ANTEPARTUM COMPLICATIONS Tracey Whitley BSN RNCOB CEFM Graduate

ANTEPARTUM COMPLICATIONS Tracey Whitley, BSN, RNC-OB, C-EFM Graduate Student University of North Carolina at Charlotte

ANTEPARTUM COMPLICATIONS � Influences on high-risk pregnancies � Biophysical � Genetic considerations � Nutritional � Maternal weight � Pica � Medical � Obstetrical � Psychosocial � Alcohol and drug use � Psychological status Box 26 -1

ANTEPARTUM COMPLICATIONS � Sociodemographic risk factors � Income � Lack of prenatal care � Age � Parity � Marital status � Residence � Ethnicity

ANTEPARTUM COMPLICATIONS � Environmental � Community risk acquired infections � Radiation, chemical, and industrial pollutants � Workplace risk

SCREENING AND DIAGNOSTIC TESTS � Indication � Routine � Obstetrical � Medical � Types � Non-invasive � Invasive

SCREENINGS � Maternal � Triple/ quad screen � Coombs � Glucose � Urine � Fetal kick counts

DIAGNOSTIC TESTING � Non-invasive � Ultrasound � Anatomy and growth � Biophysical profile � Doppler flow studies � Amniotic fluid index � Guidance for invasive procedures � MRI � Fetal monitoring (external only during antenatal period) � Non-stress test � Contraction stress test

DIAGNOSTIC TEST � Invasive �Amniocentesis (Amnio) �Genetic testing �Fetal maturity �Fetal hemolytic disease �Chorionic Villus Sampling (CVS) �Percutaneous Umbilical Blood Sampling (PUBS) � Intrauterine Fetal Transfusion

HYPERTENSION DISORDERS � Pathophysiologic mechanisms � Vasoconstriction � Vasospasms � Endothelial damage � Membrane permeability � Placental compromise � Vital organs

TYPES OF HYPERTENSION DIAGNOSTIC CRITERIA Type Diagnostic Criteria Chronic Hypertension + Present before pregnancy + Diagnosed prior to 20 weeks gestation + Continues past 6 weeks Gestational Hypertension + New onset, diagnosed after 20 weeks + Resolves before 6 weeks postpartum + No proteinuria Preeclampsia (Mild or Severe) + Hypertension and proteinuria Eclampsia + Preeclampsia with seizures/coma Superimposed preeclampsia/ eclampsia + Chronic hypertension + Addition of preeclampsia signs/ symptoms HELLP syndrome + May be associated with preeclampsia + May be present without preeclampsia

CHRONIC HYPERTENSION � Chronic Hypertension � Hypertension of ≥ 140 mm. Hg systolic or ≥ 90 mm. Hg diastolic diagnosed: � Prior to pregnancy or � Before the 20 th week of pregnancy or � Remains after 6 weeks postpartum � Mild or Severe � Mild = 140 -159/90 -109 � Severe = ≥ 160/≥ 110

GESTATIONAL HYPERTENSION � Gestational � Occurs Hypertension after the 20 th week of pregnancy � Absence of proteinuria � Resolved by 6 weeks postpartum

PREECLAMPSIA � Gestational � Definition Hypertension AND Proteinuria of proteinuria �≥ 300 mg in a 24 hour urine collection or 2 urine dipstick 1+ or greater at least 4 hours apart �Preeclampsia is a disease that affects the entire body

PREECLAMPSIA � Mild � � preeclampsia BP 140 -159/ 90 -109 Proteinuria < 5 grams in 24 hours � Severe Preeclampsia � Must have one of the following in addition to above � BP ≥ 160 systolic or ≥ 110 diastolic on 2 occasions 6 hours apart � Proteinuria ≥ 5 grams (5, 000 mg) � Cerebral or visual changes • Epigastric /right upper quadrant pain, � Fetal growth restriction � Severe headache � Impaired liver function � Oliguria (less than 500 m. L/24 hours) � Pulmonary Edema � Thrombocytopenia

