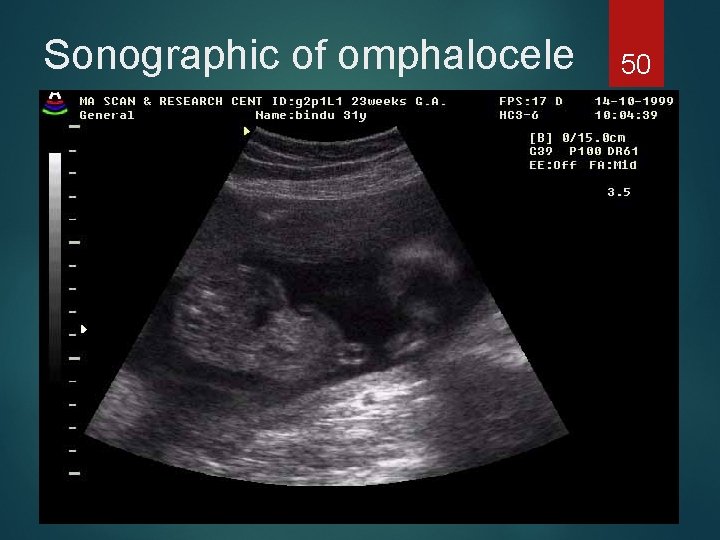
Sonographic of omphalocele 50
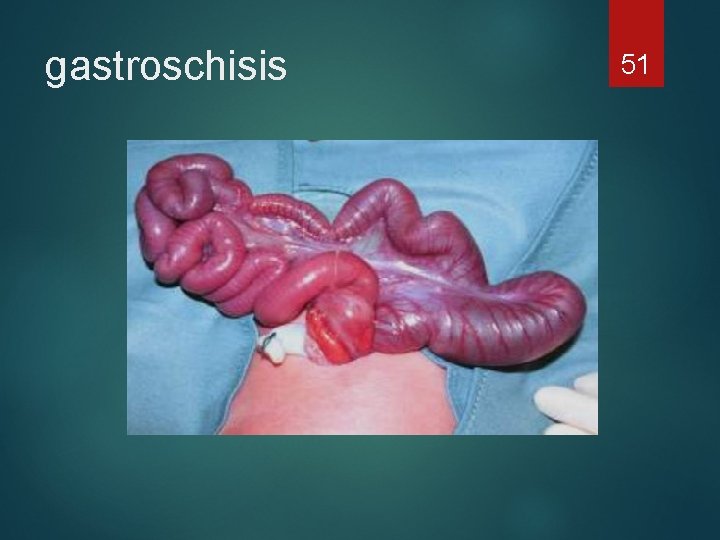
gastroschisis 51
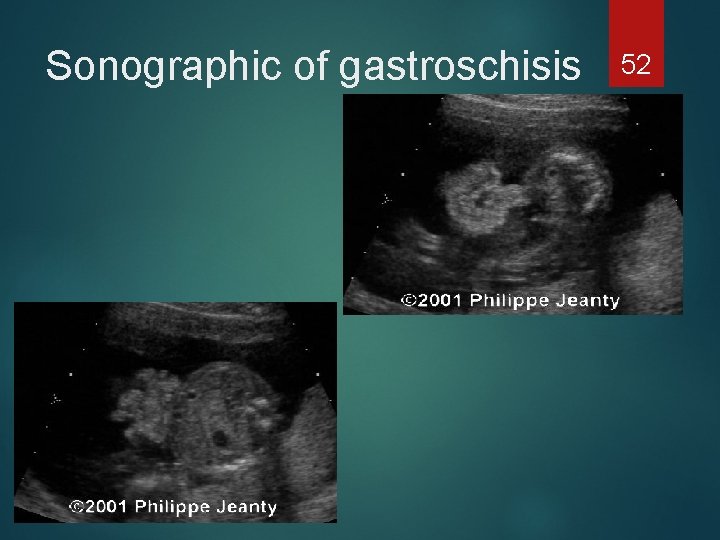
Sonographic of gastroschisis 52

Congenital Heart Disease 53 -10% associated with other defects or part of a syndrome. - They include: -Ventricular Septal Defect. -Atrial Septal Defect. - Patent Ductus Arteriosus. - Tetralogy of Fallot. - Coarctation of the aorta. - Transposition of the Great Arteries.
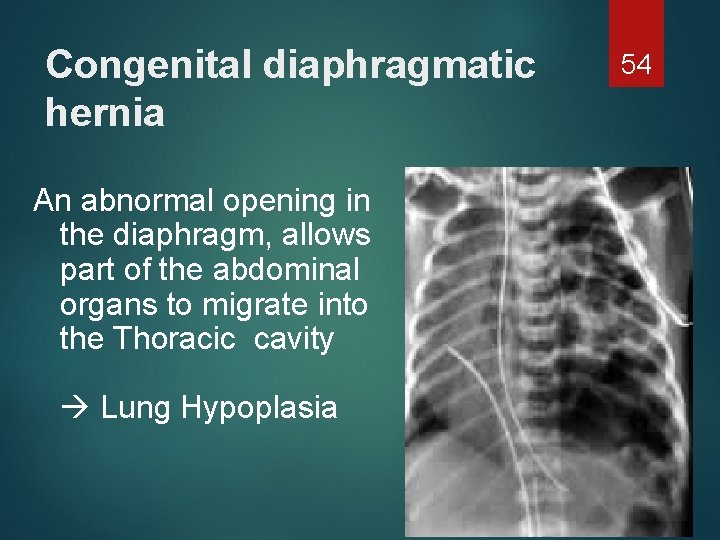
Congenital diaphragmatic hernia An abnormal opening in the diaphragm, allows part of the abdominal organs to migrate into the Thoracic cavity Lung Hypoplasia 54

55
- Slides: 55