Antiepileptic Medications The Good The Bad and the

Antiepileptic Medications The Good The Bad and the Scary Carolyn Zook Lewis, CPNP, AC/PC, PMHS UNC Child Neurology Chapel Hill, NC

Learning Objectives • Describe the factors that would guide selection of a specific antiepileptic drug for an individual patient • Discuss general considerations and patient/parent counseling regarding black box warnings and antiepileptic medication • Describe the role of therapeutic drug monitoring in the management of a patient with epilepsy • Understand the cognitive effects of various antiepileptic medications • Formulate appropriate counseling information regarding hormonal/reproductive health considerations of antiepileptic drug treatment

2017 ILAE Seizure Classification System Step One • Classifying seizure type • Identify onset • Generalized • Focal • Unknown • Specify level of awareness • Aware • Impaired awareness • Motor or non-motor onset • Sensory • Autonomic

2017 ILAE Seizure Classification System Step Two • Classify epilepsy based on seizure type • Focal-replaces partial onset to describe epilepsy associated with seizures that arise from clinical or EEG data localizing to one hemisphere • Generalized-seizures originate within or rapidly spread to both hemispheres • Combined generalized and focal-epilepsies that have both generalized and focal seizures. Includes most severe epilepsy syndromes • Unknown-epilepsies with seizures in which it cannot be clearly determined whether onset is focal or generalized.

2017 ILAE Seizure Classification System Step Three • Diagnosis of epilepsy syndrome • Incorporates seizure types, EEG, and imaging features • Considers age-dependent features such as age at onset and remission (where applicable) • Seizure triggers • Diurnal variation • Prognosis • Comorbidities • Imaging findings • Implications for etiology and treatment

2017 ILAE Seizure Classification System Step Four • Determine etiology and potential treatment implications • • • Structural (genetic or acquired or both) Genetic Infectious Metabolic Immune Unknown

Management Options • Prevention • Antiepileptic medications • Dietary • Devices • Treatment • Abortive medications • Treatment of status epilepticus

Risk of Reoccurrence Risk of seizure recurrence — A developmentally normal child with no history of a neurologic d/o and has first unprovoked seizure has a 24% risk of having another seizure in the next year and a 45% over the next 14 years • Clinical factors associated with an increased risk of recurrent seizures include: • Prior neurologic insult • Significant magnetic resonance imaging (MRI) findings • Abnormal electroencephalogram (EEG) • Practice parameter for the treatment of a child with a first unprovoked seizure published by the Quality Standards Subcommittee of the American Academy of Neurology and the Practice Committee of the Child Neurology Society provides the following recommendations: • Treatment with AEDs is not indicated for the prevention of the development of epilepsy • Treatment with AEDs may be considered when the benefits of reducing the risk of a second seizure are greater than the risks of pharmacologic and psychosocial side effects

Starting AEDs • After first unprovoked seizure- decision to start medication is based on • Risks of recurrent seizure vs potential risks and benefits of medication • Risks of not treating which include prolonged seizure/status epilepticus • Risks of long term use of AEDs, which include possible effects on school performance, behavior, and allergic reactions • Cost and financial burden of AEDs, office visits, laboratory tests, and struggles associated with administering medication should also be considered • Most children who present with a second unprovoked seizure are usually started on an AED. 2 or more unprovoked seizures is the diagnosis of epilepsy and indicates an increased risk for additional seizures • Some parents may choose not start AEDs if the seizures are infrequent and/or mild • Children with absence and atonic seizures, drop attacks, and infantile spasms are always treated as they almost always present with multiple seizures

Choosing the Right Medication • Monotherapy is the goal of epilepsy treatment as it is associated with • • better compliance fewer adverse effects less potential for teratogenicity lower cost • Medications are divided into “older” and "newer" based upon approval time and availability • Optimal choice of AED is one that is • • • highly effective for type of seizure and the epilepsy syndrome has least number of side effects easy to give and long lasting cost effective does not require lab monitoring

Older Medications • Carbamazepine • Used for partial seizures • Need to monitor blood levels, CBC and LFTs as can rarely cause leukopenia, thromocytopenia, pancreatitis, elevated liver enzymes • Increased risk for severe allergic reaction in Asian population (and recently in Northern Europeans) so FDA recommends HLA genetic testing prior to staring • Ethosuxamide • Used for absence seizures only. Rarely causes agranulocytosis, pancytopenia, leukopenia, blood dyscrasias • Phenobarbital • Used for generalized and partial seizures • Monitor blood levels. Can cause behavior problems and slowed development • Valproic Acid • Used for generalized and partial seizures • Need to monitor blood levels, CBC and LFTs as can rarely cause aplastic anemia, thrombocytopenia, pancreatitis, hepatotoxicity. Increased risk for birth defects. • Benzodiazepams (diazepam, lorazepam, chlorazepate) Usually used as a short term treatment for increased seizures

