AP Psychology Defining Abnormal Behavior Defined as behavior

AP Psychology

Defining Abnormal Behavior Defined as behavior that is personally disturbing or disabling or culturally so deviant that others judge it as maladaptive, inappropriate or unjustifiable. • Patterns: refers to finding a collection of symptoms that tend to go together • For there to be distress and dysfunction, symptoms must be sufficiently severe to interfere with one’s daily life and well being. • Deviant: differing from the norm.

Definition of a Mental Disorder • A mental disorder is syndrome characterized by clinically significant disturbance in an individual’s cognition, emotional regulation, or behavior that reflects a dysfunction in the psychological, biological or developmental processes that underlie mental functioning. • An expectable or culturally approved response to a common stressor or loss, such as the death of a loved one is NOT a disorder.

The Medical Model • Considers abnormal behavior to be a disease that manifests as mental illness. • Psychopathology: the study of the origin, development, & manifestations of mental or behavior disorders, etiology (apparent cause & development of an illness), and prognosis, which forecasts that probable course of the illness. • In May, 2013, the American Psychiatric Association provided an updated Diagnostic and Statistical Manual of Mental Disorders (DSM-5) which classifies psychological disorders by their symptoms.

The Medical Model (cont’d) • Significant changes were made to the DSM-5 that some experts believe set “new standards for the organization of disorders & quality of evidence” (Kupfer, 2012) • Others contend that the DSM-5 is “deeply flawed” (Frances, 2013). • Either way, the DSM-5 enables mental health professionals to communicate information about individuals who suffer from mental illness & assists therapists in deciding on treatment.

Pros/Cons for Diagnosing with DSM • The DSM labels too many people as “disordered” • The borders among disorders &/or disorder and normal, appears arbitrary. • Decisions about what is a disorder seem to include value judgments – what is considered deviant or normal? • Diagnostic labels direct how we view and interpret the world, telling us which behavior and mental states to see as disordered. • The stigma/stereotypes that comes from popular cultural views of mental illness, and not from the DSM. • Using the DSM may contain the information to correct inaccurate perceptions of mental illness.

Culture-Bound Syndromes Culture-bound syndromes are disorders which only seem to exist within certain cultures; they demonstrate how culture can play a role in both causing and defining a disorder. • For Example: ü Bulimia Nervosa: binging/purging, in the United States ü Running amok: violent outbursts, in Malaysia ü Hikikomori: social withdrawal, Japan

Biopsychosocial Approach

GAD (Generalized Anxiety Disorder) Panic Disorder Agoraphobia Specific Phobia Social Anxiety Disorder OCD (Obsessive Compulsive Disorder) PTSD (Post Traumatic Stress Disorder Hoarding Disorder Anxiety Disorders

GAD: Generalized Anxiety Disorder • Emotional-cognitive symptoms: ü Chronic anxiety (worrying) not associated with any subject or object ü Anxious anticipation interferes with concentration. ü Often hypervigilant and/or irritable • Physical symptoms: ü autonomic arousal including trembling, sweating, fidgeting, agitation, & sleep disruption. • Associated with decreased availability of GABA (inhibitory neurotransmitter) ü treated with benzodiapines (sedatives) such as Valium, Xanex, & Klonapin)

Panic Disorder • Panic disorder: repeated & unexpected attacks of intense anxiety along that leads to a change in behavior to avoid future panic attacks. ü Can last from a few minutes to a few hours & have no apparent trigger.

Agoraphobia • Agoraphobia is now separate from panic disorders in the DSM-5. • Extreme avoidance of possible panic triggers agoraphobia, an anxiety disorder characterized by anxiety in situations where the sufferer perceives the environment to be difficult or embarrassing to escape, such as wide-open spaces. • The sufferer may go to great lengths to avoid those situations, in severe cases becoming unable to leave their home or safe haven.
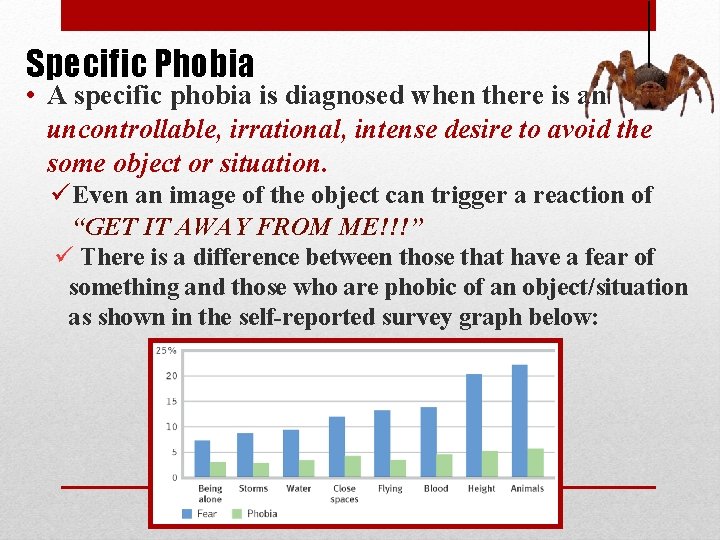
Specific Phobia • A specific phobia is diagnosed when there is an uncontrollable, irrational, intense desire to avoid the some object or situation. ü Even an image of the object can trigger a reaction of “GET IT AWAY FROM ME!!!” ü There is a difference between those that have a fear of something and those who are phobic of an object/situation as shown in the self-reported survey graph below:

