Anti Hypertensive Anti Hypertensive Types of HTN 1
















- Slides: 21

Anti Hypertensive

Anti Hypertensive Types of HTN: 1. 2. 3. 4. 5. 6. Alternate HTN. Mild HTN (DBP 91 -104 MMHg). Moderate HTN (DBP 105 -114 MMHg). Severe HTN (DBP > 115 MMHg without End organ damage). Malignant HTN (DBP > 115 MMHg with end organ damage). Systolic HTN (syst BP >160 MMHg)

ANTI HYPERTENSIVE THERAPY Diuretics: - 4 major groups 1. Carbonic anhydrase inhibitors (prox. Tubules) 2. Loop Diuretics Ø Ø Ø Bumetanide (Bumex) Ethacrynic acid (Edecrin) Furosemide (Lasix) Dose 0. 5 – 5 mg 25 – 100 mg 40 – 480 mg

3. Thiazides and Related Sulfonamide Comp. Ø Chlorothiazide (Diuril) 125 – 500 mg Ø Cyclothiazide (Anhydron) 0. 5 – 2 mg Ø Hydrochlorothiazide (Esidrix) 12. 5 – 50 mg Ø Polythiazide (Renese) 1 – 4 mg Ø Methylclothiazide (Enduron) 2. 5 – 5 mg Ø Bendroflumethiazide (Naturetin) 2. 5 – 5 mg Ø Benzthiazide (Aquatag) 12. 5 – 50 mg Ø Triclormethiazide (Metahydrin) 1 – 4 mg

Sulfonamide Compounds Ø Ø Chlorthalidone (Hygroton) Indapamide (Lozol) Metolazone (Zaroxolyn) Quinethazone (Hydromox) 12. 5 -50 mls 2 – 5 mg 1 - 10 mg 25 – 100 mg 4. Potassium – Sparing Agents Ø Ø Ø Spironolactone (Aldactone) Amiloride (Midamor) Triamterene (Dyrenium) 25 – 100 mg 5 – 10 mg 50 – 100 mg

MECHANISMS BY WHICH CHRONIC DIURETIC THERAPY MAY LEAD TO VARIOUS COMPLICATIONS Diuretic therapy Renal reabsorption of Na (and Mg) Hyponatremia Hypomagnesemia Saluresis and dluresis Plasma volume Cardiac output Renal blood flow Postural hypotension PRA GFR Pre-renal azotemia Aldosterone Proximal reabsorption uric acid Hyperuricemia Distal Ca ++ reabsorption calcium Hypercalcemia Kaliuresis Hypokalemia Glucose tolerance Hyper – cholesterolemia

Dosage and Choice of Agent Mild & Moderate HTN: With serum creatinine < 2 mg/d. L • With serum creatinine > 2 mg/d. L •

Side Effects 1. Hypolemia Ø Use small dose of diuretics. Use moderately long acting (12– 18 hours). Restrict Na+ intake. Increase dietary K+ intake. Restrict use of laxative. Combined Thiazide with K+ sparing agent. Ø Ø Ø

Side Effects (cont. ) 2. Hyponatremia 3. Hypomagnesemia 4. Hyperuricemia 5. Hypercholesterolemia 6. Hypercalcemia 7. Hyperglycemia 8. Impotence 9. Use of NSAIDs

Adrenergic Inhibitors: Ø Peripheral Inhibitors: Reserphine v Guanethidine (Ismelin) v Guanadrel (Hylorel) v Bethanidine (Tenathan) v Ø Central Inhibitors: Methyldopa (Aldomet) v Clonidine (Catapres) v

* A- Receptor Blockers: A. a 1 - Receptor Doxazosin ( Cardura) Ø Prazosin (Minipress) B. a 1 and a 2 - Receptors Ø Phentolamine (Regitine) Ø Phenoxybenzamine (Dibenzyline) Ø

* B- Receptor Blockers Ø Acebutolol Ø Atenolol Ø Betaxolol Ø Metoprolol Ø Nadolol Ø Penbutolol Ø Pindolol Ø Propranolol (Sectral) (Ternomin) (Kerlone) (Lopressor) (Corgard) (Levatol) (Visken) (Inderal)

