ANTIMICROBIAL AGENTS l ANTIBIOTICS l ANTIMICROBIAL AGENTS l

ANTIMICROBIAL AGENTS

l ANTIBIOTICS l ANTIMICROBIAL AGENTS l CHEMOTHERAPEUTIC AGENTS

ANTIBIOTICS l Natural substances produced by various species of microorganisms bacteria fungi actinomycetes l suppress growth / kill other microorganisms

ANTIMICROBIAL AGENTS l Synthetic analogues l ANTIMICROBIAL AGENTS : l includes synthetic as well as naturally obtained drugs that attenuate microorganisms

CHEMOTHERAPEUTIC AGENTS l Drugs in this class differ from all others in that they are l Designed to inhibit/kill the infecting organism and have no/minimal effect on the recipient.

Classification Of AMA’s

Microorganisms of medical impotance fall into four categories l Bacteria l Viruses l Fungi l Parasites

l Anti-bacterial l Anti-viral l Anti-fungal l Anti-parasitic agents

Mechanism of Action l Agents that inhibit synthesis of bacterial cell walls Penicillins & cephalosporins Cycloserine, Vancomycin Bacitracin Azole antifungal agents (clotrimazole, fluconazole, itraconazole)

l Agents that act directly on the cell membranes of the microorganisms Polymixin Polyene antifungal agents (Nystatin, Amphotericin B) Alter cell memb. Permeability, leakage of intracellular comp.

l Agents that affect the function of 30 S or 50 S ribosomal subunits to cause a reversible inhibition of protein synthesis l Bacteriostatic drugs Chloramphenicol, Tetracyclines, Erythromycin, Clindamycin, Pristinamycins

l Agents that bind to 30 S ribosomal subunit & alter protein synthesis, which eventually leads to cell death Aminoglycosides

l Agents that affect bacterial nucleic acid metabolism. Rifamycins which inhibit RNA polymerase Quinolones which inhibit topoisomerases

l Anti-metabolites including trimethoprim & sulphonamides l Antiviral agents Nucleic acid analogues, Non-nucleoside reverse transcriptase inhibitors, Inhibitors of viral enzymes


TYPE OF ACTION Bacteriostatic Agents Bactericidal Agents

Bacteriostatic Agents Sulphonamides Tetracyclines Chloramphenicol Erythromycin Ethambutol

Bactericidal Agents Penicillins/Cephalosporins/Carbapen ems Aminoglycosides Rifampin l Isoniazid l Pyrazinamide

Cephalosporins Vancomycin Nalidixic acid Ciprofloxacin Metronidazole & Cotrimoxazole

l Some primarily static drugs may become cidal at higher concentrations (as attained in the urinary tract) & vice-versa.

SPECTRUM Of ACTIVITY Narrow spectrum Broad spectrum

SPECTRUM Of ACTIVITY Narrow spectrum Penicillin G Streptomycin Broad spectrum Tetracyclines Chloramphenicol

Successful Antimicrobial Therapy l Concentration: site of infection Concentration should inhibit microorganisms simultaneously it should be below the level toxic to human beings. l Host Defences Immunity intact - Bacteriostatic Agents Impaired immunity - Bactericidal Agents

Source of antibiotics l Fungi l Bacteria l Actinomycetes.

Source of antibiotics l Fungi l Penicillin, Griseofulvin, Cephalosporin l Bacteria l Polymyxin B, Colistin, Bacitracin, Aztreonam. l Actinomycetes. l Aminoglycosides, Macrolides, Tetracyclines, Polyenes, Chloramphenicol

Resistance

Bacterial resistance to ANTIMICROBIAL AGENTS l 3 general categories Drug does not reach its target Drug is not active Target is altered

Drug does not reach its target Porins Absence/mutation l Reduce drug entry l Reduced effective drug concentration at the target site. l Efflux pumps Transport drugs out of the cell l Resistance to tetracyclines & β-lactam antib l

