Antimycobacterial Drugs Haitham M AlWali Ph D Pharmacology

Antimycobacterial Drugs Haitham M. Al-Wali Ph. D Pharmacology & Therapeutics Al-Nahrain college of Medicine 11/28/2020 4: 33 AM 1

• The chemotherapy of infections caused by Mycobacterium tuberculosis, M leprae, and M avium-intracellulare is complicated by numerous factors, including (1) Limited information about the mechanisms of antimycobacterial drug actions (2) The development of resistance (3) The intracellular location of mycobacteria (4)The chronic nature of mycobacterial disease, which requires prolonged drug treatment and is associated with drug toxicities. (5) Patient compliance. 11/28/2020 4: 33 AM 2
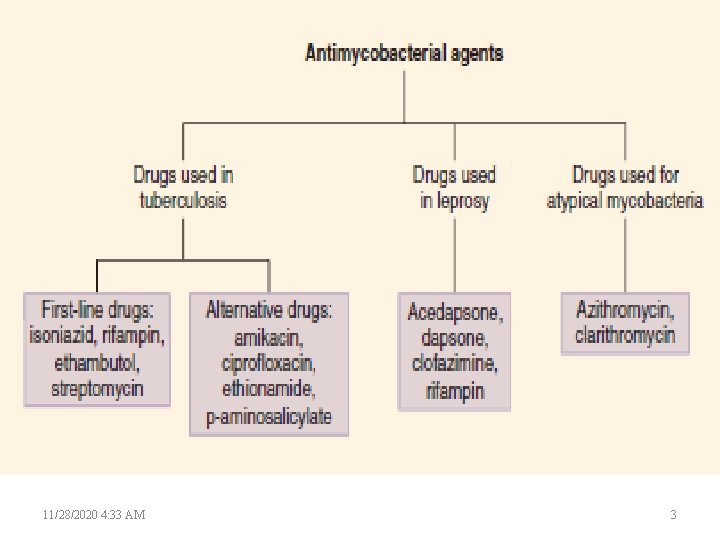
11/28/2020 4: 33 AM 3

DRUGS FOR TUBERCULOSIS • The major ( First line) drugs used in tuberculosis are Rifampin, Isoniazid (INH), Pyrazinamide, Ethambutol, and Streptomycin. (RIPES) • Actions of these agents on M tuberculosis are bactericidal or bacteriostatic depending on drug concentration and strain susceptibility. • Initiation of treatment of pulmonary tuberculosis usually involves a 3 - or 4 -drug combination regimen depending on rate of resistance to isoniazid (INH). • Directly observed therapy (DOT) regimens are recommended in noncompliant patients and in drug-resistant tuberculosis. 11/28/2020 4: 33 AM 4

• A. Isoniazid 1. Mechanisms— Isoniazid (INH) is a structural congener of pyridoxine. Its mechanism of action involves inhibition of mycolic acids, characteristic components of mycobacterial cell walls. • Resistance can emerge rapidly if the drug is used alone. • High-level resistance is associated with deletion in the kat. G gene that codes for a catalase-peroxidase involved in the bioactivation of INH. • INH is bactericidal for actively growing tubercle bacilli but is less effective against dormant organisms. 11/28/2020 4: 33 AM 5

A. Isoniazid • 2. Pharmacokinetics—INH • Well absorbed orally and penetrates cells to act on intracellular mycobacteria. The liver metabolism of INH is by acetylation and is under genetic control. • Patients may be fast or slow inactivators of the drug. INH half life in “fast acetylators” is 60– 90 min; in “slow acetylators” it may be 3– 4 h. • The proportion of fast acetylators is higher among people of Asian origin (including Native Americans) than those of European or African origin. Fast acetylators may require higher dosage than slow acetylators for equivalent therapeutic effects. 11/28/2020 4: 33 AM 6

A. Isoniazid 3. Clinical use—INH is the single most important drug used in tuberculosis and is a component of most drug combination regimens. In the treatment of latent infection (formerly known as “prophylaxis”) for close contacts of patients with active disease, INH is given as the sole drug. 11/28/2020 4: 33 AM 7

A. Isoniazid 4. Toxicity and interactions— • Neurotoxic effects are common and include peripheral neuritis, restlessness, muscle twitching, and insomnia. These effects can be alleviated by administration of pyridoxine (25– 50 mg/d orally). • INH is hepatotoxic and may cause abnormal liver function tests, jaundice, and hepatitis. Fortunately, hepatotoxicity is rare in children. • INH may inhibit the hepatic metabolism of drugs (eg, carbamazepine, phenytoin, warfarin). • Hemolysis has occurred in patients with glucose-6 phosphate dehydrogenase (G 6 PDH) deficiency. • A lupus-like syndrome has been reported. 11/28/2020 4: 33 AM 8

