Antidiabetic Medications The Nursing Process Karen Ruffin RN

Antidiabetic Medications & The Nursing Process Karen Ruffin RN, MSN Ed.

Is it Diabetes or is it Hyperglycemia? ? ? ? IS THERE A DIFFERENCE AND IF SO WHAT IS IT? ?

What is ? ? ? ? n Hyperglycemia n Insulin n The primary source of energy for our bodies

What is the difference between n Basel Insulin n Prandial Insulin


Optimal Levels of Blood Sugars n Preprandial-110 mg/dl n Postprandial-180 mg/dl


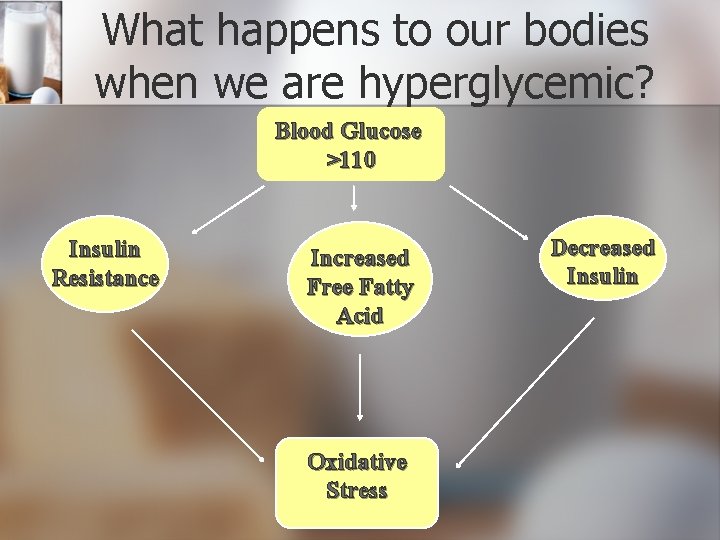
What happens to our bodies when we are hyperglycemic? Blood Glucose >110 Insulin Resistance Increased Free Fatty Acid Oxidative Stress Decreased Insulin

Oxidative Stress hypertension Vascular smooth muscle cell growth Release of chemokines Release of cytokines Expression of cellular adhesion molecules Hyper coagulation Platelet Activation Decreased Fibrinolysis
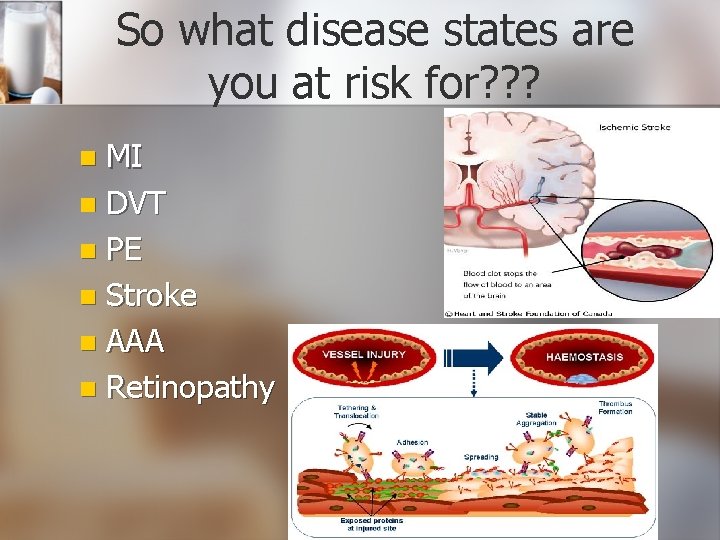
So what disease states are you at risk for? ? ? MI n DVT n PE n Stroke n AAA n Retinopathy n

