anxiety disorders probably among most common symptoms for

anxiety disorders probably among most common symptoms for which drug pharmacotherapy is prescribed
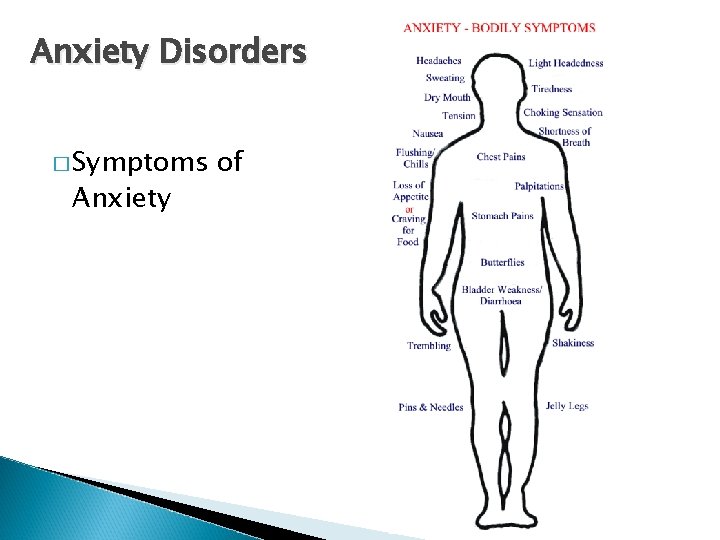
Anxiety Disorders � Symptoms Anxiety of

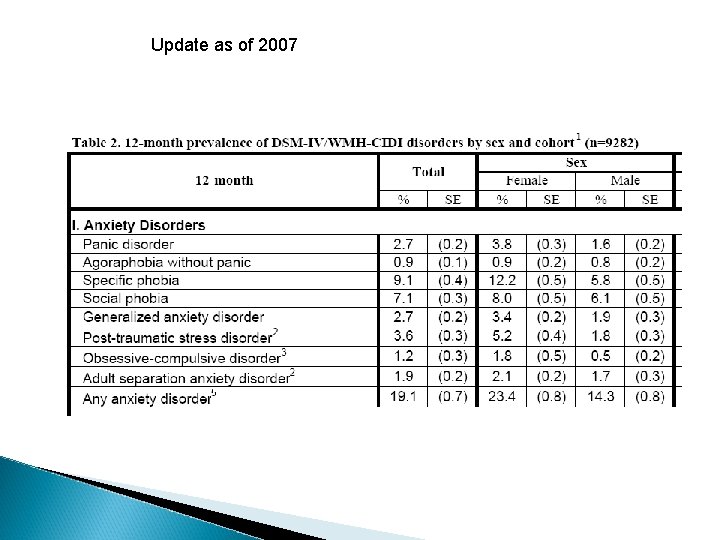
Update as of 2007

Some results from National Comorbidity Study 1 in 4 people have met the diagnostic criteria for at least 1 anxiety disorder 12 month prevalence rate of 19. 1% women have higher prevalence rate than men affecting approximately 40 million American adults ages 18 and older May occur with variety of medical or psychiatric illness

Medical conditions that could be diagnosed as anxiety– ◦ symptoms similar to anxiety disorders �hyperthyroidism �hypothyroidism �vitamin b 12 deficiency �certain tumors produce E �certain brain lesions (postenecphalitic states) �cardiac arrhthymia – can produce signs �hypoglycemia

Drugs that can induce or worsen anxiety stimulants anorectics analgesics anticholinergics hallucinogens sympathomimetics steroids neuroleptics caffeine fenfluramine salicyclates diphenhydramine cannabis ephedrine prednisone haloperidol

3 major NT associated with anxiety � GABA � NE � 5 HT

OCD � now recognized as commonly occurring disorder affecting ~ 2% of the population � 1 in 50 of US population � symptoms worsen when coexisting symptoms of depression or other comorbid conditions exist � depression is found in 1/3 of patients upon presentation and 2/3 in lifetime

Biological Theories � Developed from preclinical studies with animal models � Peripheral SNS activation ◦ Peripheral NS activity are not peculiar to anxiety disorders; not necessarily correlated with subjective experience of anxiety although there are clear exceptions!!!!

