Antimicrobial Drugs I Terminology of chemotherapy II Where

Antimicrobial Drugs I. Terminology of chemotherapy II. Where antimicrobial drugs come from III. How antimicrobials work IV. Drug resistance V. Interactions between drugs and hosts VI. Selecting the right antimicrobial drug

I. Terms When a drug is used to control an infection, the practice is termed antimicrobial chemotherapy Antimicrobial drugs: a class of compounds which inhibit or kill microorganisms. – Antibiotics -- _______ antimicrobial drugs. – Synthetics -- _______ antimicrobials. Antibiotics which have been chemically modified are called _________. – Broad spectrum agents -– Narrow spectrum agents --

Where do antimicrobials come from? • Fleming’s discovery of ________ • Main sources of useful antibiotics: Streptomyces and Bacillus (______), Penicillium and Cephalosporium (_____) • Thousands have been discovered; relatively few of these are ______.

How do they work? • The main trick if one were to “design” an antibiotic: find something the target pathogen has or does (e. g. a structure or pathway) which the host cell doesn’t. For example, most bacteria have peptidoglycan while eukaryotes don’t so a compound which destroys it or inhibits production (like penicillin) shouldn’t affect eukaryotes. • Toxicity to the host is a major concern Therapeutic Index -- ratio of a drug’s_________ to its minimum _________ dose. For example: 20 µg/ml toxic dose = ____ 16 µg/ml effective dose versus 20 µg/ml 2 µg/ml = ___

How do they work (cont. )? Four main approaches: 1) Inhibition of _______ formation -e. g. penicillin and cephalosporin 2) Inhibition of ________ synthesis -e. g. sulfonamides 3) Inhibition of ______ synthesis -- e. g. tetracycline 4) Inhibition of cell _______ function (less common) e. g. polymixin
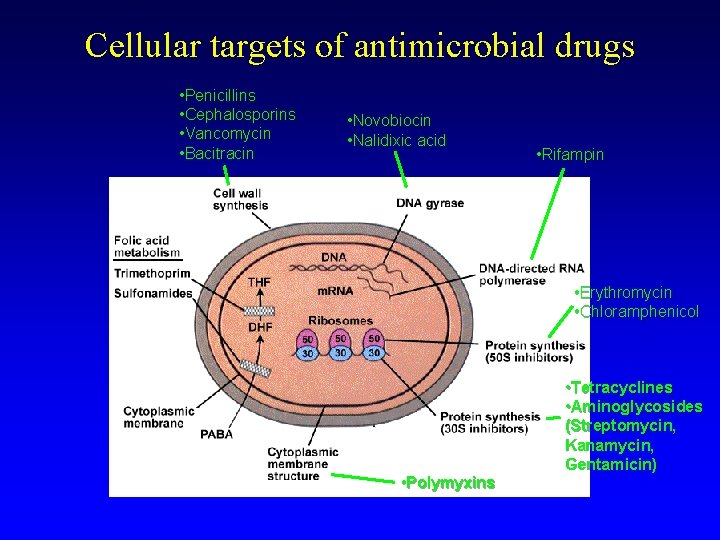
Cellular targets of antimicrobial drugs • Penicillins • Cephalosporins • Vancomycin • Bacitracin • Novobiocin • Nalidixic acid • Rifampin • Erythromycin • Chloramphenicol • Polymyxins • Tetracyclines • Aminoglycosides (Streptomycin, Kanamycin, Gentamicin)
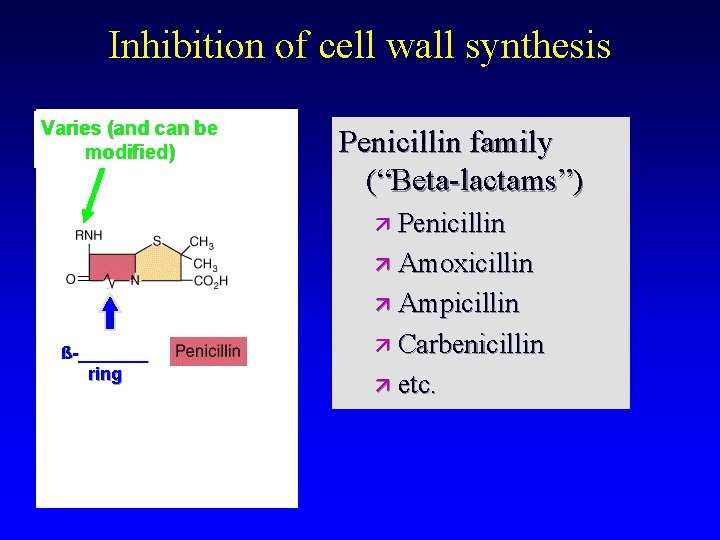
Inhibition of cell wall synthesis Varies (and can be modified) Penicillin family (“Beta-lactams”) Penicillin Amoxicillin Ampicillin ß-_______ ring Carbenicillin etc.
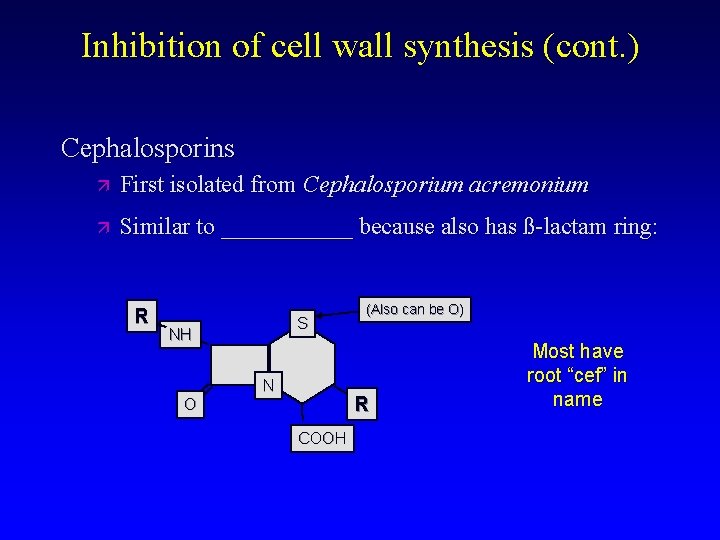
Inhibition of cell wall synthesis (cont. ) Cephalosporins First isolated from Cephalosporium acremonium Similar to ______ because also has ß-lactam ring: R S NH O N (Also can be O) R COOH Most have root “cef” in name

