ANIMAL HISTOLOGY BIOL 241 Topic 9 Skin Dr

ANIMAL HISTOLOGY BIOL 241 Topic 9: Skin Dr. Issa Al-Amri Department of Biological Sciences & Chemistry College of Arts & Sciences

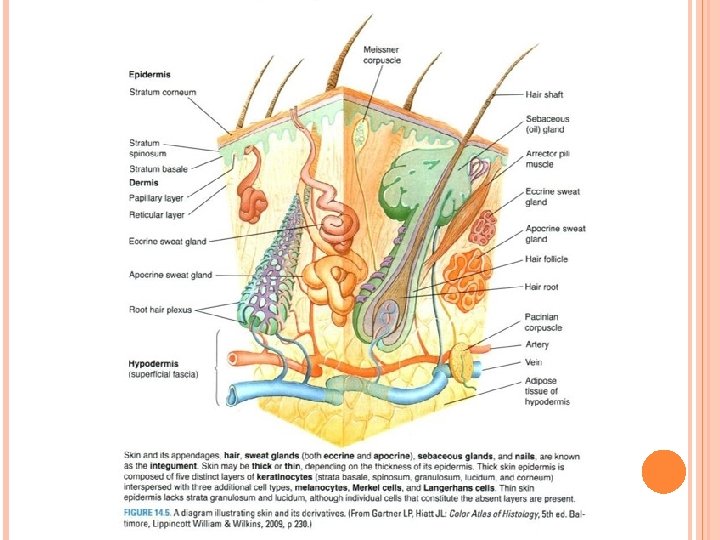
Introduction 1. Skin is the heaviest organ, about 16% of total body weight. 2. Composed of two layers; epidermis and dermis. 3. A deeper superficial fascial layer, the hypodermis, lies under the skin. Consists of loose connective tissue that binds skin loosely to subjacent tissue. 4. Skin contains several appendages (sweat glands, hair follicles, sebaceous glands, and nails). The skin and its appendages are called the integument. 5. Function. The skin protects body against injury, desiccation, and infection; regulates body temperature; absorbs ultraviolet (UV) radiation, which is necessary for synthesis of vitamin D; and contains receptors for touch, temperature, and pain stimuli from the external environment.
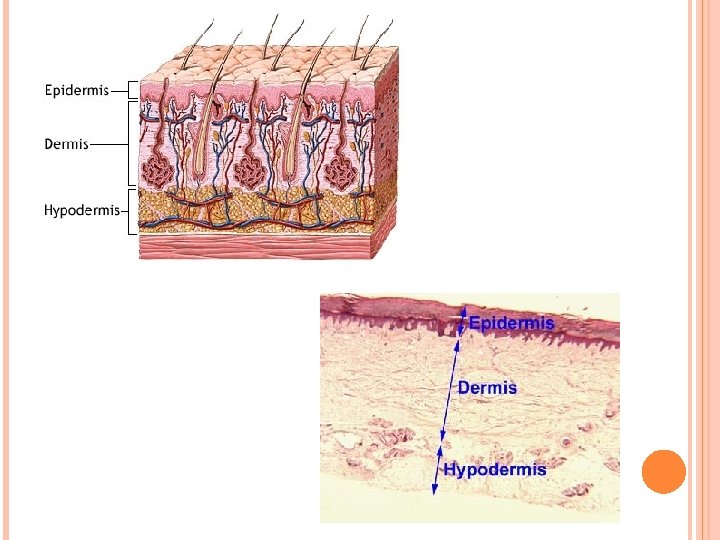
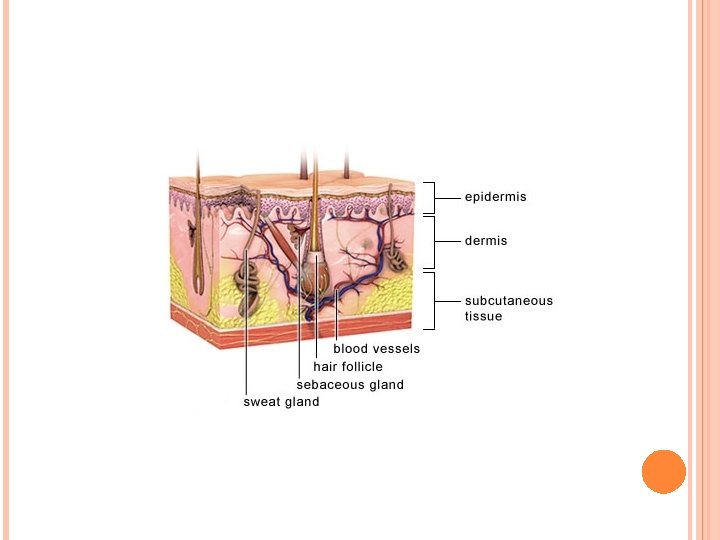

Epidermis I. Epidermis • Epidermis is the superficial layer of the skin. • Ectodermal layer of stratified squamous keratinized epithelium. • Composed of keratinocytes and three types of cells: melanocytes, Langerhans cells, and Merkel cells. • Constantly regenerated every 30 days by keratinocytes, which divide at night. • Has downgrowth (epidermal ridges) interdigitate with projections of dermis (dermal ridges), resulting in a highly irregular interface. Each dermal ridge subdivided by narrow downgrowth of epidermis (interpapillary peg).

