Approach to Abnormal Uterine Bleeding Brent E Seibel

Approach to Abnormal Uterine Bleeding Brent E. Seibel, MD Chief, Benign Gynecology Medical Director, UF Health North Jacksonville Associate Professor of Obstetrics and Gynecology University of Florida College of Medicine-Jacksonville

Disclosures v I have no conflicts to disclose

Objectives v Describe nomenclature, work up and management of abnormal uterine bleeding v Illustrate treatment plan options for the PCP

Resources • Committee on Practice Bulletins-Gynecology. Practice Bulletin no. 128: diagnosis of abnormal uterine bleeding in reproductive-aged women. Obstet Gynecol 2012; 120: 197 • Munro MG, Critchley HO, et al. FIGO classification system (PALM-COEIN) for causes of abnormal uterine bleeding in nongravid women of reproductive age. Int J Gynaecol Obstet 2011; 113: 3 • Up. To. Date. R : Approach to abnormal uterine bleeding in nonpregnant reproductive-age women. www. uptodate. com

Introduction v Abnormal uterine bleeding (AUB) v Menstrual bleeding of abnormal quantity, duration, or schedule v AUB terminology more descriptive than menorrhagia, metrorrhagia, etc. v Accounts for 1/3 outpatient visits to gynecologists v Wide variety of local and systemic diseases or medications v Annual prevalence of 53 per 1000 women v Common etiologies v Structural, anovulation, disorders of hemostasis or neoplasia

