Antifungal inhibitors Komal Pareek 1 Challenge Eukaryotes Difficult

Antifungal inhibitors Komal Pareek 1

Challenge • Eukaryotes • Difficult to find selective toxicity in eukaryotes than prokaryotes • Fungal infections r more frequent as opportunistic infections in immunocompromised • Cell membrane essential component- sterol Fungi-Ergosterol Higher animals- cholesterol 2

Antifungal inhibitors • Agents affecting Fungal Sterols Polyenes-Amphotericin B, Nystatin Azoles- Voriconazole • Agents affecting Fungal cell walls • Echinocandins • Agents inhibiting Nucleic acid-flucytocine • Other Antifungal drugs-Griseofulvin 3

Antifungal Drugs • Polyenes, such as nystatin and amphotericin B, for systemic fungal infections. Inhibition of ergosterol synthesis fungicidal. Nephrotoxic • Griseofulvin from Penicillium. Systemic/oral. Binds to tubulin For Tineae 4

Antimycotic Antibiotics Polyenes Broad spectrum. Some effect on certain protozoa. Isolated, Streptomyces sp. Binds to sterols in fungal cell membrane; cell leaks K+, PH drops , small org. molecules • Macrolaktone [26 eor 38 -ring, Larger than macrolides ( erytromycin etc)] • Polyene (Macrolides not polyenes) • Several OH-groups • amino sugar, • Bad water solibility. 5
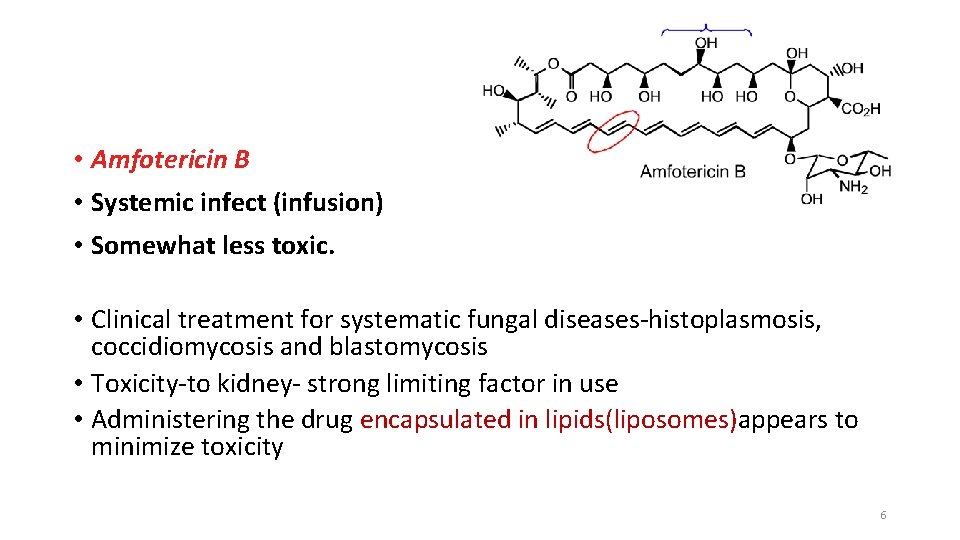
• Amfotericin B • Systemic infect (infusion) • Somewhat less toxic. • Clinical treatment for systematic fungal diseases-histoplasmosis, coccidiomycosis and blastomycosis • Toxicity-to kidney- strong limiting factor in use • Administering the drug encapsulated in lipids(liposomes)appears to minimize toxicity 6
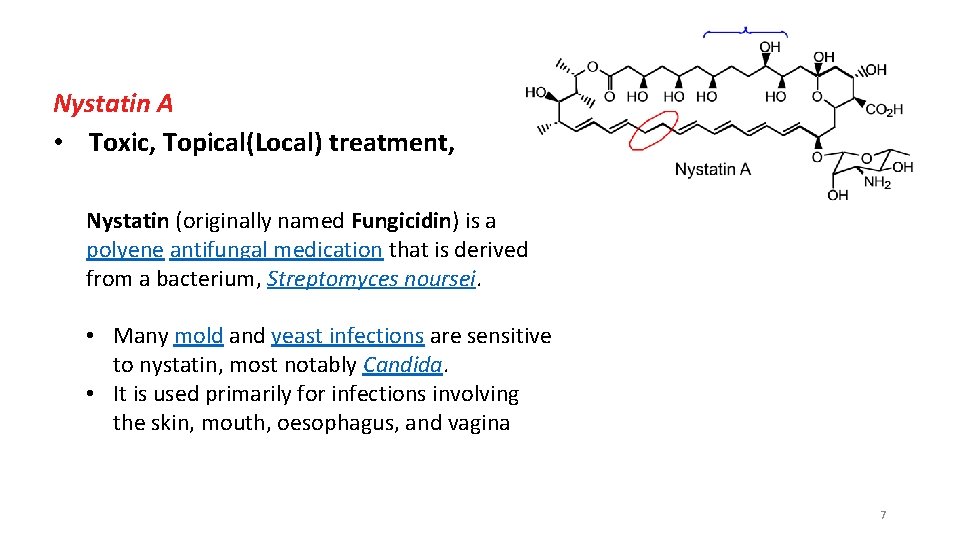
Nystatin A • Toxic, Topical(Local) treatment, Nystatin (originally named Fungicidin) is a polyene antifungal medication that is derived from a bacterium, Streptomyces noursei. • Many mold and yeast infections are sensitive to nystatin, most notably Candida. • It is used primarily for infections involving the skin, mouth, oesophagus, and vagina 7

Synthetic Antifungals Azoles • Inhibit the synthesis of sterol components of fungal membrane • Removes methyl group from lanosterol • Azoles reduces ergosterol level…. leads to loss of cytoplasmic constituents • Side effects- reduces cholesterol synthesis 8
Ketokonazol: • • Orally-used for systematic fungal infections Less toxic than Amphotercic B Occasional liver damage Topical ointment to treat dermatomycocses Voriconazole • Replaced Amphotericin B for systematic fungal infection • Treatment of Aspergillosis of the CNS…. is able to penetrate the blood –brain barrier 2 or 3 other aromatic rings 9
Griseofulvin • Produced by Penicillium griseofulvin • Active against superficical dermatophytic fungal infection of the hair(tinea capitis or ringworm) and nails even though it’s route of administration is oral. • It specifically binds to the keratin found in skin, hair follicles and nails • It’s mode of infection –to block microtubules assembly which interfere with mitosis and thereby inhibits fungal reproduction 10

Anidulafungin • It is a member of the class of antifungal drugs known as the echinocandins; • Its mechanism of action is by inhibition of (1→ 3)-β-D-glucan synthase, an enzyme important to the synthesis of the fungal cell wall. • Glucan synthase is not present in mammalian cells, so it is an attractive target for antifungal activity. 11

• Anidulafungin is manufactured via semisynthesis. • The starting material is echinocandin B (a lipopeptide) fermentation product of Aspergillus nidulans • Anidulafungin has proven efficacy against esophageal candidiasis, but its main use will probably be in invasive Candida infection; • it may also have application in treating invasive Aspergillus infection. 12
- Slides: 12