Epidermis A. Layers of the epidermis 1. Stratum basale: deepest layer of epidermis, composed of keratinocytes (cuboidal to columnar in shape). • Cells attached to basal lamina of basement membrane by hemidesmosomes, and to each other by desmosomes. • This layer also contains melanocytes and Merkel cells. 2. Stratum spinosum: consists of few layers of polyhedral keratinocytes (prickle cells). • Their extensions “intercellular bridges” terminate in desmosomes.

Epidermis 3. Stratum granulosum: most superficial layer which nuclei still present. • Made of 3 -5 layers of flattened keratinocytes contain: keratohyalin granules, bundles of keratin filaments, and few membrane-coating granules. 4. Stratum lucidum: clear, homogeneous layer superficial to stratum granulosum; found only in palmar and plantar skin. • Consists of keratinocytes (no nuclei or organelles), contain keratin filaments and eleidin. 5. The stratum corneum: most superficial layer of the epidermis. • Consist of 15 -20 layers of flattened, nonnucleated dead cells (squames) filled with keratin.
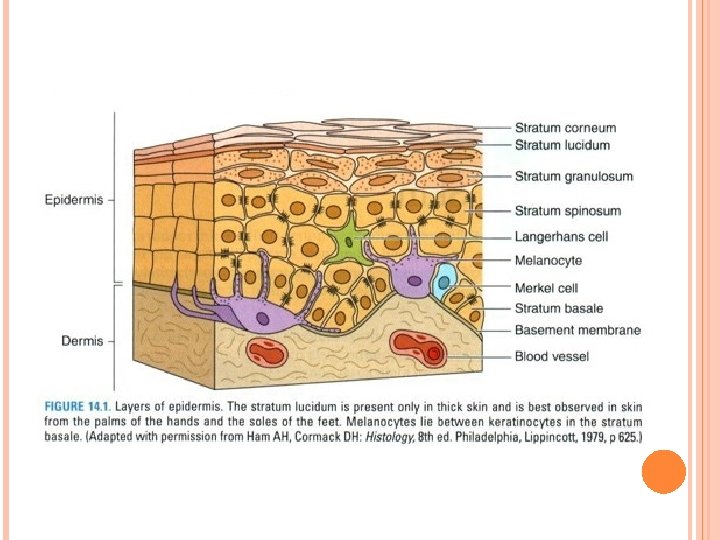
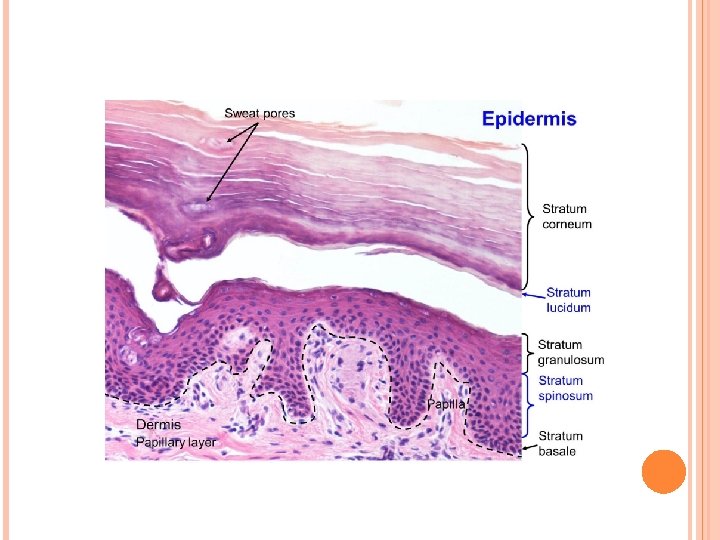

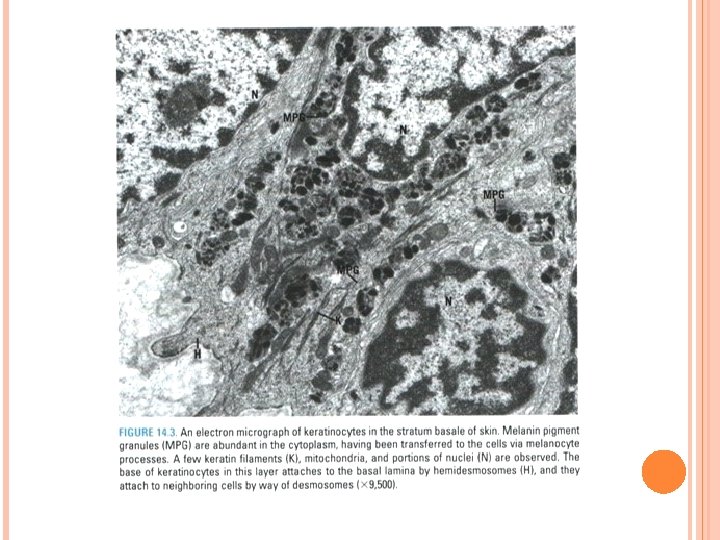

Epidermis B. Nonkeratinocytes in epidermis 1. Melanocytes: • Present in stratum basale and originate from neural crest. • Synthesize dark brown pigment (melanin) in oval-shaped organelles (melanosomes). • Melanosomes contain tyrosinase, UV-sensitive enzyme directly involved in melanin synthesis. • Melanin protects against tissue damage caused by UV radiation.