Beta-adrenoceptor blocking drugs Nonselective ISA + ISA Nadolol Pindolol Propranolol Carteolol Timolol Penbutolol Sotalol Alprenolol Tertalolol Oxprenolol Dilevalol selective with alpha-blocking activity ISA + ISA Atenolol Esmolol Metoprolol Bevantolol Bisoprolol Betaxolol Acebutolol (Practolol) Celiprolol Labetalol Bucindolol Carvedilol

VASODILATORS Direct : Ø Ø Ø Ø Hydralazine Minoxidil Nitroproside Diazoxide Nitroglycerin Calcium Blockers Converting Enz. Inh. Alpha Blockers A>V A>v A>V V>A A>V A=V

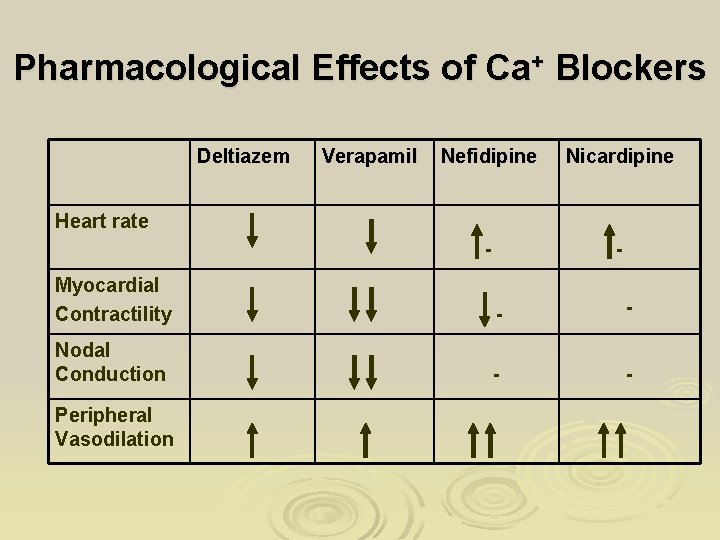
Pharmacological Effects of Ca+ Blockers Deltiazem Verapamil Nefidipine Nicardipine - - Heart rate Myocardial Contractility - - Nodal Conduction - - Peripheral Vasodilation

ACE INHIBITORS v v v v Captopril Enalipril Lisinopril Fosinopril Ramipril Quinapril Benazepril ANGIOTENSION II ANTAGONIST losartan v Olmesartan v

DRUGS COMMONLY USED B-Blockers In-patient with angina pectoris Or Ca + Channel Blockers + Peripheral Vascular Disease ACE Inhibitor Or Ca + Blocker In-patient with DM ++ In patient with hyperlipidemia Diuretics Or ACE Inhibitors In CHF Diuretics Or Ca + Blockers In CRF Diuretics Or Ca + Blockers In Asthma + COPD

