Anticoagulation in Intracerebral Hemorrhage ICH Survivors for Stroke

Anticoagulation in Intracerebral Hemorrhage (ICH) Survivors for Stroke Prevent. Ion and REcovery Webinar Jan 27, 2021 NINDS U 01 NS 106513 NCT 03907046 27 -Jan-2021 ASPIRE Webinar 0

Outline • • 27 -Jan-2021 Screening and Enrollment Activity Protocol Amendment Submitted to c. IRB Atrial Fibrillation Field Guide Sites Network Update ASPIRE Webinar 1
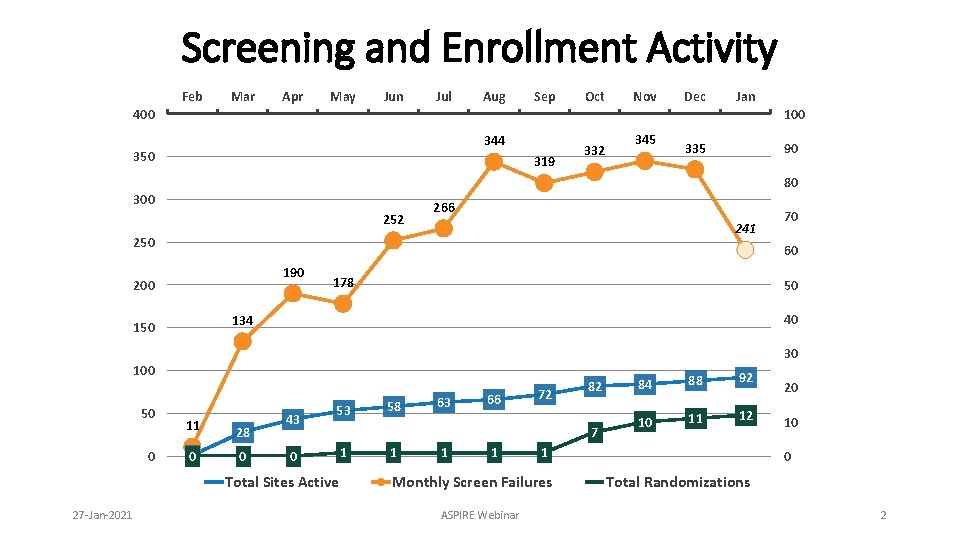
Screening and Enrollment Activity Feb Mar Apr May Jun Jul Aug Sep Oct Nov Dec Jan 400 100 344 350 319 332 345 335 90 80 300 252 266 241 250 70 60 190 200 178 50 40 134 150 30 100 50 0 11 28 1 0 0 43 53 0 Total Sites Active 27 -Jan-2021 58 63 66 72 82 7 1 1 88 92 10 11 12 1 Monthly Screen Failures ASPIRE Webinar 84 20 10 0 Total Randomizations 2
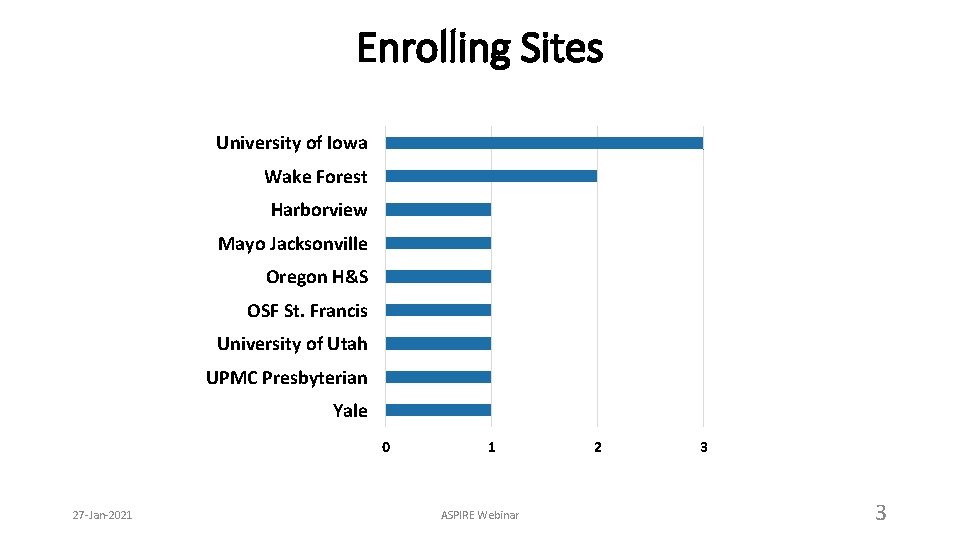
Enrolling Sites University of Iowa Wake Forest Harborview Mayo Jacksonville Oregon H&S OSF St. Francis University of Utah UPMC Presbyterian Yale 0 27 -Jan-2021 1 ASPIRE Webinar 2 3 3