Specific Phobia (cont’d) • Arachnophobia: fear of spiders • Claustrophobia: fear of enclosed spaces • Ophidiophobia: fear specifically to snakes. If other reptiles are also feared, then the more general herpetophobia is used. • Trypanophobia: fear of medical needles/injections • Agrophobia: fear of heights • Xenophobia: fear of strangers Social Anxiety Disorder (reclassified as a separate disorder in the DSM-5): refers to an intense fear of being watched and judged by others. It is visible as a fear of public appearances in which embarrassment or humiliation is possible, such as public speaking, eating, or performing.

Obsessive Compulsive Disorder (OCD) • OCD is a compound disorder of thought & behavior that interferes with everyday life. ü Obsessions: persistent, intrusive, & unwanted thoughts that are generally involve a unique topic, are often repugnant, & viewed as uncontrollable. ü Compulsions: strong feelings of “need” to repeatedly carry out an action, even though it doesn’t feel like it makes sense. ü Why OCD is considered an anxiety disorder: § obsessions can be a distraction from underlying anxiety § compulsions worsen through a cycle of negative reinforcement related to anxiety. § The OCD sufferer resists carrying out a compulsion, feels anxious, & ultimately relieves the anxiety by giving in to the compulsion. § Associated with low levels of serotonin & often treated with antidepressants.

Common OCD Behaviors Percentage of children and adolescents with OCD reporting these obsessions or compulsions There is a common pattern of Rechecking although the person already knows the door is locked. An OCD sufferer feels he/she must check again. And again.

Hoarding Disorder • Hoarding Disorder is an OCD related disorder that was newly added to the DSM-5. • Individuals with hoarding disorder: ü have difficulty discarding items due to strong perceived need to save items and/or distress associated with discarding. ü symptoms result in the accumulation possessions that congest & clutter living areas to the extent that their intended use is no longer possible or substantially impaired. ü hoarding causes clinically significant distress or impairment in social, occupational, and/or physical safety concerns for the hoarder, family & friends.

Post Traumatic Stress Disorder (PTSD) • PTSD is a result of some traumatic experience (natural disaster, war, violent crime) suffered by the victim. ü Victims relive such experiences through nightmares of flashbacks ü May have reduced involvement with the outside world, have hyper-alertness, & difficulty concentrating. ü Experience inner feelings of tension, turmoil, worry, fear, dread, angst, stress, and re-living the feelings of the trauma itself

Profile: Traumatized People who may Develop PTSD Most people experiencing trauma do NOT develop PTSD. Those that do often exhibit: • less control of the situation • Those traumatized more frequently • Those with brain differences such as a sensitive amygdala, or difficulty controlling attention. • Those who have fewer traits and behaviors of resiliency, such as finding mentors. • Those re-traumatized by intrusive debriefing. Resilience/recovery after trauma may include: ü some lingering, but not overwhelming, stress. ü finding strengths in yourself. ü finding connection with others. ü finding hope. ü seeing the trauma as a challenge that can be overcome. ü seeing yourself as a survivor.
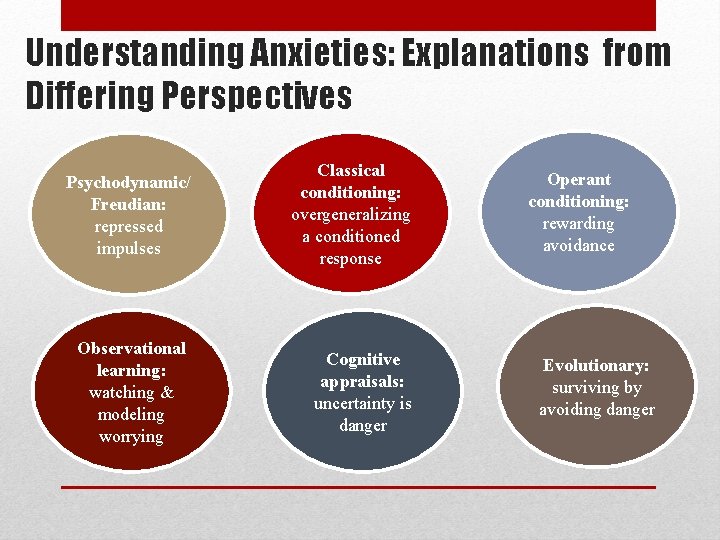
Understanding Anxieties: Explanations from Differing Perspectives Psychodynamic/ Freudian: repressed impulses Classical conditioning: overgeneralizing a conditioned response Observational learning: watching & modeling worrying Cognitive appraisals: uncertainty is danger Operant conditioning: rewarding avoidance Evolutionary: surviving by avoiding danger