Animal models Social interaction test Plus maze Novelty stress Anxiolytic drugs

Treatments for Anxiety Disorders � Probably ◦ alcohol first treatment – � first agent introduced first as sedative and soon thereafter as hypnotic ◦ bromide – mid 19 th century � Barbital – introduced in 1903 ◦ phenobarbital in 1912 ◦ over 2500 barbiturates synthesized and tested in early 1900’s ◦ ~ 50 distributed commercially

�Currently – most commonly employed medicinal treatments for clinical anxiety are antidepressants (SSRIs and SNRIs) BZ and buspirone

Benzodiazepines �Benzodiazepine (BZD) = a drug of a specific chemical structure. ◦ Thus, drugs are structurally, not pharmacologically, classified.
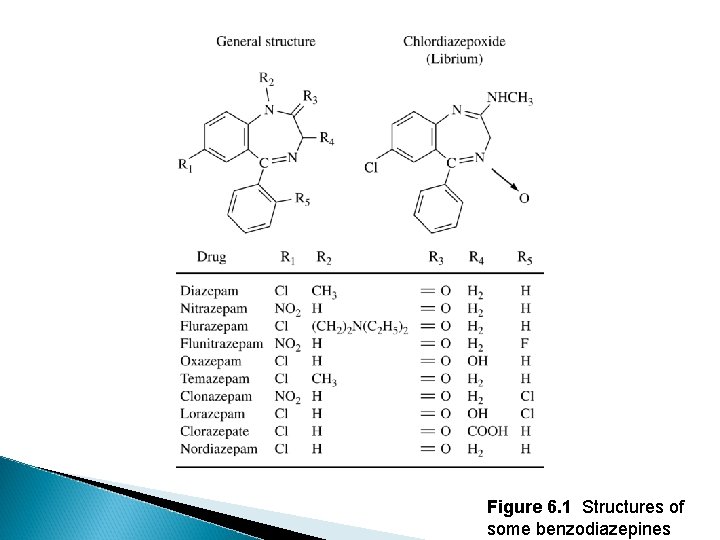
Figure 6. 1 Structures of some benzodiazepines

Benzodiazepines �Benzodiazepine (BZD) = a drug of a specific chemical structure. ◦ Thus, drugs are structurally, not pharmacologically, classified. �All are GABA-agonists, increasing chloride influx into neurons. �Any drug that activates the benzodiazepine receptor is a benzodiazepine receptor agonist (BZRA).

BZ � BZD – ◦ chlordiazepoxide (Librium) – introduced in 1961 and ushered in use of BZ ◦ all BZ have sedative, anxiolytic, anticonvulsant, muscle relaxants and amnestic effects �currently ~ 15 BZ available on the market ◦ most that have reached the marketplace were selected for high anxiolytic potency (relative to depression of CNS)

Examples of Available Benzodiazepines � Diazepam (Valium) � Chlordiazepoxide (Librium) � Flurazepam (Dalmane) � Chlorazepate (Tranxene) � Lorazepam (Ativan) � Quazepam (Dormalin) Clonazepam (Klonopin) Oxazepam (Serax) Temazepam (Restoril) Triazolam (Halcion) Alprazolam (Xanax) Estazolam (Pro. Som) Halazepam (Paxipam) Midazolam (Versed)

Pharmacokinetics � Several BZ are first biotransformed into intermediate, pharmacologically active products � metabolized extensively by CYP 450 enzymes
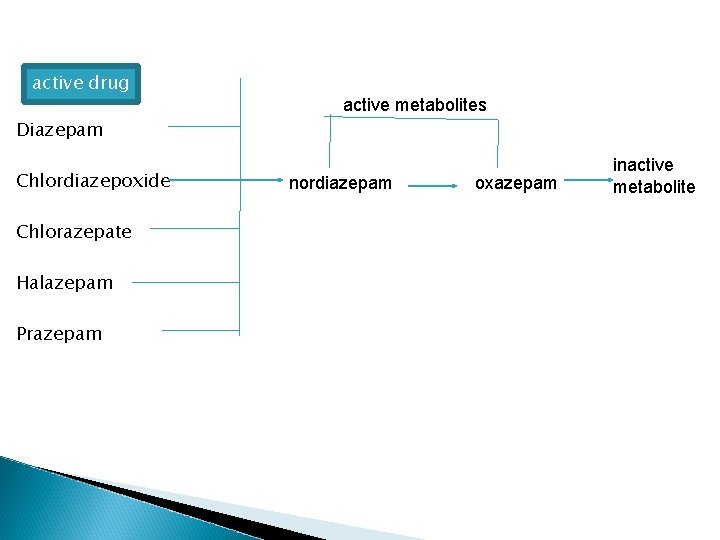
active drug active metabolites Diazepam Chlordiazepoxide Chlorazepate Halazepam Prazepam nordiazepam oxazepam inactive metabolite

