Anisa Suraya Ab Razak Identify the main classes

Anisa Suraya Ab Razak

§ Identify the main classes of antibiotic drugs § Distinguish between them in terms of mechanism of action § Recall the mechanisms of antibiotic resistance commonly used by bacteria to overcome resistance to drugs § Differentiate between the different anti-fungal drugs used to treat fungal infections § Summarise how virus uses host cells to replicate § Summarise the mechanisms of action of anti-viral drugs used to treat Herpes, Influenza, HIV and Hepatitis

§ Identify the main classes of antibiotic drugs § Distinguish between them in terms of mechanism of action § Recall the mechanisms of antibiotic resistance commonly used by bacteria to overcome resistance to drugs § Differentiate between the different anti-fungal drugs used to treat fungal infections § Summarise how virus uses host cells to replicate § Summarise the mechanisms of action of anti-viral drugs used to treat Herpes, Influenza, HIV and Hepatitis

§ SYNTHESIS • 3 components • A pentapeptide is created on N -acetyl muramic acid (NAM) • N-acetyl glucosamine (NAG) associates with NAM forming PTG § TRANSPORTATION § Bactoprenol transports PTG across the membrane § INCORPORATION § Transpeptidase enzyme cross- links Pt. G pentapeptides which then become incorporated into the cell wall

BETA LACTAMS GLYCOPEPTIDES § Bad People Count Carbs § Vancomycin § Penicillin: § Carbapenam: MOA § Cephalosporin: § bind to the pentapeptide MOA § bind covalently to transpeptidase enzyme inhibiting Pt. G incorporation into cell wall preventing PTG synthesis

MISCELLANEOUS Bacitracin § inhibits bactoprenol regeneration preventing PTG transportation Lipopeptide § disrupt Gram positive cell walls § Daptomycin Polymyxins § binds to LPS & disrupts Gram negative cell membranes

1. Which class of antibiotic does cephalosporin belong to and what is its mechanism of action?

2. What is the mechanism of action of vancomycin?

§ NUCLEIC ACID SYNTHESIS/FOLATE METABOLISM § DNA REPLICATION 1. PABA → (DHOp) → Dihydrofolate (DHF) § DNA gyrase • Catalysed by DHOp synthase 2. DHOp → Dihydrofolate (DHF) 3. DHF → Tetrahydrofolate (THF) • Catalysed by DHF reductase • THF – Important precursor in DNA synthesis • Topoisomerase releases tension to allow replication of DNA

§ RNA SYNTHESIS § PROTEIN SYNTHESIS § RNA polymerase § Ribosomes • Produces RNA from DNA template • Produce protein from RNA templates • Differ from eukaryotic RNA polymerase • Differ from eukaryotic ribosomes

§ they inhibit bacterial ribosomes § AMINOGLYCOSIDES § MACROLIDES § Gentamicin § Erythromycin § TETRACYCLINES § CHLORAMPHENICOL

§ FLUOROQUINONES § inhibit DNA gyrase & topoisomerase IV § Ciprofloxacin

§ RIFAMYCINS § inhibits bacterial RNA polymerase § Rifampicin

§ SULPHONAMIDES § DIAMINOPYRIMIDINES § Sulphonamides inhibit DHOp § Trimethoprim synthase § inhibits DHF reductase

3. Which antibiotic inhibits bacterial polymerase? a) Gentamicin b) Rifampicin c) Vancomycin d) Ciprofloxacin

4. Give an example of an aminoglycoside and how does it work?

5. Which antibiotic targets DNA synthesis? a) Ciprofloxacin b) Gentamicin c) Rifampicin d) Trimethoprim

§ Identify the main classes of antibiotic drugs § Distinguish between them in terms of mechanism of action § Recall the mechanisms of antibiotic resistance commonly used by bacteria to overcome resistance to drugs § Differentiate between the different anti-fungal drugs used to treat fungal infections § Summarise how virus uses host cells to replicate § Summarise the mechanisms of action of anti-viral drugs used to treat Herpes, Influenza, HIV and Hepatitis

