Antibiotics and Antibiotic Resistance Antibiotics and Antibiotic Resistance

Antibiotics and Antibiotic Resistance

Antibiotics and Antibiotic Resistance Copy these learning objectives into your workbooks: Learning objectives: • Understand how antibiotics can be used to treat disease in an appropriate and safe way • Be able to explain the problems associated with the overuse and misuse of antibiotics Starter: Have you taken antibiotics before? Why? What are antibiotics used for?

Antibiotics are powerful medicines that fight bacterial infection Literal translation • anti – against • biotic – living things

Discovery in 1928 Penicillium colony Alexander Fleming – He was an extremely messy scientist – Came back from holiday to see a mould growing on his Staphylococcus agar plates Bacteria – Noticed that the Staphylococcus couldn’t grow anywhere near the mould – The mould prevented bacterial growth! (Staphylococcus can cause minor skin infections, to more serious infections of the blood, lungs, heart and even causes MRSA. ) Bacteria inhibited

How antibiotics work Antibiotics can be either • Broad Spectrum – Kill a wide range of bacteria e. g. Penicillin • Narrow Spectrum – Kill a specific type or group of bacteria e. g. Isoniazid Antibiotics work in one of two ways • Bactericidal – Kills the bacteria • Bacteriostatic – Prevents the bacteria from dividing
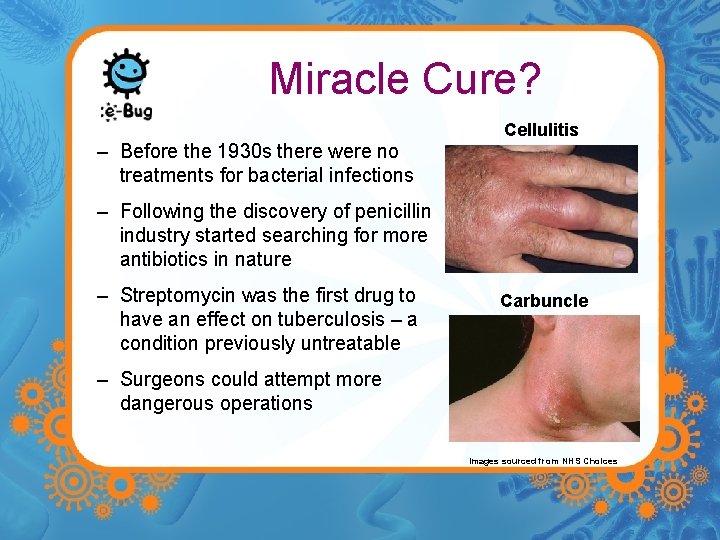
Miracle Cure? – Before the 1930 s there were no treatments for bacterial infections Cellulitis – Following the discovery of penicillin industry started searching for more antibiotics in nature – Streptomycin was the first drug to have an effect on tuberculosis – a condition previously untreatable Carbuncle – Surgeons could attempt more dangerous operations Images sourced from NHS Choices

The antibiotic timeline Images sourced from Public Health England
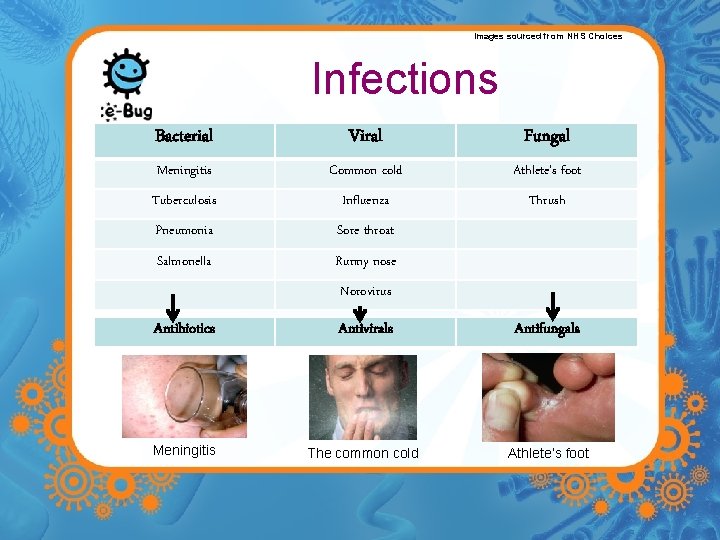
Images sourced from NHS Choices Infections Bacterial Viral Fungal Meningitis Common cold Athlete’s foot Tuberculosis Influenza Thrush Pneumonia Sore throat Salmonella Runny nose Norovirus Antibiotics Antivirals Antifungals Meningitis The common cold Athlete’s foot
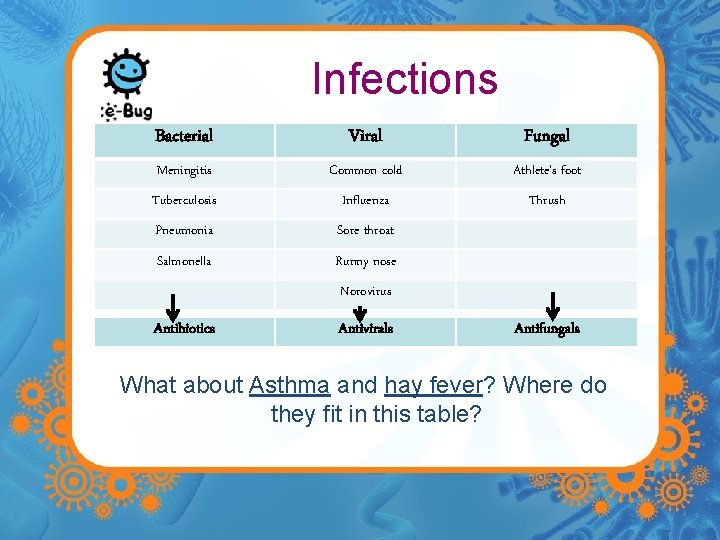
Infections Bacterial Viral Fungal Meningitis Common cold Athlete’s foot Tuberculosis Influenza Thrush Pneumonia Sore throat Salmonella Runny nose Norovirus Antibiotics Antivirals Antifungals What about Asthma and hay fever? Where do they fit in this table?

