Anticonvulsants Anxiolytics Rishi Gandhewar 240319 Overview Anticonvulsants SBAs

Anticonvulsants & Anxiolytics Rishi Gandhewar 24/03/19

Overview Anticonvulsants SBAs Anxiolytics ARQ & SAQ Feedback

LOs: Anti-Convulsants Seizures: recognise the different seizure types Anti-convulsants: recognise that anti-convulsant therapy is determined by the seizure type coupled with pharmacodynamics/pharmacokinetic properties of specific anti-convulsant drugs

What is a seizure? “sudden changes in behaviour caused by electrical hypersynchronization of neuronal networks in the cerebral cortex” Massive Jolt in Brain Activity caused by neurons being activated altogether Diagnosis: o EEG o MRI

Seizure Types - Definitions Seizure types & Symptoms 1. Tonic-clonic seizures: loss of 2. 3. 4. 5. consciousness muscle stiffening jerking/twitching deep sleep wakes up Absence seizures: brief staring episodes with behavioural arrest Tonic/atonic seizures: sudden muscle stiffening/sudden loss of muscle control Myoclonic seizures: sudden, brief muscle contractions Status epilepticus: > 5 min of continuous seizure activity
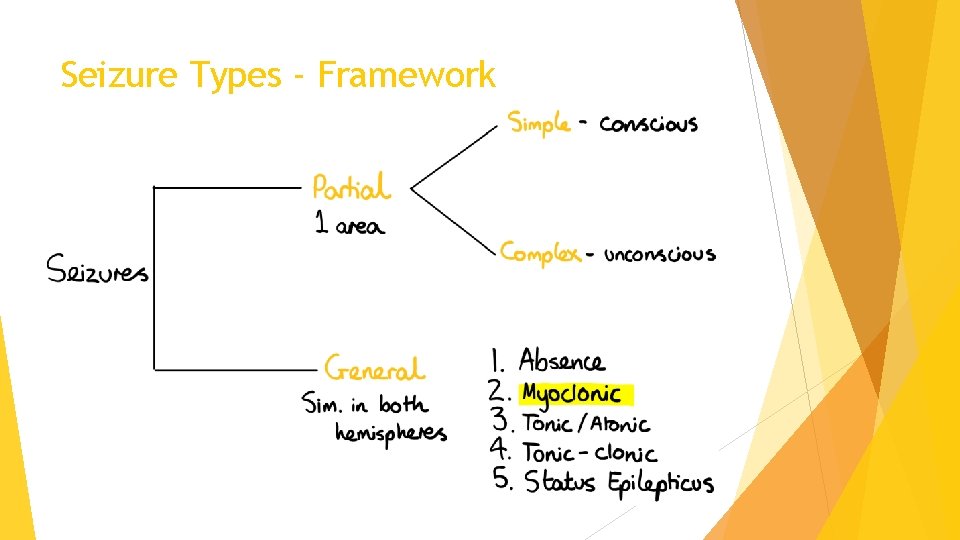
Seizure Types - Framework