Protocol Amendment Submitted Proposed Change: Removal of exclusion for “Life expectancy <1 year”. Rationale: • This exclusion was intended was to prevent enrollment of patients with very limited life expectancy due to co-morbid conditions (e. g. , advanced cancer). • In practice may be interpreted to exclude patients considered at high risk of death due to the condition under study. • Instead of requiring an arbitrary and potentially inaccurate life expectancy estimate, we have removed this criterion. Patients with fatal ICH events should be excluded as not ‘Able to be randomized within 14 -120 days’. Patients with severe co-existing medical condition, may be excluded as not ‘Able to comply with study procedures and available for duration of study’ or having a ‘Condition that precludes safe participation’. 27 -Jan-2021 ASPIRE Webinar 4

Protocol Amendment Submitted, continued Proposed Change Two assessments (Berlin Sleep Apnea and IQCODE 16 dementia questionnaires) moved from baseline to screening visit. Rationale To reduce the time required to complete the baseline/randomization visit. Procedures to follow if subject expresses wish to withdraw from active participation added. To minimize losses-to follow-up and ensure ascertainment of vital status for all subjects. 27 -Jan-2021 ASPIRE Webinar 5

Atrial Fibrillation/Flutter in the ASPIRE Trial A Field Guide

What counts as AF in terms of ASPIRE eligibility? Protocol: “Non-valvular AF (defined as atrial fibrillation or atrial flutter), documented by electrocardiography or a physician-confirmed history of AF” 27 -Jan-2021 ASPIRE Webinar 7

What counts as AF in terms of ASPIRE eligibility? Protocol: “Non-valvular AF (defined as atrial fibrillation or atrial flutter), documented by electrocardiography or a physician-confirmed history of AF” Questions covered in this guide: 1. What counts as non-valvular? 2. What counts as atrial fibrillation or atrial flutter? 3. What counts as electrocardiography? 4. What counts as physician-confirmed history? 27 -Jan-2021 ASPIRE Webinar 8

Definition of non-valvular Valvular = mechanical heart valve (any position) OR moderate-to-severe mitral stenosis reported on echocardiogram Do Not Enroll Non-valvular = any case NOT meeting valvular definition OK To Enroll 27 -Jan-2021 ASPIRE Webinar 9

Definitions of atrial fibrillation & atrial flutter Atrial fibrillation and atrial flutter are terms that describe both: 1. Clinical disorders AND 2. Findings on electrocardiography (ECG) A patient can have atrial fibrillation/flutter, the disorder An ECG tracing can show atrial fibrillation/flutter, the arrhythmia Either is good enough for ASPIRE! 27 -Jan-2021 ASPIRE Webinar 10

Definition of electrocardiography Electrocardiography (ECG), broadly defined, includes: • • Standard 12 -lead ECG Hospital telemetry Holter monitoring of varying duration External loop recorders Implantable loop recorders Consumer devices (i. Watch, Alive. Cor, etc) Others yet to be invented A finding of atrial fibrillation or atrial flutter on any ECG test must be noted on official ECG report by interpreting physician 27 -Jan-2021 ASPIRE Webinar 11