Nucleic acid synthesis inhibitors Chloroquine Trimethoprim Sulfanilamides (sulfa drugs) Are metabolic _______ of PABA (paraaminobenzoic acid), necessary for the synthesis of folic acid. Folic acid is then required for the synthesis of ______ and _______.
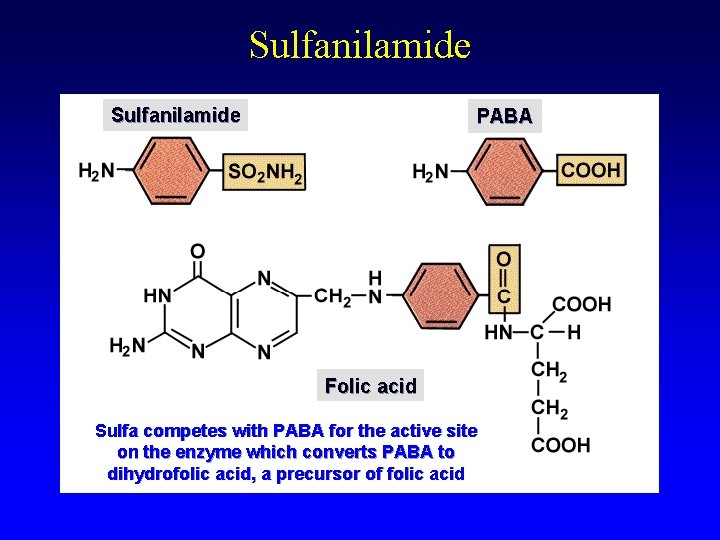
Sulfanilamide PABA Folic acid Sulfa competes with PABA for the active site on the enzyme which converts PABA to dihydrofolic acid, a precursor of folic acid

Protein synthesis inhibitors Tetracyclines -- Semisynthetic drug derived from a natural antibiotic made by Streptomyces. ________binding, bacteriostatic, broad spectrum. Erythromycin -- Ribosome-binding antibiotic derived from Streptomyces erythraeus. Also bacterio_____. In antibiotic class known as “_________” Aminoglycosides (e. g. streptomycin, kanamycin, gentimycin, neomycin). Also derived from Streptomyces, also ribosome-binding but bacteri_____.
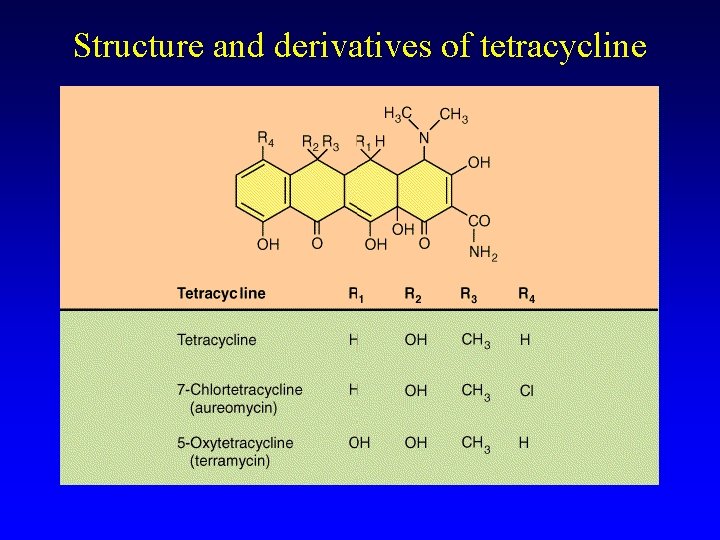
Structure and derivatives of tetracycline