Neuron Types Glutaminergic GABAergic
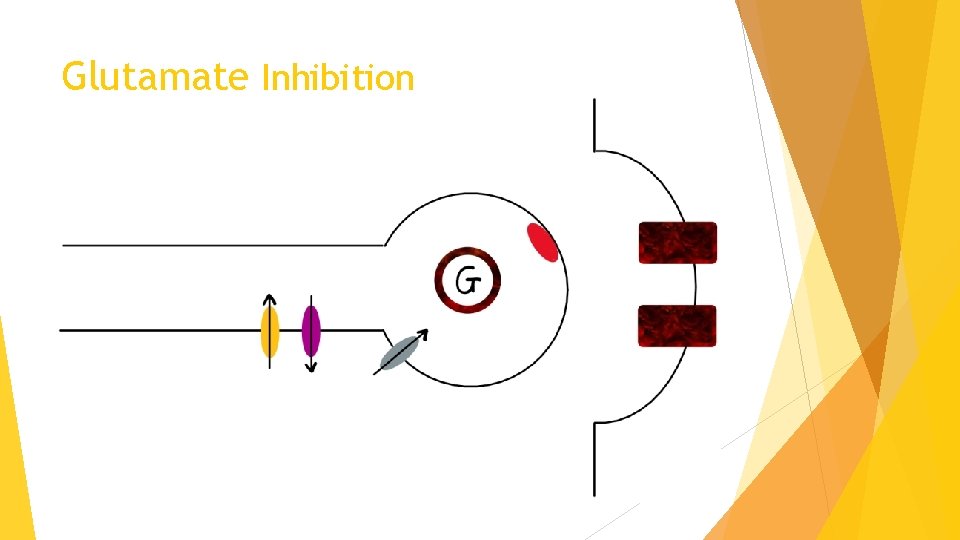
Glutamate Inhibition
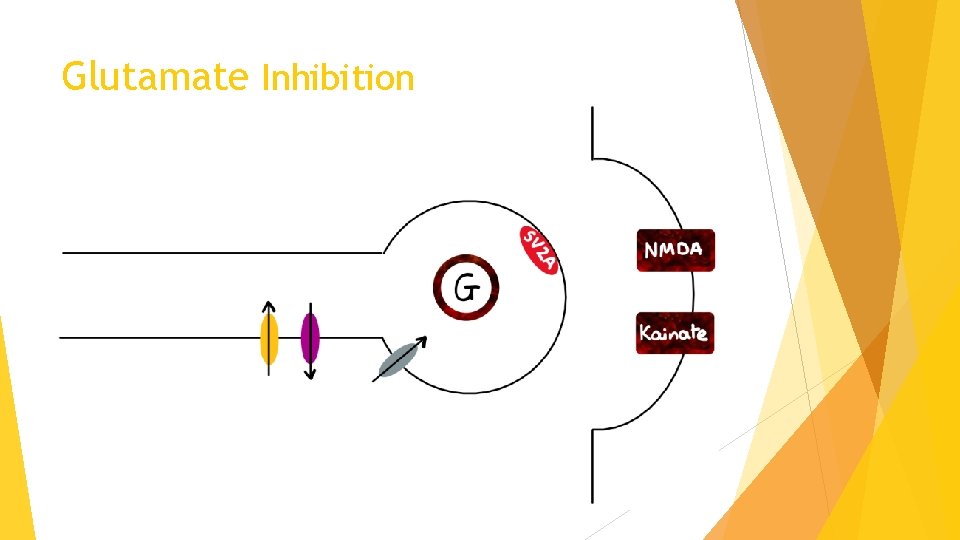
Glutamate Inhibition

Pharmacology – Na Channel Blockers Carbamazepine Pharmacodynamics • Stabilises inactive state of Na+ channel reducing neuronal activity Pharmacokinetics • Enzyme inducer • Onset of activity within 1 hour • 16 -30 hour half-life Indications • Tonic-clonic seizures; partial seizures NB: potential severe side-effects (SJS & TEN) in individuals with HLA-B*1502 allele Lamotrigine Pharmacodynamics • Inactivates Na+ channels reducing glutamate neuronal activity Pharmacokinetics • Onset of activity within 1 hour • 24 -34 hour half-life Indications • Tonic-clonic seizures; absence seizures

Pharmacology – Na Channel Blockers Carbamazepine • Stabilises inactive state • Inducer • Give w/in 1 hour Indications • Tonic-clonic seizures; partial seizures NB: potential severe side-effects (SJS & TEN) in individuals with HLAB*1502 allele Lamotrigine • Inactivates Na+ channels • Give w/in 1 hour Indications • Tonic-clonic seizures; absence seizures

Pharmacology – VG-CCB Ethosuximide • T-type Ca 2+ channel antagonist reduces activity in relay thalamic neurones Pharmacokinetics • Long half-life (50 hours) Indications • Absence seizures

Pharmacology – VG-CCB Ethosuximide • T-type Ca 2+ channel antagonist (Relay Thalamic Ns) Indications • Absence seizures

Pharmacology – Glutamate Exocytosis & Receptors Levetiracetam Pharmacodynamics • Binds to synaptic vesicle associated protein (SV 2 A) preventing glutamate release Pharmacokinetics • Fast-onset (1 hour); half-life (10 hours) Indications • Myoclonic seizures Topiramate Pharmacodynamics • Inhibits NMDA & kainate receptors • Also affects VGSCs & GABA receptors Pharmacokinetics • Fast-onset (1 hour); long half-life (20 hours) Indications • Myoclonic seizures

