Antithrombotic Therapy in Patients with Atrial Fibrillation and

Antithrombotic Therapy in Patients with Atrial Fibrillation and Acute Coronary Syndrome Treated Medically or with Percutaneous Coronary Intervention or Undergoing Elective Percutaneous Coronary Intervention Stephan Windecker on behalf of the AUGUSTUS Investigators
Background • AUGUSTUS trial — AF patients with recent ACS or PCI • Apixaban without aspirin resulted in – less bleeding – fewer hospitalizations – no significant differences in ischemic events than regimens that included a VKA, aspirin, or both


Background • AUGUSTUS trial — AF patients with recent ACS or PCI • Apixaban without aspirin resulted in – less bleeding – fewer hospitalizations – no significant differences in ischemic events than regimens that included a vitamin K antagonist, aspirin, or both • The safety and efficacy of antithrombotic regimens may differ between patients with AF who have ACS treated medically or with PCI, and those undergoing elective PCI

Pre-Specified Analysis • Using a 2× 2 factorial design apixaban was compared with VKA and aspirin with placebo in patients with AF who had ACS or were undergoing PCI and were receiving a P 2 Y 12 inhibitor • We explored bleeding, death, and hospitalization as well as death and ischemic events by antithrombotic strategy in three mutually exclusive, pre-specified subgroups: – Patients with ACS treated medically (ACS Medical) – Patients with ACS treated with PCI (ACS PCI) – Patients undergoing elective PCI (Elective PCI)
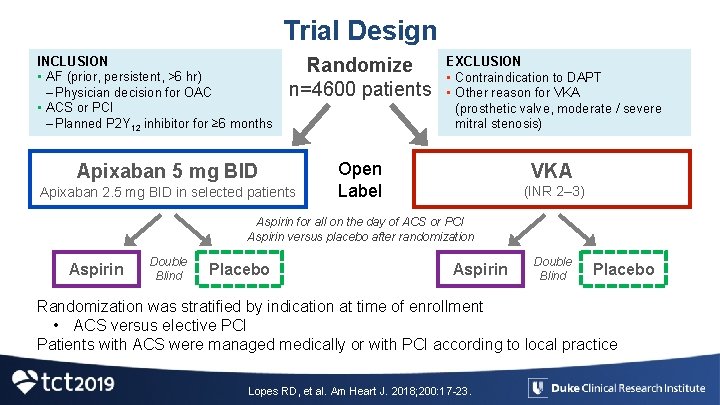
Trial Design INCLUSION • AF (prior, persistent, >6 hr) – Physician decision for OAC • ACS or PCI – Planned P 2 Y 12 inhibitor for ≥ 6 months Randomize n=4600 patients EXCLUSION • Contraindication to DAPT • Other reason for VKA (prosthetic valve, moderate / severe mitral stenosis) Open Label VKA Apixaban 5 mg BID Apixaban 2. 5 mg BID in selected patients (INR 2– 3) Aspirin for all on the day of ACS or PCI Aspirin versus placebo after randomization Aspirin Double Blind Placebo Randomization was stratified by indication at time of enrollment • ACS versus elective PCI Patients with ACS were managed medically or with PCI according to local practice Lopes RD, et al. Am Heart J. 2018; 200: 17 -23.

Trial Organization EXECUTIVE COMMITTEE John Alexander (Chair) DATA SAFETY MONITORING BOARD Lars Wallentin (Chair) Renato Lopes (PI) Robert Harrington Roxana Mehran (USA) Stuart Pocock Christopher Granger (USA) Statistical Support— Uppsala Clinical Research Shaun Goodman (Canada) Harald Darius (Germany) Stephan Windecker (Switzerland) Ronald Aronson (BMS) ACADEMIC COORDINATING CENTER Duke Clinical Research Institute CONTRACT RESEARCH ORGANIZATION Pharmaceutical Product Development (PPD) CLINICAL EVENTS CLASSIFICATION (CEC) SPONSORS COMMITTEE Bristol-Myers Squibb/ Duke Clinical Research Institute Pfizer

Outcomes Primary outcomes: Secondary outcomes: • ISTH major bleeding • Death or hospitalization • Clinically relevant non-major bleeding • Death or ischemic events – Stroke – Myocardial infarction – ARC definite or probable stent thrombosis – Urgent revascularization

Statistical Analysis • Baseline characteristics were summarized for each of the three subgroups (ACS Medical, ACS PCI, Elective PCI) by anticoagulant therapy and antiplatelet therapy. • For each of the outcomes, the proportion of patients with at least one event was calculated and summarized. • The differences between anticoagulant regimens within each of the three subgroups were tested and characterized by hazard ratios (HRs) and corresponding 95% confidence intervals (CIs) from a Cox proportional hazards model adjusted by antiplatelet regimen. • Likewise for the testing of the antiplatelet regimen where adjustment was done by the anticoagulant factor. • The effects of the randomization factor, ACS or PCI status, and their interaction, was tested using a Cox proportional hazards model.