Two New Classes of Antibiotics 1) Fosfomycin -- phosphoric acid used primarily against ___________ due to enteric bacteria (E. coli, etc. ) 2) Synercid (dalfopristin/quinupristin) and Zyvox (linezolid)-- narrow spectrum drugs used primarily against _________ pathogens such as Staphylococcus, Enterococcus, and Streptococcus.

Antimicrobial Drugs I. Terminology of chemotherapy II. Where antimicrobial drugs come from III. How antimicrobials work IV. Drug resistance V. Interactions between drugs and hosts VI. Selecting the right antimicrobial drug
Drug resistance mechanisms 1) Enzyme _______ -- e. g. ß-lactamases
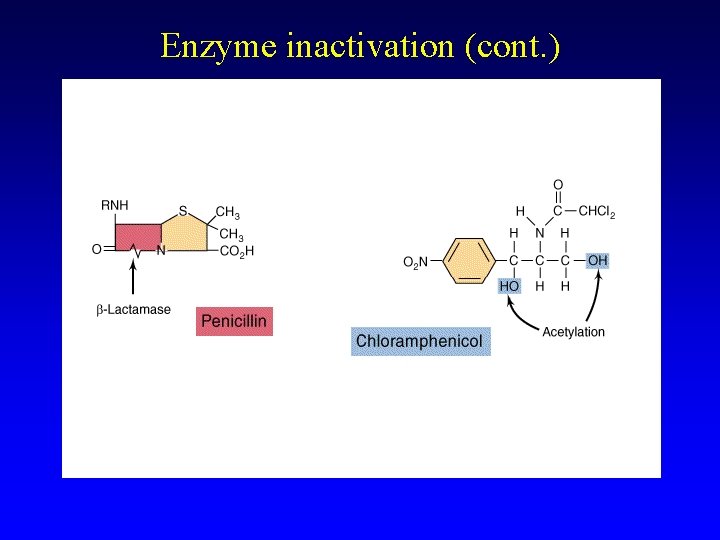
Enzyme inactivation (cont. )

The arms race: ß-lactamase inhibitors These are not antimicrobial themselves but are prescribed in conjunction with ß-lactam antibiotics to increase their effectiveness. They tend to be expensive.

Other drug resistance mechanisms 2) Decreased permeability to the drug Early penicillins could not pass the _____________ of Gram-negatives 3) Altered _______ for the drug -- altered cell wall receptors, altered target proteins (e. g. altering 50 S ribosomal binding site for erythromycin) 4) Changes in metabolic pathways or enzymes -- e. g. alteration in _________ synthesis 5) Efflux _____ -- antibiotics can be pumped out as fast as they come in. Pseudomonas are particularly famous for this. ___________ is pumped out of cells by plasmidencoded cytoplasmic membrane proteins

The emergence of antibiotic resistance Relationship between antibiotic use and the percentage of bacteria isolated from diarrheal patients resistant to the antibiotic

Percentage of reported cases of gonorrhea caused by antibiotic-resistant strains 59000 cases
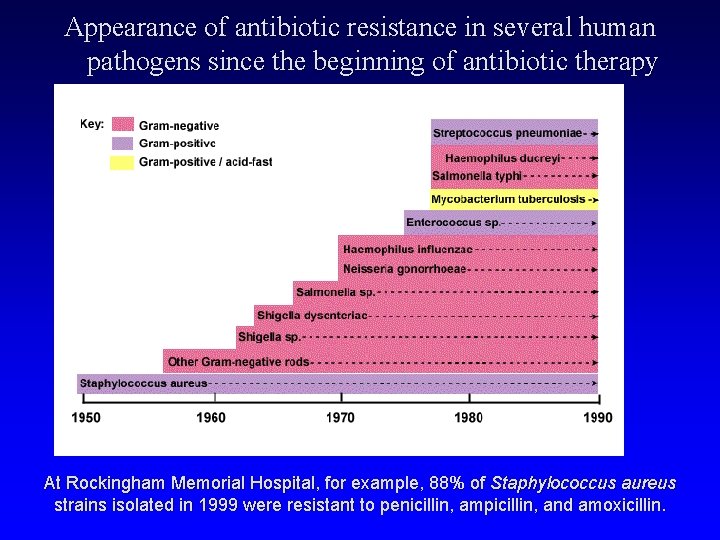
Appearance of antibiotic resistance in several human pathogens since the beginning of antibiotic therapy At Rockingham Memorial Hospital, for example, 88% of Staphylococcus aureus strains isolated in 1999 were resistant to penicillin, ampicillin, and amoxicillin.