What happens to our bodies when we are hyperglycemic? Metabolic Stress Response Stress hormones and peptides Increased Glucose Decreased Insulin
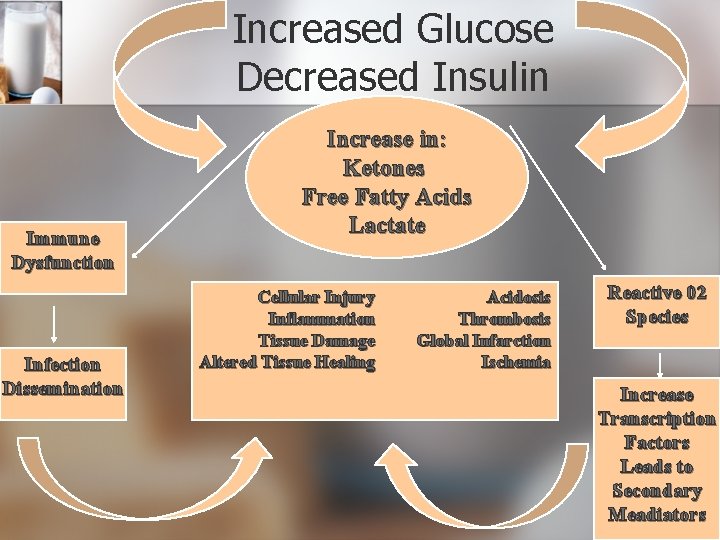
Increased Glucose Decreased Insulin Immune Dysfunction Infection Dissemination Increase in: Ketones Free Fatty Acids Lactate Cellular Injury Inflammation Tissue Damage Altered Tissue Healing Acidosis Thrombosis Global Infarction Ischemia Reactive 02 Species Increase Transcription Factors Leads to Secondary Meadiators

DID YOU KNOW ANY BLOOD SUGAR >200 STUNS YOUR ? ? ? ? FOR 2 WEEK

Criteria for Diagnosis of DM DM Screening Symptoms of diabetes + casual plasma glucose level less than or equal to 200 mg/d. L OR Fasting plasma glucose higher than or equal to 126 mg/d. L OR 2 -hour postload glucose level higher than or equal to 200 mg/d. L during an oral glucose tolerance test Impaired glucose tolerance (IGT) ◦ FPG <110 mg/d. L: normal fasting glucose ◦ FPG ≥ 110 mg/d. L but <126 mg/d. L: impaired fasting glucose (IFG) ◦ FPG ≥ 126 mg/d. L: provisional diagnosis of diabetes mellitus

What is a Hb. A 1 c? n It is a test that allows healthcare providers to see how diabetics have managed their blood glucose level over the last 2 -3 months…. n Why do you think this is important? ?


At what blood glucose level do we start treating with sliding scale? ? ? ? ? So, what do you think we are doing to our patients? ? ?

What is the Difference? ? n Type 1 diabetes n Type 2 diabetes

Type 1 Diabetes n Lack of insulin production OR n Production of defective insulin n Affected patients need exogenous insulin n Complications n Diabetic ketoacidosis (DKA) n Hyperosmolar nonketotic syndrome n Oral antidiabetic drugs not effective

Diabetes Mellitus n Symptoms n Polyuria n Polydipsia n Polyphagia n Glycosuria n Unexplained weight loss n Fatigue n Hyperglycemia

Type 2 Diabetes n Most common type n Caused by insulin deficiency and insulin resistance n Many tissues are resistant to insulin n Reduced number insulin receptors n Insulin receptors less responsive n These people respond to oral hypoglycemics


Type 2 Diabetes • Several comorbid conditions metabolic syndrome OR insulin-resistance syndrome OR syndrome X ◦ ◦ ◦ ◦ Obesity Coronary artery disease Dyslipidemia Hypertension Microalbuminemia (protein in the urine) Enhanced conditions for embolic events (blood clots) Insulin Resistance
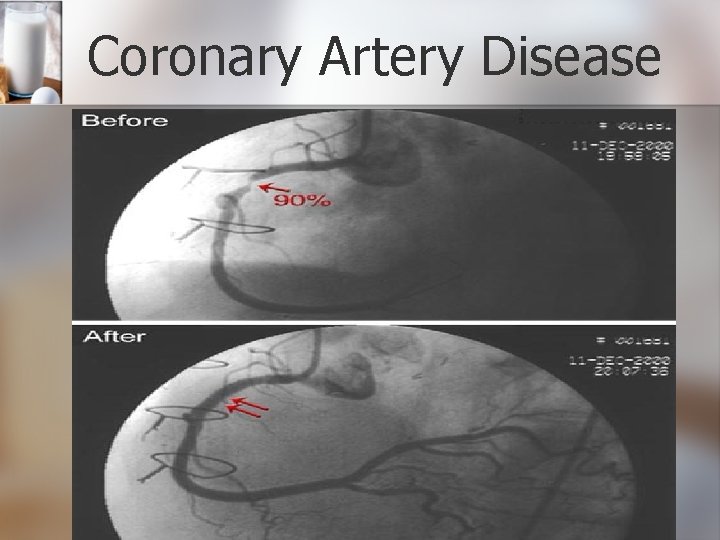
Coronary Artery Disease
Treatment DIfferences Type 1 ◦ Exogenous insulin ◦ Dietary control Type 2 ◦ Lifestyle changes Dietary control Weight reduction Exercise ◦ May require oral hypoglycemic therapy or exogenous insulin n Insulin when oral hypoglycemic medications can no longer provide glycemic control