Pharmacology – Glutamate Exocytosis & Receptors Levetiracetam • Binds SV 2 A • W/in 1 hr Indications • Myoclonic seizures Topiramate • Inhibits NMDA & kainate receptors • W/in 1 hr Indications • Myoclonic seizures
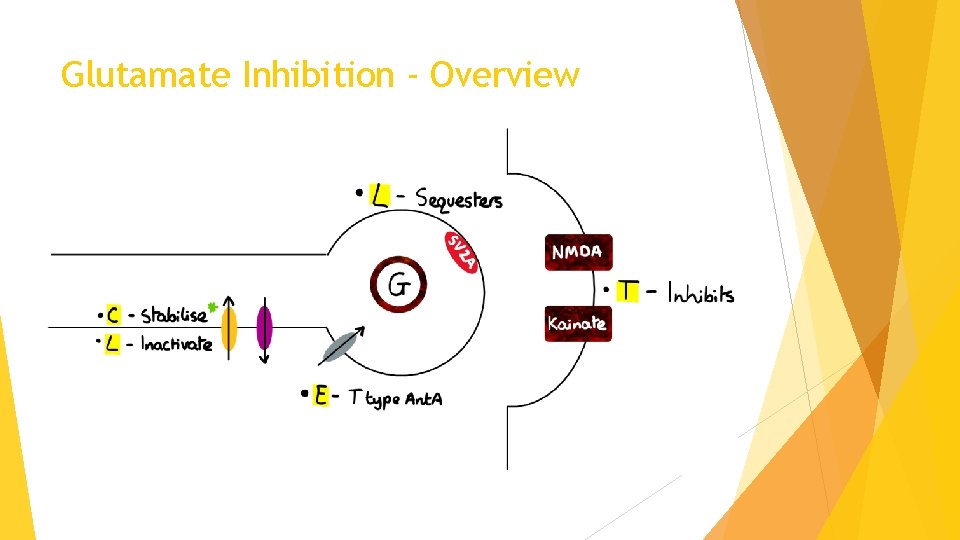
Glutamate Inhibition - Overview
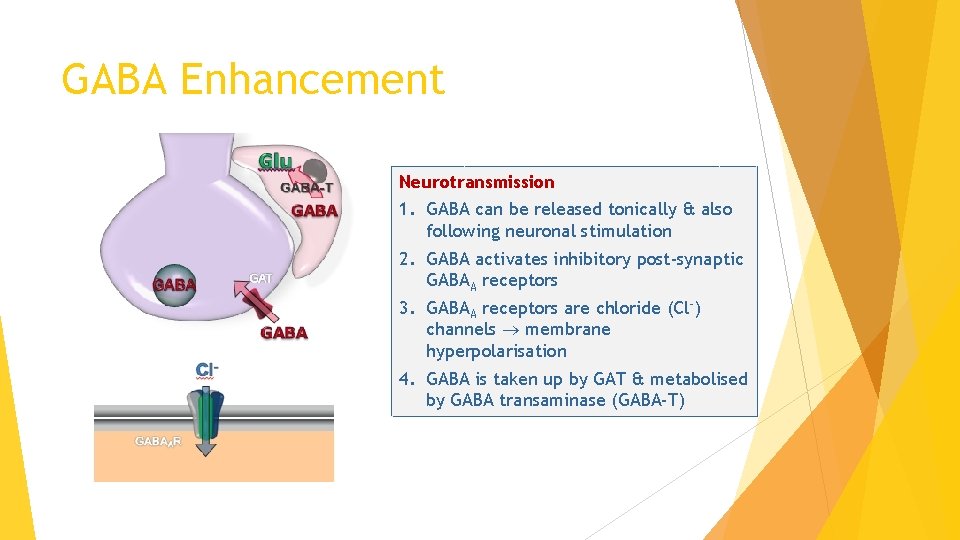
GABA Enhancement Neurotransmission 1. GABA can be released tonically & also following neuronal stimulation 2. GABA activates inhibitory post-synaptic GABAA receptors 3. GABAA receptors are chloride (Cl-) channels membrane hyperpolarisation 4. GABA is taken up by GAT & metabolised by GABA transaminase (GABA-T)
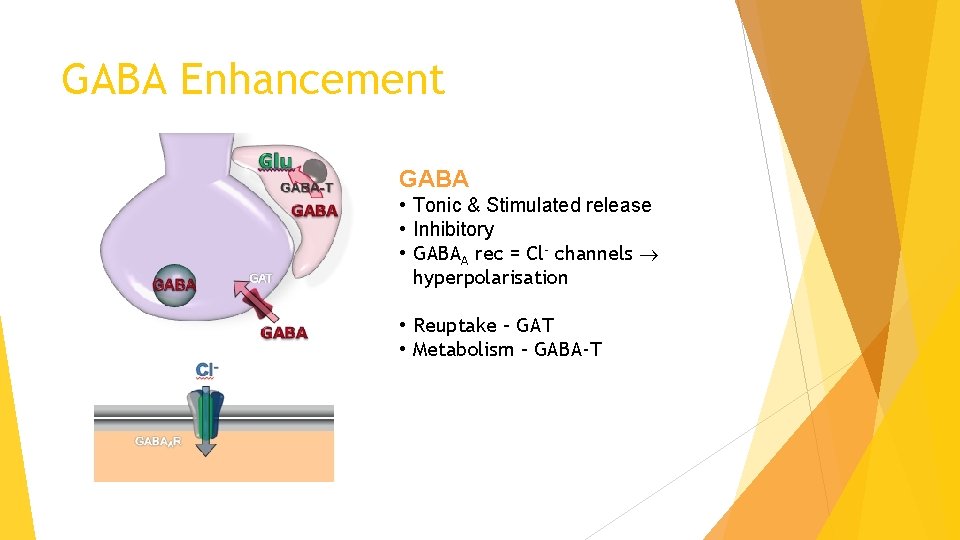
GABA Enhancement GABA • Tonic & Stimulated release • Inhibitory • GABAA rec = Cl- channels hyperpolarisation • Reuptake – GAT • Metabolism – GABA-T

