Aplastic Anemia Rakesh Biswas MD Professor Department of

Aplastic Anemia Rakesh Biswas MD, Professor, Department of Medicine, People's College of Medical Sciences, Bhanpur, Bhopal, India

Morphologic, Etiologic Possible causes: Investigations and treatment

• Definition: – Pancytopenia with hypocellularity (Aplasia) of Bone Marrow • One cell line may be affected more than the others
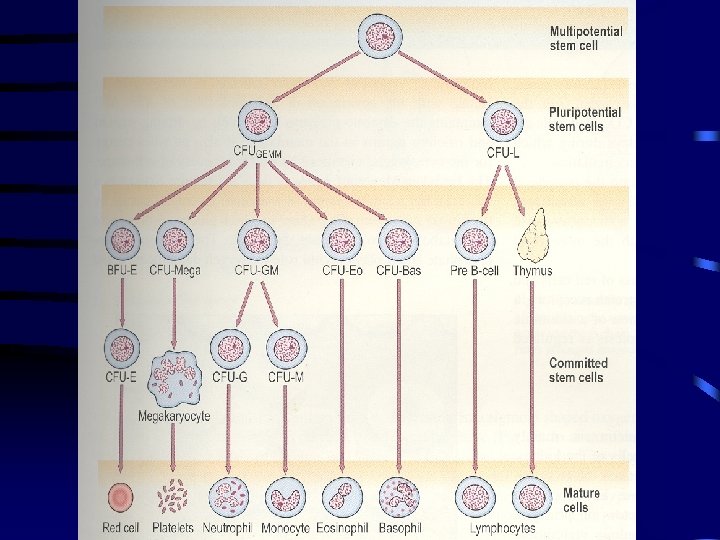

Etiology • Inherited – Fanconi’s Anemia • Acquired – Idiopathic (majority)-2/3 rd of cases – Drug : Acetazolamide, Carbamazepine, Gold, Hydantoin, Penicillin, Phenylbutazone, – Chemical – Radiation exposure – Viral illness

Pathogenesis • Immune mechanism responsible for most of the cases of Idiopathic acquired aplastic anemia • Activated Cytotoxic T cells in Blood & Bone marrow failure

Clinical Features • Signs & symptoms of : – Anemia: ………. – Bleeding: Ecchymoses , Bleeding gums, Epistaxis – Infections: Fever, Mouth ulcers
Diagnosis • Blood peripheral smear : Pancytopenia and reticulocytopenia • Bone marrow aspiration & biopsy : Hypocellular / aplastic bone marrow with increased fat spaces • Tests for underlying cause ( viral titers)

• Other causes of Pancytopenia: – Drugs, – Megaloblastic anemia – Bone Marrow infiltration or Replacement: Lymphoma, Myeloma, Acute Leukemia, Secondaries – Hyperspleenisn – SLE – Disseminated TB – PNH – Sepsis
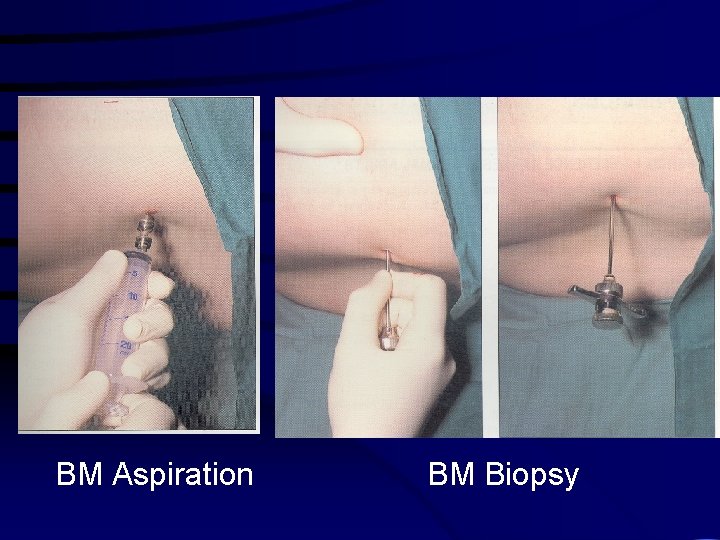
BM Aspiration BM Biopsy
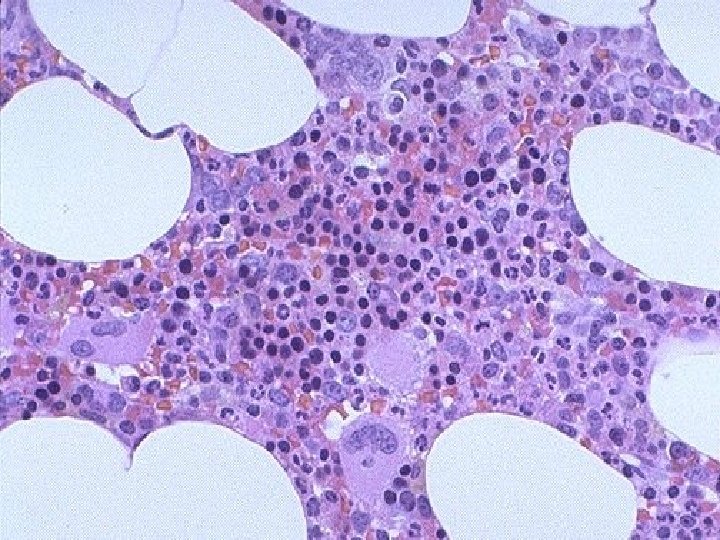
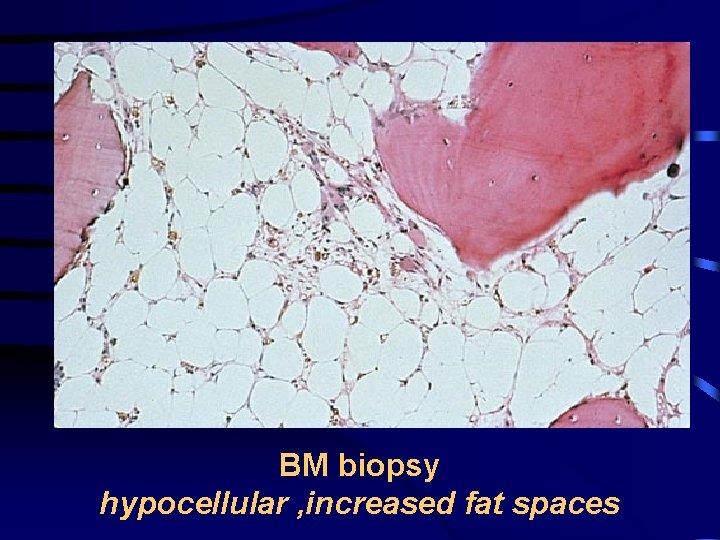
BM biopsy hypocellular , increased fat spaces