Absorption, Fate and Excretion of BZ � drugs active at BZ site divided into 4 categories (based on ½ life) ◦ ultra short acting ◦ short-acting (1/2 life less than 6 hours) – includes triazolam, zopiclone ◦ intermediate (1/2 life – 6 – 24 hr) ◦ long-acting (greater than 24 hr) – flurazepam, diazepam, quazepam

Some long-acting BZ Trade Name Generic Dosage f Active metabolite ½ life Valium diazepam Oral, p Yes Nordiazepam 24 (20 -50) 60 (50 -100) Librium chlordiazepoxi Oral de Yes nordiazepam 10 (8 -24) 60 (50 -100) Dalmane flurazepam yes 80 (70 -160) oral
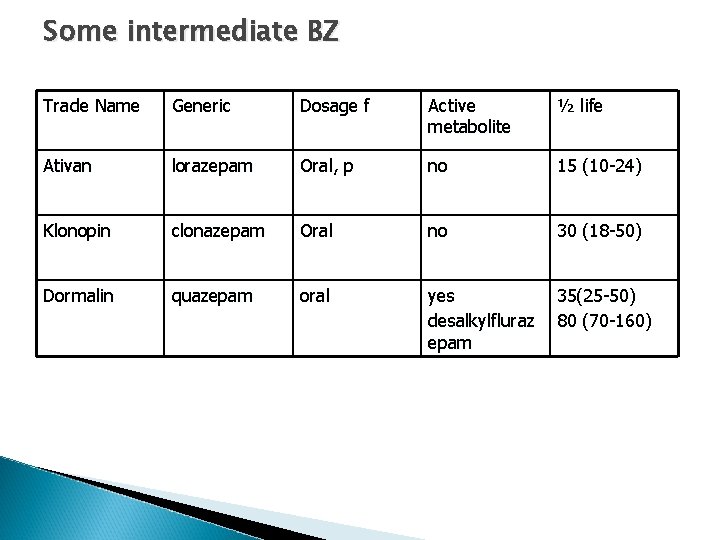

Some intermediate BZ Trade Name Generic Dosage f Active metabolite ½ life Ativan lorazepam Oral, p no 15 (10 -24) Klonopin clonazepam Oral no 30 (18 -50) Dormalin quazepam oral yes desalkylfluraz epam 35(25 -50) 80 (70 -160)
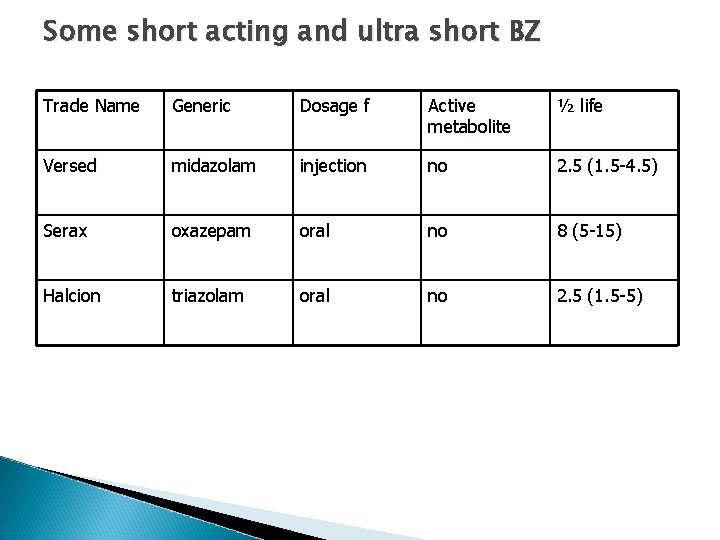
Some short acting and ultra short BZ Trade Name Generic Dosage f Active metabolite ½ life Versed midazolam injection no 2. 5 (1. 5 -4. 5) Serax oxazepam oral no 8 (5 -15) Halcion triazolam oral no 2. 5 (1. 5 -5)

Benzodiazepines: Current Uses �Treatment of debilitating anxiety �Treatment of insomnia �Treatment of muscle spasm and “tension” �Symptomatic treatment of panic attacks �Nonspecific treatment of anxiety that may accompany other psychological disorders �Treatment of alcohol dependence �presurgical txt

