Antihypertensive Drugs Dr Sasan Zaeri Pharm D Ph

























- Slides: 33

Antihypertensive Drugs Dr. Sasan Zaeri Pharm. D, Ph. D (Department of Pharmacology)

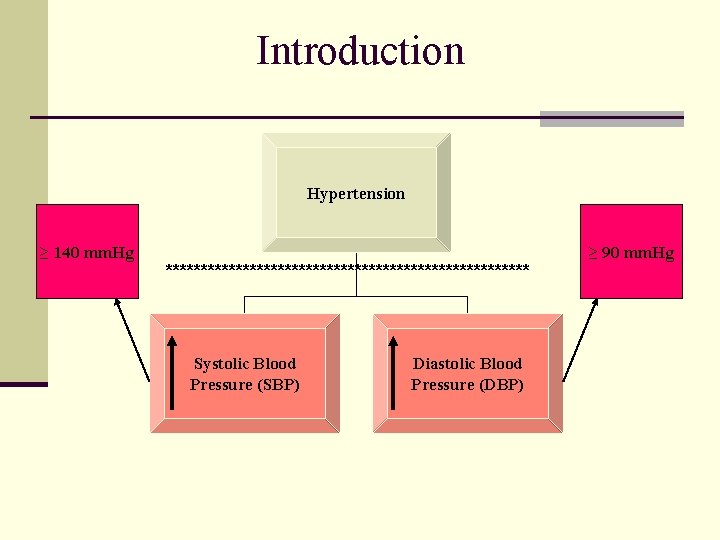
Introduction Hypertension ≥ 140 mm. Hg ************************** Systolic Blood Pressure (SBP) Diastolic Blood Pressure (DBP) ≥ 90 mm. Hg

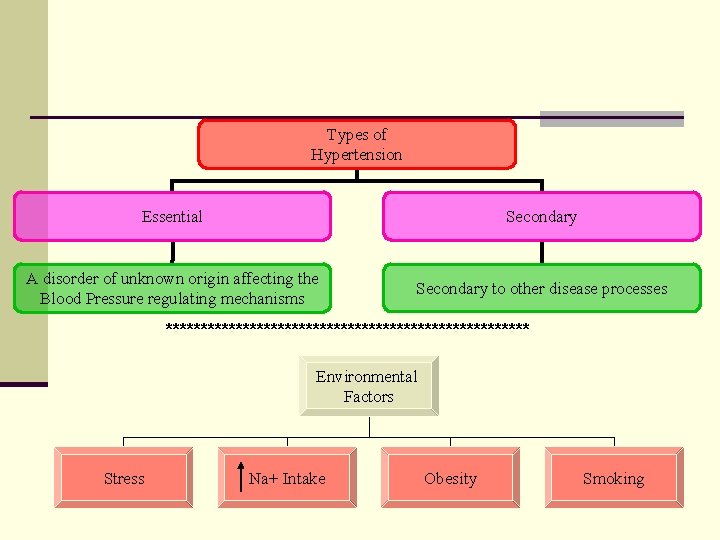
Types of Hypertension Essential Secondary A disorder of unknown origin affecting the Blood Pressure regulating mechanisms Secondary to other disease processes ************************** Environmental Factors Stress Na+ Intake Obesity Smoking

Treatment – Why? n To prevent target organ damage: n Eye (retinopathy) n Brain (stroke) n Kidney (chronic renal disease) n Heart (coronary artery disease, CHF) n Peripheral arteries (atherosclerosis) n Even asymptomatic hypertension needs to be treated