Definition of physician-confirmed history Defined as at least 2 of the following: 1. Patient was on anticoagulant before ICH admission 2. Medical record notes patient has atrial fibrillation/flutter 3. Patient’s primary care physician or cardiologist confirms patient has atrial fibrillation/flutter 27 -Jan-2021 ASPIRE Webinar 12

Additional Key Point #1 Patients can qualify even if not on anticoagulant before ICH • Anticoagulants may have been withheld before ICH for non-evidence based reasons—if patient/surrogate & treating physicians now agree with equipoise OK to randomize • Risk of ischemic stroke is greater than risk of recurrent ICH in ASPIRE target population 27 -Jan-2021 ASPIRE Webinar 13

Additional Key Point #2 Patients can qualify even with new AF diagnosis post ICH • Initial AF diagnosis can be from before or after the index ICH • Newly diagnosed AF is not uncommon after ICH, so please review post-ICH records for a new AF diagnosis 27 -Jan-2021 ASPIRE Webinar 14

Additional Key Point #3 Automated AF detection software should be manually checked • AF detection software programs on hospital telemetry, 30 -day Holters, i. Watch, etc are sensitive but prone to false positives • Potential AF cases flagged by software programs must be reviewed and confirmed by a cardiologist or other qualified clinician 27 -Jan-2021 ASPIRE Webinar 15

High-yield ways to screen for AF 1. Ask patient/surrogate about "irregular heartbeat", "irregular heart rhythm", "heart rhythm problems", "arrhythmia" 2. Free text search in EMR for "atrial" and "afib" 3. Review medication list for: • common antiarrhythmic drugs: amiodarone, dronedarone, flecainide • common anticoagulant drugs: warfarin, apixaban, rivaroxaban, dabigatran • if present, dig deeper: contact PCP, cardiologist, other relevant specialists 4. Review reports of all ECGs and echocardiograms for mention of AF (make sure an ECG is performed — this is standard of care) 5. Review telemetry reports and speak to treating team, especially bedside nurses, about any potential runs of AF on telemetry 6. Repeat AF screening shortly before hospital discharge and again shortly before end of 120 -day randomization window 27 -Jan-2021 ASPIRE Webinar 16
AF: the more you look, the more you find 27 -Jan-2021 ASPIRE Webinar 17

Site Network Update 27 -Jan-2021 ASPIRE Webinar 18
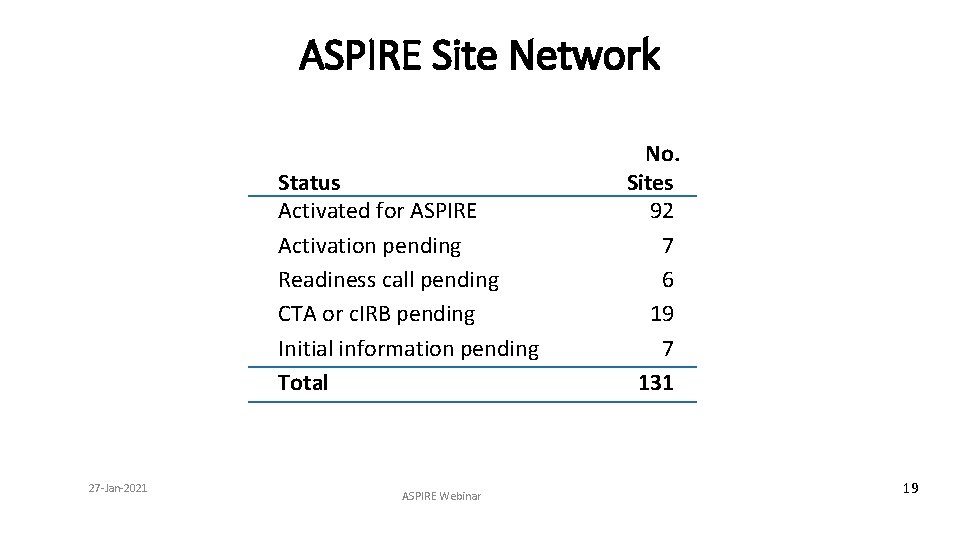

