Annie OConnor PT OCS Cert MDT Rehabilitation Institute

+ Annie O’Connor PT, OCS, Cert. MDT Rehabilitation Institute of Chicago Corporate Director Musculoskeletal Practice Clinical Manager River Forest Spine & Sport Center Conservative Care Overview of Evidence-Based Strategies

+ “PAIN INSISTS ON BEING ATTENDED TO. God whispers to us in our pleasures, speaks in our consciences, but shouts in our PAINS. It is his megaphone to rouse a deaf world. ” C. S. LEWIS (Greatest Christian Contemporary Writer)

+ OBJECTIVES n Define conservative care n Organize conservative care interventions around patient role n Outline evidence supporting conservative care interventions of patient education, active care, manual therapy and injections

+ Definition Conservative Care Medical Dictionary Translation 1. Active treatment directed immediately to the cure of the disease or injury. 1. Active not passive treatment directed at cure not management. 2. Causal treatment directed against the cause/prevention of a disease. 2. Treatment geared toward prevention of reoccurrence. 3. Conservative treatment designed to avoid radical medical therapeutic measures or operative procedures. 3. Prioritize simplest treatments patient education and active care over procedures and surgeries. 4. Empiric treatment by means that experience has proved to be beneficial. 4. Sustainable measurable change for better!!

+ Conservative Care Stakeholders Pilot Co - Pilots n PATIENT n Osteopathic Physicians n Chiropractors n Physical Therapists n Occupational Therapists n Acupuncturists n Massage Therapists n Athletic Trainers n Personal Trainers “Could a greater miracle take place, than for us to look through each other’s eyes, for an instant? ” - Henry David Thoreau

+ The Simple Message of Conservative Care for the Complex Problem of Spinal PAIN Prioritize interventions that set the patient up to be the Pilot 1. WORDS – Patient Education 2. MOVES – Active Care and Exercise 3. HANDS – Manual Therapy, Injections, Acupuncture. "Coming together is a beginning; keeping together is progress; working together is success” - Henry Ford

+ Patient Education – Evidence Based n Patients with LBP advised to exercise, increased satisfaction and improved functional outcomes. It’s helpful to provide detailed booklets in the period immediately after their consultation when back pain at worst. Little et al, 2001 n Cognitive changes were shown to be associated in self-reported exercise activity when patients were given reassurance that exercise isn’t harmful. Cherkin et al, 1996 n Patients who read Treat Your Own Back demonstrated long term improvements in pain and satisfaction also demonstrated changes in number of episodes. Udermann et al, 2004

+ Patient Education – Evidence Based n Reducing fear avoidance behaviors using neurophysiology of pain mechanism education in people with chronic pain provides an effective strategy to decrease pain related disability and improve treatment outcomes. Fletcher et al, 2016 n Advice can translate into behavior changes. Robert et al, 2002 n Avoid jargon, Use terms and phrases with which the patient is comfortable. Mc. Kenzie & May, 2003 n Education: Patients understand more than heath professionals estimate. Moseley, 2003 n Serious consideration should be given to the development of short (<8 weeks) group and healthcare professional-delivered interventions. Randhawa et al, 2015