Biology & Anxiety: Genes • Studies show that identical twins, even raised separately, develop similar phobias (more similar than two unrelated people). • Some people seem to have an inborn high-strung temperament, while others are more easygoing. • Temperament may be encoded in our genes • Genes regulate levels of neurotransmitters. • People with anxiety have problems with a gene associated with levels of serotonin (neurotransmitter involved in regulating sleep and mood) • People with anxiety also have a gene that triggers high levels of glutamate (excitatory neurotransmitter involved in the brain’s alarm centers)

Biology & Anxiety: The Brain • Traumatic experiences can ‘burn’ fear circuits into the amygdala; these circuits are later triggered and activated. • Anxiety disorders include overarousal of brain areas involved in impulse control and habitual behaviors. • In particular, the OCD brain shows extra activity in the anterior cingular gyrus, an • area of the brain which monitors our actions & checks for errors. PET scans reveal the high energy use in a brain of a typical person with OCD
Somatic Symptom Disorder Illness Anxiety Disorder Somatoform Disorders

Somatic Symptom Disorder (SSD) Criteria for SSD include: • having one or more chronic somatic symptoms about which they are excessively concerned, preoccupied or fearful, causing significant distress & dysfunction • physical symptoms cannot be explained by medical conditions, by direct effect of a substance

Illness Anxiety Disorder Illness anxiety disorder (previously called hypochondriasis) most commonly begins during early adulthood and appears to occur equally among men and women. • The patient's fears may derive from misinterpreting nonpathologic physical symptoms or normal bodily functions Symptoms and Signs • Patients are so preoccupied with the idea that they are or might become ill that their illness anxiety impairs social & occupational functioning & causes significant distress. • Patients may or may not have physical symptoms, but if they do, their concern is more about the possible implications of the symptoms than the symptoms themselves. Some patients examine themselves repeatedly. • Patients are easily alarmed by new somatic sensations. Some patients visit physicians frequently (care-seeking type); others rarely seek medical care (care-avoidant type).

Major Depressive Disorder (MDD) Bipolar Disorder Premenstrual Dysphoric Disorder Seasonal Affective Disorder Disruptive Mood Dysregulation Disorder Mood Disorders

Major Depressive Disorder (MDD) For a person to be diagnosed with MDD, a person must experience at least one of the first two symptoms listed below as well as 3 -4 of the rest of the symptoms for a period of about 2 weeks. • Depressed mood most of the day, and/or • Markedly diminished interest or pleasure in activities • Significant increase or decrease in appetite or weight (not by deliberate dieting) • Insomnia, sleeping too much, or disrupted sleep • Lethargy, or physical agitation • Fatigue or loss of energy nearly every day • Worthlessness, or excessive/inappropriate guilt • Daily problems in thinking, concentrating, and/or making decisions • Recurring thoughts of death and suicide

MDD Worldwide • An estimated 121 million people worldwide are currently living with some form of depression. • Of these individuals, fewer than 25% have access to adequate treatment. • The World Health Organization (WHO) considers depression the 4 th leading cause of disability worldwide; predictions suggest that by 2020, it will be the 2 nd leading cause of disability worldwide. • WHO reports that 60 -80% of all depression cases can be effectively treated with brief, structured forms of psychotherapy and antidepressant medications.

BIPOLAR DISORDER • Once, referred to as manic-depressive disorder • Has two polar opposite moods: mania & depression • • • Contrasting Symptoms Depressed mood: stuck, Mania: euphoric, giddy, feeling “down, ” with: easily irritated, with: exaggerated pessimism • exaggerated optimism social withdrawal • Hyper-sociality and lack of felt pleasure sexuality inactivity and no initiative • delight in everything difficulty focusing • impulsivity and fatigue and excessive overactivity desire to sleep • racing thoughts; the mind won’t settle down • little desire for sleep

BIPOLAR DISORDER (cont’d) • Rapid Cycling: characterized by short periods of mania followed by deep depression, usually of a longer duration. • Lithium carbonate has been successful in bringing symptoms under control • Many famous & successful people have lived with the ups & downs of bipolar disorder. Some speculate that the depressive periods gave them ideas & the manic episodes provided the creative energy.

