APNOEA By NICOLE STEVENS Objectives Definition of apnoea

APNOEA By: NICOLE STEVENS

Objectives �Definition of apnoea �Identify causes and incidence of apnoea �Identify the categories of apnoea �Discuss the pathophysiology of apnoea �Discuss apnoea of prematurity �Identify risk factors for apnoea �Discuss nursing management of apnoea �Pharmacological management of apnoea

Introduction �Apnoea is a disorder of respiratory control �It more commonly effects preterm infants �Is rare among full term healthy infants and, if present usually indicates an underlying pathology �Several mechanisms have been proposed to explain apnoea, and many clinical conditions have been associated with its development �Apnoea of prematurity (AOP) is seen in infants < 37 wks gestation, with the incidence increasing as gestational age decreases

Definition �The cessation of respiratory inflow; it is a disorder of respiratory control common in premature infants �Pathologic apnoea is defined as a respiratory pause of greater than 20 seconds or any pause in respirations associated with cyanosis, marked pallor, marked hypotonia, or bradycardia (Theobald et al). � Apnoea of prematurity (AOP) is a pathological apnoea with no definable cause in infants < 37 wks gestation, usually presenting between days 3 – 7 of life

Causes of Apnoea Day 1 – 2 �Sepsis �Hypoglycaemia �Impending respiratory failure �Polycythaemia Days 3 – 6 �Sepsis �Impending respiratory failure �PDA �Massive IVH �AOP

Causes of Apnoea Late Onset �Sepsis �Progressive post-extubation atelectasis �Out grown dose of methylxanthine (eg. caffeine) �Presenting symptom of RSV infection

Incidence Apnoea occurs in �Most infants < 30 wks �About 50% of infants at 30 – 32 wks �About 10% of infants at 34 wks Usually resolves by 36 wks CA Good evidence that it is not a risk factor for SIDS No evidence that AOP causes subsequent neurodevelopmental morbidity, although recurrent apnoea is concerning because of the effects of the repeated episodes of tissue hypoxia (especially on the gut and the brain)

Categories of Apnoea �Apnoea has three major types: central, obstructive & mixed CENTRAL APNOEA �No respiratory effort, displayed by a lack of chest wall movement, and no breath sounds heard on auscultation �The central controlling area for breathing, called the respiratory centre, is in the lower part of the brain stem, in the medulla oblongata �The automatic breathing rhythm is controlled by inspiratory and expiratory neurons; this automatic rhythm can be altered by afferent information

Categories of Apnoea Central cont. . . �An information exchange occurs to (afferent) and from (efferent) the respiratory centre of the brain �An afferent supply of information travels to the respiratory centre of the brain from central chemoreceptors, peripheral chemoreceptors, other areas of the brain and from the lungs �Chemoreceptors are cells that respond to chemical stimuli; central chemoreceptors are located in a part of the brain stem and they respond to the acidity of the CSF and the output from these cells influences breathing

Categories of Apnoea �The peripheral chemoreceptors that feedback to the respiratory centre are the carotid and aortic bodies – which are small pieces of tissue containing chemoreceptors that respond to O 2 & CO 2 levels in arterial blood �The carotid body in particular provides continual feedback; if the Pa. O 2 goes below 80 mm. Hg or the Pa. CO 2 goes above 40 mm. Hg then there will be an immediate increase in breathing rate

Categories of Apnoea �Other parts of the brain can also provide feedback to the respiratory centre and cause an alteration in respiratory rate eg: conscious or deliberate hyperventilation, hyperventilation in response to intensely emotional or distressing situations or sights, and hyperventilation in response to massive blood loss (coordinated by the autonomic system in the brainstem and the vasomotor centre in the brain stem) �The lungs: provide feedback via stretch receptors in the elastic tissues of the lung, the chest wall and the pulmonary blood vessels; the bronchi also have receptors cells

Categories of Apnoea �Once messages are received by the respiratory centre it will send messages back out to the body via the efferent nerves �They pass down the spinal cord to the diaphragm, intercostal muscles & accessory muscles of inspiration in the neck �The diaphragm is supplied by the phrenic nerve (C 35) �The intercostal muscles by the segmental intercostal nerves (T 1 -12) �The accessory muscles by the cervical plexus (C 1 -4)

Categories of Apnoea �So, in summary, central apnoea occurs when there is a lack of respiratory effort due to a failure in the feedback messages getting to the respiratory centre or a failure of the respiratory centre to send the messages out to the peripheral nerves and respiratory muscles required for oxygenation and ventilation �This can be due to immaturity in the system as seen in premature infants who have a decreased response to hypercapnia; head trauma; and toxin-mediated apnoea (analgesics, anaesthetics, infections)

Categories of Apnoea �Opioid drugs, such as morphine, pethidine & fentanyl (as well as illicit substances such as heroin), depress the respiratory centre’s response to hypercarbia �Some anaesthetic agents may also do this (such as with women that require a GA for caesarean section) �These drugs can cross the placenta to the fetus and when born the infant can have profound apnoea and require prolonged assistance with IPPV until spontaneous respirations are established