B. Rifampin • 1. Mechanisms— • Rifampin, a derivative of rifamycin, is bactericidal against M tuberculosis. The drug inhibits DNA-dependent RNA polymerase in M tuberculosis and many other microorganisms. • Resistance via changes in drug sensitivity of the polymerase often emerges rapidly if the drug is used alone. 11/28/2020 4: 33 AM 9

B. Rifampin • 2. Pharmacokinetics— • When given orally, rifampin is well absorbed and is distributed to most body tissues, including the central nervous system (CNS). • The drug undergoes enterohepatic cycling and is partially metabolized in the liver. Both free drug and metabolites, which are orange-colored, are eliminated mainly in the feces. 11/28/2020 4: 33 AM 10

B. Rifampin • 3. Clinical uses— • In the treatment of tuberculosis, rifampin is always used in combination with other drugs. • However, rifampin can be used as the sole drug in treatment of latent tuberculosis in INH-intolerant patients or in close contacts of patients with INH-resistant strains of the organism. 11/28/2020 4: 33 AM 11

B. Rifampin • 3. Clinical uses • In leprosy, rifampin given monthly delays the emergence of resistance to dapsone. • Rifampin may be used with vancomycin for infections due to resistant staphylococci (methicillin-resistant Staphylococcus aureus [MRSA] strains) or pneumococci (penicillinresistant Streptococcus pneumoniae [PRSP] strains). • Other uses of rifampin include the meningococcal and staphylococcal carrier states. 11/28/2020 4: 33 AM 12

B. Rifampin 4. Toxicity and interactions— • Rifampin commonly causes proteinuria and may impair antibody responses. • Occasional adverse effects include skin rashes, thrombocytopenia, nephritis, and liver dysfunction. • If given less often than twice weekly, rifampin may cause a flu-like syndrome and anemia. • Rifampin strongly induces liver drug-metabolizing enzymes and enhances the elimination rate of many drugs, including anticonvulsants, contraceptive steroids, cyclosporine, ketoconazole, methadone, terbinafine, and warfarin. 11/28/2020 4: 33 AM 13

5. Other rifamycins • Rifabutin is equally effective as an antimycobacterial agent and is less likely to cause drug interactions than rifampin. It is usually preferred over rifampin in the treatment of tuberculosis or other mycobacterial infections in AIDS patients. Rifamixin, a rifampin derivative that is not absorbed from the gastrointestinal tract, has been used in traveler’s diarrhea. 11/28/2020 4: 33 AM 14

C. Ethambutol • 1. Mechanisms— Ethambutol inhibits arabinosyl transferases involved in the synthesis of arabinogalactan, a component of mycobacterial cell walls. Resistance occurs rapidly via mutations in the emb gene if the drug is used alone. 11/28/2020 4: 33 AM 15

C. Ethambutol 2. Pharmacokinetics— The drug is well absorbed orally and distributed to most tissues, including the CNS. A large fraction is eliminated unchanged in the urine. Dose reduction is necessary in renal impairment. 3. Clinical use— The main use of ethambutol is in tuberculosis, and it is always given in combination with other drugs. 11/28/2020 4: 33 AM 16

C. Ethambutol 4. Toxicity— The most common adverse effects are dose dependent visual disturbances, including decreased visual acuity, red-green color blindness, optic neuritis, and possible retinal damage (from prolonged use at high doses). Most of these effects regress when the drug is stopped. Other adverse effects include headache, confusion, hyperuricemia and peripheral neuritis. 11/28/2020 4: 33 AM 17

D. Pyrazinamide 1. Mechanisms— The mechanism of action of pyrazinamide is not known; however, its bacteriostatic action appears to require metabolic conversion via pyrazinamidases present in M tuberculosis. Resistance occurs via mutations in the gene that encodes enzymes involved in the bioactivation of pyrazinamide and by increased expression of drug efflux systems. This develops rapidly when the drug is used alone, but there is minimal cross-resistance with other antimycobacterial drugs. 11/28/2020 4: 33 AM 18

D. Pyrazinamide 2. Pharmacokinetics— Pyrazinamide is well absorbed orally and penetrates most body tissues, including the CNS. The drug is partly metabolized to pyrazinoic acid, and both parent molecule and metabolite are excreted in the urine. The plasma half-life of pyrazinamide is increased in hepatic or renal failure. 11/28/2020 4: 33 AM 19

D. Pyrazinamide 3. Clinical use— The combined use of pyrazinamide with other antituberculous drugs is an important factor in the success of short-course treatment regimens. 4. Toxicity— 40% of patients develop non-gouty polyarthralgia. Hyperuricemia occurs commonly (asymptomatic). Others are myalgia, gastrointestinal irritation, maculopapular rash, hepatic dysfunction, porphyria, and photosensitivity reactions. Pyrazinamide should be avoided in pregnancy. 11/28/2020 4: 33 AM 20