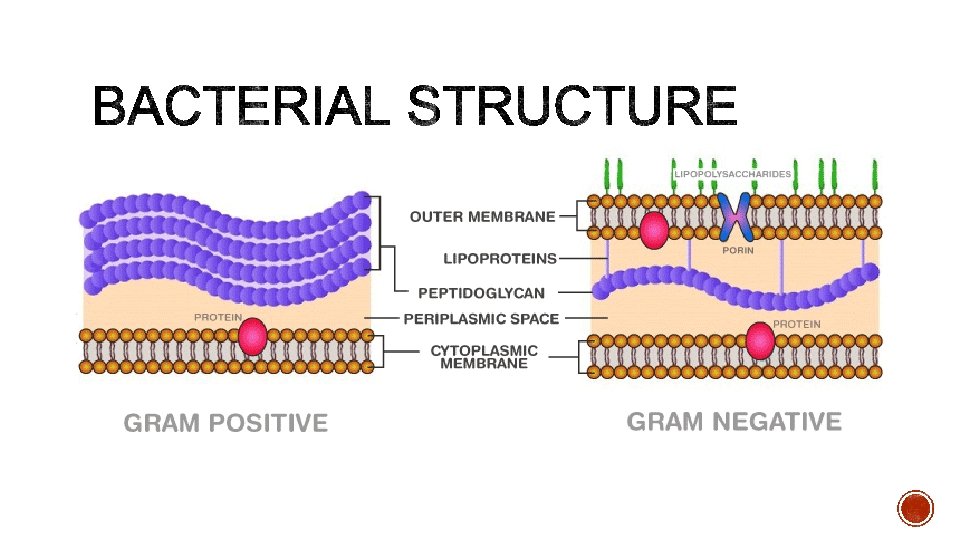
§ BAIT § B = Bypass antibiotic-sensitive pathways § A = impaired Accumulation of anitbiotic § I = enzyme-mediated drug Inactivation § T = altered Target or hyperproduction of Target

B § Additional target produced by bacteria § Unaffected by antibiotic § Example: § E Coli produce different DHF reductase enzyme, becoming resistant to Trimethoprim
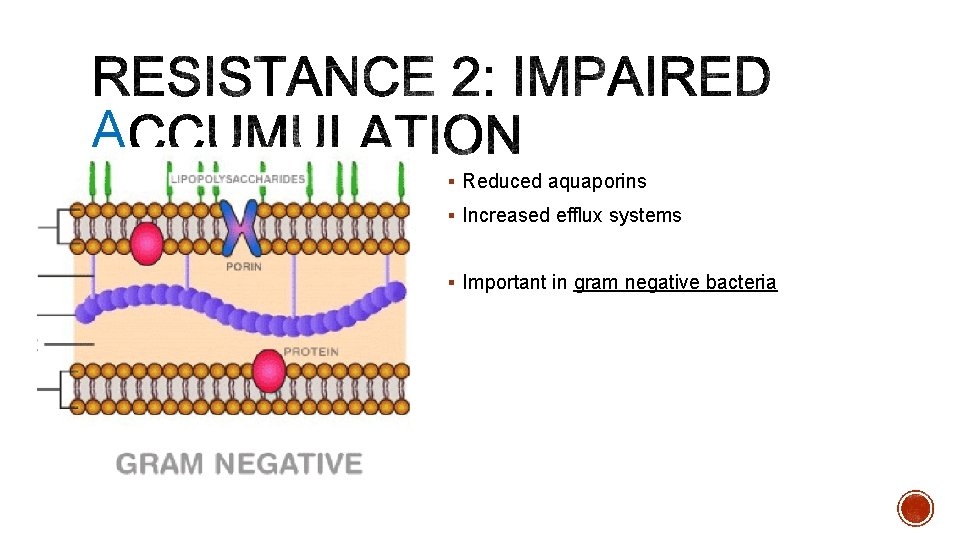
A § Reduced aquaporins § Increased efflux systems § Important in gram negative bacteria