Patient Allocation 4614 patients (492 sites, 33 countries) ACS 61. 2% Randomization stratified by ACS vs. elective PCI Elective PCI 38. 8% (n=1784) (n=2811) ACS Medical 39. 0% ACS PCI 61. 0% (n=1097) (n=1714) Patients with ACS were managed medically or with PCI according to local practice 19 pts with missing information about ACS and PCI
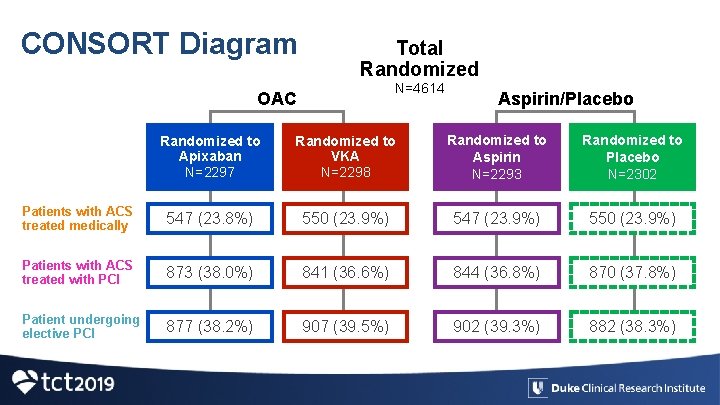
CONSORT Diagram Total Randomized N=4614 OAC Aspirin/Placebo Randomized to Apixaban N=2297 Randomized to VKA N=2298 Randomized to Aspirin N=2293 Randomized to Placebo N=2302 Patients with ACS treated medically 547 (23. 8%) 550 (23. 9%) 547 (23. 9%) 550 (23. 9%) Patients with ACS treated with PCI 873 (38. 0%) 841 (36. 6%) 844 (36. 8%) 870 (37. 8%) Patient undergoing elective PCI 877 (38. 2%) 907 (39. 5%) 902 (39. 3%) 882 (38. 3%)
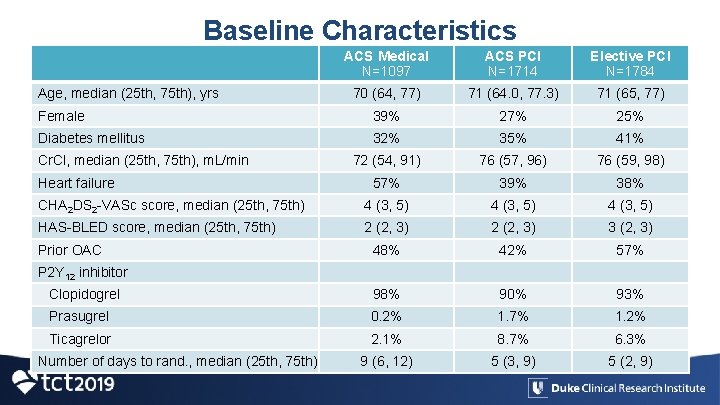
Baseline Characteristics ACS Medical N=1097 ACS PCI N=1714 Elective PCI N=1784 70 (64, 77) 71 (64. 0, 77. 3) 71 (65, 77) Female 39% 27% 25% Diabetes mellitus 32% 35% 41% 72 (54, 91) 76 (57, 96) 76 (59, 98) 57% 39% 38% CHA 2 DS 2 -VASc score, median (25 th, 75 th) 4 (3, 5) HAS-BLED score, median (25 th, 75 th) 2 (2, 3) 3 (2, 3) 48% 42% 57% Clopidogrel 98% 90% 93% Prasugrel 0. 2% 1. 7% 1. 2% Ticagrelor 2. 1% 8. 7% 6. 