Epidermis 2. Langerhans cells: • • Dendritic cells originate in bone marrow. Located in stratum spinosum. Contain characteristic paddle-shaped Birbeck granules. Function as antigen-presenting cells in immuneresponses to contact antigens (contact allergies) and skin grafts. 3. Merkel cells: • Present in small numbers in stratum basale, near areas of well-vascularized, connective tissue. • Contain desmosomes and keratin filaments. • Receive afferent nerve terminals, function as sensory mechanoreceptors.
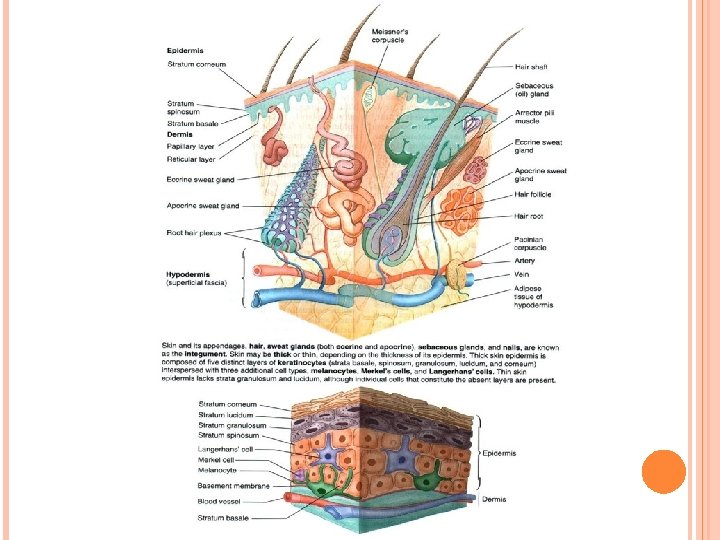
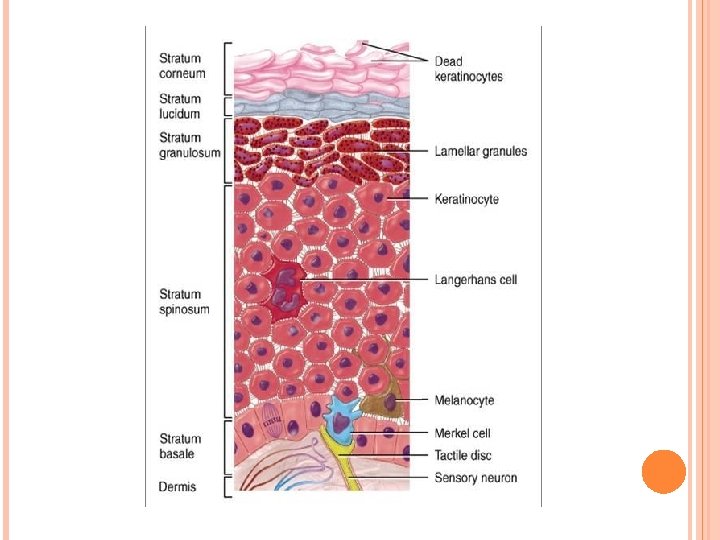