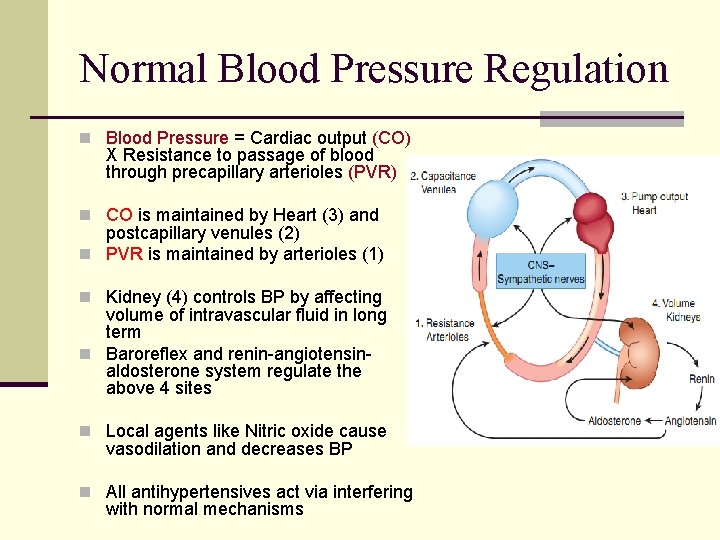
Normal Blood Pressure Regulation n Blood Pressure = Cardiac output (CO) X Resistance to passage of blood through precapillary arterioles (PVR) n CO is maintained by Heart (3) and postcapillary venules (2) n PVR is maintained by arterioles (1) n Kidney (4) controls BP by affecting volume of intravascular fluid in long term n Baroreflex and renin-angiotensin- aldosterone system regulate the above 4 sites n Local agents like Nitric oxide cause vasodilation and decreases BP n All antihypertensives act via interfering with normal mechanisms

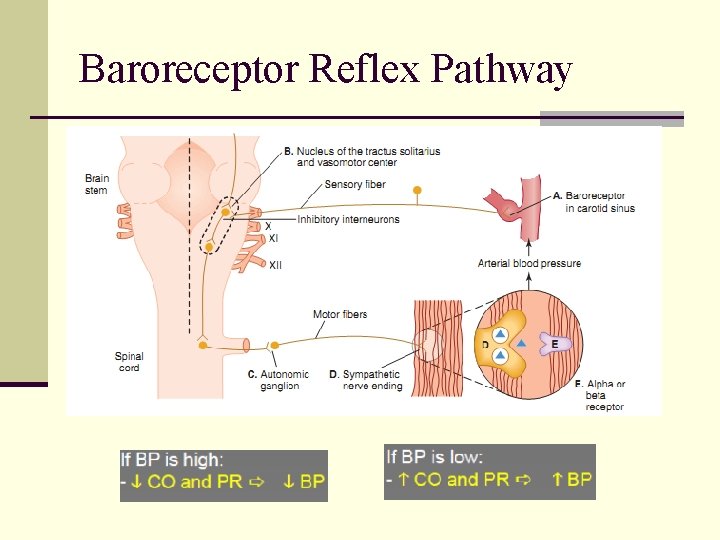
Baroreceptor Reflex Pathway

Antihypertensive Drugs Diuretics n n Thiazides, loop diuretics, K-sparing diuretics Sympathoplegic drugs n n ß-adrenergic blockers, α -adrenergic blockers, Centrally acting drugs Direct vasodilators n n Calcium channel blockers, Minoxidil, Hydralazine, Sodium nitroprusside Angiotensin antagonists n n Angiotensin-converting Enzyme (ACE) inhibitors, Angiotensin receptor 1(AT 1) blockers

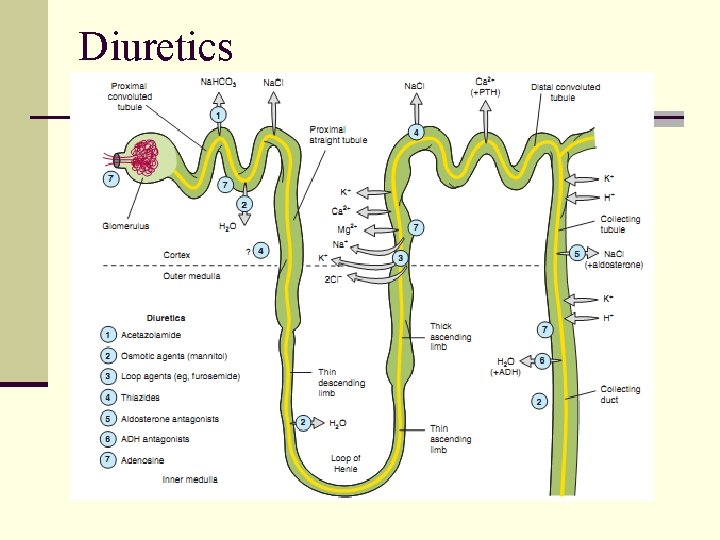
Diuretics n Mechanism of antihypertensive action: n Initially: diuresis – depletion of Na+ and body fluid volume – decrease in cardiac output n Subsequently after 4 - 6 weeks, reduction in total peripheral resistance (TPR) n n n Thiazides: Hydrochlorothiazide Loop diuretics: Furosemide K+ sparing diuretics: Spironolactone, triamterene and amiloride