Gestational Diabetes ◦ Hyperglycemia that develops during pregnancy ◦ Insulin must be given to prevent birth defects ◦ 4% of all pregnancies ◦ Must be reclassified if it persists 6 weeks postdelivery ◦ Usually subsides after delivery ◦ 30% of patients may develop Type 2 DM within 10 to 15 years

Major Long-Term Complications of DM (Both Types) ◦ Macrovascular (atherosclerotic plaque) Coronary arteries Cerebral arteries Renal arteries Peripheral vessels ◦ Microvascular (capillary damage) Retinopathy Neuropathy Nephropathy

Complications Associated with Diabetes Mellitus Cardiovascular disease, including hypertension n Peripheral vascular disease n n Delayed healing Visual defects, including blindness n Renal disease n Infection n Neuropathies n Impotence n

Oral Hypoglycemics n Sulfonylureas (oldest) n Meglitinides n Biguanide n Thiazolidinediones

Indications for Oral Hypoglycemics They are used to lower blood sugar levels in patients that diet and exercise have failed. n The patient must have some pancreatic function left. n They can be used as a monotherapy or in conjunction with other oral hypoglycemics. n

Contraindications Know drug allergy n Active hypoglycemia n Usually not used during pregnancy subq insulin's are used then. n Liver disease n Kidney disease n n Depending on the metabolic pathways of the medication

Sulfonylureas n First generation: n chlorpropamide (Diabinese), n tolazamide (Tolinase) n tolbutamide (Orinase) n Second generation: n glimepiride (Amaryl) n glipizide (Glucotrol) n glyburide (Dia. Beta, Micronase)

Sulfonylureas n Stimulate insulin secretion from the beta cells of the pancreas, thus increasing insulin levels n Beta cell function must be present n Improve sensitivity to insulin in tissues n Result: lower blood glucose levels n First-generation drugs not used as frequently now

Adverse Effects n Sulfonylureas n n n Hypoglycemia hematologic effects nausea epigastric fullness heartburn many others

Interactions n Sulfonylureas n Hypoglycemic effect increases when taken with alcohol, anabolic steroids, many other drugs n Adrenergics (beta blockers) may mask many of the symptoms of hypoglycemia n Hyperglycemia: corticosteroids, phenothiazines, diuretics, oral contraceptives, thyroid replacement hormones, phenytoin, diazoxide and lithium. n Allergic cross-sensitivity may occur with loop diuretics and sulfonamide antibiotics n May interact with alcohol/OTC medication containing alcohol) - causing a disulfiram (Antabuse) -type reaction (facial flushing, pounding headache, feeling of breathlessness, and nausea)

Meglitinides n repaglinide n n (Prandin) nateglinide (Starlix) Meglitinides n Action similar to sulfonylureas n Increase insulin secretion from the pancreas

Adverse Effects n Meglitinides n Headache n hypoglycemic effects n Dizziness weight gain n joint pain n upper respiratory infection or flu-like symptoms n

Biguanides n metformin (Glucophage) n Biguanides n Decrease production of glucose n Increase uptake of glucose by tissues n Does not increase insulin secretion from the pancreas (does not cause hypoglycemia)

Adverse Effects n Metformin n Primarily affects GI tract: abdominal bloating, nausea, cramping, diarrhea, feeling of fullness n May also cause metallic taste, reduced vitamin B 12 levels n Lactic acidosis is rare but lethal if it occurs n Does not cause hypoglycemia