INACTIVATION DRUG § Production of destruction enzymes i. e. which inactivates the drugs § Beta lactamases hydrolyse C-N bond of the beta lactam ring § Example: § Penicillin G and Penicillin V - gram positive activity but destroyed by beta lactamases § Flucloxacillin – gram positive activity, resistant to beta-lactamases § Temocillin – gram negative activity, resistant to beta-lactamases § Amoxicillin with clavulanic acid – brpad spectrum, resistant to beta-lactamases

T ALTERED § Alteration to enzyme targeted by antibiotic § Enzyme still working but antibiotic now ineffective § Example: § Staph Aureus – mutations in the Par. C region of topoisomerase IV leads to resistance to quinolones

HYPERPRODUCTION OF T § Significant increase in levels of target enzyme

§ 6. Name 2 mechanisms by which bacteria can acquire resistance to antibiotic treatment.

§ 7. Give an example of anitbiotic resistance due to drug inactivation.

§ Identify the main classes of antibiotic drugs § Distinguish between them in terms of mechanism of action § Recall the mechanisms of antibiotic resistance commonly used by bacteria to overcome resistance to drugs § Differentiate between the different anti-fungal drugs used to treat fungal infections § Summarise how virus uses host cells to replicate § Summarise the mechanisms of action of anti-viral drugs used to treat Herpes, Influenza, HIV and Hepatitis

TYPES OF INFECTION: § Superficial – outermost layers § Dermatophyte – skin, hair, nails § Subcutaneous – innermost skin layers § Systemic – mainly respiratory tract
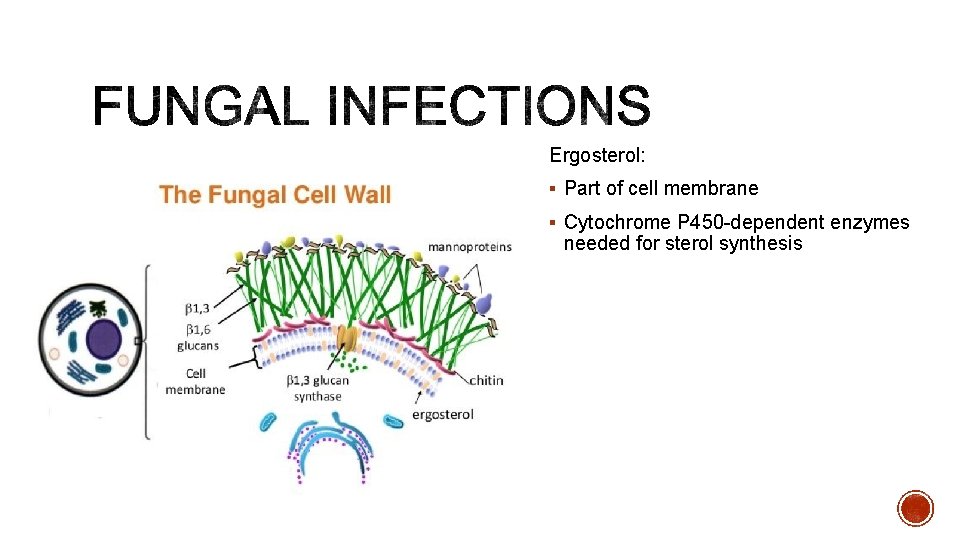
Ergosterol: § Part of cell membrane § Cytochrome P 450 -dependent enzymes needed for sterol synthesis