Categories of Apnoea OBSTRUCTIVE APNOEA �Results from attempts to breath through an occluded airway �Can be the result of a congenital problem (smaller airway patency) �Other causes of obstructive apnoea are an aspirated foreign body or vocal cord paralysis

Categories of Apnoea MIXED APNOEA �Has characterisics of both mixed and obstructive �Eg: a premature infant with central apnoea who has an obstruction due to nasal congestion brought on by a viral illness �Gastro oesophogeal reflux is thought to cause this mixed picture as regurgitated gastric contents may occlude the airway and block laryngeal chemoreceptors from sending signals for dilation to the brain

Primary & Secondary Apnoea Types of apnoea at delivery: �Primary: when asphyxiated the infant responds with an initial increase in respiratory effort, they then become apnoeic and heart rate drops – but they will be quickly responsive to tactile stimulation +/- IPPV �Secondary: when asphyxia continues beyond primary apnoea, the infant responds with gasping respirations, falling HR and BP; they take a last breath, enter the secondary apnoea phase and death will occur if resuscitation does not commence immediately. Will not be responsive to stimulation

Apnoea of Prematurity �AOP is a diagnosis of exclusion and should only be considered after secondary causes have been excluded Premature babies are more at risk or apnoea because of : �Central immaturity �Alterations in CO 2 response �Hypoxia �Immature sleep patterns �Greater risk of pharyngeal obstruction �Greater risk of laryngeal obstruction �More reflux induced problems
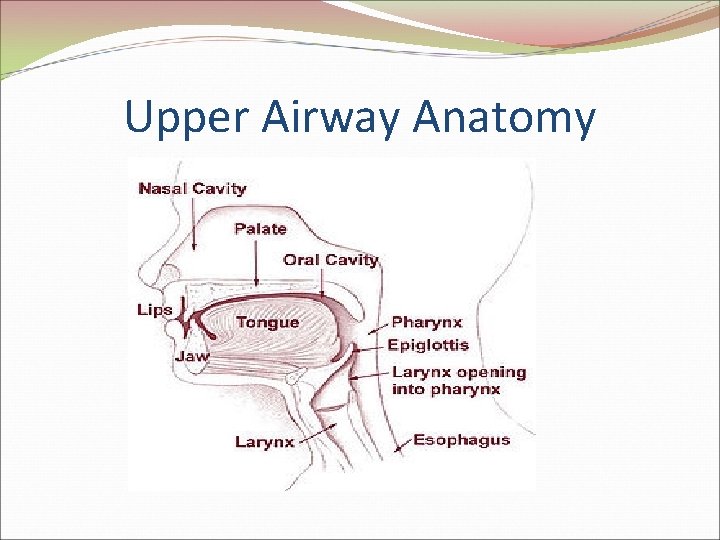
Upper Airway Anatomy

Sleep States �Premature babies are at increased risk of apnoea because of immature sleep patterns �Breathing in infants is strongly influenced by sleep states �Apnoeic spells occur more frequently in REM sleep than active sleep �REM sleep predominates in preterm infants (80% of the day)

Differential Diagnosis Although AOP is the most common cause of apnoea there are other conditions that may cause or aggravate apnoea: �Anatomical anomalies of upper airway �Infection: sepsis, NEC �Temperature disturbances �Metabolic: hyper or hypocalcaemia, hypoglycaemia, hyponatraemia, acid/base disturbances �Haematological: anaemia, polycythaemia �Pulmonary: impending respiratory failure

Differential Diagnosis �CVS disorders: causes of cardiac failure or impaired oxygenation eg. PDA, congenital defects, arrhythmias �CNS disorders: IVH, intracranial haemorrhage, seizures, asphyxia, increased intracranial pressure, cerebral abnormalities �Drugs: prenatal (narcotics, betablockers, Mg. SO 4, maternal smoking) and postnatal (sedatives, hypnotics, narcotics, prostaglandin)

Monitoring �All infants < 34 wks gestation should be monitored for apnoea �Monitoring can be with a full cardiorespiratory monitor, Sa. O 2 and heart rate monitor or an apnoea monitor only �Type of monitoring required will depend on other factors: gestation of the baby, availability of equipment & what level of care can be provided at the particular hospital �If the preterm baby can not be adequately monitored & managed they need to be moved to a hospital that can provide an appropriate level of care

Evaluation of Apnoea �Take a history, including apgar scores �Physical examination �Sepsis risk? �Consider age (GA, and day of life) �See if apnoeic events are associated with feeds �Determine frequency of events and intervention required (if any) �Evaluated associated bradycardia and cyanosis �Repeated apnoeas with quick recovery, or any profound apnoeas need to be reported to medical personnel