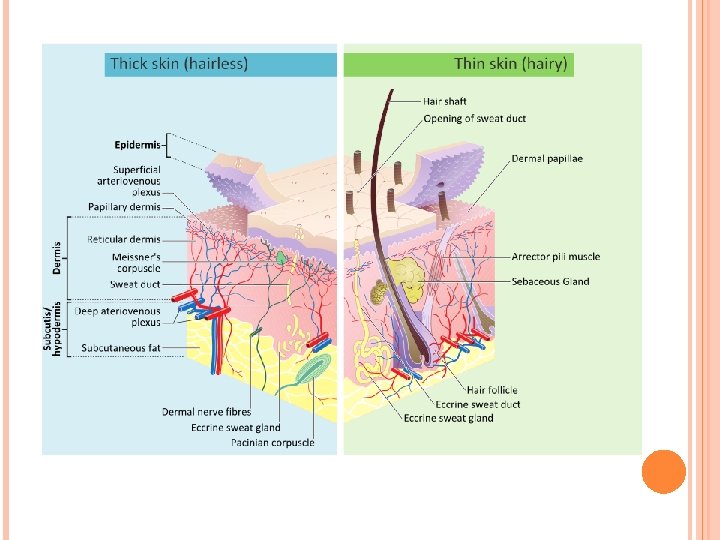
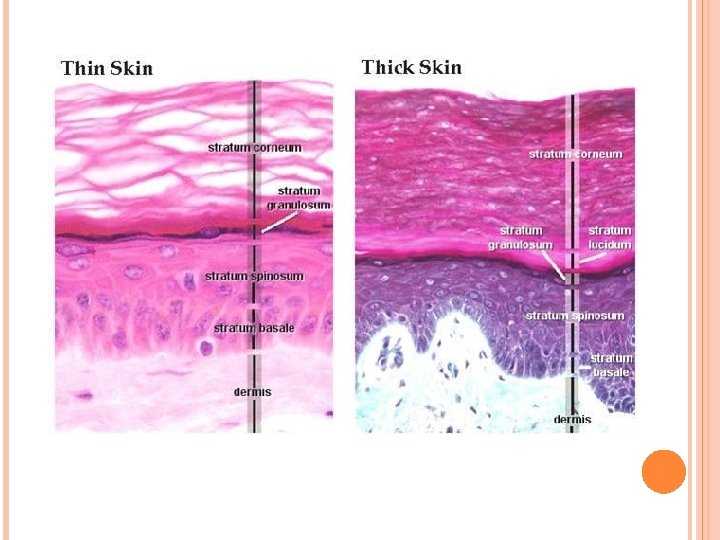
Epidermis C. Thick and thin skin (based on thickness of epidermis): 1. Thick skin (400 -600 µm thick). • Prominent stratum corneum, stratum granulosum, and stratum lucidum. • Lines palms of the hands and soles of the feet. • Lacks hair follicles, sebaceous glands, arrector pili muscles. 2. Thin skin (75 -150 µm thick). • Has less prominent stratum corneum, lacks stratum granulosum and stratum lucidum. • Thin skin covers most of the body and contains hair follicles, sebaceous glands, andarrector pili muscles.
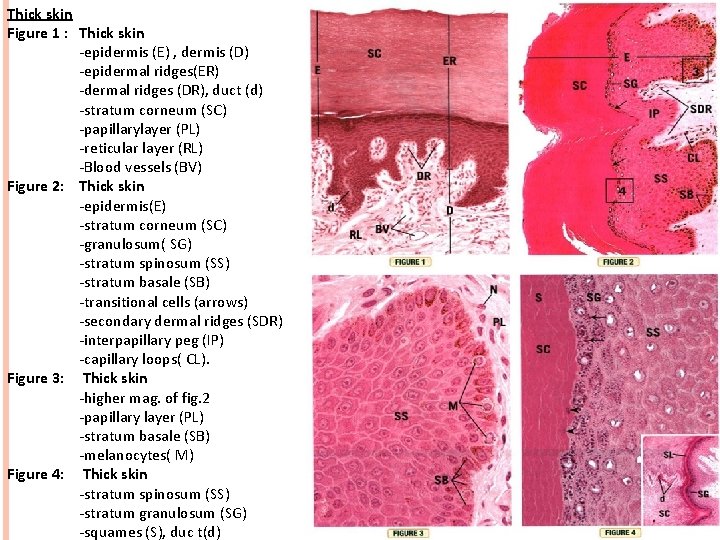
Thick skin Figure 1 : Thick skin -epidermis (E) , dermis (D) -epidermal ridges(ER) -dermal ridges (DR), duct (d) -stratum corneum (SC) -papillarylayer (PL) -reticular layer (RL) -Blood vessels (BV) Figure 2: Thick skin -epidermis(E) -stratum corneum (SC) -granulosum( SG) -stratum spinosum (SS) -stratum basale (SB) -transitional cells (arrows) -secondary dermal ridges (SDR) -interpapillary peg (IP) -capillary loops( CL). Figure 3: Thick skin -higher mag. of fig. 2 -papillary layer (PL) -stratum basale (SB) -melanocytes( M) Figure 4: Thick skin -stratum spinosum (SS) -stratum granulosum (SG) -squames (S), duc t(d)
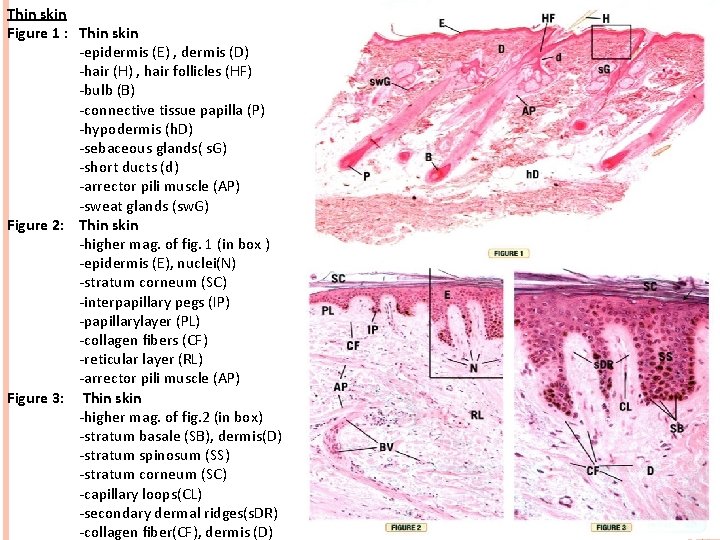
Thin skin Figure 1 : Thin skin -epidermis (E) , dermis (D) -hair (H) , hair follicles (HF) -bulb (B) -connective tissue papilla (P) -hypodermis (h. D) -sebaceous glands( s. G) -short ducts (d) -arrector pili muscle (AP) -sweat glands (sw. G) Figure 2: Thin skin -higher mag. of fig. 1 (in box ) -epidermis (E), nuclei(N) -stratum corneum (SC) -interpapillary pegs (IP) -papillarylayer (PL) -collagen fibers (CF) -reticular layer (RL) -arrector pili muscle (AP) Figure 3: Thin skin -higher mag. of fig. 2 (in box) -stratum basale (SB), dermis(D) -stratum spinosum (SS) -stratum corneum (SC) -capillary loops(CL) -secondary dermal ridges(s. DR) -collagen fiber(CF), dermis (D)