§ AZOLES § POLYENES § Target ergosterol production § Punch holes within cell membrane and § MOA: Inhibit cytochrome P 450 - dependent enzymes § Example: Fluconazole (oral) for candidiasis and systemic infections disrupts stability § MOA: Interact with sterols in cell membrane forming channels § Example: Amphotericin (IV) for systemic infections

§ 8. Woman was found to have vaginal thrush in clinic. Which drug would be an effective treatment and how would it work? a) Oral Fluconazole b) Amphotericin c) Ciprofloxacin d) Co-trimoxazole

§ Identify the main classes of antibiotic drugs § Distinguish between them in terms of mechanism of action § Recall the mechanisms of antibiotic resistance commonly used by bacteria to overcome resistance to drugs § Differentiate between the different anti-fungal drugs used to treat fungal infections § Summarise how virus uses host cells to replicate § Summarise the mechanisms of action of anti-viral drugs used to treat Herpes, Influenza, HIV and Hepatitis
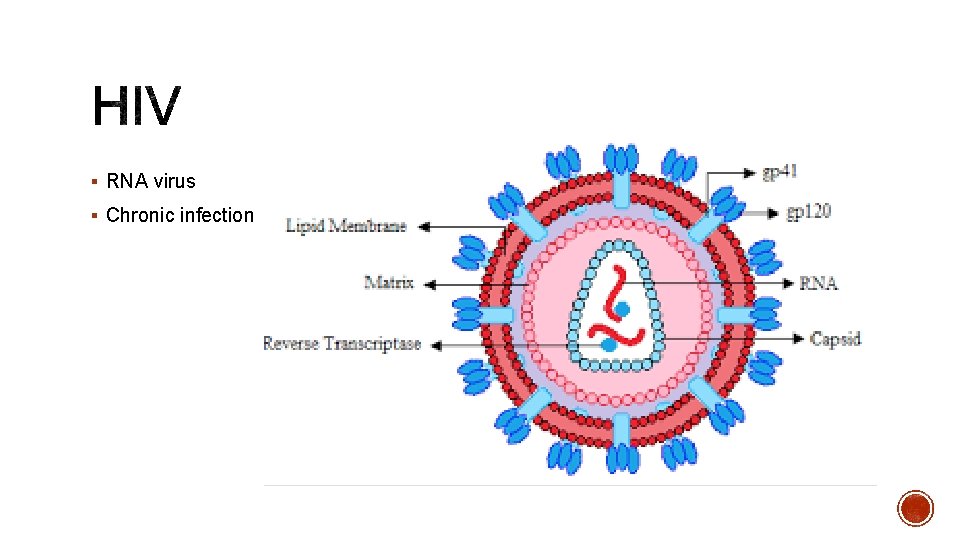
§ RNA virus § Chronic infection

§ 6 key steps: 1. Attachment – GP 120 binds to CCR 5, CXCR 4 and CD 4 receptors on CD 4 T cells 2. Entry – GP 41 penetrates host cell membrane, leading to viral capsid endocytosis 3. Replication – viral reverse transcriptase converts RNA intro DNA in cytoplasm 4. Integration – viral DNA is transported into nucleus and integrated by viral integrase host DNA 5. Assembly – production of viral RNA and proteins and host cell machinery. Viral Gag precursor encodes all viral structural proteins, cleaved by HIV protease. 6. Release – virus assembled and mature virus released

§ Entry inhibitors § Enfuvirtide - binds to GP 41 transmembrane protein § Maraviroc – blocks CCR 5 chemokine receptor § Reverse Transcriptase inhibitors (NRTI, NNRTI) § Nucleoside analogue – zidovudine (3 steps phosphorylation required) § Nucleotide analogue – Tenopfovir (Fewer phosphorylation) § Non-nucleoside analogue – Efavirenz (Np phosphorylation)