Thiazolidinediones n pioglitazone (Actos), n rosiglitazone (Avandia) n Also known as “glitazones” n Thiazolidinediones n Decrease insulin resistance n “Insulin sensitizing drugs” n Increase glucose uptake and use in skeletal muscle n Inhibit glucose and triglyceride production in the liver

Adverse Effects n Thiazolidinediones n Moderate weight gain n Edema n Mild anemia n Hepatic toxicity—monitor liver function tests

Alpha-glucosidase Inhibitors n Alpha-glucosidase inhibitors n acarbose (Precose) n miglitol (Glyset) n Alpha-glucosidase inhibitors n Reversibly inhibit the enzyme alpha-glucosidase in the small intestine n Result: delayed absorption of glucose n Must be taken with meals to prevent excessive postprandial blood glucose elevations (with the “first bite” of a meal)

Adverse Effects n α-glucosidase inhibitors n Flatulence n n diarrhea abdominal pain n Do not cause hypoglycemia, hyperinsulinemia, or weight gain

Insulins n Mechanism of Action n Substitute for & same effects as endogenous insulin n n Restores the diabetic patient’s ability to: n Metabolize carbohydrates, fats, and proteins n Store glucose in the liver n Convert glycogen to fat stores Some derived from porcine sources n Most now human-derived, using recombinant DNA technologies n Goal: tight glucose control n To reduce the incidence of long-term complications

Indications n To treat both types of diabetes n Each patient requires careful customization of the dosing regimen for optimal glycemic control

Contraindications n Anyone who is hypoglycemic? ? ?

Adverse Effects n Are all signs and symptoms of hypoglycemia including shock and death.

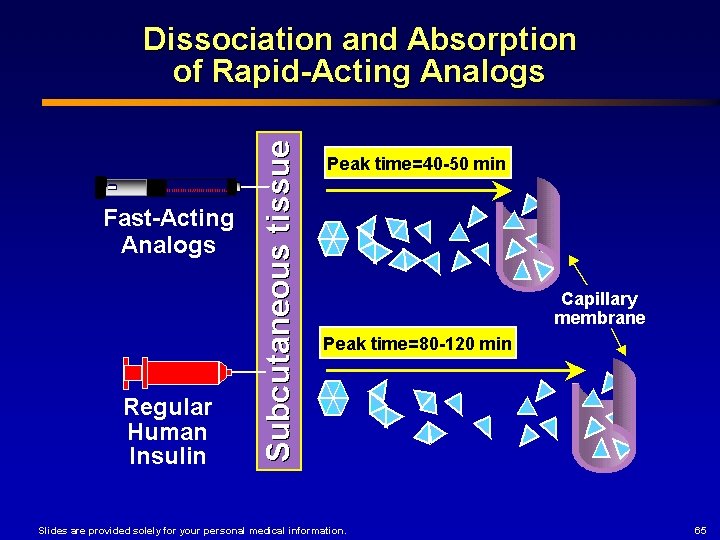
Human-Based Insulins n Rapid-Acting n n Most rapid onset of action Shorter duration Insulin Onset (mins) Peak (hrs) Duration (hrs) aspart (Novolog) 2 -33 1 -3 3 -5 lispro (Humalog) 2 -33 30 mins – 2. 5 3 -6. 5 glulisine (Apidra) 2 -33 30 mins – 1. 5 1. -25 May be given SC or via continuous SC infusion pump (but not IV)


Human-Based Insulins n Short-Acting n regular insulin (Humulin R, Novolin R) Insulin Onset (mins) Peak (hrs) Duration (hrs) Humulin R 30 mins to 4 hrs 2. 5 -5 5 -10 Novolin R 30 2. 5 -5 8 n Onset n The 30 – 60 minutes only insulin product that can be given by IV bolus, IV infusion, or even IM
Sliding-Scale Insulin Dosing n SC rapid or short-acting doses adjusted according to blood glucose test results n Typically used in hospitalized diabetic patients n n Or in patients on TPN / enteral tube feedings or receiving steroids Subcutaneous insulin is ordered in an amount that increases as the blood glucose increases

