Anna English Health History Developmental StagesTheories Physical Assessment



























- Slides: 34

Anna English

�Health History �Developmental Stages/Theories �Physical Assessment �Identify nursing problem/plan of care �Related Nursing Research

� 2 years & 2 weeks �Male �Admitted 1/6/16 �Admitted for central line infection �Allergies: Topical Iodine

�Intestinal malrotation→ bowel removal �G-tube dependent �TPN dependent �Hx central line infections �GERD

�Family separated due to frequent hospitalizations � 6 siblings �Financial burden of chronic illness �Single parent household �Special needs �Gastric tube dependent at home �TPN dependent at home

�Both parents involved, but unmarried/not together �Chronic illness �Low socioeconomic status �Developmentally delayed

�Central Line Infection �Klebsiella pneumoniae �Replace line �Short Bowel Syndrome

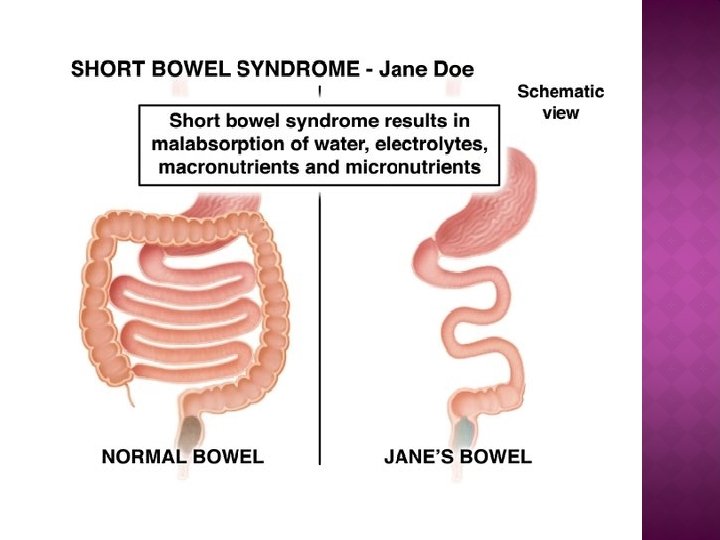
� Short bowel syndrome �Malabsorptive disorder that occurs as a results of decreased mucosal surface area Less absorptive area in intestines for fluid, electrolytes, and nutrients �Usually a result of extensive resection of the small intestine Necrotizing enterocolitis; born with insufficient amount of intestine leading to malrotation; cannot absorb enough �Pts need TPN to get sufficient nutrients �Patients on chronic TPN like this one, survival rates about 60% �Nutritional support greatest concern


�Strict I&O �Daily weights �NPO �Vital signs/assessment q 4 h �Nutrition �Cyclic TPN �Continuous 52 m. L/hr �Ethanol G-tube feeds—Elecare 30 kcal @ lock 70% MWF when off TPN �Posey bed �Plan to try bowel lengthening before bowel transplant at Georgetown

�Hx central line infection �TPN dependence �G-tube dependence �Fever �GERD

� Erikson �Autonomy � Piaget vs. Shame and Doubt �Pre-operational Stage �Egocentric �Animism �Magical thinking

�Personal/Social: 1. Increased independence from parent. 2. Parallel play. � Speech/Language: 1. 2. � Fine Motor/Adaptive: 1. 2. � Uses 2 -3 word phrases. Understands directional commands. Turns pages of book one at a time. Builds tower of 6 -7 cubes. Gross Motor: 1. 2. Picks up object without falling. Runs fairly well, with wide stance.