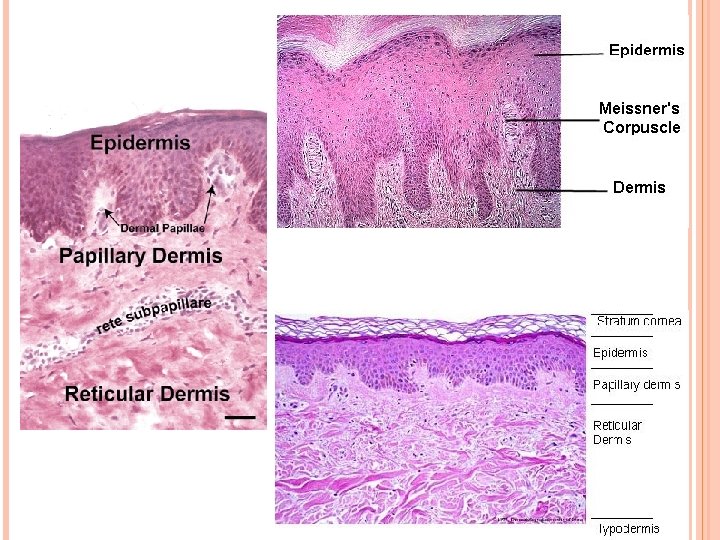
Dermis II. Dermis • Layer of skin underlying epidermis. • Mesodermal layer of dense, irregular connective tissue contains type I collagen fibers and networks of thick elastic fibers. • Divided into superficial papillary layer and deeper reticular layer. A. Dermal papillary layer: uneven, forms dermal ridges (dermal papillae), which interdigitate with epidermal ridges. • Composed of thin, loosely arranged fibers and cells and contains capillary loops and Meissner corpuscles; fine-touch receptors (identify two different coins by feeling them).

Dermis B. Dermal reticular layer: • Constitutes major portion of the dermis. • Composed of dense bundles of collagen fibers and thick elastic fibers. • Deeper; contain Pacinian corpuscles; a pressure receptors, as well as Krause end-bulbs.
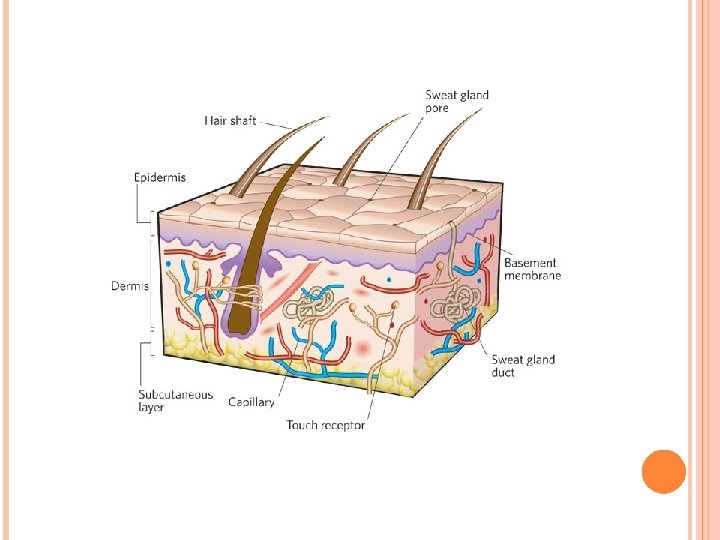

