ANTIINFLAMMATORY PAINREDUCING DRUGS Chapter 13 1 OBJECTIVES Terminology

ANTI-INFLAMMATORY & PAIN-REDUCING DRUGS Chapter 13 -1

OBJECTIVES Terminology used to describe antiinflammatory drugs MOA by which inflammation occurs MOA which glucocorticoids and NSAIDs work Comparisons of glucocorticoids and NSAIDs in their effects and side effects Precautions that apply to glucocorticoids, nonsteroidal anti-inflammatory drugs, and cyclooxygenase-2 inhibitor drugs

Terminology Anti-inflammatories: Drugs that relieve pain or discomfort by blocking or reducing the inflammatory process Steroidal anti-inflammatory drugs (corticosteroids) Nonsteroidal anti-inflammatory drugs (NSAIDs) not considered to be true analgesics Opoids work on CNS and reduce perception of pain

MOA - Inflammation EICOSANOIDS
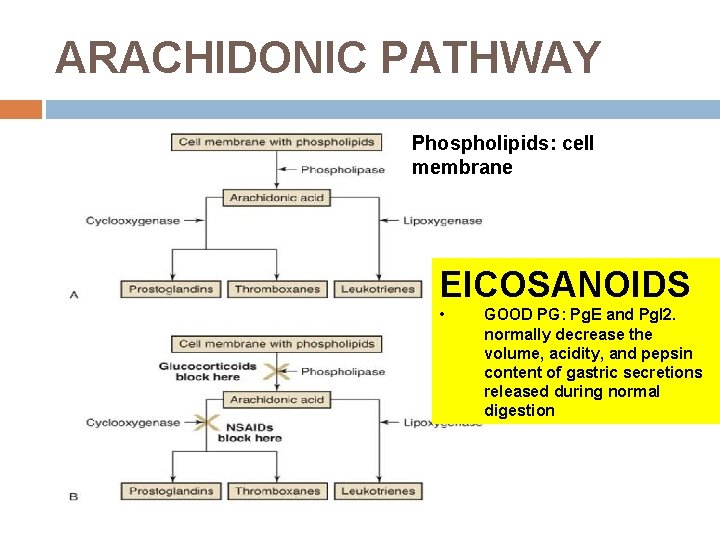
ARACHIDONIC PATHWAY Phospholipids: cell membrane EICOSANOIDS • GOOD PG: Pg. E and Pg. I 2. normally decrease the volume, acidity, and pepsin content of gastric secretions released during normal digestion

Anti-inflammatory Drugs Two main groups of anti-inflammatory drugs Steroidal antiinflammatory drugs block the action of phospholipase (lipoxygenase) Nonsteroidal antiinflammatory drugs block the action of cyclooxygenase (thromboxane)
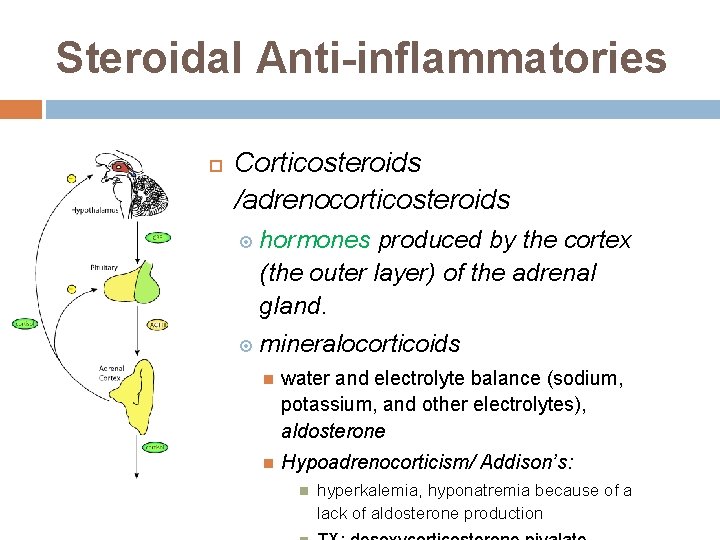
Steroidal Anti-inflammatories Corticosteroids /adrenocorticosteroids hormones produced by the cortex (the outer layer) of the adrenal gland. mineralocorticoids water and electrolyte balance (sodium, potassium, and other electrolytes), aldosterone Hypoadrenocorticism/ Addison’s: hyperkalemia, hyponatremia because of a lack of aldosterone production