The Arms Race Continues: S. aureus resistance to a brand-new antibiotic 07/20/2001 Associated Press LONDON – In a frustrating development in the battle against drugresistant bacteria, scientists report that the first entirely new type of antibiotic in 35 years has been beaten by the staph supergerm little more than a year after being introduced. Researchers at Harvard Medical School describe in the Lancet medical journal this week how an 85 -year-old man on dialysis came down with a staph infection in the lining of his intestines that was not vulnerable to the new drug, Zyvox [Linezolid]. It is the first report of staph resistance to the medicine.

Antimicrobial Susceptibility Profiles of Selected Aerobes, Rockingham Memorial Hospital, 1999

EXPOSURE TO DISINFECTANTS SUCH AS PINE-BASED CLEANERS MAY CONTRIBUTE TO ANTIBIOTIC RESISTANCE Repeated exposure to household cleaners containing pine oil may cause bacteria to develop resistance to some common antibiotics, say researchers from Tufts University School of Medicine in the December 1997 issue of the journal Antimicrobial Agents and Chemotherapy. In the study the researchers repeatedly exposed the bacteria Escherichia coli to a household cleaner containing the disinfectant pine oil or pure pine oil itself in order to isolate pine-oil resistant strains. The resistant strains were then tested against a variety of antibiotics. All pine oil-resistant strains were also multidrug resistant. “To our knowledge, the selection of chromosomal antibiotic resistance, albeit low level, by a disinfectant has not previously been reported for gram-negative bacteria, ” say the researchers. “Whether pine oil in products meant for household use could lead to a significant problem of antibiotic resistance is not know. However, it seems possible that additional disinfectants might be capable of selecting for resistance to antibiotics and vice versa. ” (M. Moken, L. M. Mc. Murry and S. Levy. 1997. Selection of multiple-antibioticresistant mutants of Escherichia coli by using the disinfectant pine oil: roles of the mar and acr. AB loci. Antimicrobial Agents and Chemotherapy. 41: 27702772. )

Host/drug reactions (adverse or “side” effects) Tissue toxicity -- kidneys, liver, heart, skin, nerves, teeth and bones _______ reactions • • sensitized on first contact. often due to reaction to a metabolic byproduct Disruption of normal flora (‘mucking with the microbial ecology of our bodies’) • frequent cause of diarrhea • __________ -- secondary infection caused by destruction of normal microflora. Example: yeast (Candida albicans) infections caused by destruction of vaginal lactobacilli with broad-spectrum antibiotics

Picking the right antimicrobial drug 1) Identify (if possible) the agent 2) Determine (if possible) the ________ of the agent -- e. g. Kirby-Bauer susceptibility test (will do in lab) tube dilution test Minimum Inhibitory Concentration = minimum concentration of a drug that visibly _____.
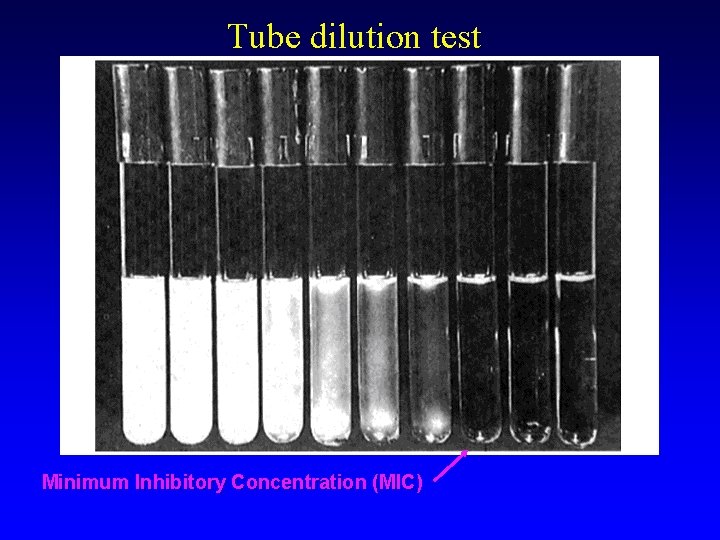
Tube dilution test Minimum Inhibitory Concentration (MIC)
- Slides: 27