Human-Based Insulins n Intermediate-Acting n isophane insulin suspension (also called NPH) (Humulin N, Novolin N) n isophane insulin suspension & insulin injection (Humulin 50/50 , Humulin 70/30, Novolin 70 -30) n Lispro protamine suspension (Humalog 75/25, Novolog Mix 70/30) n insulin zinc suspension (Lente, Novolin L) Cloudy appearance n Slower in onset and more prolonged duration than endogenous insulin n
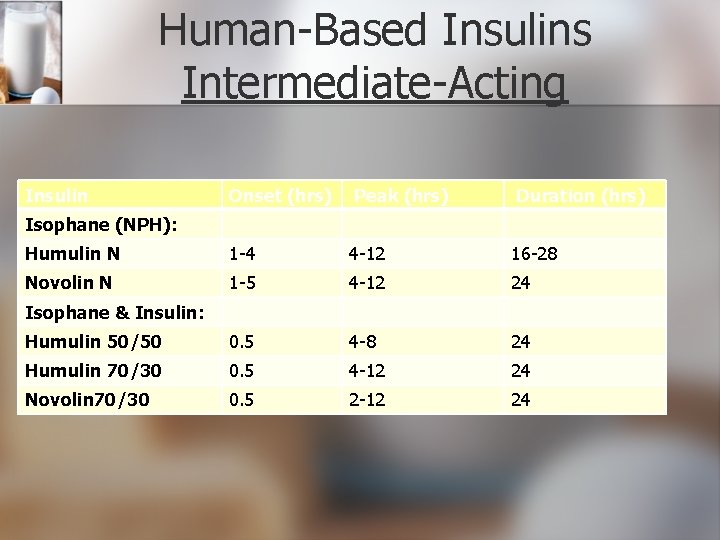
Human-Based Insulins Intermediate-Acting Insulin Onset (hrs) Peak (hrs) Duration (hrs) Humulin N 1 -4 4 -12 16 -28 Novolin N 1 -5 4 -12 24 Humulin 50/50 0. 5 4 -8 24 Humulin 70/30 0. 5 4 -12 24 Novolin 70/30 0. 5 2 -12 24 Isophane (NPH): Isophane & Insulin:
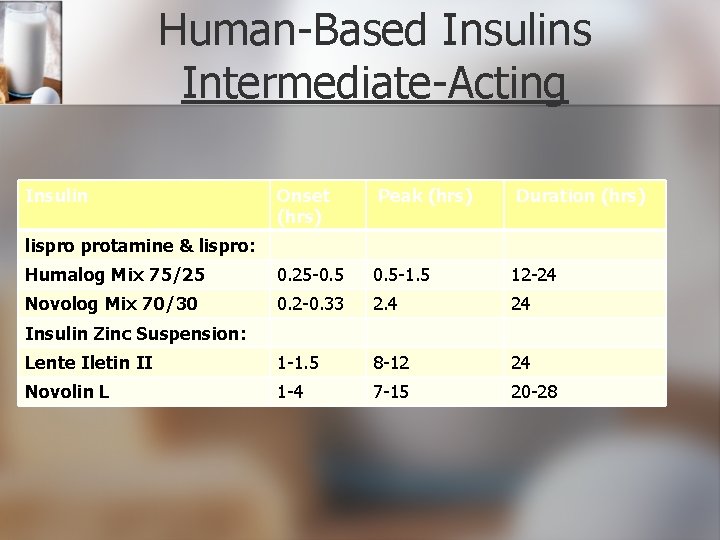
Human-Based Insulins Intermediate-Acting Insulin Onset (hrs) Peak (hrs) Duration (hrs) Humalog Mix 75/25 0. 25 -0. 5 -1. 5 12 -24 Novolog Mix 70/30 0. 2 -0. 33 2. 4 24 Lente Iletin II 1 -1. 5 8 -12 24 Novolin L 1 -4 7 -15 20 -28 lispro protamine & lispro: Insulin Zinc Suspension:

Human-Based Insulins n Combination Insulin Products n NPH 70% and regular insulin 30% (Humulin 70/30, Novolin 70/30) n NPH 50% and regular insulin 50% (Humulin 50/50) n insulin lispro protamine suspension 75% and insulin lispro 25% (Humalog Mix 75/25)
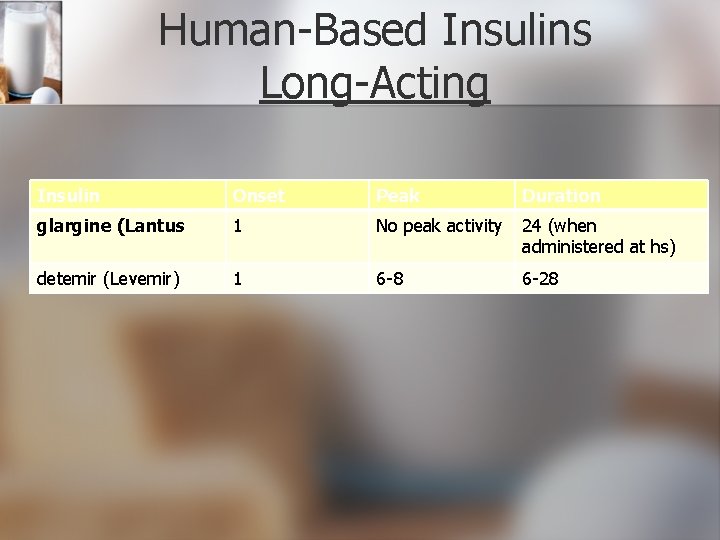


Human-Based Insulins Long-Acting Insulin Onset Peak Duration glargine (Lantus 1 No peak activity 24 (when administered at hs) detemir (Levemir) 1 6 -8 6 -28



DM Monitoring – Daily AC & HS n Ante Cibum: before meals n HS: Hour of Sleep: prior to taking any HS snack n Rapid or short acting insulin used to cover any blood sugar (accucheck, chemstrip) n Dose by protocol (protocols are usually hospital-based) for any result greater than 150 mg/d. L n Usually 1 -2 U for every 50 mg/d. L >150 with special instructions to notify physician if >300 mg/d. L
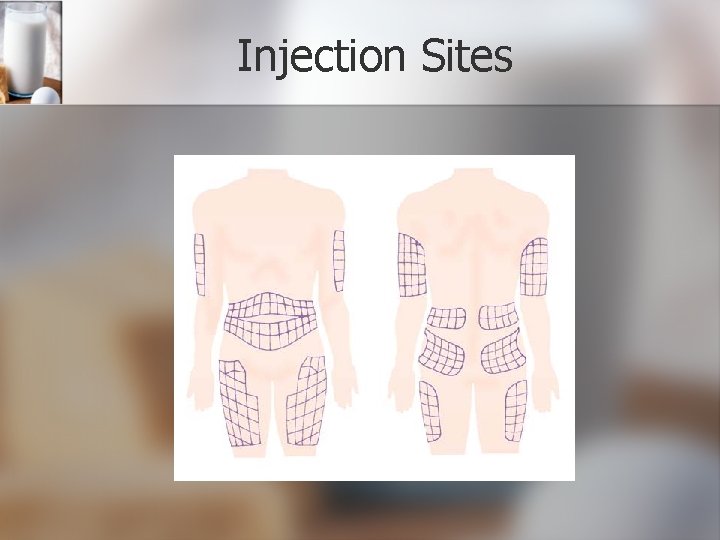
Injection Sites
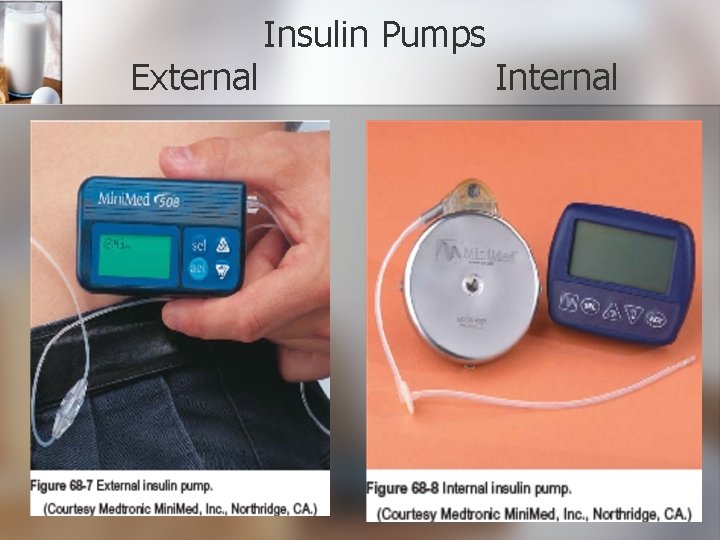
External Insulin Pumps Internal

Hypoglycemia Adverse Effect of Insulin Early ◦ Confusion, irritability, tremor, sweating Later ◦ Hypothermia, seizures ◦ Coma and death will occur if not treated Abnormally low blood glucose level Mild cases can be treated with diet—higher intake of protein and lower intake of carbs—to prevent a rebound postprandial hypoglycemia (<50 mg/d. L)



Good way to remember!!!