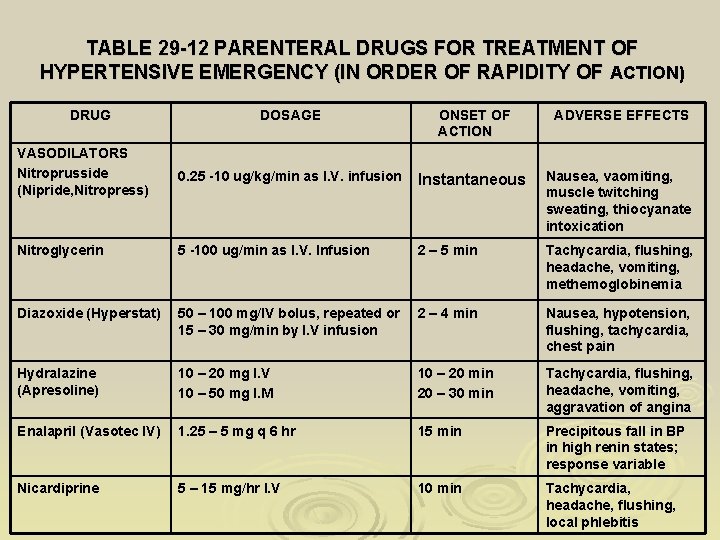
TABLE 29 -12 PARENTERAL DRUGS FOR TREATMENT OF HYPERTENSIVE EMERGENCY (IN ORDER OF RAPIDITY OF ACTION) DRUG DOSAGE ONSET OF ACTION ADVERSE EFFECTS VASODILATORS Nitroprusside (Nipride, Nitropress) 0. 25 -10 ug/kg/min as I. V. infusion Instantaneous Nausea, vaomiting, muscle twitching sweating, thiocyanate intoxication Nitroglycerin 5 -100 ug/min as I. V. Infusion 2 – 5 min Tachycardia, flushing, headache, vomiting, methemoglobinemia Diazoxide (Hyperstat) 50 – 100 mg/IV bolus, repeated or 15 – 30 mg/min by I. V infusion 2 – 4 min Nausea, hypotension, flushing, tachycardia, chest pain Hydralazine (Apresoline) 10 – 20 mg I. V 10 – 50 mg I. M 10 – 20 min 20 – 30 min Tachycardia, flushing, headache, vomiting, aggravation of angina Enalapril (Vasotec IV) 1. 25 – 5 mg q 6 hr 15 min Precipitous fall in BP in high renin states; response variable Nicardiprine 5 – 15 mg/hr I. V 10 min Tachycardia, headache, flushing, local phlebitis

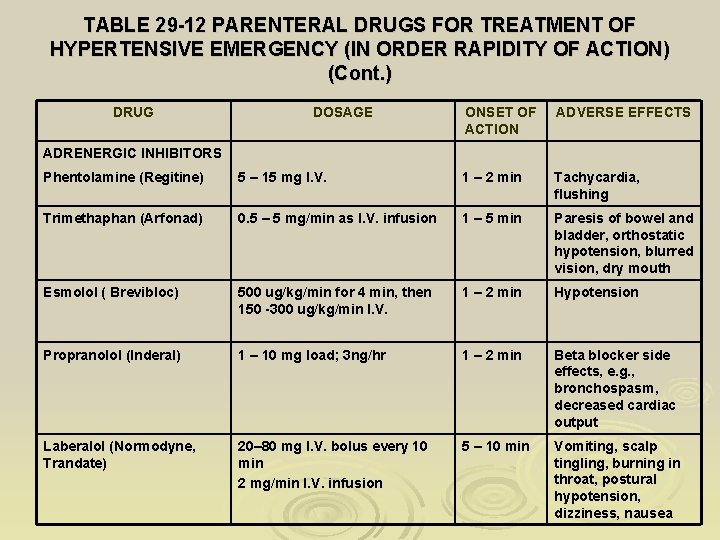
TABLE 29 -12 PARENTERAL DRUGS FOR TREATMENT OF HYPERTENSIVE EMERGENCY (IN ORDER RAPIDITY OF ACTION) (Cont. ) DRUG DOSAGE ONSET OF ACTION ADVERSE EFFECTS ADRENERGIC INHIBITORS Phentolamine (Regitine) 5 – 15 mg I. V. 1 – 2 min Tachycardia, flushing Trimethaphan (Arfonad) 0. 5 – 5 mg/min as I. V. infusion 1 – 5 min Paresis of bowel and bladder, orthostatic hypotension, blurred vision, dry mouth Esmolol ( Brevibloc) 500 ug/kg/min for 4 min, then 150 -300 ug/kg/min I. V. 1 – 2 min Hypotension Propranolol (Inderal) 1 – 10 mg load; 3 ng/hr 1 – 2 min Beta blocker side effects, e. g. , bronchospasm, decreased cardiac output Laberalol (Normodyne, Trandate) 20– 80 mg I. V. bolus every 10 min 2 mg/min I. V. infusion 5 – 10 min Vomiting, scalp tingling, burning in throat, postural hypotension, dizziness, nausea