+ You Don’t Get Pain without a Brain Patient Education Topics: 1. Pain Alarm System – Pain comes from brain not the body – what do the signals mean? ? 2. Understand Dominating Pain Mechanism – Where is the breakdown in the alarm system? Nociception Brain Body 3. Movement Safe Pain – A guide to return to activity – Is my pain a green, yellow or red light? 4. Role of Emotions, Social Context to Pain – Are my thoughts, words, beliefs negative or positive? How am I coping with life pressures?
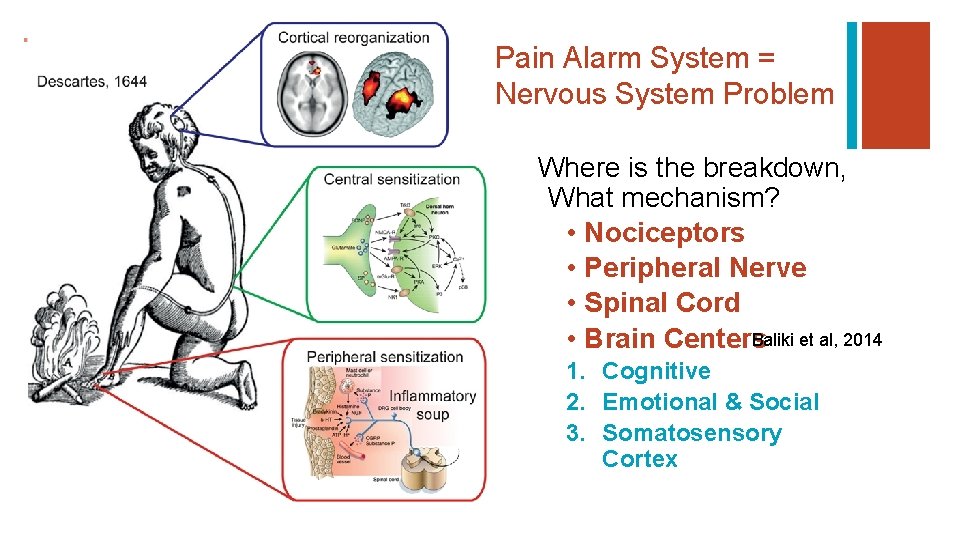
+ Pain Alarm System = Nervous System Problem Where is the breakdown, What mechanism? • Nociceptors • Peripheral Nerve • Spinal Cord Baliki et al, 2014 • Brain Centers 1. Cognitive 2. Emotional & Social 3. Somatosensory Cortex
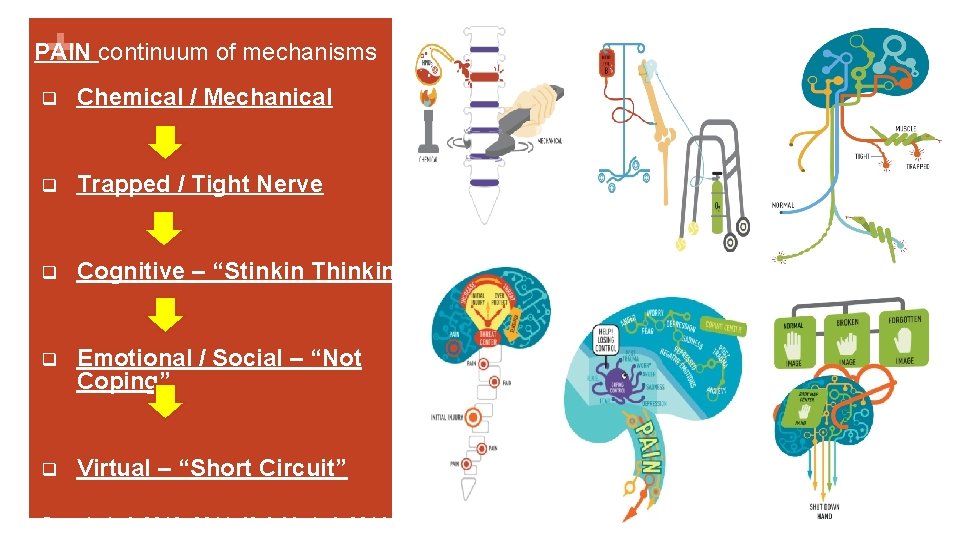
+ PAIN continuum of mechanisms q Chemical / Mechanical q Trapped / Tight Nerve q Cognitive – “Stinkin Thinkin” q Emotional / Social – “Not Coping” q Virtual – “Short Circuit” Smart et al, 2010, 2011; Kolski et al, 2014

+ Words Can Hurt, Harm or Heal!!! Wrong Words Right Words 1. Pain Receptors 1. Nociceptor 2. Pain Pathways 2. Spinal Nociceptor 3. Pain Fibers 3. Nociceptor Pathway 4. Pain Message 4. Nociceptor message 5. Pain Signal 5. Nociceptor Signal 6. Pain Stimulus 6. Noxious Stimulus Patient Friendly Words 1. Danger Detector 2. Danger transmitter 3. Danger Messenger = Nerve 4. Danger Message 5. Potentially Dangerous Stimulus Kolski, OConnor 2015. “World of Hurt: A Guide to Classifying Pain”

+ MOVES - Exercise Matters – “Movement Pill” Subgrouping Assures - we deliver the correct dosage, frequency and intensity!! Directional Preference – sometimes they need a direction 1. n Remodel Tight, Weak Tissues– sometimes they need to cause pain 2. n Exercises that produce, increase symptoms but no worse – “No Pain No Gain” Restore Function – sometimes they need to move efficient 3. n 4. Exercises to abolish symptoms – Centralization & Directional Preference Exercise that address function – learn to “do it differently” – apply Physics principles to the human kinetic chain Restore Life & Leisure – sometimes they need to gradually expose fear and / or pleasure – Learn to think and believe differently
+ Exercise Selection Patient Exercise Outcome