Disruptive Mood Dysregulation Disorder (DMDD) • DDMD is a relatively new diagnosis in the field of mental health. • Some of these children were previously diagnosed with bipolar disorder, even though they often did not have all the signs and symptoms. • Research evidences that children with DMDD usually do not go on to have bipolar disorder in adulthood. They are more likely to develop problems with depression or anxiety. The symptoms of DMDD include: • Severe temper outbursts at least three times a week • Sad, irritable or angry mood almost every day • Reaction is bigger than expected • Child must be at least six years old • Symptoms begin before age ten • Symptoms are present for at least a year • Child has trouble functioning in more than one place

Premenstrual Dysphoric Disorder (PMDD)
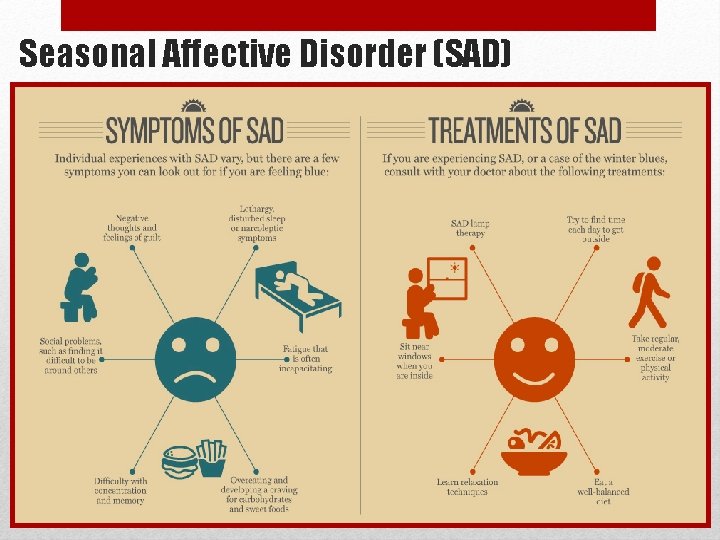
Seasonal Affective Disorder (SAD)

Suicide & Self-Injury • Every year, 1 million people commit suicide, giving up on the process of trying to cope and improve their emotional well-being. • This can happen when people feel frustrated, trapped, isolated, ineffective, and see no end to these feelings. • The numbers for suicide attempts each year increase when we consider suicidal gestures, acts that look like suicide attempts, without clear intent to succeed. • The numbers get much larger if we consider those who have had thoughts about suicide or wanting to be dead. • Non-suicidal self-injury may be a call for help or a means of self punishment. ü Such self-injury can be a distraction from emotional pain, an excuse to cry when emotional pain doesn’t feel justified, or to get the endorphin response which can come especially with repeated self-cutting.

Evolutionary Perspective on Depression § Depression, in its milder, nondisordered form, may have had survival value. § Under stress, depression is social-emotional hibernation. It allows humans to: § conserve energy. § avoid conflicts and other risks. § let go of unattainable goals. § take time to contemplate.
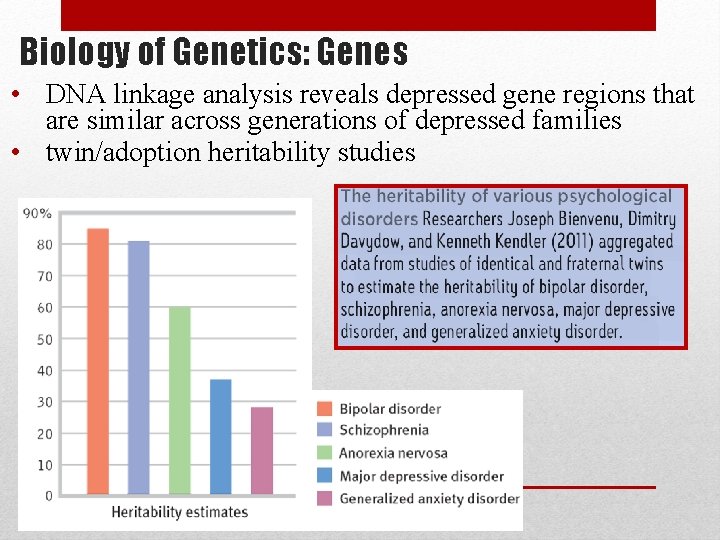
Biology of Genetics: Genes • DNA linkage analysis reveals depressed gene regions that are similar across generations of depressed families • twin/adoption heritability studies
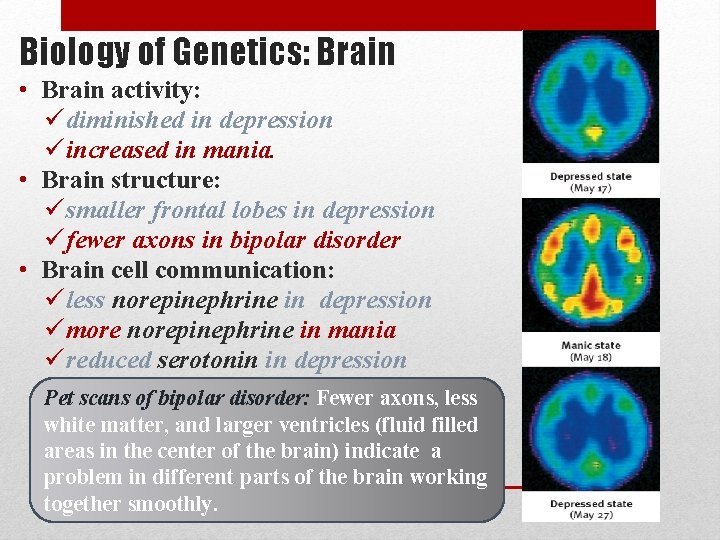
Biology of Genetics: Brain • Brain activity: ü diminished in depression ü increased in mania. • Brain structure: ü smaller frontal lobes in depression ü fewer axons in bipolar disorder • Brain cell communication: ü less norepinephrine in depression ü more norepinephrine in mania ü reduced serotonin in depression Pet scans of bipolar disorder: Fewer axons, less white matter, and larger ventricles (fluid filled areas in the center of the brain) indicate a problem in different parts of the brain working together smoothly.