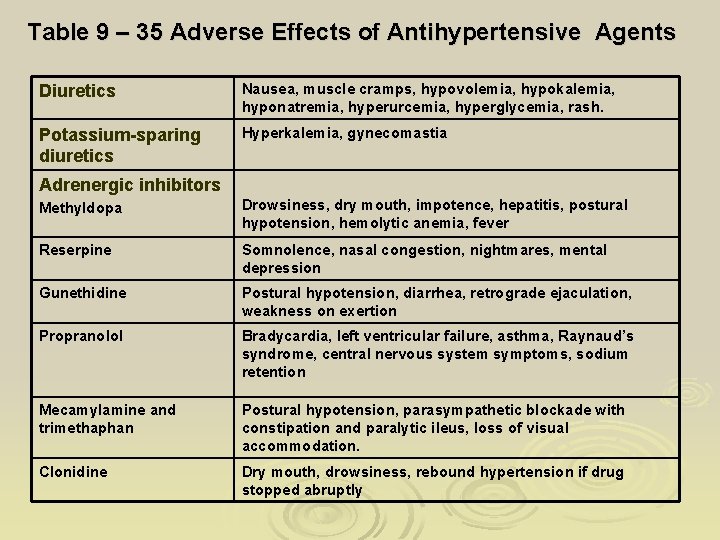
Table 9 – 35 Adverse Effects of Antihypertensive Agents Diuretics Nausea, muscle cramps, hypovolemia, hypokalemia, hyponatremia, hyperurcemia, hyperglycemia, rash. Potassium-sparing diuretics Hyperkalemia, gynecomastia Adrenergic inhibitors Methyldopa Drowsiness, dry mouth, impotence, hepatitis, postural hypotension, hemolytic anemia, fever Reserpine Somnolence, nasal congestion, nightmares, mental depression Gunethidine Postural hypotension, diarrhea, retrograde ejaculation, weakness on exertion Propranolol Bradycardia, left ventricular failure, asthma, Raynaud’s syndrome, central nervous system symptoms, sodium retention Mecamylamine and trimethaphan Postural hypotension, parasympathetic blockade with constipation and paralytic ileus, loss of visual accommodation. Clonidine Dry mouth, drowsiness, rebound hypertension if drug stopped abruptly

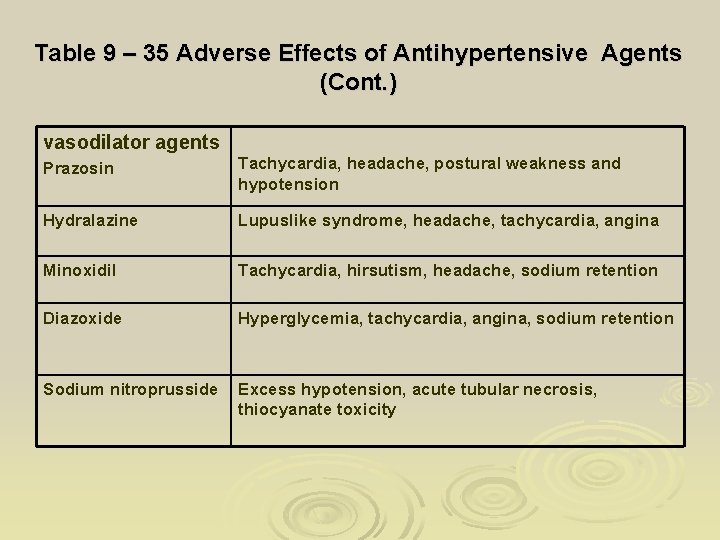
Table 9 – 35 Adverse Effects of Antihypertensive Agents (Cont. ) vasodilator agents Prazosin Tachycardia, headache, postural weakness and hypotension Hydralazine Lupuslike syndrome, headache, tachycardia, angina Minoxidil Tachycardia, hirsutism, headache, sodium retention Diazoxide Hyperglycemia, tachycardia, angina, sodium retention Sodium nitroprusside Excess hypotension, acute tubular necrosis, thiocyanate toxicity