Pharmacology – GABA Diazepam Pharmacodynamics • GABA receptor, PAM increases GABA-mediated inhibition Pharmacokinetics • Rectal gel - Fast-onset (within 15 min); half-life (2 hours) Indications • Status epilepticus Sodium Valproate Pharmacodynamics • Inhibits GABA transaminase increases GABA-mediated inhibition Pharmacokinetics • Fast onset (1 h); half-life (12 h) Indications • Indicated for ALL forms of epilepsy

Pharmacology – GABA Diazepam • GABA- PAM (positive allosteric modulator) enhances GABA effect • Rectal gel - 15 min onset Indications • Status epilepticus Sodium Valproate • Inhibits GABA-T • Fast onset (1 h) Indications • Indicated for ALL forms of epilepsy
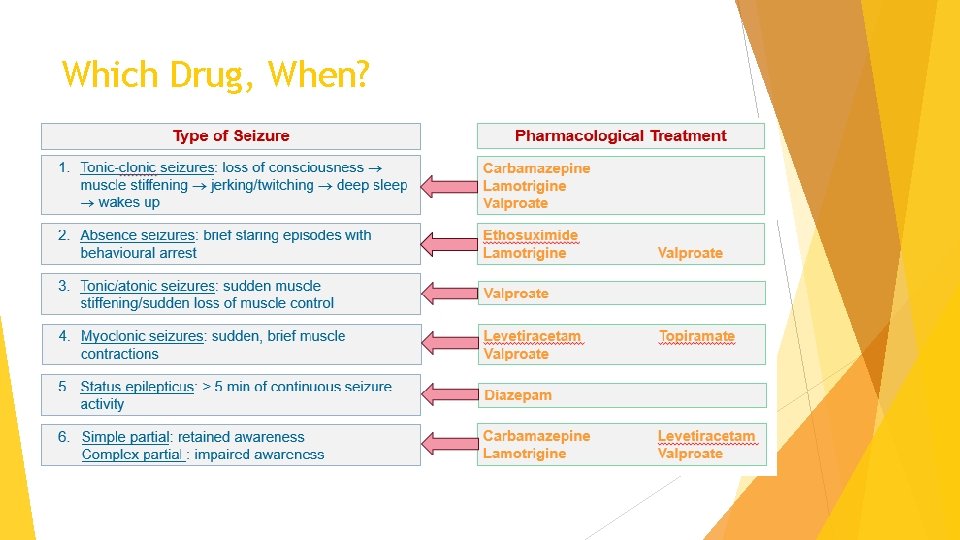
Which Drug, When?
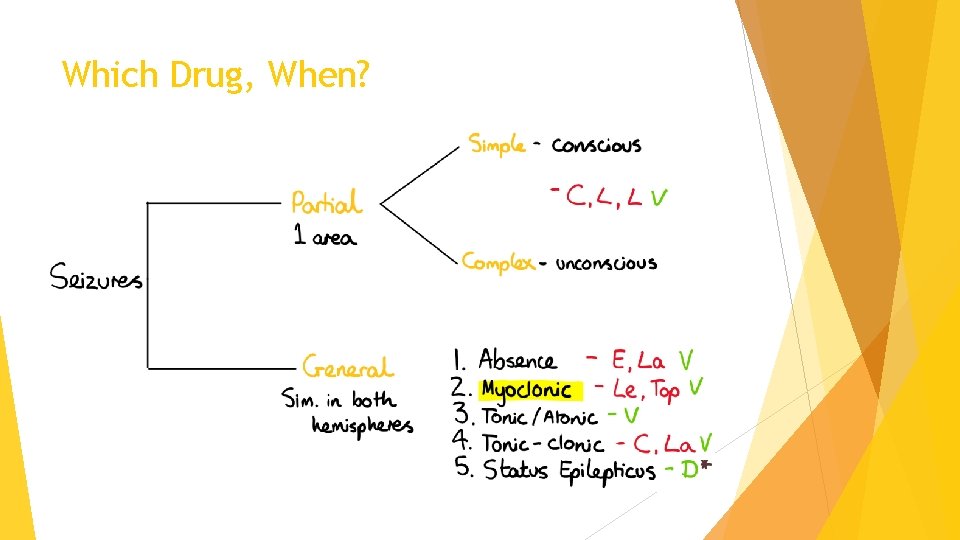
Which Drug, When?
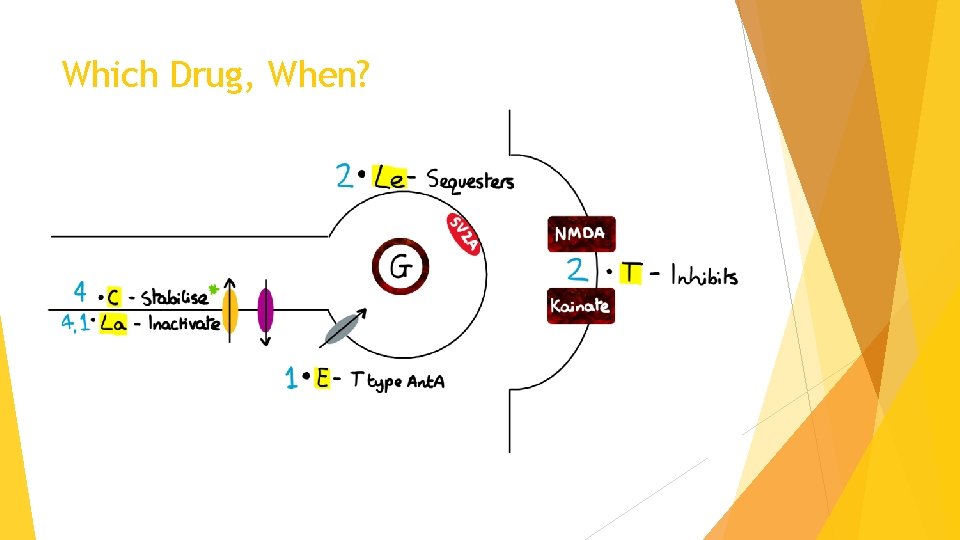
Which Drug, When?