§ Integration inhibitor § Raltegravir – inhibits viral integrase § Protease inhibitors § Saquinavir – 1 st generation PI § Ritonavir – reduces PI metabolism at low doses – co-adminstered as “booster”
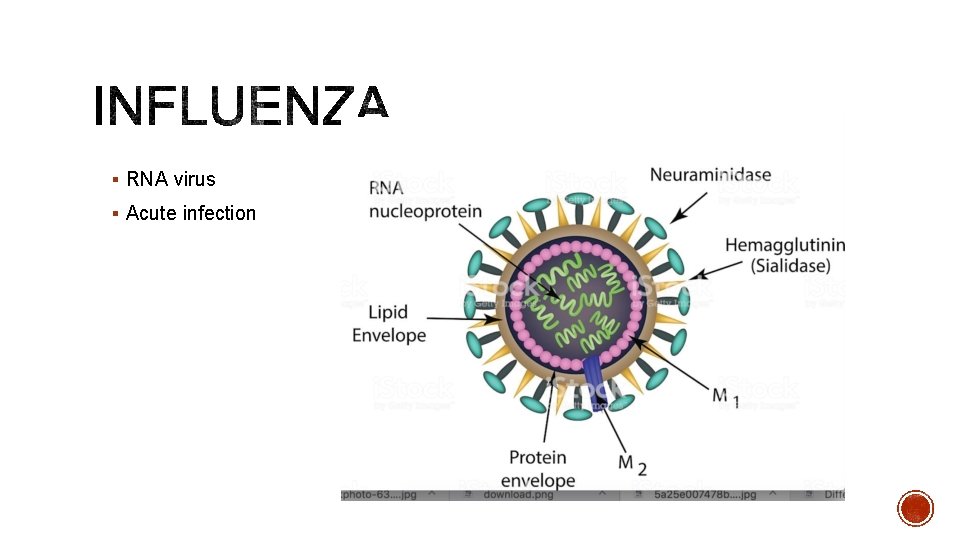
§ RNA virus § Acute infection

§ NA cleaves sialic acid to expose receptor on host cells § HA binds to sialic acid receptor allowing entry into host cell § Cleavage of HA by clara tryptase in lungs allows release, replicate in nose, throat, bronchi

§ Neuraminidase inhibitor - Oseltamivir

§ DNA virus § Acute/chronic infection § Infects liver hepatocytes § REPLICATION: § Uses reverse transcriptase and viral integrase to integrate into host DNA § ANTIVIRAL: § Nucleotide analogue – Tenofovir, sometimes given with peg-interferon alpha

§ RNA virus § Acute/chronic infection § Infects liver hepatocytes § REPLICATION: § Uses viral RNA polymerase § Uses viral protease to cleave viral polypeptide into viral particles

§ ANTIVIRAL: § Nucleoside analogue – Ribavarin with peg-interferon alpha § Protease inhibitors – e. g. bocoprevir most effective against HCV genotype 1 – NS 3/4 A inhibitors (previr) – NS 5 A inhibitors – NS 5 B/RNA polymerase inhibitors (buvir)

§ DNA virus § Acute/chronic infection § HSV 1 – cold sores § HSV 2 genital herpes § ANTIVIRALS § Nucleoside analogues - Aciclovir

§ 9. Which of the following statements is not true of HIV antiviral therapy? a) Raltegravir inhibits HIV viral integrase b) Maraviroc inhibits PG 41 HIV viral transmembrane protein c) Monotherapy is recommended for HIV treatment d) Zidovudine is a CCR 5 chemokine receptor blocker

§ 10. A 30 year old man was admitted to hospital last night and found to have positive PCR of influenza viral RNA. What would be an effective treatment for him? 1. Gentamicin 2. Oseltamivir 3. Efavirenz 4. Ribavirin

§ 11. A 56 year old man has become acutely unwell. Blood test revealed deranged liver function. He mentioned having tried IV drug use on one occasion in his university days. What is the likely diagnosis? § Name a possible class of drug which can be used to treat this condition.

§ tiny. cc/tutorialfeedback
- Slides: 48