Glucocorticoids. Antiinflammatories Inhibit phospholipase, and to a lesser degree cyclooxygenase Decreasing the production of prostaglandins and leukotrienes Every corticosteroid drug has both mineralocorticoid (sodium retention) and glucocorticoid (anti-inflammatory effects to some degree Are regulated by negative feedback
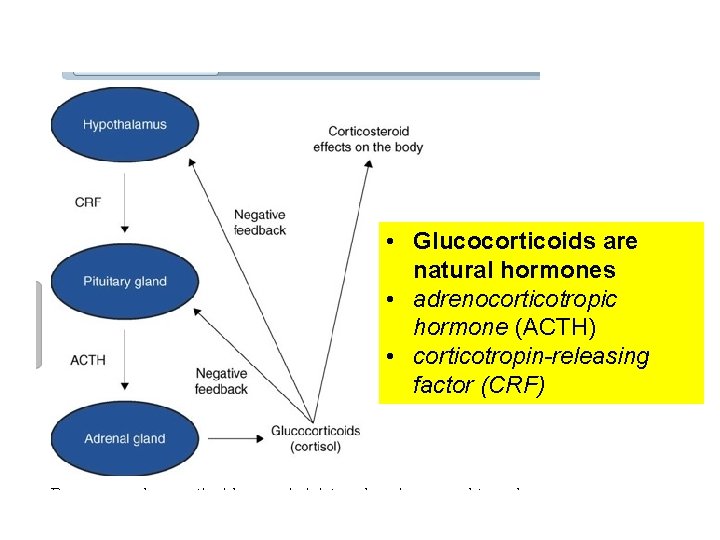
• Glucocorticoids are natural hormones • adrenocorticotropic hormone (ACTH) • corticotropin-releasing factor (CRF)

Glucocorticoid - Pros decrease inflammation relieve pruritus help maintain the integrity of the capillaries decreases swelling inhibit fibroblasts: reduce scarring by delaying wound healing normal therapeutic doses of glucocorticoid does not affect humoral immunity so ok to vaccinate animals on these drugs

Glucocorticoid - Cons Dec. fibroblast activity delay wound healing Suppress T-lymphocytes (normal therapy dose): Protects fungal agents (e. g. , histoplasmosis…) Horses: fungal eye infections Inc. gastric acid secretion and decrease mucus production: hyperacidity and GI ulceration catabolize protein in the cornea > deepening ulcer, Desmetocele: poor prognosis +/- induce abortion: cattle and mares , bitches Stress leukogram: lymphopenia, monocytopenia, eosinopenia, neutrophilia: sequestered - lungs, spleen
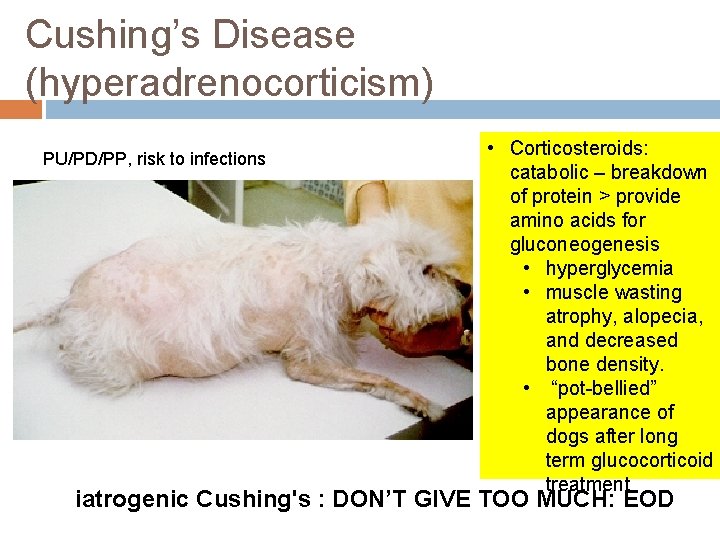
Cushing’s Disease (hyperadrenocorticism) PU/PD/PP, risk to infections • Corticosteroids: catabolic – breakdown of protein > provide amino acids for gluconeogenesis • hyperglycemia • muscle wasting atrophy, alopecia, and decreased bone density. • “pot-bellied” appearance of dogs after long term glucocorticoid treatment iatrogenic Cushing's : DON’T GIVE TOO MUCH: EOD

Addison’s Disease (hypoadrenocorticism) • extended use of glucocorticoid: lack of CRF and ACTH • adrenal cortex begins to atrophy > natural cortisol is diminished. weakness, lethargy, vomiting, and/or diarrhea Taper off slowly

Uses for Glucocorticoid Drugs Overreaction of the immune system: Autoimmune reactions such as lupus, Autoimmune hemolytic anemia, Hypersensitivity reactions such as allergic reactions Shock Systemic disease (Addison’s) OR iatrogenic cushion’s disease Cancer: Lymphosarcoma: lymphocytosis glucocorticoids are part of the treatment protocol for this cancer Inflammatory conditions: Ocular inflammation, MSK inflammation, IVD Lameness (horses) Pregnancy termination (Don’t use in pregnant animals)

CORTICOSTEROIDS (ADRENOCORTICOSTEROIDS) GLUCOCORTICOIDS Topical steroids almost always effect systematically so don’t give to immunocompromised/ pregnant animals Short-acting: < 12 hrs Hydrocortisone: topical Cortisone Intermediate-acting: 12 to 36 hrs; EOD; allergies/ inflammation Prednisone Prednisolone Triamcinolone Methylprednisolone (depomedrol) Isoflupredone Long-acting: 12 to 36 hours Dexamethasone Betamethasone Flumethasone

