Antibiotic Resistance and Medicinal Drug Policy Dr Ken

Antibiotic Resistance and Medicinal Drug Policy Dr. Ken Harvey School of Public Health, La Trobe University, Melbourne, Australia 1

Lecture outline • Why the concern about antibiotic resistance? • The history, microbiological and social determinants of antibiotic resistance • Containing antibiotic resistance: microbiological surveillance, antibiotic utilization studies and other interventions • One country’s response: the quality use of medicines pillar of Australian drug policy • The current challenge – using information technology to further improve antibiotic use 2

Press Release WHO/41 12 June 2000 DRUG RESISTANCE THREATENS TO REVERSE MEDICAL PROGRESS Curable diseases – from sore throats and ear infections to TB and malaria -- are in danger of becoming incurable A new report warns that increasing drug resistance could rob the world of its opportunity to cure illnesses and stop epidemics. 3

The start of antibiotic resistance: Penicillin Fleming 1928 Florey & Chain 1940 4

History of resistance 5
Bacterial evolution vs mankind’s ingenuity • Adult humans contains 1014 cells, only 10% are human – the rest are bacteria • Antibiotic use promotes Darwinian selection of resistant bacterial species • Bacteria have efficient mechanisms of genetic transfer – this spreads resistance • Bacteria double every 20 minutes, humans every 30 years • Development of new antibiotics has slowed – resistant microorganisms are increasing 6

Surveillance of resistance: Australia Data are collected from 29 laboratories around Australia, including public hospital and private laboratories, in both metropolitan and country areas. Australia, like China, is a contributor to the WHO A -R Infobank: http: //oms 2. b 3 e. jussieu. fr/arinfobank/ 7

Resistance: Australia 2000 • Hospitals – vancomycin-resistant enterococci (VRE’s) – multi-resistant Staph. aureus (MRSA) NB. vancomycinresistant strains have been found in Japan and the USA but not yet in Australia • Community – Strep. Pneumoniae (Penicillins 15% I, 2% R; macrolides & tetracyclines 20% R) – Haemophilis influenzae (Penicillins 20% R ; macrolides & tetracyclines 10% R) – E. coli (amoxycillin 45% R ; amoxy-clav 10% R ; trimeth 15%R) 8

Resistance: The World 2000 • In much of South-East Asia, resistance to penicillin has been reported in up to 98% of gonorrhoea strains. • In Estonia, Latvia, and parts of Russia and China, over 10% of tuberculosis (TB) patients have strains resistant to the two most effective anti-TB drugs. • Thailand has completely lost the use three of the most common anti-malaria drugs because of resistance. • A small but growing number of patients are already showing primary resistance to AZT and other new therapies for HIV-infected persons. 9

The consequences of antibiotic resistance • Increased morbidity & mortality – “best-guess” therapy may fail with the patient’s condition deteriorating before susceptibility results are available – no antibiotics left to treat certain infections • Greater health care costs – more investigations – more expensive, toxic antimicrobials required – expensive barrier nursing, isolation, procedures, etc. • Therapy priced out of the reach of some third-world countries 10

Therapy priced out of the reach of the poor • A decade ago in New Delhi, India, typhoid could be cured by three inexpensive drugs. Now, these drugs are largely ineffective in the battle against this life-threatening disease. • Likewise, ten years ago, a shigella dysentery epidemic could easily be controlled with cotrimoxazole – a drug cheaply available in generic form. Today, nearly all shigella are non-responsive to the drug. • The cost of treating one person with multidrug-resistant TB is a hundred times greater than the cost of treating nonresistant cases. New York City needed to spend nearly US$1 billion to control an outbreak of multi-drug resistant TB in the early 1990 s; a cost beyond the reach of most of the world's cities. 11

Social factors fuelling resistance • Poverty encourages the development of resistance through under use of drugs – Patients unable to afford the full course of the medicines – Sub-standard & counterfeit drugs lack potency • In wealthy countries, resistance is emerging for the opposite reason – the overuse of drugs. – Unnecessary demands for drugs by patients are often eagerly met by health services and stimulated by pharmaceutical promotion – Overuse of antimicrobials in food production is also contributing to increased drug resistance. Currently, 50% of all antibiotic production is used in animal husbandry and aquiculture • Globalization, increased travel and trade ensure that resistant strains quickly travel elsewhere. So does excessive promotion. 12

Postponing the end of the antibiotic era • Antibiotic stewardship (prudent use) • Contain the spread of resistant microorganisms and relevant genes (infection control) • Develop new antibiotics that have novel modes of action or circumvent bacterial mechanisms of resistance (research) 13