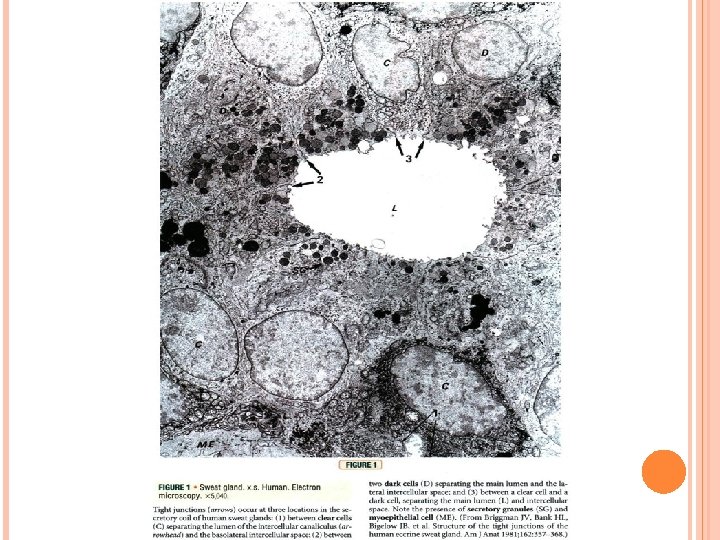
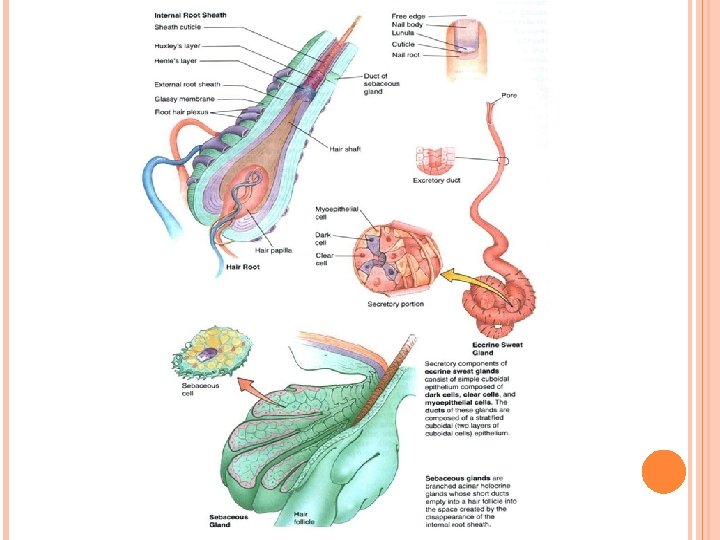
Glands in skin III. Glands In the Skin A. Eccrine sweat glands: Simple coiled tubular glands consisting of secretory unit and a single duct. • Present in skin throughout the body. 1. Secretory unit of eccrine sweat glands: embedded in dermis, composed of three cell types: a. Dark cells: line lumen of gland. contain mucinogen-rich secretory granules. b. Clear cells: underlie dark cells, rich in mitochondria, glycogen, contain intercellular canaliculi extend to lumen of the gland. Secrete a watery, electrolyte-rich material. c. Myoepithelial cells: lie beneath clear cells. They contract and aid in expressing gland’s secretions into the duct.
Glands in skin 2. Duct of eccrine sweat glands: narrow, lined by stratified cuboidal epithelial cells; contain many keratin filaments and have a prominent terminal web. • Cells forming external (basal) layer of duct have many mitochondria and a prominent nucleus. a. Duct leads from secretory unit through superficial portions of dermis to penetrate an interpapillary peg of epidermis and spiral through all of its layers to deliver sweat to the outside. b. As secreted material passes through duct, its cells reabsorb some electrolytes and excrete other substances (such as urea, lactic acid, ions, and certain drugs)
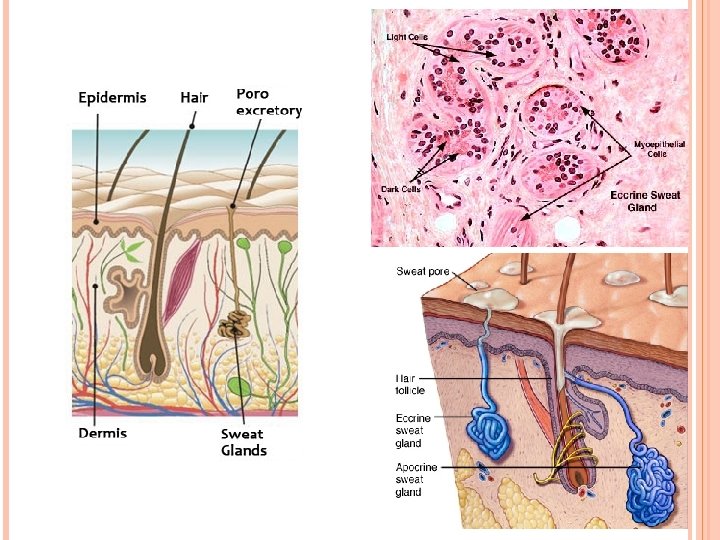
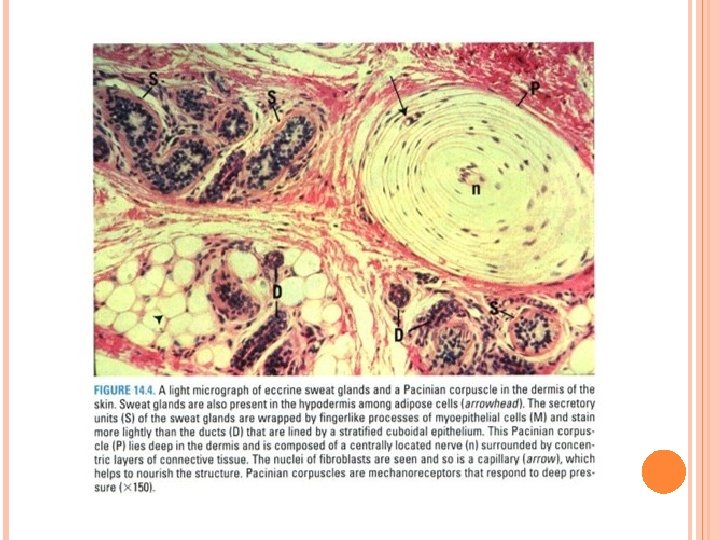