Miracle Cure? Overuse of antibiotics can damage our normal/good bacteria. – Many antibiotics prescribed by the doctor are broad spectrum – These kill the body’s good bacteria as well as the bad – With the good bacteria gone there is more room for bad microbes to invade!

Miracle Cure? Antibiotics resistance – Bacteria are very good at adapting to their environment – Many bacteria have developed the ability to become resistant to antibiotics. – These bacteria are now a major threat in our hospitals. – Antibiotic resistant bacteria include Methicillin Resistant Staphylococcus aureus (MRSA)
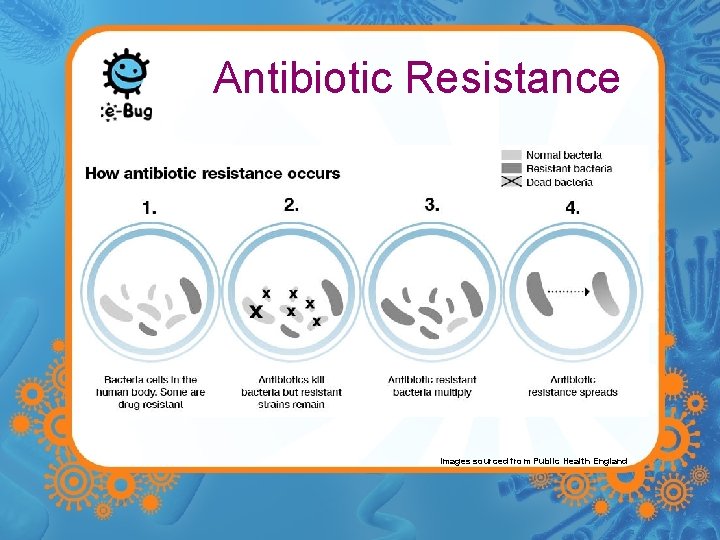
Antibiotic Resistance Images sourced from Public Health England

Antibiotic Resistance The Causes of antibiotic resistance are: – Overuse • Antibiotics used to treat self-limiting infections i. e. for colds, flu, sore throat etc. • Antibiotics used in farming and veterinary care – Misuse • Not completing a prescribed course • Using antibiotics not prescribed for you

Task 1: can antibiotics do that? 1. Cut out the table and stick it into your exercise book 2. Cut out the statements and sort (then stick) them into each column

Antibiotics can’t 1. Kill bacteria 2. Treat only symptoms 4. Stop bacteria growing 3. Help colds get better more quickly 6. Help Pneumonia get better more quickly 5. Kill viruses 8. Kills many of our good bacteria in the body 13. Help patients who have bacterial infections after operations get better quicker 14. Encourage our good bacteria to become resistant to antibiotics 7. Help hay fever get better more quickly 9. Help coughs get better more quickly 10. Help sore throats get better more quickly 11. Help ear ache get better more quickly 12. Help asthma get better more quickly

Task 2: can you avoid antibiotic resistance? Aim of the game: To keep as many ‘normal bacteria’ as possible. How to play: 1. Start with 4 ‘normal bacteria’ cards. Place the rest in a deck on the desk. 2. Place the ‘resistant bacteria’ in a deck on the desk. Place the action cards in a deck (face downwards) on the desk. 3. Player 1 picks up an action card. Read the instructions aloud and follow the instructions. If you do not have the cards you need to follow the instructions return the action card. 4. Return cards to relevant decks (return action cards to the bottom) How does it end? : The game ends when someone has a full hand of ‘resistant bacteria’. How do I win? : The winner is the person with the fewest ‘resistant bacteria’.

How can antibiotic resistance be prevented? 1. 2. Individually or in groups, think of ways that antibiotic resistance could be prevented. You could use a spider diagram to show your ideas Hint: Think about the information from the card game

How antibiotic resistance can be prevented – Antibiotics should be the last line of defence NOT the first • Most common infections will get better by themselves through time, bed rest, liquid intake and healthy living. – Only take antibiotics prescribed by a doctor – If prescribed antibiotics, finish the course. – Do not use other peoples or leftover antibiotics • Different antibiotics work on different bacterial infections – Wash your hands with warm soapy water to prevent the spread of infection

Anagram Activity Can you work out these anagrams of bacterial infections? 1. pnoinmeua 2. ginnemitis 3. butlerosisuc 4. malleasnol 1. Pneumonia 2. Meningitis 3. Tuberculosis 4. Salmonella

Antibiotics and Antibiotic Resistance Learning objectives: • Understand how antibiotics can be used to treat disease in an appropriate and safe way • Be able to explain the problems associated with the overuse and misuse of antibiotics
- Slides: 20