E. Streptomycin This aminoglycoside is now used more frequently than before because of the growing prevalence of drug-resistant strains of M tuberculosis. Streptomycin is used principally in drug combinations for the treatment of lifethreatening tuberculous disease, including meningitis, and severe organ tuberculosis. The pharmacodynamic and pharmacokinetic properties of streptomycin are similar to those of other aminoglycosides. 11/28/2020 4: 33 AM 21

F. Alternative Drugs Several drugs with antimycobacterial activity are used in cases that are resistant to first-line agents; they are considered second-line drugs because they are no more effective, and their toxicities are often more serious than those of the major drugs. v. Amikacin is indicated for the treatment of tuberculosis suspected to be caused by streptomycin-resistant or multidrug-resistant mycobacterial strains. To avoid emergence of resistance, amikacin should always be used in combination drug regimens. 11/28/2020 4: 33 AM 22

F. Alternative Drugs v Ciprofloxacin and ofloxacin are often active against strains of M tuberculosis resistant to first-line agents. The fluoroquinolones should always be used in combination regimens with two or more other active agents. v. Ethionamide is a congener of INH, but crossresistance does not occur. The major disadvantage of ethionamide is severe gastrointestinal irritation and adverse neurologic effects at doses needed to achieve effective plasma levels. 11/28/2020 4: 33 AM 23

F. Alternative Drugs v P-Aminosalicylic acid (PAS) is rarely used because primary resistance is common. In addition, its toxicity includes gastrointestinal irritation, peptic ulceration, hypersensitivity reactions, and effects on kidney, liver, and thyroid function. Other drugs of limited use because of their toxicity include capreomycin (ototoxicity, renal dysfunction) and cycloserine (peripheral neuropathy, CNS dysfunction). 11/28/2020 4: 33 AM 24

G. Antitubercular Drug Regimens 1. Standard regimens— For empiric treatment of pulmonary TB (in most areas of <4% INH resistance), an initial 3 -drug regimen of INH, rifampin, and pyrazinamide is recommended. If the organisms are fully susceptible (and the patient is HIV-negative), pyrazinamide can be discontinued after 2 mo and treatment continued for a further 4 mo with a 2 -drug regimen. 11/28/2020 4: 33 AM 25

G. Antitubercular Drug Regimens 2. Alternative regimens— Alternative regimens in cases of fully susceptible organisms include INH + rifampin for 9 mo, or INH + ETB for 18 mo. 11/28/2020 4: 33 AM 26

3. Resistance • If resistance to INH is higher than 4%, the initial drug regimen should include ethambutol or streptomycin. • Tuberculosis resistant only to INH: (RIF + pyrazinamide + ethambutol or streptomycin) for 6 mon. • Multidrug-resistant organisms (resistant to both INH and rifampin) should be treated with 3 or more drugs to which the organism is susceptible for a period of more than 18 mon. 11/28/2020 4: 33 AM 27

• DRUGS FOR LEPROSY • A-Dapsone remains the most active drug against M leprae. The mechanism of action of sulfones may involve inhibition of folic acid synthesis. • Because of resistance, it is recommended that the drug be used in combinations with rifampin and/or clofazimine. • Dapsone can be given orally, penetrates tissues well, undergoes enterohepatic cycling. • Common adverse effects include gastrointestinal irritation , fever, skin rashes, and methemoglobinemia. Hemolysis may occur, especially in patients with G 6 PDH deficiency. 11/28/2020 4: 33 AM 28

• DRUGS FOR LEPROSY • B. Other Agents • Drug regimens usually include combinations of dapsone with rifampin (or rifabutin) plus or minus clofazimine. • Clofazimine, a phenazine dye that may interact with DNA, causes gastrointestinal irritation and skin discoloration ranging from red-brown to nearly black. 11/28/2020 4: 33 AM 29

DRUGS FOR ATYPICAL MYCOBACTERIAL INFECTIONS: • Mycobacterium avium complex (MAC) is a cause of spread infections in AIDS patients. Currently, clarithromycin or azithromycin with or without rifabutin is recommended for primary prophylaxis. Treatment of MAC infections requires a combination of drugs, one favored regimen consisting of azithromycin or clarithromycin with ethambutol and rifabutin. 11/28/2020 4: 33 AM 30

DRUGS FOR ATYPICAL MYCOBACTERIAL INFECTIONS: • Infections resulting from other atypical mycobacteria (eg, M marinum, M ulcerans), though sometimes asymptomatic, may be treated with the described antimycobacterial drugs (eg, ethambutol, INH, rifampin) or other antibiotics (eg, amikacin, cephalosporins, fluoroquinolones, macrolides, or tetracyclines). 11/28/2020 4: 33 AM 31
- Slides: 31