Newer Medications • Lamotrigine-Used for generalized and partial seizures. Can have a severe allergic reaction with Steven’s. Johnson rash so started very slowly • Levetiracetam-Used for generalized and partial seizures. Can cause irritability • Oxcarbazepine- Used for partial seizures. May cause dizziness and double vision • Topiramate- Used for generalized and partial seizures. Can cause kidney stones, glaucoma, weight loss, inability to sweat, memory problems, and difficulty with concentration • Zonisamide- Used for generalized and partial seizures. Can cause loss of appetite, upset stomach, headache, dizziness, fatigue, kidney stones, and decreased sweating • Rufinamide-FDA approved in 2008 to be used as an adjunctive medicine in children >4 years and adults with Lennox-Gastaut syndrome • Lacosamide- FDA approved 2008 to be used as an adjunctive medicine in adults with partial-onset epilepsy • Clobazam - Approved 1/12 for adjunctive treatment of seizures associated with Lennox-Gastaut syndrome (LGS) in patients two years and older • Vigabatrin - Approved in 1/09 for infantile spasms, but with very strict stipulations. Approved in many other countries for many years. 25 % of patients who take it for a long time suffer damage to the retina of the eye which affects the visual fields
Prevention Medications Focal Onset • Carbamazepine • Oxcarbazepine • Lacosamide Used for both focal and generalized Generalized Onset • Phenobarbital • Valproic Acid • Lamotrigine • Ethosuxamide • Levetiracetam Special uses • Topiramate • Benzodiazepams (diazepam, lorazepam, chlorazepate)-Usually used as a short term treatment for increased seizures • Vigabatrin • Clobazam • Zonisamide
Medications to Treat a Seizure • Rectal Diazepam – Used to treat a prolonged seizure – Dosed according to age • 2 -5 years 0. 5 mg/kg • 6 -11 years 0. 3 mg/kg • 12+ years 0. 2 mg/kg • Intranasal/intrabucchal Midazolam – Not yet FDA approved but being studied – Studies show works as well as Diastat – Less invasive, less expensive – Currently have to use IV version • Intrabucchal Ativan

Treatment Outcomes • About 50% of people with seizures never have another seizure after starting AEDs • About 80% eventually have seizure under control with standard treatment • The remaining 20% continue to have seizures despite trials of several medications. They are considered intractable • If a patient fails 2 -3 drugs at maximally tolerated doses(intractable) there is about a 5% chance that further medications will be successful • That is when other options are considered • Ketogenic diet • Biomechanical devices (VNS, RNS) • Epilepsy surgery

Alternatives • Ketogenic diet-High fat, adequate protein, very low carbohydrate diet (ratio of fat to carbohydrates+protein) • Places body into ketosis which is thought to improve seizure control • Have to consider all sources of sugar, including OTC and RX medications, toothpaste, etc. Need “sugar free” medications, usually can not take liquid antibiotics or chewables, will need capsules or tablets • Vagus Nerve Stimulator-(VNS) prevent seizures by sending pulses of electrical energy to the brain via the vagus nerve. Pulses are supplied by a device similar to a pacemaker (generator) implanted into chest with wire extending into the neck and attaching to the vagus nerve • Responsive Neurostimulation-(RNS)-neurostimulator placed under the scalp and within the skull with one or two leads placed at the seizure target and connected to the neurostimulator. The neurostimulator continuously monitors the brain’s activity and is programmed to detect and record atterns that could lead to a seizure. When patterns are detected, the neurostimulator responds with brief pulses of electricity intended to disrupt the abnormal brain activity before a seizure occurs. Detection and stimulation settings are individualized for each patient’s patterns and so that stimulation is not felt. Patient gets a take-home monitor so that brain activity data can be sent to Neurologist between visits
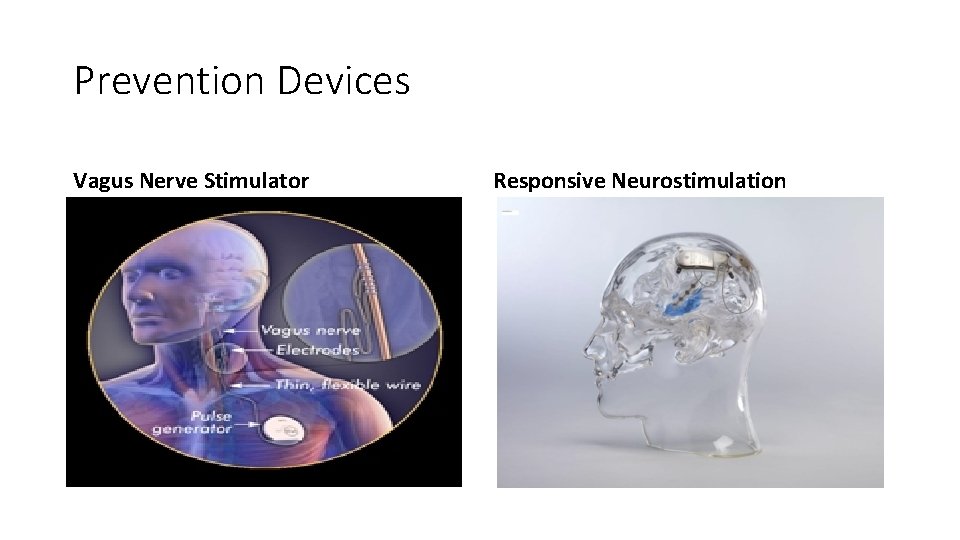
Prevention Devices Vagus Nerve Stimulator Responsive Neurostimulation