Abnormal Uterine Bleeding Heavy Menstrual Bleeding (AUB-HMB) Intermenstrual Menstrual Bleeding (AUB-IMB) PALM: Structural Polyp (AUB-P) Adenomyosis (AUB-A) Leiomyoma (AUB-L) Malignancy and Hyperplasia (AUB-M) COEIN: Non-Structural Coagulopathy (AUB-C) Ovulatory Dysfunction (AUB-O) Endometrial (AUB-E) Iatrogenic (AUB-I) Not Yet Classfied (AUB-N)
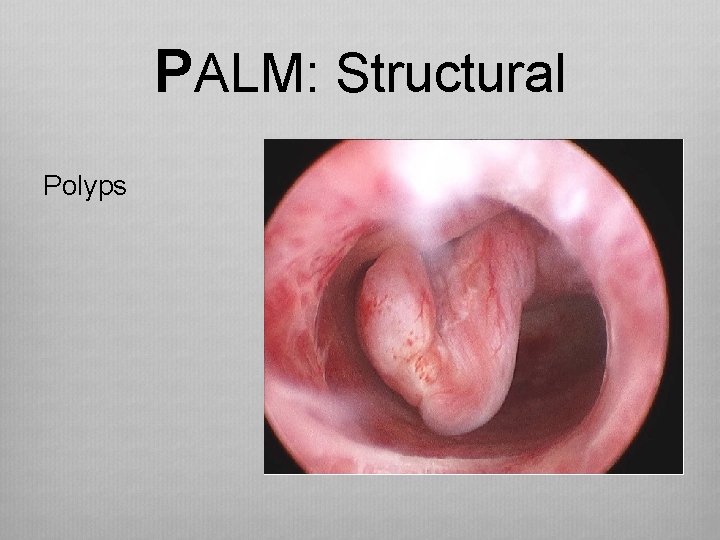
PALM: Structural Polyps
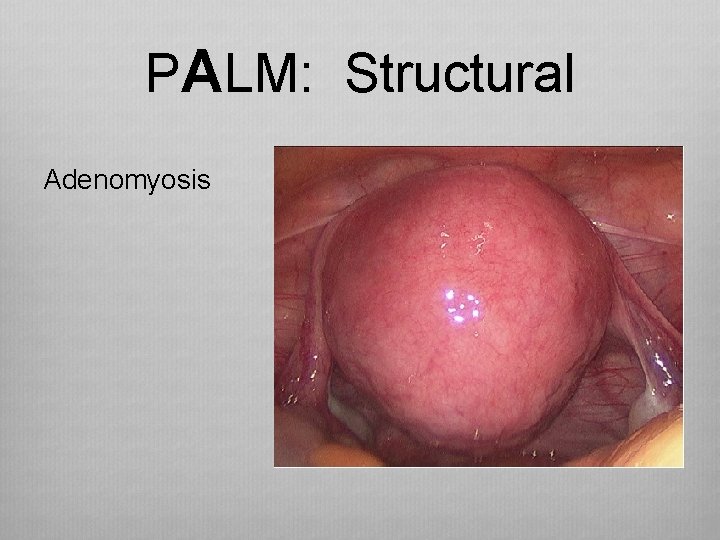
PALM: Structural Adenomyosis
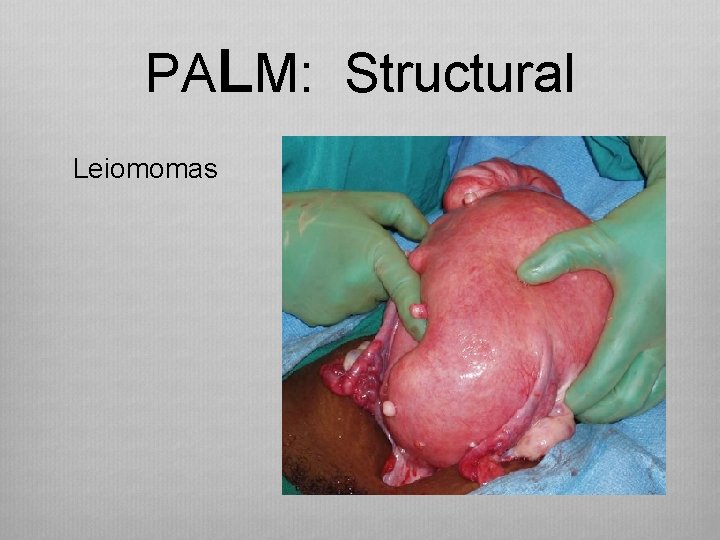
PALM: Structural Leiomomas
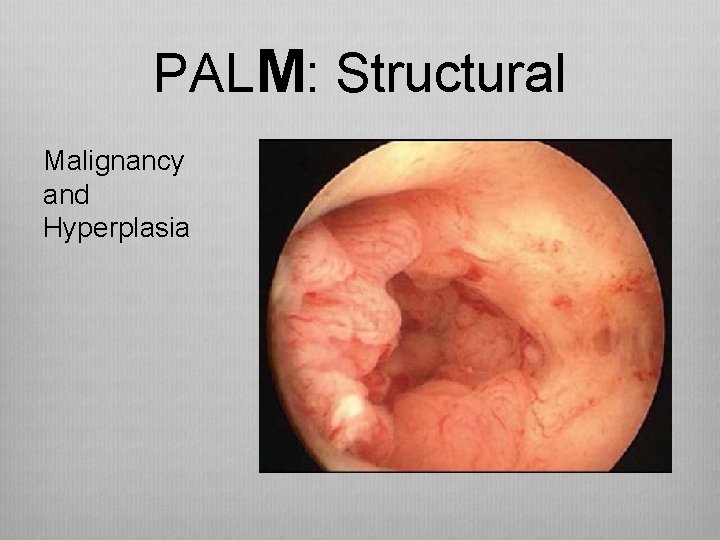
PALM: Structural Malignancy and Hyperplasia

COEIN: Non-structural v Coagulopathy v Inherited and acquired v May occur in up to 20% of patients with HMB v Indications for evaluation v HMB since menarche v Postpartum hemorrhage, excessive surgical bleeding or bleeding with dental work, or any two of the following v Bruising 1 -2 times per month v Epitaxis 1 -2 times per month v Frequent gum bleeding v Family history of bleeding symptoms