3% 9 (6, 12) 5 (3, 9) 5 (2, 9) Age, median (25 th, 75 th), yrs Cr. Cl, median (25 th, 75 th), m. L/min Heart failure Prior OAC P 2 Y 12 inhibitor Number of days to rand. , median (25 th, 75 th)
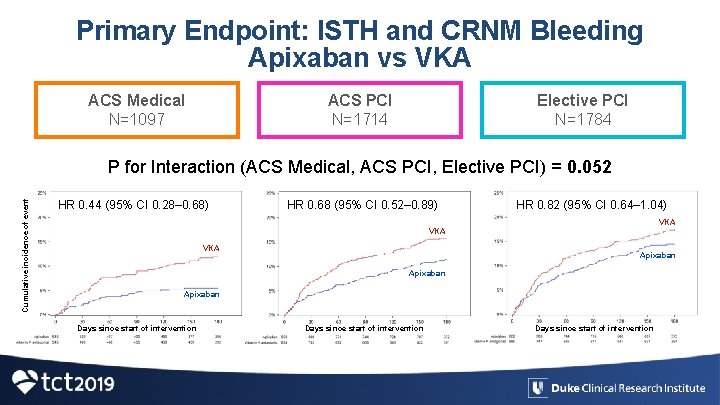
Primary Endpoint: ISTH and CRNM Bleeding Apixaban vs VKA ACS Medical N=1097 ACS PCI N=1714 Elective PCI N=1784 Cumulative incidence of event P for Interaction (ACS Medical, ACS PCI, Elective PCI) = 0. 052 HR 0. 44 (95% CI 0. 28– 0. 68) HR 0. 68 (95% CI 0. 52– 0. 89) HR 0. 82 (95% CI 0. 64– 1. 04) VKA VKA Apixaban Days since start of intervention
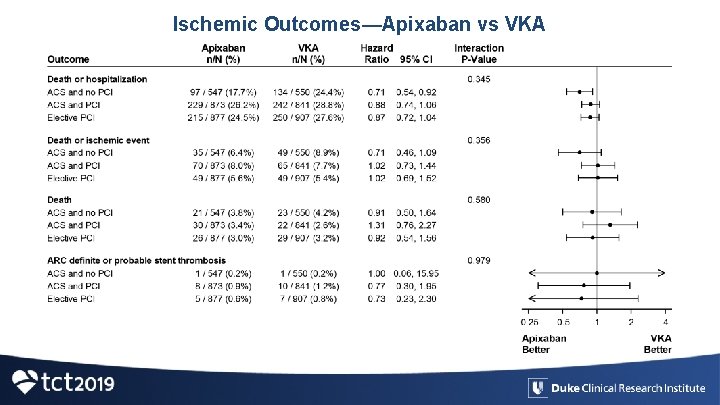
Ischemic Outcomes—Apixaban vs VKA
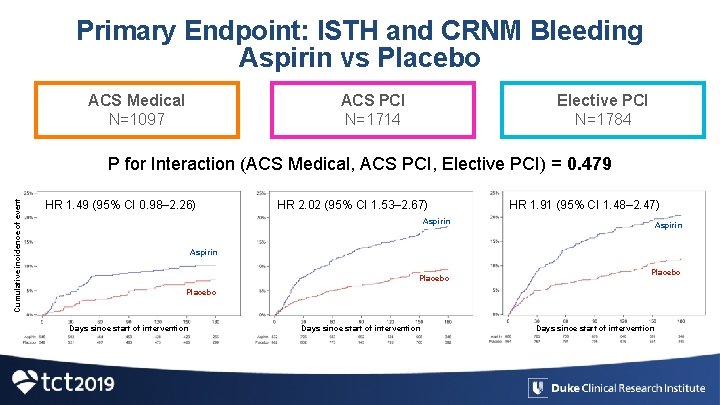
Primary Endpoint: ISTH and CRNM Bleeding Aspirin vs Placebo ACS Medical N=1097 ACS PCI N=1714 Elective PCI N=1784 Cumulative incidence of event P for Interaction (ACS Medical, ACS PCI, Elective PCI) = 0. 479 HR 1. 49 (95% CI 0. 98– 2. 26) HR 2. 02 (95% CI 1. 53– 2. 67) HR 1. 91 (95% CI 1. 48– 2. 47) Aspirin Placebo Days since start of intervention
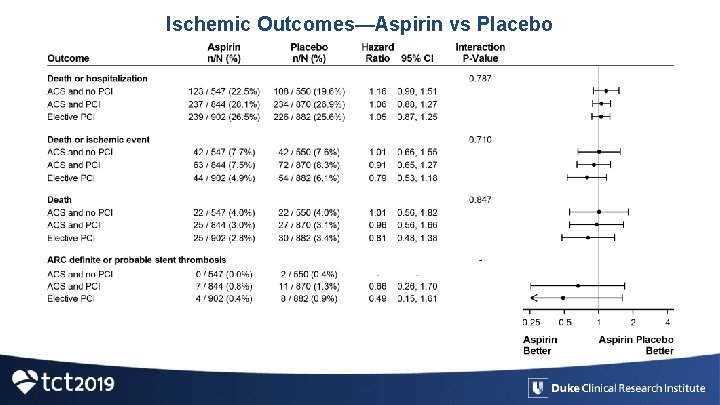
Ischemic Outcomes—Aspirin vs Placebo
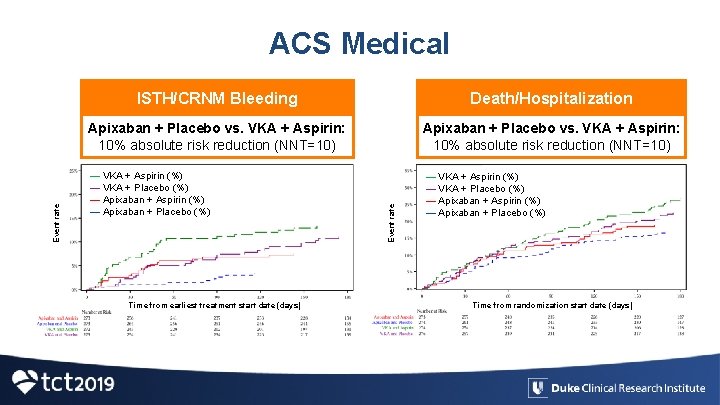