Diabetic Ketoacidosis n n State of hyperglycemia with ketosis Usually results from infection, environment, or emotional stressor n As a result of Lack of Insulin, Breakdown: n Fat – free fatty acids in liver – ketone bodies – ketones in urine n Protein – to form new glucose / increased BUN n Glycogen to glucose (decrease use of glucose because of decreased insulin) n Osmotic diuresis n Dehydration / Electrolyte Imbalance n Hyperosmolality Hemoconcentration n Acidosis n Death

Diabetic Ketoacidosis n n n Sudden onset Factors: infection, stressors, inadequate insulin Kussmaul respiration / fruity odor to breath, nausea, abdominal pain Dehydration, electrolyte imbalance, polyuria, polydipsia, weight loss, dry skin, sunken eyes, soft eyeballs, lethargy, coma Glucose >300 mg/d. L p. H <7. 35 / Bicarbonate < 15 m. Eq/L Cr >1. 5 mg/d. L n Blood & Urine Ketones - Positive n Na – low / K+ </> /


Hyperglycemic-hyperosmolar nonketotic syndrome (HHNS) State of hyperglycemia without ketosis n Little breakdown of fat (little or no ketone bodies) n Breakdown n n Glycogen– formation of new glucose – hyperglycemia n Very high levels of glucose >800 mg d. L n Osmotic diuresis – extracellular dehydration n Renal insufficiency – hyperosmolality – intracellular dehydration n Hypokalemia – shock – tissue hypoxia - Coma

Hyperglycemic-hyperosmolar nonketotic syndrome (HHNS) n n n n n Gradual onset Factors: infection, other stressors, poor fluid intake Altered CNS function – neurologic symptoms Dehydration / electrolyte loss Glucose > 800 mg/d. L p. H >7. 4 / Bicarbonate >20 m. Eq/L Na & K+ normal or low Bun & Cr – elevated Blood & Urine Ketones - negative

Hyperglycemic-hyperosmolar nonketotic syndrome (HHNS Treatment n Rehydrate with NS (if severe) or ½ NS n Use n CVP or PCWP / UO / blood pressure monitoring IV insulin According to Sliding Scale n Never n Reduce hyperglycemia by 10% /hr Replace Potassium (will not be as severe as DKA)

Antidiabetic Drugs: Nursing Implications n Before giving any drugs that alter glucose levels, obtain and document: n. A thorough history n Vital signs n Blood glucose level, Hb. A 1 c level n Potential complications and drug interactions

Antidiabetic Drugs: Nursing Implications n Before giving any drugs that alter glucose levels: n Assess the patient’s ability to consume food n Assess blood glucose level n Assess for nausea or vomiting n Hypoglycemia may be a problem if antidiabetic drugs are given and the patient does not eat n If a patient is NPO for a test or procedure, consult physician to clarify orders for antidiabetic drug therapy

Antidiabetic Drugs: Nursing Implications n Keep in mind that overall concerns for any diabetic patient increase when the patient: n Is under stress n Has an infection n Has an illness or trauma