COEIN: Non-structural v Ovulatory Dysfunction (From amenorrhea and oligomenorrhea to frequent irregular menses) v Hypothalimic hypogonadotropic hypogonadism v Thyroid dysfunction v Hyperprolactinemia v Hyperandrogenemia/PCOS v Premature ovarian insufficiency v Idiopathic anovulation v Chronic illness

COEIN: Non-structural v Endometrial Abnormalities v Abnormal endometrial angiogenesis v Prostaglandin production v Vasoconstriction v Increased fibrinolysis

COEIN: Non-structural v Iatrogenic v Contraceptives v OCPs, patch or ring v Depo Provera (DMPA) v Contraceptive implant (Nexplanon) v Intrauterine device (IUD) v Other medications v Antipsychotics v Anticoagulants v other

Evaluation: History v Age of menarche v Menstrual bleeding pattern v Severity of bleeding v Pain v Medical history v Surgical history v Family history v Bleeding disorders, PCOS, diabetes, cancer

Evaluation: Medications v Anticoagulants v Hormonal medications v NSAIDS v Antipsychotics v Supplements

v Evaluation: Physical Exam Weight extremes v Skin v Acanthosis nigrans v Hirsuitism v Acne v Pallor v Petechiae or echymosis v Thyroid v Abdomen v Pelvic

Evaluation: Labs v Pregnancy test v STD testing if indicated v Pap smear v CBC v TSH

Evaluation: Labs v Bleeding disorder v PT/PTT/INR v Platelet function v Fibrinogen v Hyperandrogenism/PCOS v Testosterone v DHEAS v 17 -OHP v Hgb. A 1 C, lipids, CMP

Evaluation: Labs v Amenorrhea/Oligomenorrhea v Prolactin v FSH/LH v Estradiol
Evaluation: Imaging v Transvaginal ultrasound v Saline Infusion Sonohysterogram (SIS) v Excellent for cavity assessment v MRI v Fibroid mapping v Mullerian anomalies v Adenomyosis

Evaluation: Tissue Sampling v Endometrial biopsy v Women > age 45 with AUB v Women < age 45 with chronic anovulation v Obese v PCOS v Unopposed estrogens v Hysteroscopy v D&C

Treatment: Medical v Combined oral contraceptives v Progesterone therapy v Oral v Intramuscular v Levonorgestrel intrauterine system (IUD) v Tranexamic acid v NSAIDs