BZ mechanisms
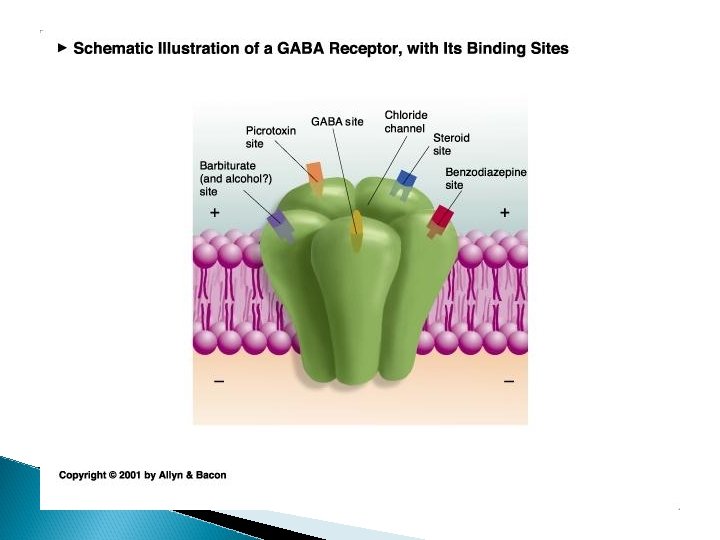

potential advantages of BZ � frequent use is likely a reflection of their effectiveness, their rapid onset of anxiolytic effect and their tolerability � therapeutic tolerance? ◦ probably not

Advantages of BZs �SAFE! Very low toxicity, unlike barbiturates or alcohol �Do not induce metabolic enzymes; do not accelerate their own metabolism. �Act on CNS and peripheral organs (e. g. , liver) are not impaired.

Negative Issues with BZ � BZ side effects – ◦ most common include sedation and impairment of cognition and fine motor function (motor appears more impaired), ◦

Motor impairments �BZDs, even at low, normal clinical doses impair real-world driving performance. ◦ 1 mg alprazolam impaired driving comparable to a BAC of 0. 15 mg % ◦ Women more affected than men ◦ Significant detrimental effects on driving, memory, and divided attention ◦ Clinical implications are enormous – who is responsible? � Source: Verster, et al. (2002). Effects of alprazolam on driving ability, memory functioning and psychomotor performance: A randomized, placebo-controlled study. Neuropsychopharmacology, 27, 260– 269.

CONCLUSION: Benzodiazepine users were found to be at a significantly increased risk of motor vehicle collisions compared to nonusers, and these differences may be accounted for by a difficulty in maintaining road position.

� BZ side effects – ◦ most common include sedation and impairment of cognition and fine motor function (motor appears more impaired), ◦ in elderly (particularly) – common cause for confusion, delirium and falls (with fractures)
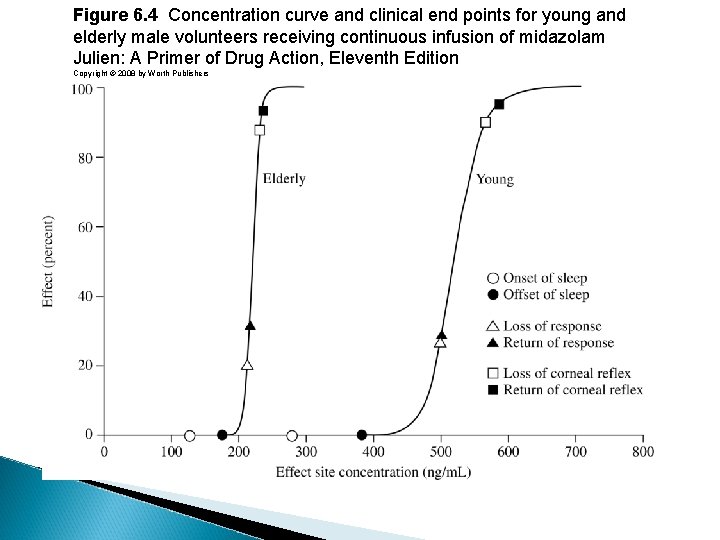
Figure 6. 4 Concentration curve and clinical end points for young and elderly male volunteers receiving continuous infusion of midazolam Julien: A Primer of Drug Action, Eleventh Edition Copyright © 2008 by Worth Publishers

Am J Geriatr Psychiatry. 2008 Aug; 16(8): 686 -92. CONCLUSIONS: Benzodiazepine exposure in the elderly increases the risk of hip fractures. This is true even with modest dosage, short-acting agents and short-term exposures. Clinicians should prescribe benzodiazepines judiciously with the elderly to minimize drug-related hip fractures.

� BZ side effects – ◦ most common include sedation and impairment of cognition and fine motor function (motor appears more impaired), ◦ in elderly (particularly) – common cause for confusion, delirium and falls (with fractures) ◦ confusion, anterograde amnesia

Disadvantages of Benzodiazepines Amnesia �more likely observed if high doses; or adm iv �Anterograde �Primarily for episodic memory �May be useful for presurgical preparation. �May not be a problem if taken for sleep.