Text book Treatment • Treatment of underlying cause –if possible • Removal of cause • Supportive care – Blood & platelet transfusion – Infection: Broad spectrum antibiotics – Asepsis • Bone Marrow Transplant (SCT) – patient age <40 yrs , availability of a HLAidentical sibling marrow donor

• Immunosuppression: – Cyclosporine, – Glucocorticoids : in cong Pure Red Cell Aplasia – Antilymphocyte or Antithymocyte globulin (ALG / ATG) – Cyclophosphomide • Androgens • Thymectomy : for Adult Pure Red Cell Aplasia
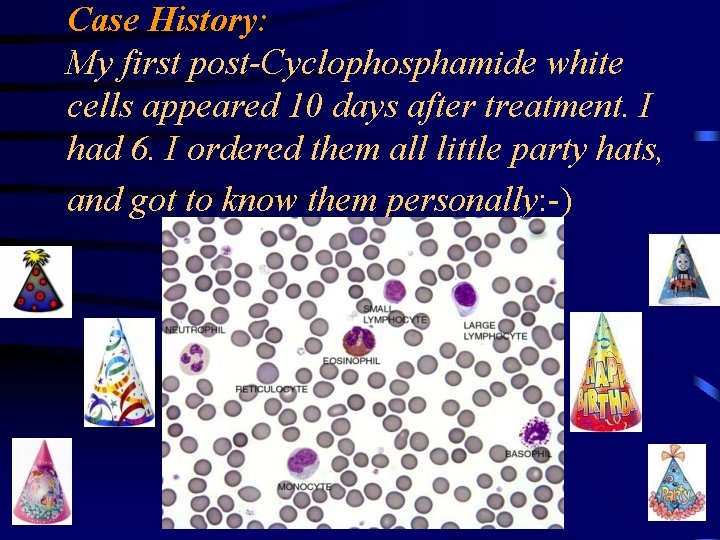
Case History: My first post-Cyclophosphamide white cells appeared 10 days after treatment. I had 6. I ordered them all little party hats, and got to know them personally: -)

Severe AA (SAA) Bad prognosis Two of three peripheral blood criteria: • Neutrophils < 500 / cmm, • Platelets < 20, 000/cmm, • Reticulocyte < 0 -0. 5%

Prognosis • Improved survival with newer treatment modalities • Relates to severity • Evolution to MDS, PNH, AML`

Agranulocytosis • Leukopenia: Decrease in Total Leukocyte Count • Neutropenia: Decrease in Neutrophil count < 1500 / micro L • Agranulocytosis: severe neutropenia < 500 neutrophils / micro L

Causes • Congenital • Drug induced: Chloramphenicol, CBZ, Carbimazole , Co-trimoxazole, Gold, Phenytoin, Sulfa drugs • Infections: – Viral-Hepatitis, Influenza, HIV – Bacterial-Typhoid, Miliary TB • Benign ( familial/racial) • Cyclical • Immune: AI, SLE, Felty’s,

Clinical Features • Mouth infection, Sore throat ( Mucositis) • Ulcers of : Mouth & throat , Skin, Anus • Features of Sepsis (Gm +ve &–ve): – Fever +/– Hypotension, – MODS • In prolonged neutropenia Fungal infections are likely to develop: Candida (Oral), Aspergillus(Pulm)
Investigations and Treatment The peripheral blood smear shows a marked decrease or absence of neutrophils. The bone marrow may show myeloid hypoplasia or absence of myeloid precursors. In many cases, the bone marrow is cellular with a maturation arrest at the promyelocyte stage. On occasion, the marrow may be hypercellular.
- Slides: 22