Diuretics

Diuretics n Thiazide diuretic is the first-choice drug in mild hypertension n Thiazide diuretic can be used with a potassium sparing diuretic n Example: Triamterene-H n Loop diuretics are used only in complicated cases n CRF, CHF marked fluid retention cases

Thiazide diuretics n Adverse Effects (mostly seen in higher doses): n Hypokalaemia n Hyperglycemia: precipitation of diabetes n Hyperlipidemia: rise in total LDL level – risk of stroke n Hyperurecaemia: inhibition of uric acid excretion n Hypercalcemia n Thiazide diuretics reduce mortality and morbidity in patients with BP

Beta-adrenergic blockers n Mechanism of action: n n Reduction in CO Decrease in renin release from kidney (beta-1 mediated) n Non-selective: Propranolol (others: nadolol, timolol, pindolol, labetolol) n Cardioselective: Metoprolol (others: atenolol, esmolol, betaxolol) n Advantages: n Prevention of sudden cardiac death in post MI patients n Prevention of CHF progression

Beta-adrenergic blockers n Advantages of cardio-selective over non-selective: n In asthma n In diabetes mellitus n In peripheral vascular disease n Current status in treatment of BP: n First line along with diuretics and ACEIs n Preferred in angina pectoris n Preferred in Post MI patients – useful in preventing progression to CHF and mortality

Αlpha-adrenergic blockers n Mechanism of action: n Vasodilatation by blocking of alpha adrenergic receptors in smooth muscles: Reduction in PVR, reduction in CO by reduction in venomotor tone n Specific alpha-1 blockers: prazosin, terazosin and doxazosine n Non selective alpha blockers (phenoxybenzamine, phentolamine) are not used in chronic essential hypertension n Only used in pheochromocytoma

Αlpha-adrenergic blockers n Adverse effects: n n Prazosin causes postural hypotension n First-dose effect Fluid retention in monotherapy n Advantages: n n n Improvement of carbohydrate metabolism (diabetics) Improvement of lipid profile (↓ LDL, ↑ HDL) Treatment of benign prostatic hyperplasia (BPH) n Current status in treatment of PB: n Not used as first line agent, used in addition with other conventional drugs which are failing – diuretic or beta blocker

Centrally-Acting Drugs n Mechanism of action: n Inhibition of adrenergic discharge in brain by agonizing alpha -2 receptors: fall in PVR and CO n Methyldopa n Various adverse effects – cognitive impairement, postural hypotension, hemolytic anemia n Not used therapeutically now except in Hypertension during pregnancy n Clonidine n Not frequently used now because of tolerance and withdrawal hypertension