ECLAMPSIA � Tonic-clonic (grand-mal) seizures or coma in a patient diagnosed with preeclampsia, when other causes of the seizure have been ruled out � Timing � Antepartum: 38%-53% � Intrapartum: 18%-36% � Postpartum: 11%-44% � Delivery is cure � After medically stabilized induction or cesarean birth is recommended

SUPERIMPOSED PREECLAMPSIA � Superimposed Preeclampsia � One or more of the following in addition to chronic hypertension � New onset of proteinuria or dramatic increase � Hypertension with proteinuria before the 20 th week � Sudden increase in BP when well controlled � Impaired liver function � Thrombocytopenia
HELLP �H Hemolysis � Red blood cells are damaged/destroyed � EL Elevated Liver Enzymes � Hepatic dysfunction SGOT > 70 U/L � LD > 600 U/L � � LP Low Platelets � <100, 000 � Severity may be dependent on level of platelets � 100, 000 -150, 000 mild � 50, 000 - 100, 000 moderate � <50, 000 severe

HELLP � Presents with nonspecific symptoms � Malaise � Viral type symptoms � Worse at night � Most often in 2 nd or early 3 rd trimester before signs and symptoms of preeclampsia show � Delay in treatment due to non- specific symptoms � Delivery is cure

RISK FACTORS FOR PREECLAMPSIA � Extremes of maternal age � Race � Comorbidities � Multi-fetal pregnancy � Previous history or preeclampsia � First pregnancy or first pregnancy with new partner

MATERNAL COMPLICATIONS � Maternal � Respiratory � Pulmonary � Acute edema, ARDS renal failure � Liver failure, hemorrhage or rupture � Cerebral edema, stroke, temporary blindness, retinal detachment, seizures (eclampsia) � Cardiac failure � DIC- Disseminated Intravascular Coagulation � Maternal death

FETAL COMPLICATIONS � Fetal � Intrauterine Growth Restriction � Oligiohydramnios � Abruptio placenta � Placental insufficiency causing fetal heart rate changes

NURSING ASSESSMENTS � History Blood pressure trends � Risk factors � CBC � CMP � � � Current physical assessment Blood pressure � Visual changes, epigastric pain � Deep tendon reflexes � Edema � Review lab work � Review fetal assessments Fetal heart rate monitoring � Fetal growth � Fetal Doppler studies �

NURSING MANAGEMENT AND TEACHING � Diet – p. 663 � Activity restrictions � Pharmacology therapy � Magnesium Sulfate � Antihypertensive drugs- table 27 -5 � Labetalol Hydrochloride � Hydralazine � Methyldopa � Nifedipine � Postpartum care � Future pregnancies and health care