Predictors of positive outcomes at 2 weeks and 1 year With and without radiculopathy Despite presence of yellow flags Despite non-red flag neurological status per QTF Acutes: Up to 90% Chronics: Up to 50%

+ PAIN WAS ONLY OUTCOME CONSIDERED Searle A, Spink M, Ho A. Exercise interventions for the treatment of chronic low back pain: a systematic review and meta-analysis of randomized controlled trial. Clinical Rehabilitation 2015 Dec; 29(12): 1155 -67. RESULTS: Significant effect for strength/resistance and coordination/stabilization programs THE ACT OF MOVEMENT WAS NOT ADJUSTED

+ All Hands on Deck – Manual Medicine Last line of defense in Conservative Care Manual Medicine – should be offered when active care plateaus 1. Peripheral mechanism is derived from studies that demonstrate local mechanical hypoalgesia and reflex changes to muscles innervated by the treated joint. Bialosky et al. , 2009 2. Central mechanism - neurophysiological effect is seen in studies that find regional mechanical hypoalgesia, changes in SNS function, changes in spinal cord hyperexcitability, and changes in sensorimotor integration and motor control following manipulation (Bialosky et al. , 2009; Bishop, Beneciuk, & George, 2011; Coronado et al. , 2012; Haavik & Murphy, 2012; Schmid, Brunner, Wright, & Bachmann, 2008). 3. However neurophysiological effects of manipulation should not be equated with actual improvements in pain and outcome as many mechanistic studies are not designed to make this link.

+ All Hands on Deck –Needle Last line of defense in Conservative Care 1. n Injections – should be offered when active care is worsening symptoms and a chemically mediated inflammatory mechanism is dominating. A Randomized Trial of Epidural Glucocorticoid Injections for Spinal Stenosis. Janna L. Friedly, M. D. et al. N Engl J Med 2014; 371: 11 -21 July 3, 2014

+ All Hands on Deck –Needle Last line of defense in Conservative Care 2. Acupuncture – should be offered when active care has no effect; n symptoms are chemically mediated and unable to have steroids or pharmacy dominated peripherally n n beneficial effect when treating many inflammatory diseases and painful conditions, is thought to be useful to replace generally accepted pharmacological intervention. Ziilstra et al, 2003 symptoms are emotionally or socially mediated with poor active coping and dominated centrally and need overall calming n modulates activity within specific brain areas, including somatosensory cortices, limbic system, basal ganglia, brain stem, and cerebellum but also affective and cognitive processing. Wenjing et al, 2012

+ g n i h T d l O e Sam

+ Right Treatment, Right Patient, Right Time!!!!

+ Thank you "A community that excludes even one member is no community at all” - Pope Francis

+ References: www. musculoskeletal-pain. com Coupon code: 12$ off wohseminar PAIN INTERVENTION PRIORITY 1. WORDS 2. MOVES 3. HANDS

+ References: n Bialosky, J. E. , Bishop, M. D. , Price, D. D. , Robinson, M. E. , & George, S. Z. (2009). The mechanisms of manual therapy in the treatment of musculoskeletal pain: A comprehensive model. Manual Therapy, 14, 531– 538. n Bishop, M. D. , Beneciuk, J. M. , & George, S. Z. (2011). Immediate reduction in temporal sensory summation after thoracic spinal manipulation. The Spine Journal: Official Journal of the North American Spine Society, 11, 440– 446. n Coronado, R. A. , Gay, C. W. , Bialosky, J. E. , Carnaby, G. D. , Bishop, M. D. , & George, S. Z. (2012). Changes in pain sensitivity following spinal manipulation: A systematic review and meta-analysis. Journal of Electromyography and Kinesiology: Official Journal of the International Society of Electrophysiological Kinesiology, 22, 752– 767. n Haavik, H. , & Murphy, B. (2012). The role of spinal manipulation in addressing disordered sensorimotor integration and altered motor control. Journal of Electromyography and Kinesiology: Official Journal of the International. Society of Electrophysiological Kinesiology, 22, 768– 776. n Schmid, A. , Brunner, F. , Wright, A. , & Bachmann, L. M. (2008). Paradigm shift in manual therapy? evidence for a central nervous system component in the response to passive cervical joint mobilisation. Manual Therapy, 13, 387– 396. n Little, P. , Roberts, L. , Blowers, H. , Garwood, J. , Cantrell, T. , Langridge, J. et al. (2001). Should we give detailed advice and information booklets to patients with back pain? A randomized controlled factorial trial of a self-management booklet and doctor advice to take exercise for back pain. Spine, 26(19), 2065 -2072. n Roberts, L. , Little, P. , Chapman, J. , Cantrell, T. , Pickering, R. & Langridge, J. (2002). The back home trial: General practitionersupported leaflets may change back pain behavior. Spine, 27(17), 1821 -1828. n Cherkin, D. C. , Deyo, R. A. , Street, J. H. , Hunt, M. & Barlow, W. (1996). Pitfalls of patient education: Limited success of a program for back pain in primary care. Spine, 21(3), 345 -355 n Udermann, B. E. , Spratt, K. F. , Donelson, R. G. , Mayer, J. , Graves, J. E. , & Tillotson, J. (2004). Can a patient educational book change behavior and reduce pain in chronic low back pain patients? Spine Journal, 4(4), 425 -435.