Treating Depression: Using Knowledge of Biology • Keeping neurotransmitter levels higher with the use of antidepressant medications could improve communication between the nerve cells which may strengthen circuits in the brain regulating mood. ü Use of Wellbutrin to reduce depression by increasing norepinephrine ü Prozac, Zoloft, Paxil & Celexa (SSRIs: selective serotonin reuptake inhibitors) increase the availability of serotonin. • Increase serotonin levels with exercise • Reduce brain inflammation with a healthy diet (Mediterranean diet that promotes the use of olive & fish oils). • Decrease alcohol use which only leads to changes in the brain but also problems with behavior & coping skills

Depression: Social-Cognitive Approach
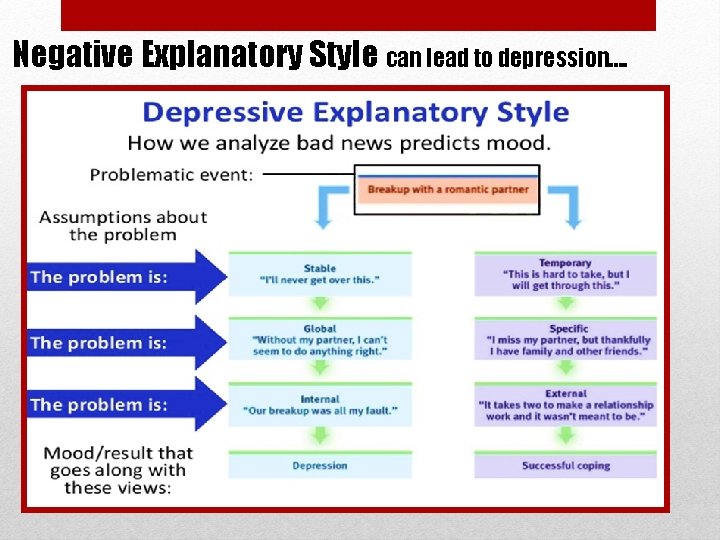
Negative Explanatory Style can lead to depression….
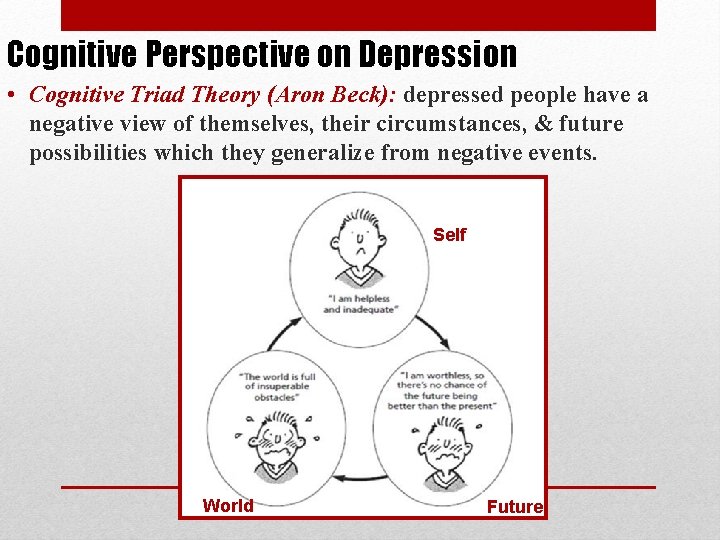
Cognitive Perspective on Depression • Cognitive Triad Theory (Aron Beck): depressed people have a negative view of themselves, their circumstances, & future possibilities which they generalize from negative events. Self World Future

Other Perspectives on Depression • Psychoanalytic Perspective: due to early loss of or reject by a parent, resulting in depression when the person experiences losses later in life & turns anger inward. • Behavioral Perspective: depressed people elicit negative reactions from others, resulting in the maintenance of depressed behaviors.