EARLY BLEEDING CAUSES � Miscarriage � Several different types (Table 28 -1) � Premature dilation � Ectopic � Hydatidiform mole
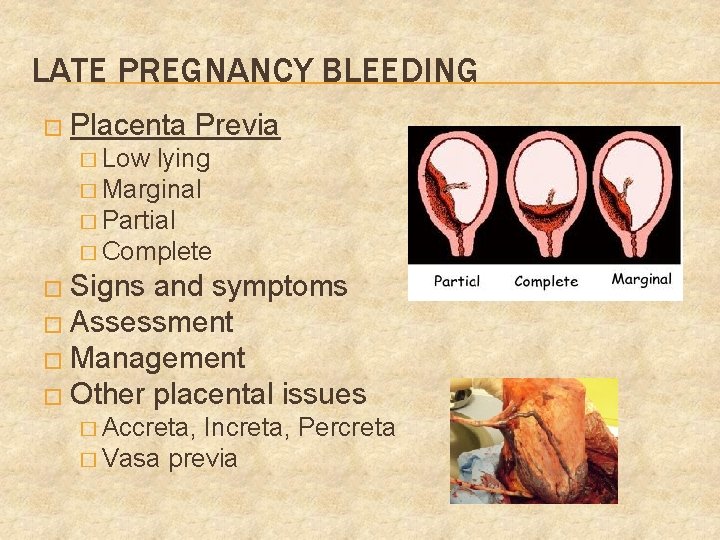
LATE PREGNANCY BLEEDING � Placenta Previa � Low lying � Marginal � Partial � Complete � Signs and symptoms � Assessment � Management � Other placental issues � Accreta, Increta, Percreta � Vasa previa
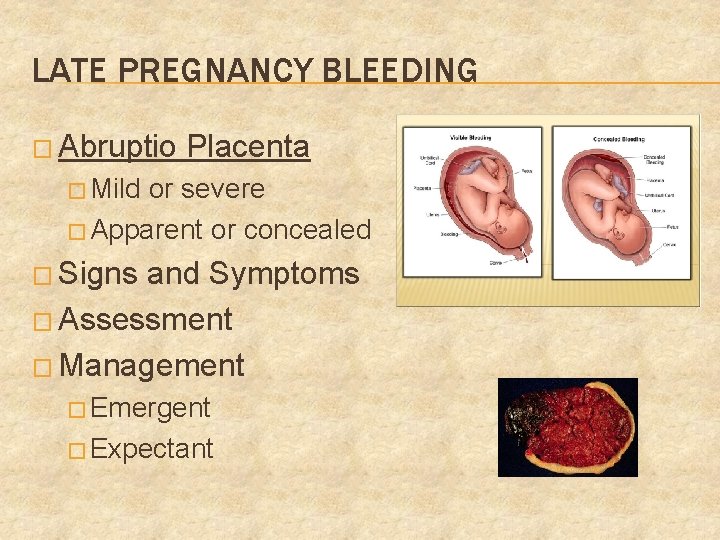
LATE PREGNANCY BLEEDING � Abruptio Placenta � Mild or severe � Apparent or concealed � Signs and Symptoms � Assessment � Management � Emergent � Expectant
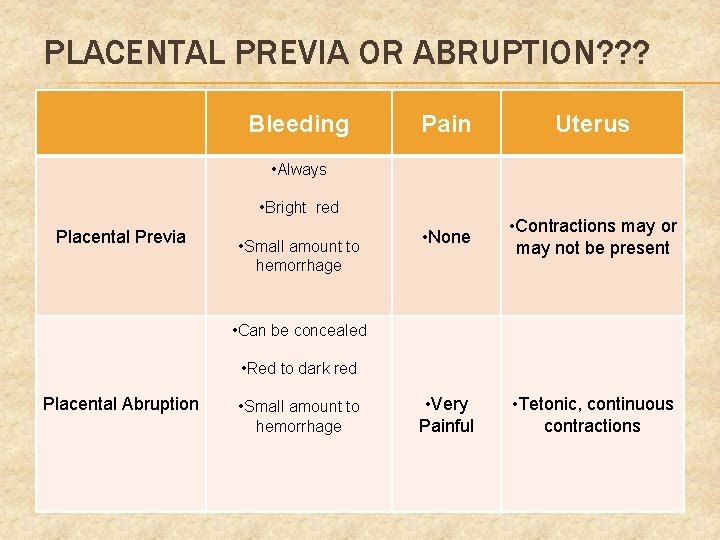
PLACENTAL PREVIA OR ABRUPTION? ? ? Bleeding Pain Uterus • None • Contractions may or may not be present • Very Painful • Tetonic, continuous contractions • Always • Bright red Placental Previa • Small amount to hemorrhage • Can be concealed • Red to dark red Placental Abruption • Small amount to hemorrhage