Glands in skin B. Apocrine sweat glands: • Include large, specialized sweat glands (e. g. , axilla) and ceruminous (wax) glands of external auditory canal. 1. These glands responsive to hormonal influences. 2. Their large coiled secretory units are enveloped by scattered myoepithelial cells. 3. These glands empty their viscous, odorless secretions into hair follicles. Bacteria act on these secretions to produce odors that are somewhat specific to each individual.

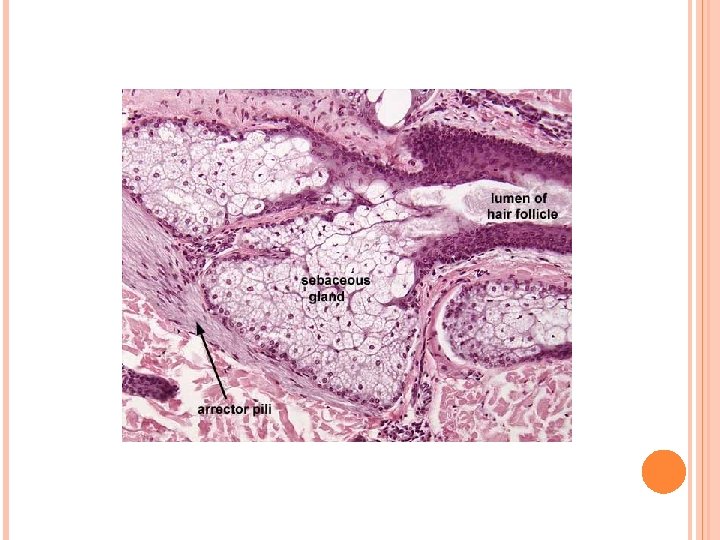
Glands in skin C. Sebaceous glands: branched acinar glands having a lobular appearance. • The clustered acini of one sebaceous gland empty into a single short duct. 1. The duct empties into the neck of a hair follicle. 2. Sebaceous glands are embedded in the dermis over most of the body’s surface but are absent from the palms and soles. They are most abundant on the face, forehead, and scalp. 3. These holocrine glands release sebum (composed of an oily secretion and degenerating epithelial cells).
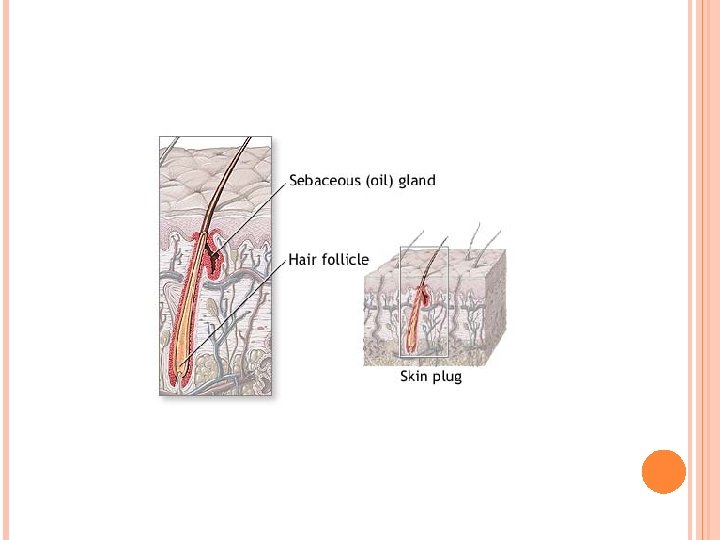