ASPIRE Site Network Status Activated for ASPIRE Activation pending Readiness call pending CTA or c. IRB pending Initial information pending Total 27 -Jan-2021 ASPIRE Webinar No. Sites 92 7 6 19 7 131 19

Sites in Progress Suspended due to COVID Pending Activation UAMS 27 -Jan-2021 Readiness Call Needed Banner University Boston Medical Center Froedtert Hospital Houston Methodist Hospital Kaiser Permanente Sacramento Javon Bea Hospital - Riverside Kings County Hospital Center NYP Columbia University Lahey Hospital & Medical Center University Medical Center of El Paso St. Cloud Hospital University of Nebraska The Queen's Medical Center ASPIRE Webinar 20
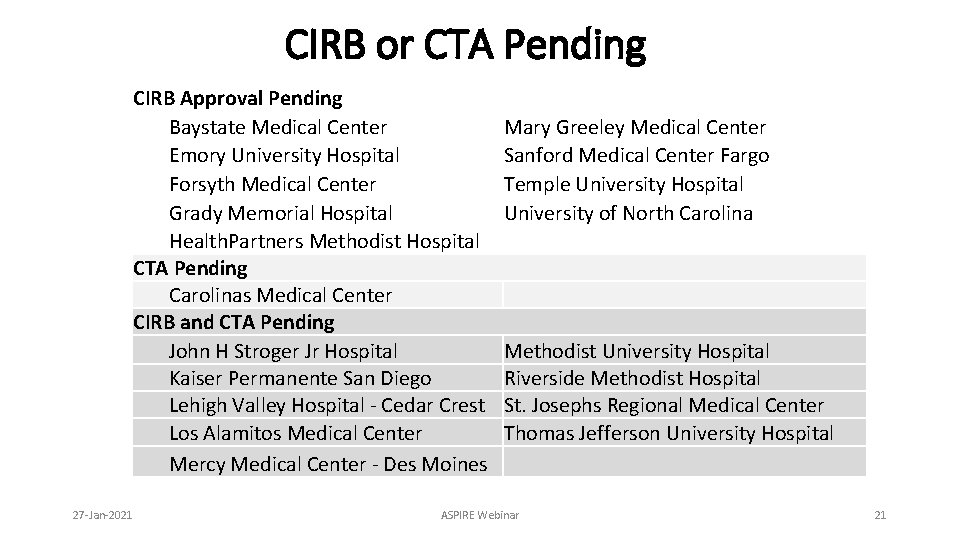

CIRB or CTA Pending CIRB Approval Pending Baystate Medical Center Emory University Hospital Forsyth Medical Center Grady Memorial Hospital Health. Partners Methodist Hospital CTA Pending Carolinas Medical Center CIRB and CTA Pending John H Stroger Jr Hospital Kaiser Permanente San Diego Lehigh Valley Hospital - Cedar Crest Los Alamitos Medical Center Mercy Medical Center - Des Moines 27 -Jan-2021 Mary Greeley Medical Center Sanford Medical Center Fargo Temple University Hospital University of North Carolina Methodist University Hospital Riverside Methodist Hospital St. Josephs Regional Medical Center Thomas Jefferson University Hospital ASPIRE Webinar 21

Initial Site Information Pending CHI Health Creighton University Medical Center - Bergan Mercy Desert Regional Medical Center El Camino Hospital - Mountain View Campus Lenox Hill Hospital Nuvance Health Danbury Hospital Nuvance Health Vassar Brothers Medical Center UC Davis Medical Center 27 -Jan-2021 ASPIRE Webinar 22

Thank You 27 -Jan-2021 ASPIRE Webinar 23
- Slides: 24