DIABETES IN PREGNANCY � Metabolic changes in pregnancy � Maternal glucose use � Maternal insulin use � Fetal glucose and insulin use � Type of diabetes � Pregestational � Type 1 � Type 2 � Gestational
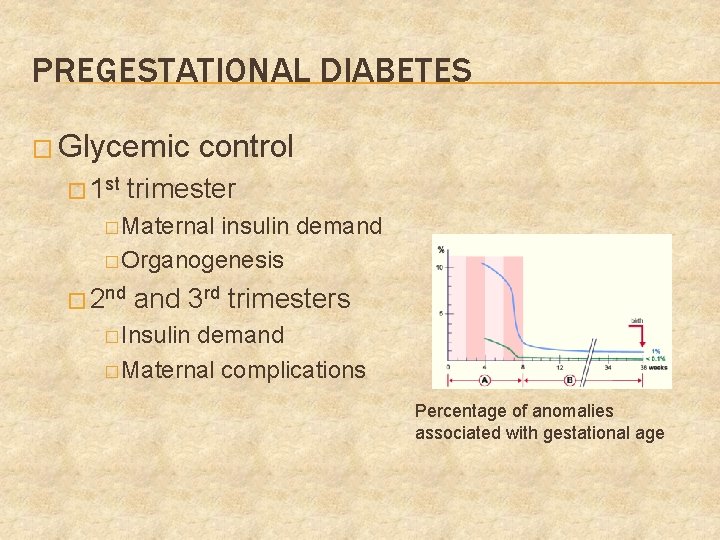
PREGESTATIONAL DIABETES � Glycemic � 1 st control trimester � Maternal insulin demand � Organogenesis � 2 nd and 3 rd trimesters � Insulin demand � Maternal complications Percentage of anomalies associated with gestational age

GESTATIONAL DIABETES � Diagnosed in the 2 nd half of pregnancy � Screening � Glucola � Oral Glucose Tolerance Test (OGTT) � Management � Diet � Exercise � Monitoring of blood glucose � Medications � Fetal Surveillance

DIABETES AND MATERNAL COMPLICATIONS � Increase risk of miscarriage (pregestational) � Macrosomia (shoulder dystocia, assisted delivery, c-section) � Hydramnios � Preeclampsia � Infections � Ketoacidosis � Hypoglycemia

DIABETES AND FETAL COMPLICATIONS � Congenital defects � Large for gestational age � Neonatal hypoglycemia � Control of maternal blood sugar � Antenatal � Intrapartum

HYPEREMESIS � � Unclear of causes but may be associated with high levels of estrogen and h. CG but also has a psychological component Hyperemesis is N&V with: � � � Weight loss Electrolyte imbalance Nutritional deficiencies Ketonuria Interventions � � IV therapy- fluids and electrolyte replacement Once acute vomiting has stopped Small frequent meals � Bland food but what sounds good � Ginger tea/ ginger ale � Compassionate, calm, and sympathetic care �

RESOURCES Cashion, K. (2012). Assessment for risk factors in pregnancy. In D. L. Lowermilk, S. E. Perry, K. Cashion, and K. R. Alden (Eds). Maternity & Women’s Health Care (10 th ed. )(pp. 637 -653). St. Louis, MO: Elsevier Mosby Cashion, K. (2012). Antepartum hemorrhagic disorders. In D. L. Lowermilk, S. E. Perry, K. Cashion, and K. R. Alden (Eds). Maternity & Women’s Health Care (10 th ed. )(pp. 670 -687). St. Louis, MO: Elsevier Mosby Cashion, K. (2012). Endocrine and metabolic disorders in pregnancy. In D. L. Lowermilk, S. E. Perry, K. Cashion, and K. R. Alden (Eds). Maternity & Women’s Health Care (10 th ed. )(pp. 688 -708). St. Louis, MO: Elsevier Mosby Dix, D. (2012). Hypertensive disorders in pregnancy. In D. L. Lowermilk, S. E. Perry, K. Cashion, and K. R. Alden (Eds). Maternity & Women’s Health Care (10 th ed. )(pp. 654 -669). St. Louis, MO: Elsevier Mosby Pictures from Google images
- Slides: 34