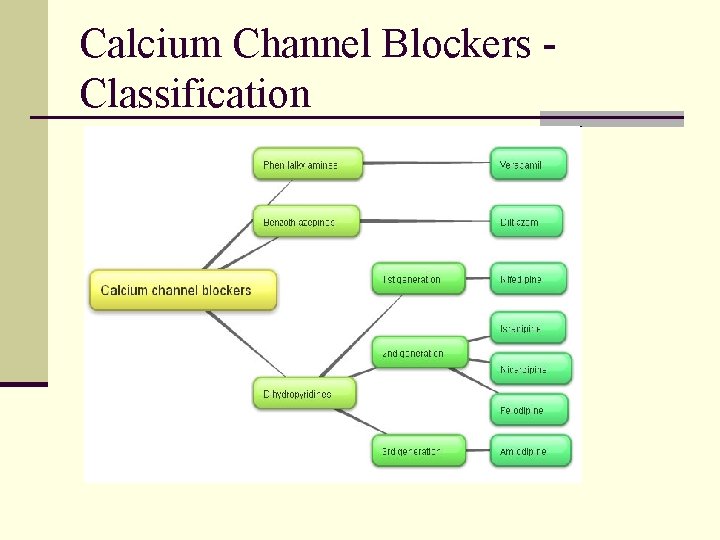
Calcium Channel Blockers Classification

Calcium Channel Blockers (CCBs) n Mechanism of action: n Blockade of L-type voltage-gated calcium channels in heart and vessels: vascular smooth muscle relaxation (↓ PVR), negative chronotropic and ionotropic effects in heart (↓CO) n DHPs (amlodipine and nifedipine) have highest smooth muscle relaxation followed by diltiazem and verapamil

Calcium Channel Blockers n Advantages: n Can be given to patients with n n Asthma with BP Angina with/without BP Peripheral vascular disease Prophylaxis of migraine n Immediate acting Nifedipine is not encouraged anymore n Not first line of antihypertensive unless indicated

Vasodilators - Hydralazine n Mechanism of action: Hydralazine molecules combine with receptors in the endothelium of arterioles and causes Nitric oxide release – relaxation of vascular smooth muscle – fall in PVR n Adverse effects: n Reflex tachycardia n Salt and water retention n Drug-induced lupus erythematosus n n Uses: n n Moderate hypertension when 1 st line fails – with betablockers and diuretics Hypertension in pregnancy

Vasodilators-Sodium Nitroprusside n Mechanism of action: n Rapidly produces nitric oxide to relax both resistance and capacitance vessels (↓PVR and CO) n Uses: Hypertensive Emergencies n (slow infusion)

Vasodilators – Minoxidil n Mechanism of action: n Hyperpolarization of smooth muscles by opening potassium channels and thereby relaxation of vascular smooth muscles n mainly 2 major uses – antihypertensive and alopecia n Rarely indicated in hypertension n Only in life threatening chronic hypertensions e. g. in chronic renal failure n More often in alopecia to promote hair growth

Angiotensin Converting Enzyme (ACE) Inhibitors What is Renin – Angiotensin System (RAS)?

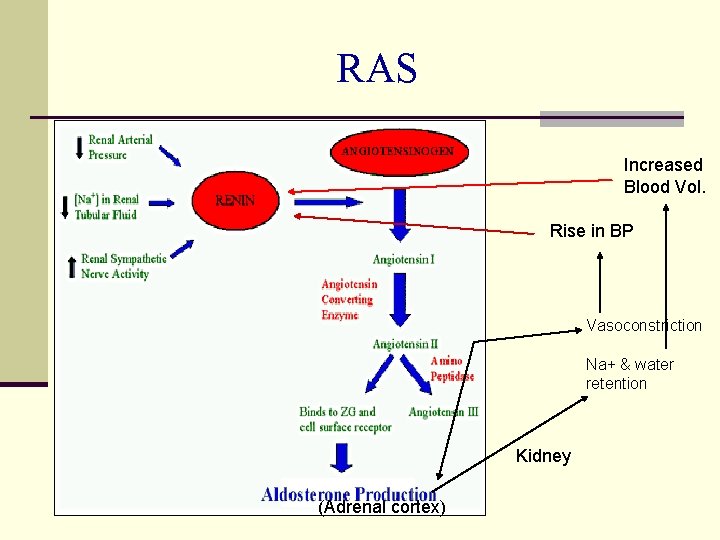
RAS n Renin is produced by juxtaglomerular cells of kidney n Renin is secreted in response to: n Decrease in arterial blood pressure n Decrease in Na+ in tubular fluid n Increased sympathetic nervous activity n Renin acts on a plasma protein, Angiotensinogen, and cleaves it to produce Angiotensin-I n Angiotensin-I is rapidly converted to Angiotensin-II by ACE (present in luminal surface of vascular endothelium) n Angiotensin-II stimulates Aldosterone secretion from Adrenal Cortex