�Ritualism �Characteristic in quest for autonomy �Sameness and reliability provide a sense of comfort �Always approached pt smiling and saying his name �Used toys each time before implementing interventions �Important to establish a routine

� Neuro: Developmentally delayed � Cardiovascular/Neurovascular: PIV R hand 24 gauge; Hickman CVL upper right chest; belt to protect CVL � GI: G-tube abdomen LUQ � Musculoskeletal: Posey bed, unable to stand/walk � Skin: PIV R hand 24 gauge; granulation tissue around G-tube site � Psychosocial: Parent/guardian never present � Fall Risk: High (Humpty Dumpty)


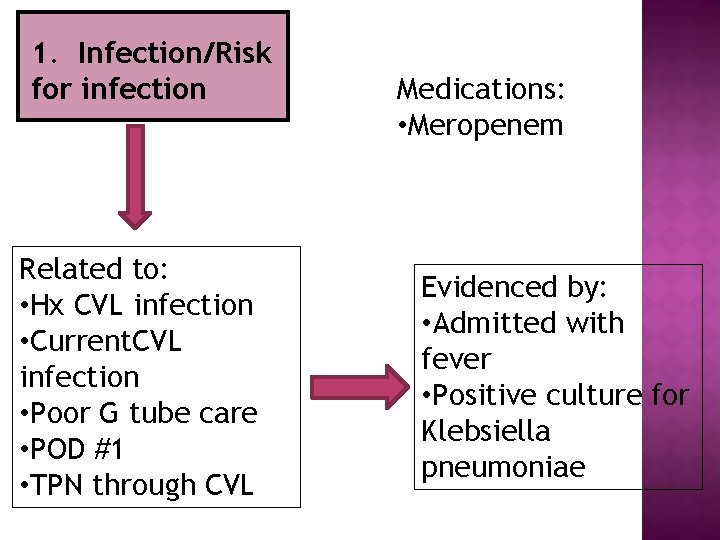
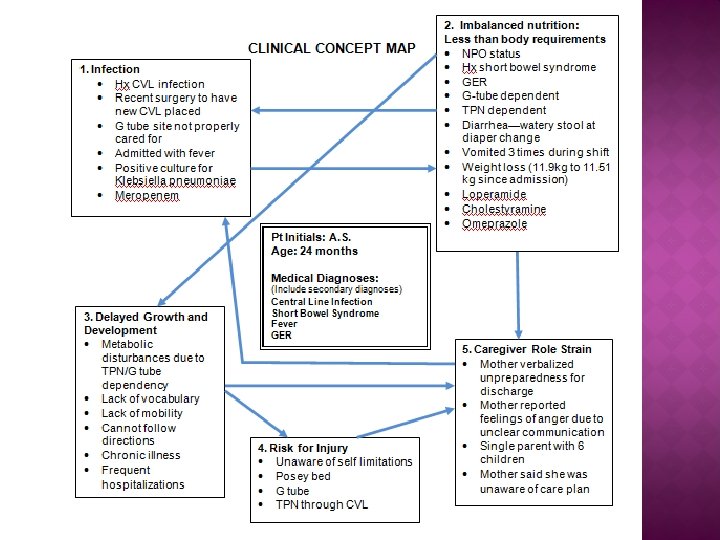
1. Infection/Risk for infection Related to: • Hx CVL infection • Current. CVL infection • Poor G tube care • POD #1 • TPN through CVL Medications: • Meropenem Evidenced by: • Admitted with fever • Positive culture for Klebsiella pneumoniae

�Wash hands prior to and after patient contact �Ensure CVL dressing dry and intact without drainage �Administer meropenem as ordered �Monitor vital signs q 4 h Expected outcome: Maintain patient’s temperature at baseline (axillary 36. 6 C) and receive negative culture results before discharge.

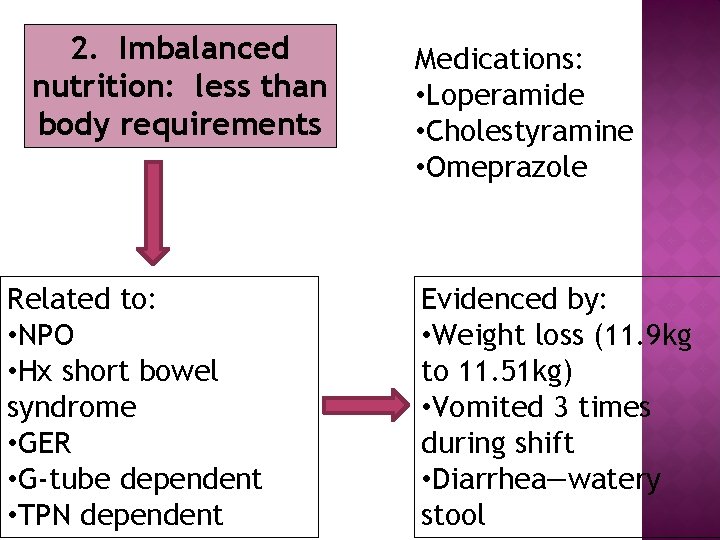
2. Imbalanced nutrition: less than body requirements Related to: • NPO • Hx short bowel syndrome • GER • G-tube dependent • TPN dependent Medications: • Loperamide • Cholestyramine • Omeprazole Evidenced by: • Weight loss (11. 9 kg to 11. 51 kg) • Vomited 3 times during shift • Diarrhea—watery stool