Schizophrenia

Schizophrenia • Once divided into subtypes, the DSM-5 has discontinued those groupings, judging that they have low reliability & validity In schizophrenia, the mind is split from reality; there is a split from one’s own thoughts so that they appear as hallucinations. • Characterized by psychosis (lack of touch with reality)

Positive & Negative Symptoms of Schizophrenia

Symptoms of Schizophrenia Thinking & Speaking • Disorganized speech: includes the “word salad” of loosely associated phrases • Delusions (illusory beliefs): often bizarre, most common are delusions of grandeur &/or persecution • Problems with selective attention: difficulty filtering thoughts & choosing which thoughts to believe &/or say out loud Disturbed Perceptions • Hallucinations: perceptual experiences not shared by others • Hearing voices no one else hears: often with upsetting or shameful content, the most common form of hallucinations • Hallucinations can also be visually, tactile, olfactory, or gustatory.

Symptoms of Schizophrenia (cont’d) Inappropriate Emotions • Odd & socially inappropriate responses: such as looking bored or amused while hearing of a death • Flat affect: facial/body expression is “flat” with no visible emotional content • Impaired perception of emotions: such as not “reading” others’ intentions and feelings Inappropriate Behaviors Socially inappropriate behavior can result from: • errors in social perception. • disorganized, unfiltered thinking. • delusions and hallucinations. The schizophrenic body exhibits symptoms such as: • Repetitive behaviors: such as rocking and rubbing. • Catatonia: sitting motionless and unresponsive for hours.

Facts about Schizophrenia Typically, schizophrenic symptoms appear at the end of adolescence and in early adulthood, later for women than for men. • Nearly 1 in 100 people develop schizophrenia, slightly more men than women. • Between one-third to one-half of all homeless adults have schizophrenia. • Studies have indicated that 25% of those having schizophrenia recover completely, 50% are improved over a 10 -year period, 25% do not improve over time. • 50% of people diagnosed with schizophrenia have received no treatment. • Treatment can include not only medication but psychosocial rehabilitation, exercise, psychotherapy, supervised group homes, case management, daily living skills support, and vocational programs.
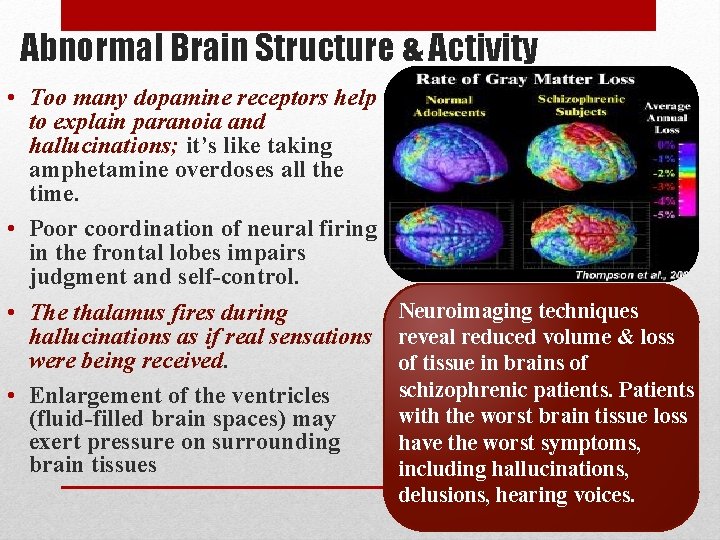
Abnormal Brain Structure & Activity • Too many dopamine receptors help to explain paranoia and hallucinations; it’s like taking amphetamine overdoses all the time. • Poor coordination of neural firing in the frontal lobes impairs judgment and self-control. • The thalamus fires during hallucinations as if real sensations were being received. • Enlargement of the ventricles (fluid-filled brain spaces) may exert pressure on surrounding brain tissues Neuroimaging techniques reveal reduced volume & loss of tissue in brains of schizophrenic patients. Patients with the worst brain tissue loss have the worst symptoms, including hallucinations, delusions, hearing voices.