Antidiabetic Drugs: Patient Education Thorough patient education is essential regarding: ◦ Disease process ◦ Other Risk Factors: Smoking HTN CAD ◦ Self-Care: Medication Psychological adjustment Nutrition Activity and Exercise Blood-glucose testing Self-administration of insulin or oral drugs ◦ Potential complications How to recognize and treat hypoglycemia and hyperglycemia
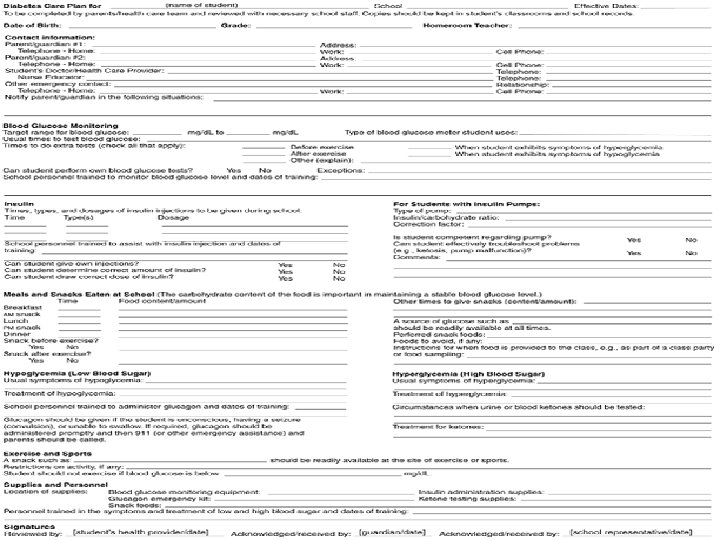

FIGURE 36 -3 Diabetes health care plan. Mosby items and derived items © 2007, 2004 by Mosby, Inc. , an affiliate of Elsevier Inc.

Nursing Implications Insulin When insulin is ordered, ensure: ◦ ◦ Correct route Correct type of insulin Timing of the dose Correct dosage Insulin order and prepared dosages are second -checked with another nurse ◦ ◦ ◦ Check blood glucose level before giving insulin Roll vials between hands them to mix suspensions – no shaking! Ensure correct storage of insulin vials ONLY insulin syringes, calibrated in units, to administer insulin Ensure correct timing of insulin dose with meals

Nursing Implications Insulin n When drawing up two types of insulin in one syringe: n Always withdraw the regular or rapid-acting insulin first n Provide thorough patient education regarding self-administration of insulin injections, including timing of doses, monitoring blood glucoses, and injection site rotations

Nursing Implications Oral Antidiabetic drugs n Always check blood glucose levels before giving n Usually given 30 minutes before meals n Administer the medication at exact time – with meal or when food is in sight* n Alpha-glucosidase inhibitors are given with the first bite of each main meal n Metformin is taken with meals to reduce GI effects

Nursing Implications Insulin & hypoglycemic medications Assess for signs of hypoglycemia n If hypoglycemia occurs: n n Give glucagon or n Have the patient eat glucose tablets or gel, corn syrup, honey, fruit juice, or nondiet soft drink or n Have the patient eat a small snack such as crackers or half a sandwich n Monitor blood glucose levels


Nursing Implications n Monitor for therapeutic response n Decrease in blood glucose levels to the level prescribed by physician n Measure hemoglobin A 1 c to monitor longterm compliance to diet and drug therapy n Watch for hypoglycemia and hyperglycemia


Review n When administering insulin, the nurse must keep in mind that the most immediate and serious adverse effect of insulin therapy is which of the following? n A: Hyperglycemia n B: Hypoglycemia n C: Bradycardia n D: Orthostatic Hypotension

Review n A dose of long acting insulin has been ordered for bedtime for a diabetic patient. The nurse expects to give which type of insulin? n A: Regular n B: Lente n C: NPH n D: Glargine (Lantus)

Review n A Patient is to be placed on an insulin drip to control his high blood glucose levels. The nurse knows that which of the following is the only type of insulin that can be given IV? n A: Regular n B: Lente n C: NPH n D: Ultralente

Review n While monitoring a patient who is receiving insulin therapy, the nurse observes for signs of hypoglycemia, such as which of the following? n A: Decreased pulse and respiratory rate and flush skin. n B: Increased pulse rate and a fruity, acetone breath odor. n C: Weakness, sweating, and confusion. n D: Increased urine output and edema.

Review n When giving oral acarbose (Precose), the nurse should administer it at what time? n A: 15 minutes before meal n B: 30 minutes before meal n C: with the first bite of a meal n D: 1 hour after eating

Review n A patient taking rosiglitazone (Avandia) tells the nurse, “There’s my insulin pill!” The nurse describes the mechanism of action of Avandia by explaining that this drug is not insulin but it works by: n A: Stimulating the beta cells of the pancreas to produce insulin. n B: Decreasing insulin production. n C: Inhibiting hepatic glucose production. n D: Decreasing intestinal absorption of glucose.
- Slides: 92