�Promote rest by tucking patient in bed to decrease metabolic demand �Assess fluid status and glucose levels q 4 h �Monitor I & O when starting feedings/TPN and at diaper changes �Monitor daily weights Expected outcome: Patient will be adequately nourished evidenced by maintaining weight throughout discharge.

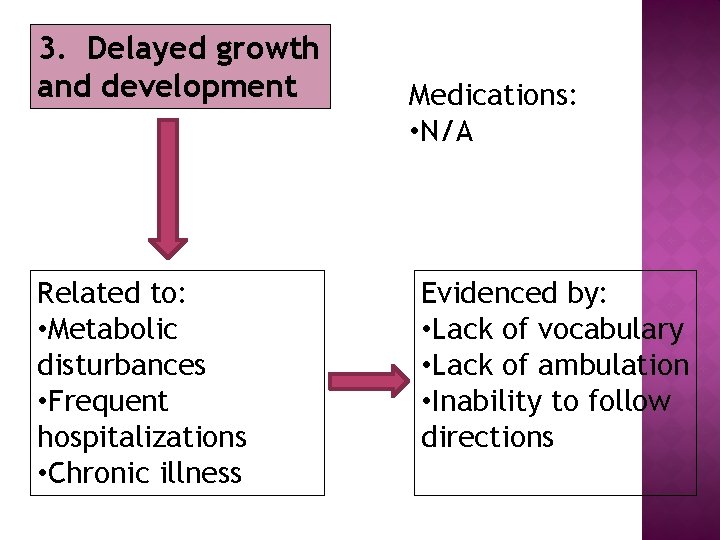
3. Delayed growth and development Related to: • Metabolic disturbances • Frequent hospitalizations • Chronic illness Medications: • N/A Evidenced by: • Lack of vocabulary • Lack of ambulation • Inability to follow directions

� Assess parental knowledge related to development by asking questions � Compare height and weight measurements to growth chart � Engage the child in appropriate play activities, like building blocks � Assess patient’s ability to follow directional commands Expected outcome: Patient will display evidence of age appropriate developmental tasks like parallel play before discharge.

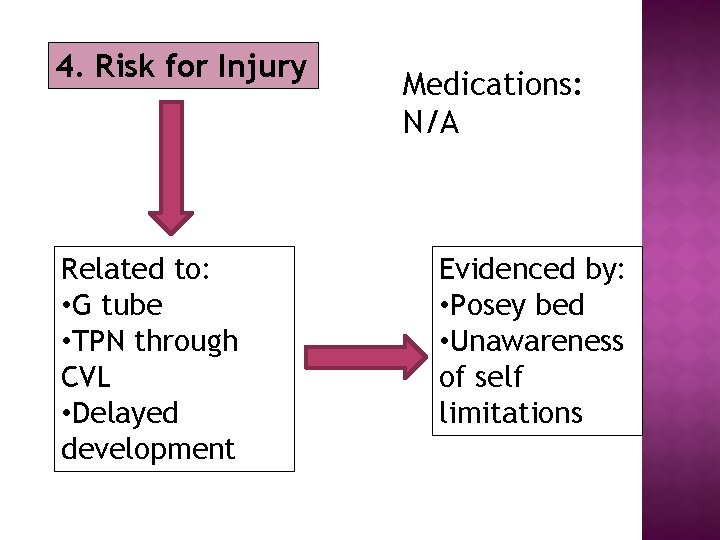
4. Risk for Injury Related to: • G tube • TPN through CVL • Delayed development Medications: N/A Evidenced by: • Posey bed • Unawareness of self limitations

� Remove any possible hazards from environment � Keep Posey bed in locked position � Teach parents about close supervision when playing � Keep TPN and G tube lines untangled to reduce risk of being pulled � Use belt around upper chest to protect CVL Expected outcome: Patient remains free of injury throughout discharge.