Treatment: Surgical v Dilation and Curettage (D&C) v Hysteroscopy v Diagnostic v Operative (polypectomy, myomectomy) v Endometrial ablation v Uterine artery embolization (UAE) v Myomectomy v Hysterectomy
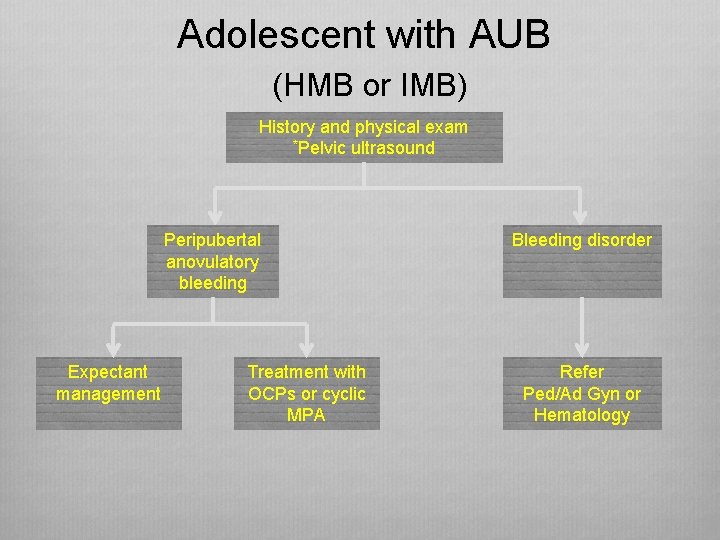
Adolescent with AUB (HMB or IMB) History and physical exam *Pelvic ultrasound Peripubertal anovulatory bleeding Expectant management Treatment with OCPs or cyclic MPA Bleeding disorder Refer Ped/Ad Gyn or Hematology
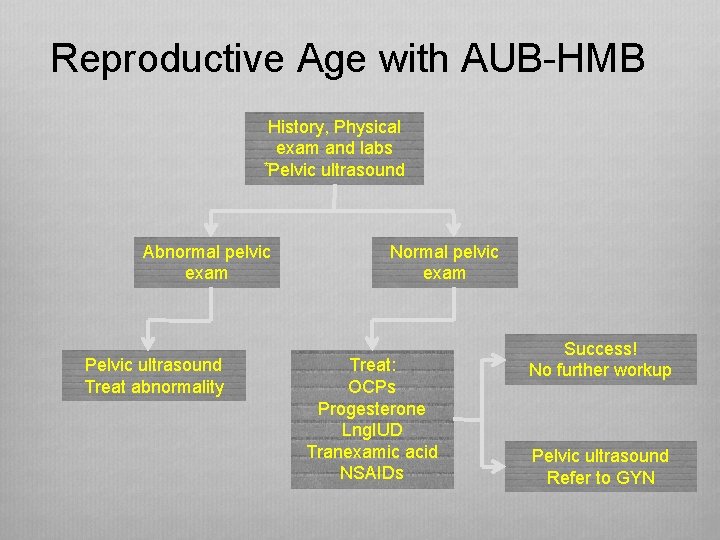
Reproductive Age with AUB-HMB History, Physical exam and labs *Pelvic ultrasound Abnormal pelvic exam Pelvic ultrasound Treat abnormality Normal pelvic exam Treat: OCPs Progesterone Lng. IUD Tranexamic acid NSAIDs Success! No further workup Pelvic ultrasound Refer to GYN
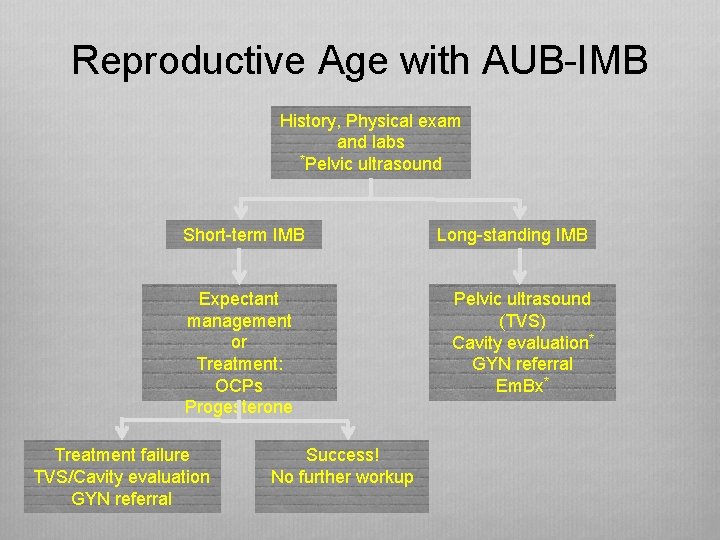
Reproductive Age with AUB-IMB History, Physical exam and labs *Pelvic ultrasound Short-term IMB Expectant management or Treatment: OCPs Progesterone Treatment failure TVS/Cavity evaluation GYN referral Success! No further workup Long-standing IMB Pelvic ultrasound (TVS) Cavity evaluation* GYN referral Em. Bx*

Summary v AUB a common condition among reproductive age women v Evaluation and initial management by PCP v Differentiate between structural and non- structural causes v PALM – COEIN terminology

Thank you! v Questions?
- Slides: 29