Cannabidiol (CBD) • Cannabidiol(CBD)- one of the chemicals in the cannabis sativa plant (marijuana). There are over 60 cannabinoids(chemicals in the cannabis plant) of which cannabidiol and THC are present in greatest concentrations. Cannabidiol is hypothesized to have anti seizure properties. • THC(tetrahydrocannabinol)- also one of the main chemicals in marijuana. It is the part that makes people high. Hemp has very low levels of THC. The effect of THC on seizures is unknown • Marijuana and hemp are both varieties of the same plant but the marijuana plant has been bred to have high amounts of THC, and the hemp plant has very low levels of THC, but higher levels of cannabidiol (the component that is thought to be possibly effective at treating seizures)

Cannabidiol (CBD) • Hemp oil is produced by pressing the seeds, stalks or leaves from the hemp plant. There is little to no THC in hemp oil and larger amounts cannabidiol. Most commercially available hemp oils do not have enough cannabidiol to have a therapeutic effect on seizures • Cannabidiol oil(CBD) is made from a cannabis plant that has a higher concentration of CBD. It can also be made from different extraction processes to make it more concentrated • “Charlotte’s Web” is a particular strain of the cannabis sativa plant that was originally grown in Colorado that claims to be high in cannabidiol and has anecdotally helped children who have difficult to control seizures gain better seizure control • THERE ARE CURRENTLY NO PUBLISHED EVIDENCE BASED TRIALS TO DATE ESTABLISHING EFFICACY OR SAFETY OF CANNABIDIOL • Cannabidiol oil and hemp oil are not regulated anyone can make them. There are varying amounts (if any) of cannabidiol in these products making it difficult to know the correct amount or side effects. Since the oils are not regulated by the FDA there may be contaminants in them that are harmful (pesticides, solvents, molds) • There are studies in progress using a pharmacy grade form of cannabidiol (Epidiolex) that are showing positive results and some side effects. No FDA approval yet. States have different laws about use • NC Law: SESSION LAW 2015 -154 and HOUSE BILL 766

Management of AEDs • If a patient continues to have seizures at maximally tolerated dose another AED is started • If patient has good seizure control after completing taper up on new AED then wean of old medication is considered • Studies have shown best time frame to wean off AEDs is 6 -8 weeks • If a patient is seizure free for a minimum of 2 -3 years on AEDs it is time to consider weaning off

Role of Genetic Testing • Of approx. 20, 000 different genes at least 1/3 are expressed in the brain • Influence development and function of the brain • Combined with environmental factors gene changes can also determine risk for disease and course the disease will follow • It is now thought that genetic factors account for about 40% of the etiologic causes of epilepsy • Current studies showing up to 500 different genes are associated with epilepsy • Genetic changes associated with epilepsy • Encode subunits of ion channels involved in stabilizing or propagating neuronal activity, including components of the voltage gated sodium, potassium, and calcium channels and gated gamma aminobutyric (GABA) and nicotinic acetylcholine receptor channels • Non ion channel genes associated with a variety of neurotransmitter, storage and other neurometabolic disorders, • Genes causing syndromic forms of epilepsy, many of which are involved in transcriptional activation or repression