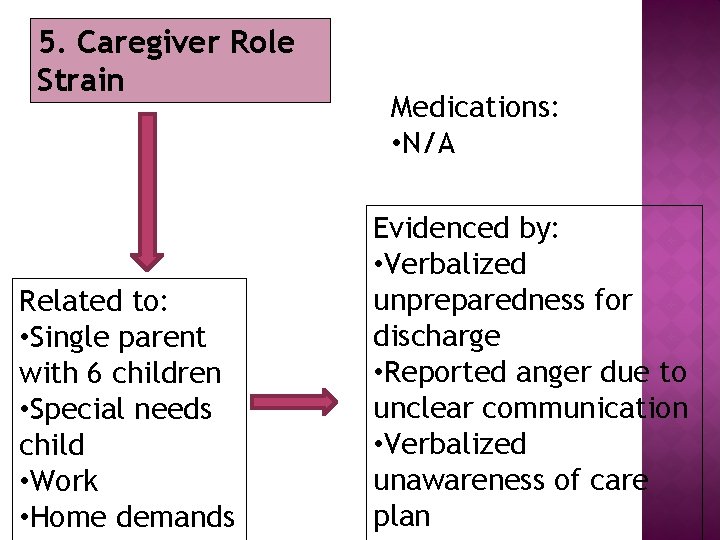
5. Caregiver Role Strain Related to: • Single parent with 6 children • Special needs child • Work • Home demands Medications: • N/A Evidenced by: • Verbalized unpreparedness for discharge • Reported anger due to unclear communication • Verbalized unawareness of care plan

� Encourage caregiver to talk about feelings of uncertainty, concerns � Help caregiver problem solve to meet patient’s needs. � Help caregiver identify and utilize support systems � Assess caregiver’s attitude/level of stress toward caring for patient Expected outcome: Family will verbalize understanding of care plan and verbalize preparedness for discharge within 24 hours.


�Traditional �Cluster care �Complimentary/Alternative �Television on for comfort �Play �Security objects Teddy bear �Collaborative �Child life was consulted

� Care options �Lengthening procedure—bowel transplant � Daycare help/home health � Gastrostomy tube care �If pulled out, cover with small clean dressing and tape…call doctor or nurse �If clogged, try to slowly push warm water into the tube with a 10 ml syringe. Repeat steps every 10 -15 minutes. Never use object to unclog it. If unable to unclog, call doctor or nurse. �Keep dressing clean and dry � CVL �Keep dressing dry and intact �Always secured

�Prospective study on central line associated bloodstream infections �Purpose: �Assess incidence rates and characteristics of CLABSIs � 152 patients; total of 14752 CVC days �Results: �CLABSI occurrence differed by type of catheter and patient group �Port-a-cath CVCs significantly lower risk of infection compared to tunneled CVCs, esp. long-term use

�Pt has history of CLABSIs �POD #1 �TPN via CVL �Bacteria �Pt thrive on sugar has tunneled CVL for longterm use, Port-a-cath deemed lower risk

�Pathophysiology �Physical Assessment Data �Developmental Theory �Holistic Plan of Care �Supplemental Nursing Research


Image retrieved from https: //i. vimeocdn. com/video/457068409_6 40. jpg. Wagner, M. , Bonhoeffer, J. , Erb, T. O. , Glanzmann, R. , Hacker, F. M. , Paulussen, M. , … Heininger, U. (2011). Prospective study on central venous line associated bloodstream infections. Archives of Disease in Childhood, 96, 827 -831. Wong, D. L. , Hockenberry, M. J. , & Wilson, D. (2015). Wong's nursing care of infants and children. St. Louis, MO: Mosby/Elsevier.