The Genetic Basis for Schizophrenia • The lifetime risk of developing schizophrenia increases with genetic similarity • Schizophrenia tends to cluster in families • If one identical twin develops schizophrenia, the risk for the other twin also developing schizophrenia is 48% • Adoption studies have consistently shown that if either biological parent has schizophrenia, the adopted child is at greater risk for developing schizophrenia • Research has found many genes that are associated with schizophrenia, but it may take environmental factors to turn these genes on
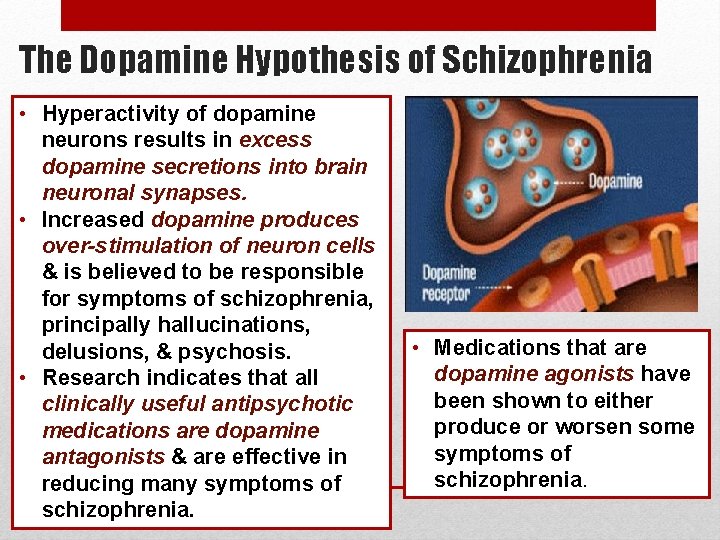
The Dopamine Hypothesis of Schizophrenia • Hyperactivity of dopamine neurons results in excess dopamine secretions into brain neuronal synapses. • Increased dopamine produces over-stimulation of neuron cells & is believed to be responsible for symptoms of schizophrenia, principally hallucinations, delusions, & psychosis. • Research indicates that all clinically useful antipsychotic medications are dopamine antagonists & are effective in reducing many symptoms of schizophrenia. • Medications that are dopamine agonists have been shown to either produce or worsen some symptoms of schizophrenia.

Stress-Vulnerability Model of Schizophrenia • Similar to the diathesis-stress model which suggests biological predisposition for schizophrenia can be triggered by stressful life experiences • In addition to biological vulnerability & environmental stress, the stress-vulnerability also includes a person’s coping skills.

Antisocial Avoidant Borderline Narcissistic Obsessive-Compulsive (OCPD) Schizotypal Personality Disorders

Personality Disorders • Individuals diagnosed with personality disorders have longstanding, maladaptive thought & behavior patterns that are difficult for others to cope with, may be harmful, &/or illegal. • Impair the patient’s social functioning, but the person does NOT experience anxiety, depression, or delusions • Personality Disorders are generally characterized by: ü Distorted thinking patterns; Problematic emotional responses ü Over- or under-regulated impulse control; Interpersonal difficulties • Usually become evident by adolescent or early adulthood • The DSM 5 has changed the classification to include 6 distinct groups of personality disorders.

Antisocial Personality Disorder • Antisocial personality disorder refers to acting impulsively or fearlessly without regard for others’ needs and feelings. • Violate other people’s rights without guilt/remorse. Manipulative, exploitive, self-indulgent, can be charming. May commit large number of violent crimes. (more common in males). • May exhibit symptoms of Deceitfulness conduct disorder as a child Disregard for safety of self or others The diagnostic criteria include a pattern of violating the rights of others since age 15, including three of these: Irritability & Aggressiveness Failure to conform to social norms Lack of remorse Impulsivity and failure to plan ahead Irresponsibility regarding jobs, family, and money

Risk factors for Antisocial Personality Disorder • About half of children with persistent antisocial behavior develop lifelong Antisocial Personality Disorder Which children are at risk? • those who in preschool were impulsive, uninhibited, unconcerned with social rewards, & low in anxiety. • those who endured child abuse, and/or were inconsistent, unavailable Biological Risk Factors • Antisocial or unemotional biological relatives increases risk (some genes have been identified). § Risk factors: body-based fearlessness, lower levels of stress hormones, & low physiological arousal in stressful situations § Fear conditioning is impaired. § Reduced prefrontal cortex tissue leads to impulsivity. § Substance dependence is more likely.

Avoidant Personality Disorder • Avoidant personality disorder is an enduring pattern of feelings of inadequacy, hypersensitivity to being negatively evaluated by others, extreme shyness, & inflexibility that begins by early adulthood. • Results in significant distress or impairment in occupational, social, or other areas of functioning. • Generally desire social connection, but are crippled by a sense of personal inadequacy and intense fears of social rejection. • Avoids occupational activities involving significant interpersonal contact, due to fears of criticism, disapproval, or rejection

Borderline Personality Disorder

Narcissistic Personality Disorder Symptoms include being unrealistically self-important, manipulative, lacking empathy, expecting special treatment, can’t take criticism, arrogant & haughty, envious, requiring admiration, having power fantasies & an extreme sense of entitlement.

Obsessive Compulsive Personality Disorder (OCPD) • OCPD is a syndrome that characterizes a person’s overall orientation towards life where a person is often described as rigid, inflexible and/or perfectionist. • Demands everything be organized according to a particular system, loves rules, regulations, order, & control • OCPD individuals often have difficulty with people who can’t or won’t abide by their standards. • Often undertake projects with a great deal of initial energy & zeal only to leave them unfinished when obstacles &/or imperfections arise. • More common among men; most psychologists agree that it cannot be accurately diagnosed until about 18 years of age

Schizotypal Personality Disorder • Described as odd/eccentric; usually have few, if any, close relationships. • Often misinterpret others' motivations & behaviors; leads to distrust of others • Often dress in peculiar ways, believe in special powers, & have odd styles of speech • Have excessive social anxiety & flat emotions • This disorder can easily be confused with schizophrenia. While people with schizotypal personalities may experience brief psychotic episodes with delusions or hallucinations, they are not as frequent, prolonged or intense as in schizophrenia. • People with schizotypal personality usually can be made aware of the difference between their distorted ideas & reality.