Pros and Cons of Genetic Testing Pros • Yield up to 35 % if FH epilepsy or child has DD, drug resistant epilepsy, abnormal neuro findings • Chance of finding potentially treatable conditions (vitamin responsive epilepsy) • Helps explain prognosis and family acceptance • Helps with choice of AED • Avoidance of AED • Diagnoses conditions such as glucose transporter d/o leading to treatment with ketogenic diet • Leads to development of novel therapies Cons • Yield of usual cases is so low does not justify cost unless family history of epilepsy, child has DD, drug resistant epilepsy, or abnormal neuro findings • Cost • Variants of unknown significance (1/3 of results)

Implications • Sodium channel abnormalities such as SCN 1 A • Severe type associated with Dravet syndrome and Lennox Gastaut (called epileptic encephalopathies) • Avoid sodium channel AEDs (carbamazepine, lamotrigine) makes seizures worse • Poor prognosis • Milder version –GEFS+ (generalized epilepsy with febrile seizures plus afebrile seizures • Better prognosis • Avoid sodium channel drugs • POLG-gene that codes mitochondrial DNA polymerase gamma • Poor prognosis • Avoid valproic acid and Depakoke-can cause severe liver problems and death • HLA- US FDA recommends HLA testing prior to treatment with carbamazepine (Tegretaol) in Asian patients due to high risk for SJS • Potassium channel abnormalities KCNQ 2 and KCNQ 3 - associated with BECTS (BRE)

Label Warning Suicide • In 2008 FDA issued a warning about increased risk of suicidal thoughts when taking AEDs • Recommended patients being treated with antiepileptic drugs for any indication should be monitored for the emergence or worsening of depression, suicidal thoughts or behavior, or any unusual changes in mood or behavior • Data from pharmaceutical companies reviewed information from 199 placebo controlled trials of 11 AEDs used for various indications (25% epilepsy patients, 27% psychiatric patients and 48% other conditions). Included 28, 000 people taking AEDs and over 16, 000 people taking placebo • Found that patients taking AEDs had about twice the risk of suicidal behavior compared with patients taking a placebo. • The absolute risk amounted to about 1 added case of suicidal thoughts or behaviors for every 500 patients taking the antiepileptic drugs versus placebo. • The mechanism linking antiepileptic drugs with potential suicide risk remains unknown • As a result of the analysis, the FDA required that all manufacturers of drugs in this class include a warning in their labeling and develop a medication guide for patients, informing them of the risks of suicidal thoughts or actions

Black Box Warnings • Lamotrigine (Lamictal)-serious skin rashes (and SJS) can occur. Rate is 8/1000. Usually happens in first 8 weeks of therapy but can occur later with dose increases • Carbamazepine (Tegretol)-can cause serious skin reactions such as toxic epidermal necrolysis and Stevens Johnson Syndrome, especially in Asian population. Also associated with aplastic anemia and agranulocytosis. CBC with platelets recommended prior to starting and periodically based on clinical judgement • Valproic Acid (Depakote)- hepatotoxicity, teratogenicity, and pancreatitis. Education important in females of childbearing age before starting. Monitor LFTs • Felbamate- aplasitic anemia-parents have to sign a consent form • Perampanel (Fycompa)-serious or life-threatening psychiatric and behavioral adverse reactions including aggression, hostility, irritability, anger, and homicidal ideation and threats, even in patients without prior psychiatric history, or aggressive behavior

Therapeutic Drug Monitoring • TDM is used when trying to optimize dosage to get best clinical efficacy while minimizinge side effects • Reference ranges are only guidelines that to indicate range of likely therapeutic response, however many patients may require target concentrations outside the reference range. • Clinical decisions about dosing are based on multiple factors including • • type and severity of epilepsy pathological and physiological states drug interactions variability of pharmacogenetics • Many factors can effect serum concentration of medication • timing of taking medication and blood draw- even trough levels fluctuate up to 15 to 20 percent in many patients who take the drug on a consistent schedule. • patients who are frequently noncompliant may take enough medication shortly before the test to attain a therapeutic level • laboratory errors • generic substitution for brand-name AEDs • variable potency of pills (following improper storage, for example) • menstrual cycle (midcycle levels may be higher than during the premenstrual period or menses)

Mood Disorders and Epilepsy • • Psychiatric comorbidities occur in 37%-77% of pediatric patients with epilepsy Attention deficit hyperactivity disorder is most common in children Depression was the most common psychiatric comorbidity in adolescent Studies have shown prevalence of depression ranging between 30% to 50% in all people with epilepsy Meta-analysis of 12 studies showed people with epilepsy are more than 5 times as likely to commit suicide than the general population AEDs have mechanisms of action responsible for anti-seizure activity and effect on mood and behavior A number of studies have suggested some AEDs are associated with symptoms of depression while others act as antidepressants Anxiety, panic, and phobic disorders also occur more frequently especially in patients with frontal or temporal lobe seizures (areas involved in memory and emotion)