SBA 1 A patient complains about their body going ‘tight and then loose’ and this lasts for a couple of minutes but they remain conscious. What type of seizure is this person having? a) Tonic-Clonic b) Complex Partial c) Myoclonic d) Tonic-Atonic e) Status Epilleticus

SBA 1 A patient complains about their body going ‘tight and then loose’ and this lasts for a couple of minutes but they remain conscious. What type of seizure is this person having? a) Tonic-Clonic b) Complex Partial c) Myoclonic d) Tonic-Atonic e) Status Epilleticus

SBA 2 A patient seen in A&E is suffering a seizure- including fitting and jerking lasting 10 minutes Which medication is most appropriate a) Topiramate b) Ethosuximide c) Valproate d) Carbamazepine e) Diazepam [Test yourself by trying to remember what types of seizures the other drugs are used to treat]

SBA 2 A patient seen in A&E is suffering a seizure- including fitting and jerking lasting 10 minutes Which medication is most appropriate a) Topiramate b) Ethosuximide c) Valproate d) Carbamazepine e) Diazepam [Test yourself by trying to remember what types of seizures the other drugs are used to treat]

Anxiolytics - LOs GABA: identify the processes (e. g. receptors, transporters & enzymes) involved in GABAergic central neurotransmission Drugs targeting GABA: list the principal clinical uses and adverse effects of drugs acting on the GABAergic system and explain how pharmacokinetic differences determine clinical use

What is the difference between anxiolytics & sedatives/hypnotics? Anxiolytic = Anxiety ( mental/physical activity) Sedatives = mental/physical activity ( Hypnotics = Induce Sleep zzz. ZZZZ consciousness)

Anxiolytics vs Sedatives & Hypnotics Anxiolytics are LONG-acting diluted action, lasting the whole day Diazepam, Oxazepam (1/2 life- 8 h) Sedative & Hypnotics are SHORT-acting concentrated action, quick onset Oxazepam, Temazepam (1/2 life- 28 h) BOTH enhance GABA transmission, which reduces excitation Calmness

GABA Most important INHIB. NT in the brain Short Interneurons + some longer (nigrostriatal tract) Pre-/Post-synaptic Functions: Motor, Extrapyramidal, Emotional, Endocrine

GABA agonists should… HAVE WIDE MARGIN OF SAFETY NOT DEPRESS RESPIRATION PRODUCE NATURAL SLEEP (HYPNOTICS) NOT INTERACT WITH OTHER DRUGS NOT PRODUCE ‘HANGOVERS’ NOT PRODUCE DEPENDENCE