Glucocorticoids Formulations Aqueous solutions combined with a salt: Na-phosphate or Na-succinate to make them soluble (dissolvable) in water. E. g. dexamethasone sodium phosphate and prednisolone sodium succinate (Solu-Delta-Cortef) Adv: can be given in large doses intravenously with less risk of an adverse reaction; shock or CNS trauma DA: pain, irritation, or inflammation at the site of injection in hot/cold climate Alcohol solutions Suspensions: acetate-glucocorticoid lipid soluble: topical ophthalmic medications acetate, diacetate, pivalate, acetonide, or valerate appended to the glucocorticoid drug name

Safe Use of Glucocorticioid • Use NSAID rather than a glucocorticoid (as long as no contraindications exist for NSAID use). • Avoid continuous use of glucocorticoids: it is preferable to use an intermediate-acting glucocorticoid such as prednisolone rather LA-glucocorticoids: systemic administration (versus topical administration • Use the smallest dose of glucocorticoids that provides a clinical response. EOD Tapering: to avoid Addison’s Cat’s not really affected

NSAID COX-2 inhibitors: Carprofen (Rimadyl), Etodolac (Eto. Gesic), Deracoxib (Deramaxx), Meloxicam (Metacam), Firocoxib (Previcox) Tepoxalin (Zubrin) Phenylbutazone Aspirin (salicylates) Propionic acid derivatives: Ibuprofen (Advil, Motrin), Ketoprofen (Ketofen), Naproxen (Aleve) Flunixin meglumine (Banamine) Meclofenamic acid (Arquel) Dimethyl sulfoxide (DMSO) Chondroprotective agents Polysulfated glycosaminoglycans Hyaluronic acid Glucosamine Chondroitin sulfate (Cosequin) Acetaminophen Orgotein (superoxide dismutase)
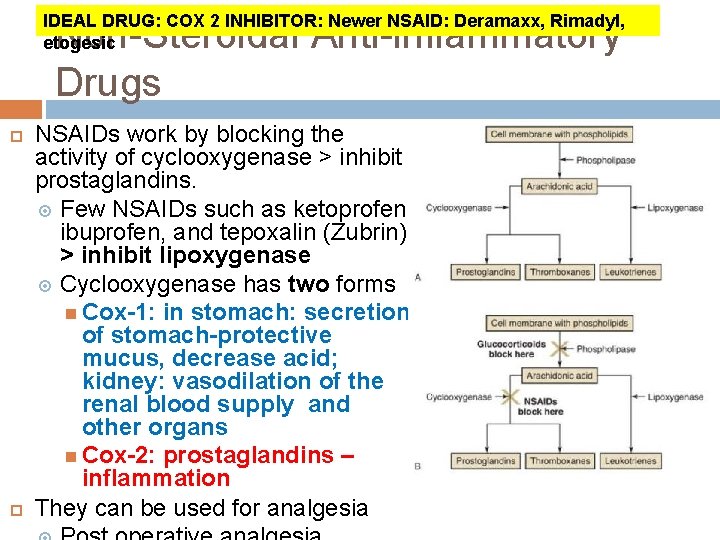
IDEAL DRUG: COX 2 INHIBITOR: Newer NSAID: Deramaxx, Rimadyl, etogesic Non-Steroidal Anti-inflammatory Drugs NSAIDs work by blocking the activity of cyclooxygenase > inhibit prostaglandins. Few NSAIDs such as ketoprofen, ibuprofen, and tepoxalin (Zubrin) > inhibit lipoxygenase Cyclooxygenase has two forms Cox-1: in stomach: secretion of stomach-protective mucus, decrease acid; kidney: vasodilation of the renal blood supply and other organs Cox-2: prostaglandins – inflammation They can be used for analgesia

NSAID - CON NSAID overdose/ nonselective NSAIDs extended period : anorexia, diarrhea, ulcerations of the stomach or duodenum sucralfate, histamine 2 (H 2) blockers (e. g. , cimetidine or ranitidine), and omeprazole are used to treat the open ulcer and reduce the acidity of the stomach, misoprostol: like PG-E Protein bound hence toxic in hypoalbuminemia Block good PG (Pg. E and Pg. I 2): Hypotension > prostaglandin E 2 is released by the kidney to dilate vessels Cox -2 inhibitors: Flavorful hence put away from animals to avoid toxicities Hepatotoxicity GI SE is reported much more frequently in dogs than horses E. g phenylbutazone (old NSAID) toxic in dogs: gastritis/ melena Cats: poorly tolerant of NSAIDs Low dose aspirin

References Bill, R. L. Clinical Pharmacology and Therapeutics for the Veterinary Technician, 3 rd edition. 2006. Romich, J. A. Pharmacology for Veterinary Technicians, 2 nd edition. 2010.
- Slides: 21