Inactivation of Drug l Second general mechanism of drug resistance β-lactam antibiotics - β-lactamase Aminoglycosides - Aminoglycoside modifying enzymes l Variant: failure of bacterial cell to convert an inactive drug to its active metabolite. Resistance to INH in mycobacterium TB

Alteration of the Target l Mutation of natural target l Target modification The new target does not bind the drug for native target Resulting in resistance to antibiotic.

l Components mediating resistance to β –lactam antibiotics in psuedomonas aeruginosa
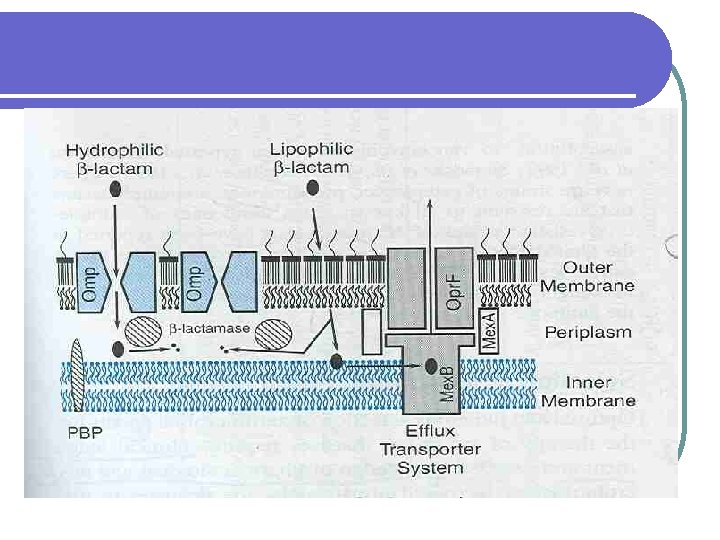

lβ –lactam antibiotics hydrophilic l Must cross outer membrane barrier of the cell via outer membrane protein (Omp) channel or porins l Mutation/missing/deleted l Drug entry slow or prevented.

lβ - lactamase concentrated between the inner & outer membrane in the periplasmic space l constitutes an enzymatic barrier l Drug destroyed l Effective concentration not achieved

l Target: PBP penicillin binding protein l Low affinity for drug l Altered

l Efflux transporter l Mex A, Mex B & Opr F l Pumps the antibiotic across the outer membrane l Reduced intracellular concentration of active drug RESISTANCE

Mutations l May occur in l Target protein l Drug transport protein l Protein important for drug activation l Random events l Survival advantage upon re-exposure to the drug

l Resistance is acquired by horizontal transfer of resistance determinants from a donor cell, often of another bacterial species by l Transduction l Transformation l Conjugation

l Insatiable need for new antibiotics

l Emergence of antibiotic resistance in bacterial pathogens both nosocomially & in the community setting is a very serious development that threatens the end of antibiotic era.

l Responsible approach to the use of antibiotics l That are now available & new agents that might be developed in future l Is essential the end averted. l If of antibiotic era is to be

CROSS RESISTANCE

CROSS RESISTANCE l Acquisition of resistance to one AMA conferring resistance to another antimicrobial agent to which the organism has not been exposed, is called cross resistance l Seen b/w chemically or mechanistically related drugs.

l Resistance to one sulphonamide means resistance to all others l Resistance to one tetracyclines means insenstivity to all others l Complete cross resistance

l Resistance to one aminoglycoside may not extend to others, Gentamycin resistant strains may respond to amikacin. l partial cross resistance

l Sometimes unrelated drugs show partial cross resistance, e. g. Tetracyclines & Chloramphenicol

PREVENTION DRUG RESISTANCE

Prevention DRUG RESISTANCE l Use of AMAs should not be: indiscriminate inadequate unduly prolonged l Use rapidly acting & narrow spectrum (Selective) AMA whenever possible.

Prevention DRUG RESISTANCE l Combination l AMA whenever prolonged therapy is undertaken. Tuberculosis, SABE l Infection by organism notorious for developing resistance Staph, E. Coli, M. Tuberculosis must be treated intensively.
- Slides: 49