GABA agonists should… 1. Safety/ Pre-Effect: Wide margin, not interact with other drugs 2. Effect: Not depress Respiration & should produce Natural Sleep (hypnotics) 3. Post-Effect: Hangovers, Dependence
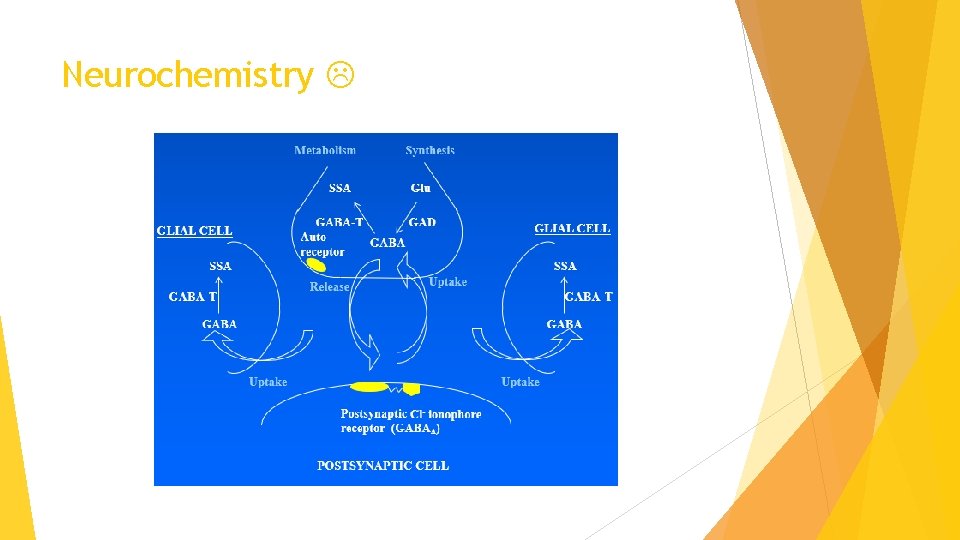
Neurochemistry GABA-T POSTSYNAPTIC CELL

GABA Storage & Release: Stored at GABAergic vesicles (AP Exocytosis) Inactivation: Rapid Re-uptake at Pre-synaptic Membranes & Glial Cells (via GAT) Reuptake is dependent on Na+/ATP therefore saturable Metabolism:

GABA receptors! GABA-A Type 1 (Pentameric Ionotropic) Cl- influx Hyper-polarised Inhibitory Post Synaptic Potential (IPSP) Agonist – GABA, Muscimol Antagonist- Bicuculline GABA-B Type 2 (Gi) Decrease c. AMP Decreased Ca 2+ conductance decreased exocytosis Agonist – Baclofen Antagonist - Saclofen
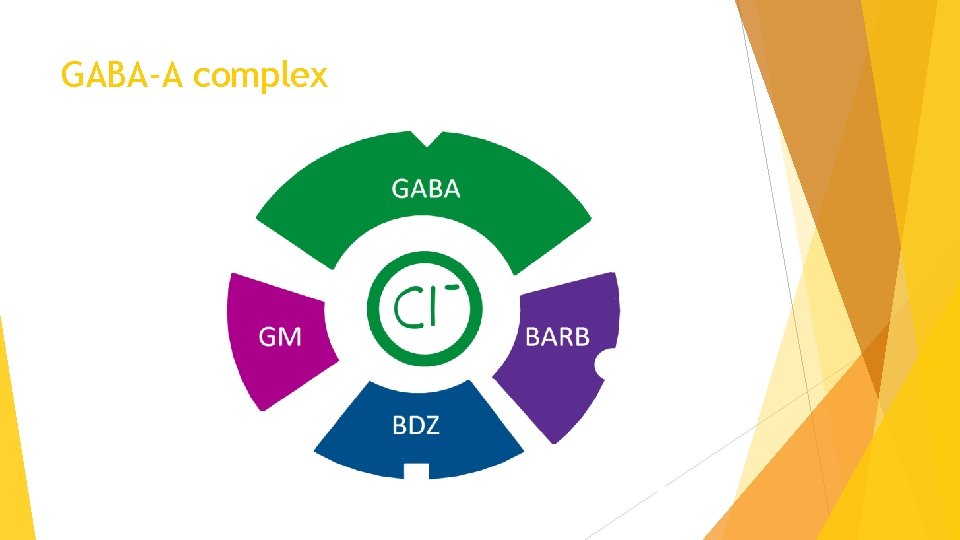
GABA-A complex
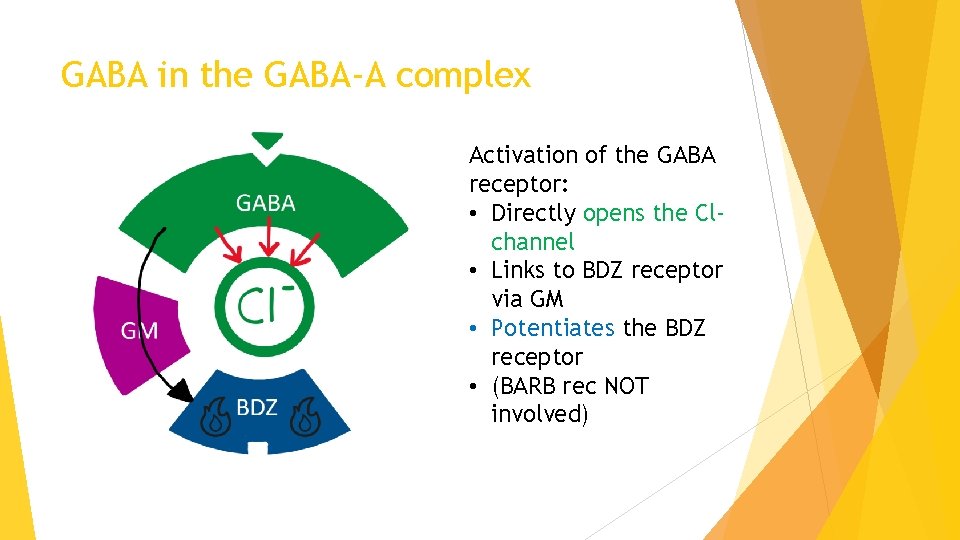
GABA in the GABA-A complex Activation of the GABA receptor: • Directly opens the Clchannel • Links to BDZ receptor via GM • Potentiates the BDZ receptor • (BARB rec NOT involved)
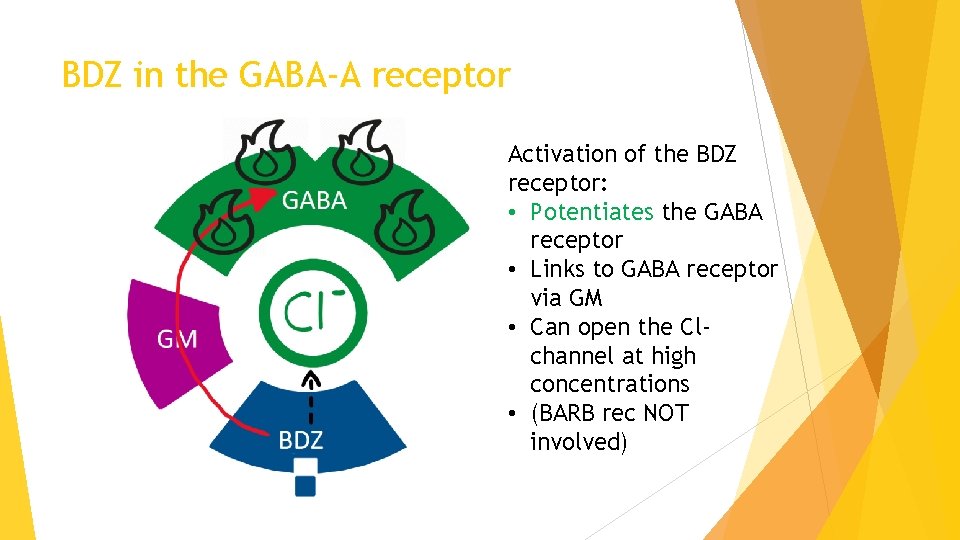
BDZ in the GABA-A receptor Activation of the BDZ receptor: • Potentiates the GABA receptor • Links to GABA receptor via GM • Can open the Clchannel at high concentrations • (BARB rec NOT involved)
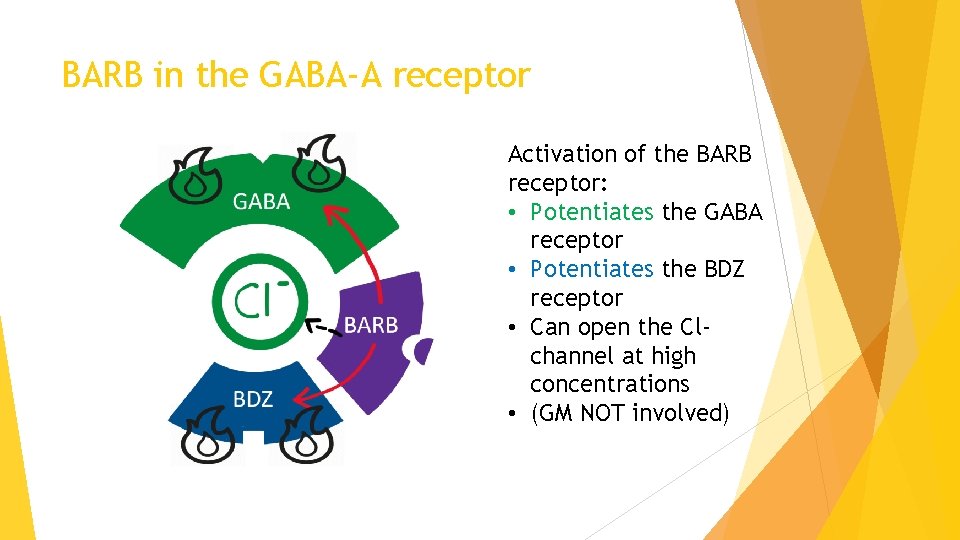
BARB in the GABA-A receptor Activation of the BARB receptor: • Potentiates the GABA receptor • Potentiates the BDZ receptor • Can open the Clchannel at high concentrations • (GM NOT involved)