ISTH/CRNM Bleeding Death/Hospitalization Apixaban + Placebo vs. VKA + Aspirin: 10% absolute risk reduction (NNT=10) — VKA + Aspirin (%) — VKA + Placebo (%) — Apixaban + Aspirin (%) — Apixaban + Placebo (%) Time from earliest treatment start date (days) Event rate ACS Medical Time from randomization start date (days)
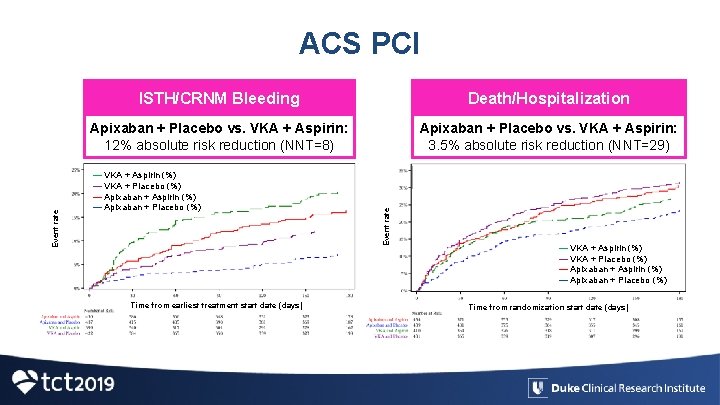
ISTH/CRNM Bleeding Death/Hospitalization Apixaban + Placebo vs. VKA + Aspirin: 12% absolute risk reduction (NNT=8) Apixaban + Placebo vs. VKA + Aspirin: 3. 5% absolute risk reduction (NNT=29) — VKA + Aspirin (%) — VKA + Placebo (%) — Apixaban + Aspirin (%) — Apixaban + Placebo (%) Time from earliest treatment start date (days) Event rate ACS PCI — VKA + Aspirin (%) — VKA + Placebo (%) — Apixaban + Aspirin (%) — Apixaban + Placebo (%) Time from randomization start date (days)
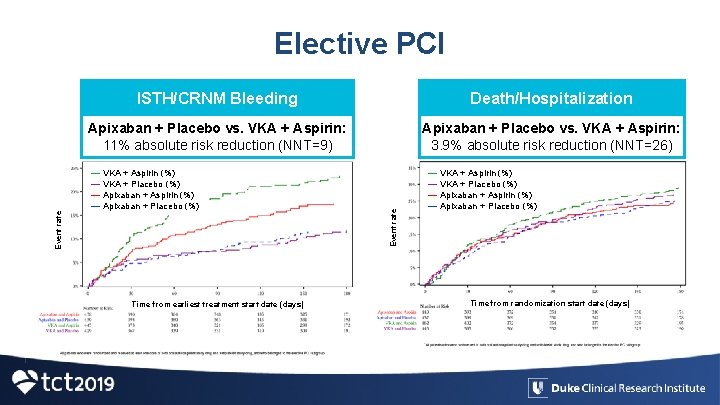
Elective PCI Death/Hospitalization Apixaban + Placebo vs. VKA + Aspirin: 11% absolute risk reduction (NNT=9) Apixaban + Placebo vs. VKA + Aspirin: 3. 9% absolute risk reduction (NNT=26) Event rate — VKA + Aspirin (%) — VKA + Placebo (%) — Apixaban + Aspirin (%) — Apixaban + Placebo (%) Time from earliest treatment start date (days) Event rate ISTH/CRNM Bleeding — VKA + Aspirin (%) — VKA + Placebo (%) — Apixaban + Aspirin (%) — Apixaban + Placebo (%) Time from randomization start date (days)