Dissociative Amnesia Dissociative Identity Disorder (DID) Dissociative Disorders

Dissociative Disorders (DID) • Dissociation refers to a separation of conscious awareness from thoughts, memory, bodily sensations, feelings, or even from identity. • Dissociation can serve as a psychological escape from an overwhelmingly stressful situation • Someone with a dissociative disorder escapes reality in ways that are involuntary & unhealthy. • They experience a disconnection & lack of continuity between thoughts, memories, surroundings, actions and identity. • Symptoms can range from amnesia to alternate identities & usually develop as a reaction to trauma, helping to keep difficult memories at bay. • Times of stress can worsen symptoms, making them more obvious & cause problems with functioning in everyday life. • Treatment for dissociative disorders may include psychotherapy and medication. • Although treating dissociative disorders can be difficult, people learn new ways of coping and lead healthy, productive lives.

Dissociative Amnesia • The main symptom is memory loss that is more severe than normal forgetfulness and that can't be explained by a medical condition. • You can't recall information about yourself or events and people in your life, especially from a traumatic time. • Dissociative amnesia can be specific to events in a certain time, such as intense combat, or more rarely, can involve complete loss of memory about yourself. • It may sometimes involve travel or confused wandering away from your life (dissociative fugue). An episode of amnesia may last minutes, hours, or, rarely, months or years.

Dissociative Identity Disorder (D. I. D) • Formerly known as multiple personality disorder • Characterized by "switching" to alternate identities. • You may feel the presence of one or more other people talking or living inside your head, and you may feel as though you're possessed by other identities. • Each of these identities may have a unique name, personal history and characteristics, including obvious differences in voice, gender, mannerisms and even such physical qualities. • Differences also may exist in how familiar each identity is with the other personalities. • Often accompanied by dissociative amnesia According to the DSM 5, diagnosis should include: ü transitions in identity may be observable by others or selfreported. ü Reports of recurrent gaps in recall for everyday events, not just for traumatic experiences.

D. I. D. (cont’d) Differing Perspectives on DID: • Psychodynamic: repression of anxiety &/or trauma caused by Evidence for D. I. D: disturbances in home life. • Different personalities have • Behavioral: learned coping evolved with: response with production of symptoms in order to obtain ü different brain wave patterns. rewards or relief from stress ü different left-right handedness. • Sociocultural: symptoms as ü different visual acuity and eye product of social reinforcement muscle balance patterns. • Social Learning: symptoms are part of an intricate role playing • Patients with D. I. D. also show heightened activity in areas of the brain associated with managing and inhibiting traumatic memories.
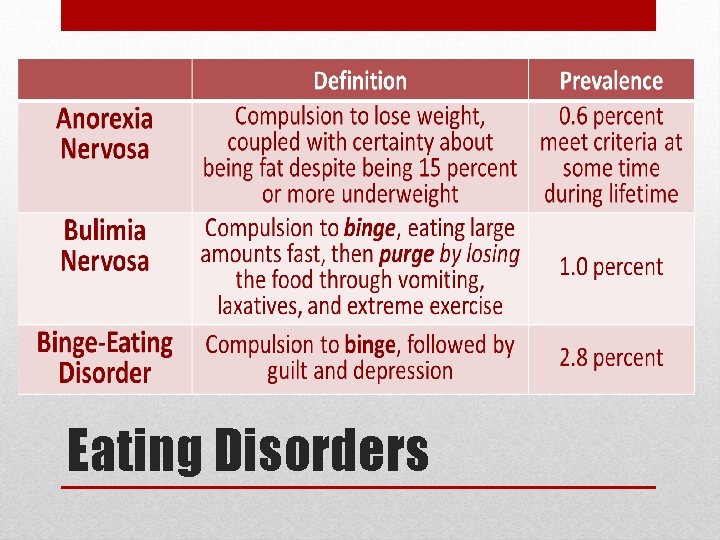

Eating Disorders

Eating Disorders: Risk Factors May Involve: • unrealistic body image and extreme body ideal. • a desire to control the body through food when all else is out of control. • cycles of depression. • health problems. Family factors: • having a mother focused on her weight & on child’s appearance and weight • negative self-evaluation in the family • for bulimia, if childhood obesity runs in the family • for anorexia, if families are competitive, high-achieving, and protective Cultural factors: • unrealistic ideals of body appearance
- Slides: 68