Cognitive Effects of AEDs • Antiepileptic drugs (AEDs) as well as seizures are known to affect learning, education, social development and behavior • 20 -30% of children with epilepsy have learning difficulties • No AED is free from unfavorable cognitive or behavioral effects, although some (phenobarbital) cause more than others (Depakote, carbamazepine, lamotrigine) • Some AEDs interfere with processing and memory and some cause fatigue which interferes with the ability to learn • Word-finding difficulty observed with topiramate does not occur with other AEDs • Use of a single drug (monotherapy) is better that polypharmacy • Levitiracitam does not cause learning difficulties but can cause irritability and aggressive behavior

How to Help Children with Epilepsy in School • Based on seizure focus, frequency of seizures, and medication, the child with epilepsy may experience trouble with • Executive function • Language-speech, communication, comprehension • Attention and concentration • Processing speed • memory • Child may also have • intermittent disruptions in their learning that specifically relate to their seizures, sleep patterns, and medications. These disruptions in their ability to attend and learn can change from day to day, or even hour to hour • Night-time seizures or poor sleep patterns caused by abnormal brain activity can increase fatigue during the school day. As a result the child is less attentive and less available to learn • Subclinical seizures which can interfere with processing, consolidation, and retrieval of information recently learned • Seizures during the school day can cause disruptions in memory that result in forgeting what they have just learned • In some cases they cannot remember much about what happened just before or for some time after the seizure

Adolescence • Puberty appears to have an effect on epilepsy • Etiology not completely understood but appears to be multifactoral and both males and females are affected • As puberty is reached hepatic metabolism slows to a rate similar to adults which may lead to a rise in AED levels • Pubertal growth spurts result in rapid weight changes and can lower AED levels • More frequent monitoring of plasma levels and dose adjustments may be needed

Contraception • Interactions between AEDs and oral contraceptives are common • No increased seizure activity with addition of contraceptives but enzyme inducing AEDs (EIAEDs) decrease the effectiveness of contraceptives • WHO recommends women taking EIAEDs including lamotrigine use a method of contraception other than hormonal pill, patch, or ring contraceptives Long-acting reversible contraceptives (LARC), including copper or levonogestrel intrauterine devices and etonogestrel implants are highly effective alternatives that carry no or much less potential for drug-drug interactions • Oral estrogen-progestin contraceptives can increase the metabolism of lamotrigine and reduce plasma drug concentration by about 50% percent. Levels can rise significantly upon discontinuation of oral contraceptive, even during the 7 -day pill free interval. Continuous dosing is preferred • Higher estrogen doses (at least 50 mcg) is recommended for women talking EIAEDs • Progestin only contraception not recommended • IM Medroxyprogesterone (Depo Provera) is ok, but may need to give more frequently in patients on EIAEDs. Long term use should be avoided due to association with decreased bone mineral density. Because of inhibitory effect is being studied as treatment for catmenial epilepsy

Contraceptives Enzyme Inducers • Carbamazepine • Phenobarbital • Phenytoin • Felbamate(mild) • Oxcarbazepine (mild) • Topamax (mild) Non Enzyme Inducers • Gabapentin • Lamotrigine • Levetiracetam • Tiagabine • Valproate • Zonisamide

Pre-pregnancy Counseling • Preconception information should be offered to all females with childbearing potential • Folic acid supplementation should be provided to all women of child bearing potential • Women with epilepsy have a slightly increased risk of fetal malformation in comparison with the general population • This is somewhat due to AED used (3% greater risk with CBZ or LMT, 7% with VPA, 15% with 2 or more AEDs) • Most major malformations occur in the early stages of pregnancy

Common Malformations MAJOR • 4 -8% of all pregnancies-in comparison to 2 -4% in general population • Usually associated with older drugs • Cleft palate and lip • VSD • Neural tube deficits MINOR • 7 -15% of all pregnancies-about 2 times general population • Frequently involve face and digits • Learning and behavior problems

Bone Health • Females and males with epilepsy are at higher risk for bone disease (osteoporosis and osteopenia) that general population • Metabolic bone disease is a recognized consequence of EIAEDs • Mechanism thought to be caused by reduced levels of vitamin D, with subsequent decrease calcium absorption and increased parathyroid concentrations • Valproate is not an enzyme inducer but has been linked to impaired bone health • Recommend patients on AEDS take a vitamin D and calcium supplement and check levels routinely
- Slides: 35