Other disadvantages �Dependence/withdrawal �Abuse �Potentiation of other sedative-hypnotics

Other issues � BZ withdrawal – cannot discontinue suddenly – � those predisposed to substance abuse have increased risk for BZ abuse � lack antidepressant efficacy and can induce or amplify comorbid depression � rebound anxiety

Guidelines � 1998 – advocates initiating pharmacotherapy for panic disorders with SSRI and BZ for acute anxiety management rather than long-term treatment � BZ continue to be prescribed frequently for a variety of anxiety disorders (Stevens and Pollack, 2005 review) � alprazolam agent – single most prescribed anxiolytic

Nonbenzodiazepine BZRAs � Not anxiolytic � Most bind to GABA 1 A receptor. � Currently 3 are on the market.

Nonbenzodiazepine BZRAs – or 2 nd generation anxiolytics �Currently 3 on the market: ◦ Zolpidem (Ambien): ◦ Zaleplon (Sonata): ◦ Eszopiclone (Lunesta):

BZ like � zolpidem (Ambien) ◦ binds to GABAA receptor ◦ acts mostly as a sedative (rather than anxiolytic) ◦ Half-life of 2– 2. 5 hours. ◦ Overdoses not fatal even at very high doses.

Partial agonists � definition: binds and activates a receptor, but with only partial efficacy at the receptor relative to a full agonist � partial GABAA agonist � advantage of partial agonist ◦ less withdrawal; less physical dependence;

� Zaleplon (Sonata) ◦ non. BZ agonist binding to GABA 1 A ◦ released late 1999 for clinical use as a hypnotic drug ◦ ½ life is less than 1 hr; only about 30% reaches bloodstream ◦ does not appear to affect psychomotor function, driving… the next morning

�Eszopiclone (Lunesta) ◦ Similar to zolpidem and traditional BZs. ◦ Long half life (5– 7 hours), increased risk of nextday sedation. ◦ Only non-benzodiazepine BZRA approved for longer-term use in treating insomnia.

These are not without their own issues – “Sleep Driving” �FDA 2007 requirement of warning of “sleep driving”

These are not without their own issues – “Sleep Driving” �FDA 2007 requirement of warning of “sleep driving” ◦ Driving while not fully awake and having no memory of the event. ◦ Extends to making phone calls, preparing and eating food, etc? �Blood levels of drug sufficient to block memory formation in absence of sleep state.

other options for treating anxiety? � beta blockers ◦ propanolol – reduces physiological symptoms of arousal (useful for subtypes of anxiety like performance anxiety, social anxiety, etc)

Serotonin Receptor Agonists as Anxiolytics � Anxiety may result, in part, from defects in serotonin transmission. � All six clinically available SSRI antidepressants are widely prescribed for anxiety disorders. ◦ Actually considered to be first choice drugs for anxiety.

buspirone (Bu. Spar) � unique class of anxioselective drugs � does not cause sedation, hypnosis, anticonvulsant effects or muscle relaxation � takes 3 – 6 weeks to achieve maximum anxiolytic effects

Buspirone (Bu. Spar) � mechanism of action of buspirone is not clear � In vitro preclinical studies - has a high affinity for serotonin (5 -HT 1 A) receptors (probably works on both pre and post) � has no significant affinity for BZ receptors � doesn’t affect GABA binding � may bind to DA 2?

antidepressants � SSRIs and SNRIs ◦ first line treatment for GAD ◦ paroxetine (Paxil, Paxil CR), escitalopram (Lexapro) ◦ venlafaxine (Effexor XR) – first FDA approved drug for both depression and GAD �both an SSRI and an SNRI

other antidepressants � tricyclic antidepressants ◦ can be used for treating panic disorders �imipramine, desipramine, amitrypityline, trazadone � MAO inhibitors -

Some antiepileptic agents �gabapentin (Neurontin) ◦ anticonvulsant – used to treat social anxiety disorder �Retigabine – ◦ novel antiepileptic drug that opens K+ channels�reduces anxiety in rodent models �pregabalin ◦ GABA agonist – ◦ may be useful for GAD ◦ new agent -

http: //www. neurotransmitter. net/newdrugs. html

alternative txt for insomnia

Alternatives to Benzodiazepines � Ramelteon: agonist a selective melatonin receptor ◦ Melatonin is regulated by pineal gland on a 24 -hour cycle, with levels increasing towards bedtime. ◦ Nonaddictive

OCD treatment � antidepressants have emerged as more effective treatments � clomipramine (Anafranil) and SSRIs � buspirone – more often used as adjunct with SSRIs

PTSD � increasingly recognized as prevalent psychiatric disorder � antidepressants ◦ TCAs and MAOIs; maybe SSRIs
- Slides: 60