RAS Increased Blood Vol. Rise in BP Vasoconstriction Na+ & water retention Kidney (Adrenal cortex)

RAS – Actions of Angiotensin-II 1. Powerful vasoconstrictor particularly arteriolar 2. It increases myocardial force of contraction (CA++ influx promotion) 3. Mitogenic effect – cell proliferation 4. Aldosterone secretion stimulation – retention of Na++ and water in body 5. Vasoconstriction of renal arterioles – rise in IGP – glomerular damage

Angiotensin-II n What are the chronic ill effects? n Volume overload and increased PVR n Hypertension – long standing will cause ventricular hypertrophy n Cardiac hypertrophy and remodeling n Renal damage Risk of increased CVS related morbidity and mortality n n ACE inhibitors reverse actions of Ang II

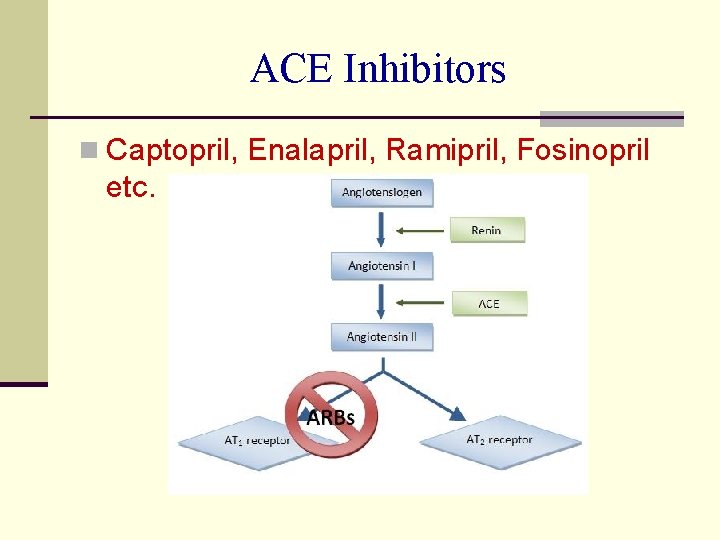
ACE Inhibitors n Captopril, Enalapril, Ramipril, Fosinopril etc.

ACEIs – Antihypertensive action n RAS is overactive in 80% of hypertensive cases and contributes to the maintenance of vascular tone and volume overload n RAS inhibition by ACEIs causes Lower PVR and volume overload hence lower BP

ACEIs – Adverse effects n Cough – persistent cough in 20% cases induced by inhibition of bradykinin breakdown in lungs n Hyperkalemia (routine check of K+ level) n Acute renal failure (bilateral renal artery stenosis) n Angioedema: swelling of lips, mouth, nose etc. n Foetopathic: hypoplasia of organs, growth retardation etc n Contraindications: Pregnancy, bilateral renal artery stenosis, hypersensitivity and hyperkalaemia

Place of ACE inhibitors in HTN n Drug of choice in: n HTN with diabetes (nephroprotective) n HTN with chronic renal disease n HTN with CHF n HTN with MI n Minimal worsening of quality of life – general wellbeing, sleep and work performance etc.

ACE inhibitors – other uses n Congestive Heart Failure (CHF) n Myocardial Infarction (MI) n Diabetic Nephropathy

Angiotensin Receptor Blockers (ARBs) Angiotensin Receptors: Most of the physiological actions of angiotensin are mediated via AT 1 receptor n ARBs block the actions of A-II: vasoconstriction, aldosterone release n No inhibition of ACE, therefore no accumulation of bradykinin n Cough is rare with ARBs n Indications of ARBs are similar to those of ACEIs. n Examples: Losartan, candesartan, valsartan and telmisartan