Investigations �Septic workup (FBE, CRP, blood culture +/- SPA of urine & LP) �Other pathology: Electrolytes, TBG, gases �Chest Xray �Abdominal Xray �Neurological investigations (Cr. US, MRI, physical assessment) �Reflux investigations

Emergency Management �Provide tactile stimulation �Reposition, paying attention to minimising airway obstruction, ie. Get chin off chest – position head in a neutral or slightly extended position �Suction airway briefly, repeat tactile stimulation �Provide IPPV in air/oxygen – CALL FOR HELP �If still no response, continue IPPV and consider intubation

Symptomatic Management �If an infectious aetiology is suspected treat with antibiotics �Correct any electrolyte disturbances �Supportive management for respiratory compromise �Consider managment of cardiovascular issues eg. indocid for PDA, inotropes for low BP or poor cardiac contractility �If CNS issues: antiseizure medication, antimicrobials (menigitis), ventricular decompression �Consider PRBC and ongoing iron supplementation �GI considerations: NEC, obstruction, dysmotility

Ongoing Management Not all episodes of apnoea require treatment; the following is suggested list from the NETS handbook: �Episodes needing brief stimulation for cyanosis & bradycardia: > 6 events every 12 hrs �Episodes needing vigorous stimulation & oxygen: > 1 event every 24 hrs �Episodes needing IPPV +/- oxygen: > 1 event every 24 hrs

Ongoing Management �Position infant to avoid upper airway obstruction (neck rolls, prone or side lying) �Give smaller volume feeds (increase frequency with smaller volumes and/or reduce TFI if possible), to avoid excessive stomach distention �Consider maintaining temperature at lower end of normal spectrum �Low amounts of ambient oxygen (ie cot oxygen at 2324%) – must have continuous Sa. O 2 monitoring, and upper limit lowered to prompt weaning to avoid hyperoxia

Pharmacological Management �Methylxanthines and continuous positive airway pressure (CPAP) form the mainstay of treatment of apnoea in neonates; mechanical ventilation is reserved for when the apnoea is resistent to these treatments �Methylxanthines include caffeine and theophylline(oral form) & aminophylline(IV form); are thought to stimulate breathing efforts in neonates and have been used in clinical practice since the 1970’s �Cochrane review (2010) suggests caffeine preferable to theophylline

Pharmacological Management CAFFEINE �Has a comparable efficacy to theophylline but with less side effects, and does not require regular blood sampling for levels �Caffeine has a longer half life (so only requires once daily administration), more reliable enteral absorption and there are less instances of having to reduce doses due to tachycardia and feed intolerance �Different institutions will vary in practice guidelines for prophylactic administration and maintenance doses

Pharmacological Management Caffeine cont. . �Loading dose 20 mg/kg (IV or oral) �Then maintenance dose of 5 mg/kg daily(may see increases in this dose in symptomatic infant to 10 mg/kg) �Dose may be ceased in the asymptomatic infant from 34 -36 wks CA, or in some cases, the infant may be allowed to ‘grow out of the dose’ – not increasing the dose as the infants weight increases

Pharmacological Management Caffeine cont. . . �Other infants may remain symptomatic and continue on caffeine beyond term corrected age �Infants born at < 28 wks GA will often remain symptomatic of AOP beyond term corrected age �Because of caffeines long half life (approx. 100 hrs) infants should be monitored for 5 – 7 days post cessation of medication (apnoea monitors are usually sufficient if the infant is otherwise well)

Other Management CPAP �Used to manage obstructive and mixed apnoeas �Splints the nasopharynx and prevents pharyngeal collapes �Stabilizes the chest wall musculature �Alters various reflexes �Increases functional residual capacity �Initial settings would be 5 – 7 cm/H 2 O, adjusted according to clinical response �NETS should be consulted if in a non-NICU centre

Parents �Inform and educate parents of risk of apnoea (particularly if they have had a premature baby) �Inform if apnoeas are occurring and if treatment is required �Explain expected length of treatment �Explain need for ongoing monitoring (including after medications are ceased) �Provide reassurance �Consider CPR training for any parents who have had a baby in a SCN or a NICU

Reference List � Aggarwal, R. , Singhal, A. , Deorar, A. , & Paul, V. Apnea in the Newborn. Division of Neonatolgy. Department of Paediatrics. All India Institute of Medical Sciences. www. newbornwhocc. org � Hansen, T. N. , Cooper, T. R. and Weisman, L. E. (1995) Neonatal Respiratory Diseases handbooks in Health Care Co. , Newtown, Pennsylvania � Theobald, K. , Botwinski, C. , Albanna, S. & Mc. William, P. (2000). Apnea of Prematurity: Diagnosis, Implications for Care and Pharmacologic Management. Neonatal Network, Vol 19. No. 6 17 – 22. � Neonatal Handbook: Apnoea. (2011). www. rch. org. au/nets/handbook
- Slides: 37