Benzodiazepines & Barbiturates How do they work? PAMs! (Positive Allosteric Modulators) This means they enhance the normal activity of GABA rather than opening the Chlorine Channel Directly
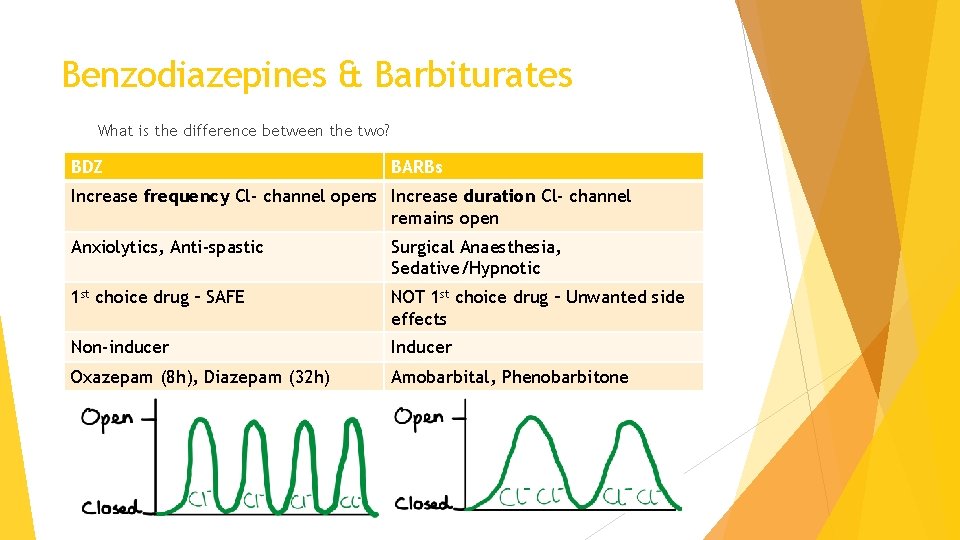
Benzodiazepines & Barbiturates What is the difference between the two? BDZ BARBs Increase frequency Cl- channel opens Increase duration Cl- channel remains open Anxiolytics, Anti-spastic Surgical Anaesthesia, Sedative/Hypnotic 1 st choice drug – SAFE NOT 1 st choice drug – Unwanted side effects Non-inducer Inducer Oxazepam (8 h), Diazepam (32 h) Amobarbital, Phenobarbitone

Other drugs to be aware of… Sedatives/Hynotics: Zopiclone Anxiolytics: SSRIs Anticonvulsants (Valproate, Tiagabine) Antipsychotics (Olanzapine, Quetiapine) Beta-blockers (Propranolol) Buspirone (Serotonin receptor agonist)

ARQ 1 A: BDZs always open the Cl- channel directly R: BDZs enhance the effect of GABA a) TT – assertion explains reason b) TT – assertion does not explain reason c) TF d) FF e) FT

ARQ 1 A: BDZs always open the Cl- channel directly R: BDZs enhance the effect of GABA a) TT – assertion explains reason b) TT – assertion does not explain reason c) TF d) FF e) FT

SAQ 1 List 6 ideal features of GABA agonists for clinical use.

SAQ 1 List 6 ideal features of GABA agonists for clinical use. (Pre-effect) 1. Wide margin of safety 2. Does not interact with other drugs (Effect) 3. Does not depress respiration 4. Induces normal sleep (Post-Effect) 5. No hangover 6. No dependence

FEEDBACK (please) bit. ly/muslimmedics
- Slides: 48