+ References: n Smart KM, Curley A, Blake C, Staines A, Doody C. (2010)The reliability of clinical judgments and criteria associated with mechanisms-based classifications of pain in patients with low back pain disorders: a preliminary reliability study. Journal of Manual and Manipulative Therapy, Volume 18, No. 2: 102 -110. n Smart KM, Blake C, Staines A, Doody C. (2010) Clinical indicators of ‘nociceptive’, ‘peripheral neuropathic’ and ‘central’mechanisms of musculoskeletal pain. A Delphi survey of expert clinicians. Manual Therapy; 15: 80 -87. n Smart, K. , Blake, C. , Staines, A. , & Doody, C. (2011) The Discriminative validity of “nociceptive”, “peripheral neuropathic”, and “central sensitization” as mechanisms-based classifications of musculoskeletal pain. Clin J Pain; 27(8), 655 -663. n Kolski M, OConnor A, Van. Derlaan K, Jungwha A, Koslowski A, Deutch A. (2014) Validation of a pain mechanism classification system (PMCS) in physical therapy practice. Journal of Manual and Manipulative Therapy; 08 September, 1 -8. n Long A, Donelson R, Fung T. Does it matter which exercise? A randomized controlled trial of exercise for low back pain. Spine. 2004; 29(23): 2593 -602. n Cook C, Hegedus E, Ramey K. Physical therapy exercise intervention based on classification using the patent response method: a systematic review of the literature. J Manip Phys'l Ther. 2005; 13: 152 -62. n Mc. Kenzie, R. , & May, S. (2003). The lumbar spine mechanical diagnosis and therapy (Vol. 1, 2 nd ed. ). Waikanae, New Zealand: Spinal Publications New Zealand Ltd

+ References: n Moseley GL(2003). Unravelling the barriers to reconceptualisation of the problem in chronic pain: the actual and perceived ability of patients and health professionals to understand the neurophysiology. The Journal of Pain, 4(4), 184 -189. n Randhawa K, Côté P, Gross DP, Wong JJ, Yu H, Sutton D, Southerst D, Varatharajan S, Mior S, Stupar M, et al. J Can Chiropr Assoc. 2015 Dec; 59(4): 349 -62. The effectiveness of structured patient education for the management of musculoskeletal disorders and injuries of the extremities; a systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. n Claire Fletcher, BS, PTa, d, Lynley Bradnam, Ph. Db, c, and Christopher Barr, Ph. D d, The relationship between knowledge of pain neurophysiology and fear avoidance in people with chronic pain: A point in time, observational study. PHYSIOTHERAPY THEORY AND PRACTICE, 2016, VOL. 32, NO. 4, 271– 276 n Baliki, M. N. , Mansour, A. R. , Baria, A. T. , and Apkarian, A. V. (2014 b). Functional reorganization of the default mode network across chronic pain conditions. PLo. S ONE 9, e 106133. n Wenjing Huang, et al Plos One 2012; 7(4): e 32960; Characterizing Acupuncture Stimuli Using Brain Imaging with f. MRI - A Systematic Review and Meta-Analysis of the Literature. Published online 2012 Apr 9. doi: 10. 1371/journal. pone. 0032960 n Ziilstra et al, Anti-inflammatory actions of acupuncture. Mediators Inflamm. 2003 Apr; 12(2): 59– 69. doi: 10. 1080/0962935031000114943
- Slides: 26