Antibiotic stewardship: Australia 14

What are Antibiotic Guidelines? • Best practice recommendations concerning the treatment of choice for common clinical problems • Written by national experts • Evidence based where possible, peer-consensus where not • Regularly updated every 2 years • Endorsed by the Australian Medical Association, etc. • Used for medical education, problem look-up and drug audit 15
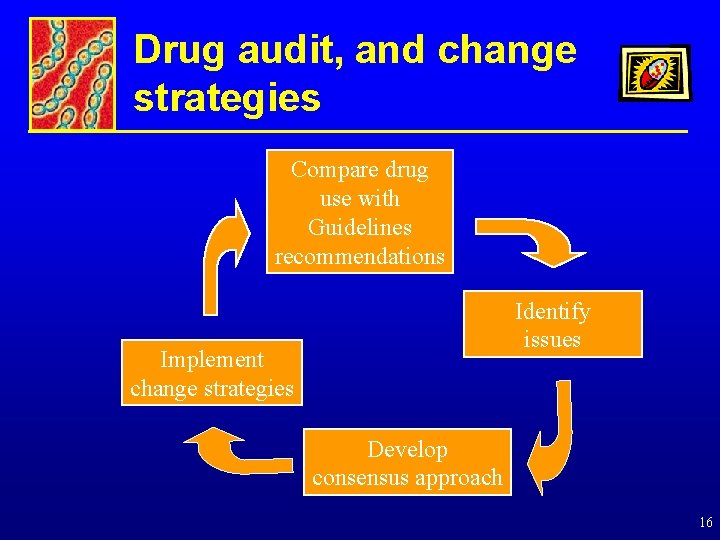
Drug audit, and change strategies Compare drug use with Guidelines recommendations Identify issues Implement change strategies Develop consensus approach 16

First Australian drug audits: 1978 -82 • The 700 bed Royal Melbourne Hospital was surveyed. The 240 bed sample comprised: – 3 general medical units – gastroenterology unit – haematology-oncology unit – 4 general surgical units – orthopaedic unit 17

Inappropriate prescribing • Example of a drug not required: – A patient with suspected infected burns received oral flucloxacillin and penicillin V. Therapy was continued for 23 days despite the failure of 3 separate swabs to produce any growth on culture. Culture of the fourth swab grew methicillin-resistant Staphylococcus aureus. 18

Inappropriate prescribing Example of incorrect administration: Surgical antibiotic prophylaxis accounted for 100 prescriptions and, of these, 23 were given 2 to 12 hours AFTER the operation, a delay that largely nullified their value. Example of inadequate cover: A patient received gentamicin for peritonitis, thereby ignoring the anaerobic flora of the bowel. Metronidazole or clindamycin should have been added 19

Change strategies used • Feedback of audit results to prescribers followed by discussion at grand rounds and unit meetings • Use of Antibiotic Guidelines in undergraduate and postgraduate teaching • Rewriting the next edition of Antibiotic Guidelines, incorporating additional text to clarify misunderstandings and problems observed 20
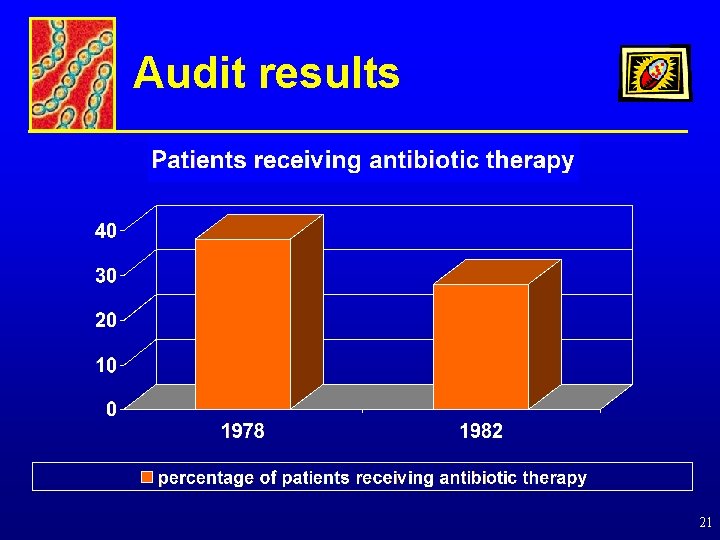
Audit results 21
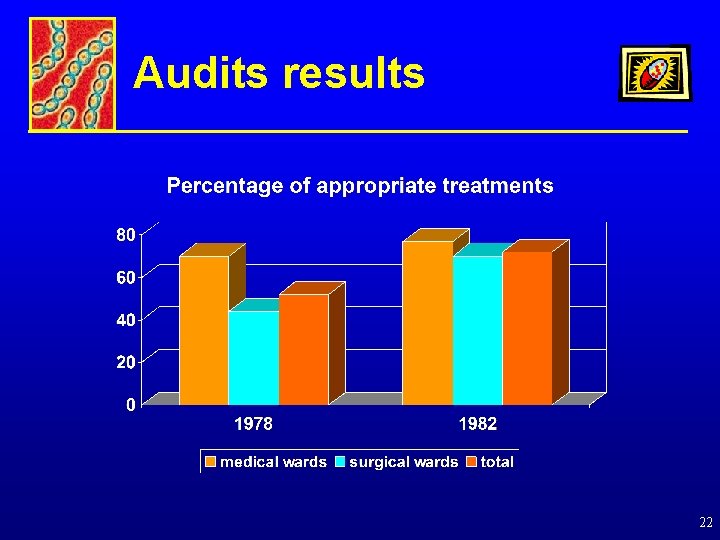
Audits results 22

Initial conclusions • Antibiotic prescribing improved • Surgeons (prophylaxis) were responsible for more inappropriate prescribing than physicians • Some persisting patterns of inappropriate antibiotic use appeared to reflect pharmaceutical company promotion • There was also a need for ongoing campaigns because hospital staff changed 23

Australian therapeutic guidelines: Today 24

Dr. Harvey’s visit to China was sponsored by The World Health Organization and hosted by Professor Yong-Hong Yang Beijing Children’s Hospital & Professor Li Dakui Peking Union Medical College 25
- Slides: 25