Limitations • The trial was powered for the primary safety endpoint (ISTH major/CRNM bleeding). The data for three reported subgroups are underpowered. • All patients received aspirin during their hospitalization for the index ACS and/or PCI and for a median of 6– 9 days prior to randomization. Therefore, the term dual antithrombotic therapy refers to the period after randomization. • The present study does not address the optimal treatment duration for the combined anticoagulation and P 2 Y 12 inhibitor regimen, as all patients were treated for 6 months. • The present study does not address the optimal short-term treatment duration of aspirin after PCI before initiation of dual antithrombotic therapy.

Conclusions • The overall results of the AUGUSTUS trial are consistent across the three clinically important subgroups (ACS medical, ACS PCI, elective PCI). • Accordingly, anticoagulation with apixaban, at the dose approved for stroke prevention in patients with AF, combined with a P 2 Y 12 inhibitor without aspirin should be preferred in patients with AF and ACS irrespective of management with medical therapy or PCI, and those undergoing elective PCI than regimens that include VKAs, aspirin, or both.

Acknowledgement Thank you to the national leaders, investigators, study coordinators, and study participants who made AUGUSTUS possible.
![CIRCULATION. 2019; [PUBLISHED ONLINE AHEAD OF PRINT]. DOI: 10. 1161/CIRCULATIONAHA. 119. 043308 ANTITHROMBOTIC THERAPY CIRCULATION. 2019; [PUBLISHED ONLINE AHEAD OF PRINT]. DOI: 10. 1161/CIRCULATIONAHA. 119. 043308 ANTITHROMBOTIC THERAPY](http://slidetodoc.com/presentation_image_h/10a9f48cecfbf26c3a62a0b116b3a5a9/image-23.jpg)
CIRCULATION. 2019; [PUBLISHED ONLINE AHEAD OF PRINT]. DOI: 10. 1161/CIRCULATIONAHA. 119. 043308 ANTITHROMBOTIC THERAPY IN PATIENTS WITH ATRIAL FIBRILLATION AND ACUTE CORONARY SYNDROME TREATED MEDICALLY OR WITH PERCUTANEOUS CORONARY INTERVENTION OR UNDERGOING ELECTIVE PERCUTANEOUS CORONARY INTERVENTION: INSIGHTS FROM THE AUGUSTUS TRIAL STEPHAN WINDECKER; RENATO D. LOPES; TYLER MASSARO; CHARLOTTE JONES-BURTON; CHRISTOPHER B. GRANGER; RONALD ARONSON; GRETCHEN HEIZER; SHAUN G. GOODMAN; HARALD DARIUS; W. SCHUYLER JONES; MICHAEL ASCHERMANN; DAVID BRIEGER; FERNANDO CURA; THOMAS ENGSTRØM; VILIAM FRIDRICH; SIGRUN HALVORSEN; KURT HUBER; HYUN-JAE KANG; JOSE L. LEIVA-PONS; BASIL S. LEWIS; GERMAN MALAGA; NICOLAS MENEVEAU; BELA MERKELY; DAVOR MILICIC; JOÃO MORAIS; TATJANA S. POTPARA; DIMITAR RAEV; MANEL SABATÉ; SUZANNE DE WAHA-THIELE; ROBERT C. WELSH; DENIS XAVIER; ROXANA MEHRAN; JOHN H. ALEXANDER ; ON BEHALF OF THE AUGUSTUS INVESTIGATORS CIRCULATION HTTPS: //WWW. AHAJOURNALS. ORG/DOI/10. 1161/CIRCULATIONAHA. 119. 043308 25
- Slides: 23