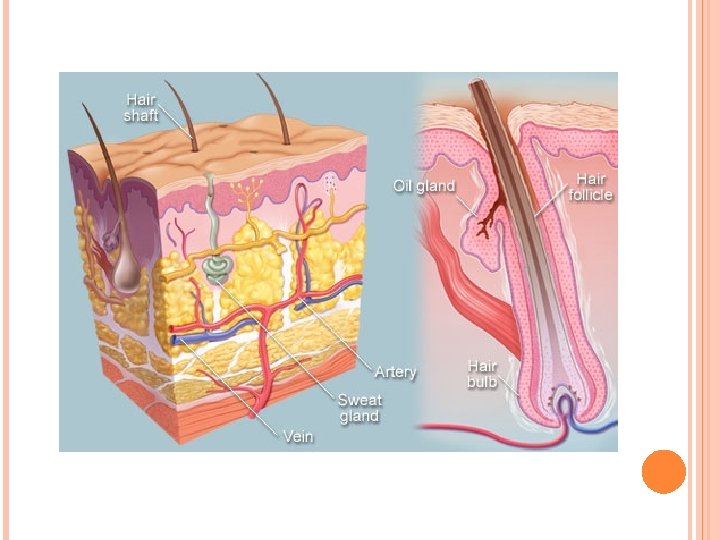
Hair follicle IV. Hair follicle • Hair follicle is an invagination of the epidermis extending deep into the dermis. 1. Hair shaft: long, slender filament in center of follicle extends above surface of epidermis. consists of inner medulla, cortex, and outer cuticle of the hair. At its deep end, it is continuous with the hair root. 2. Hair bulb: terminal expanded region of hair follicle wher hair is rooted. indented by dermal papilla; contains capillary network for sustaining the follicle. Hair bulb contains cells form internal root sheath and medulla of hair shaft.

Hair follicle 3. The internal root sheath lies deep to the entrance of the sebaceous gland. It is composed of the Henle layer, the Huxley layer, and the cuticle. 4. The external root sheath is a direct continuation of the stratum malpighii of the epidermis. 5. The glassy membrane is a noncellular layer, a thickening of the basement membrane. It separates the hair follicle from the surrounding dermal sheath.
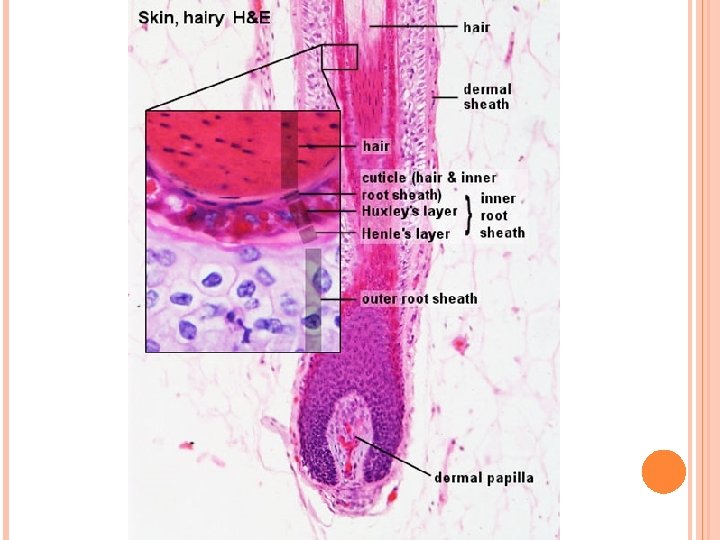
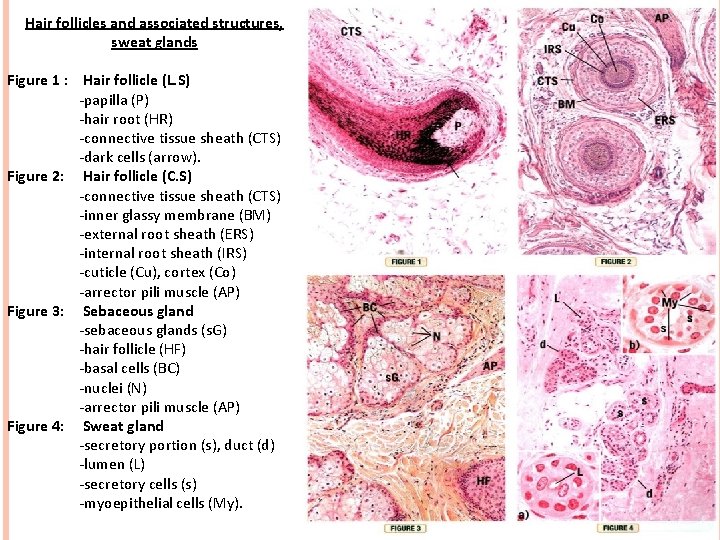
Hair follicles and associated structures, sweat glands Figure 1 : Hair follicle (L. S) -papilla (P) -hair root (HR) -connective tissue sheath (CTS) -dark cells (arrow). Figure 2: Hair follicle (C. S) -connective tissue sheath (CTS) -inner glassy membrane (BM) -external root sheath (ERS) -internal root sheath (IRS) -cuticle (Cu), cortex (Co) -arrector pili muscle (AP) Figure 3: Sebaceous gland -sebaceous glands (s. G) -hair follicle (HF) -basal cells (BC) -nuclei (N) -arrector pili muscle (AP) Figure 4: Sweat gland -secretory portion (s), duct (d) -lumen (L) -secretory cells (s) -myoepithelial cells (My).

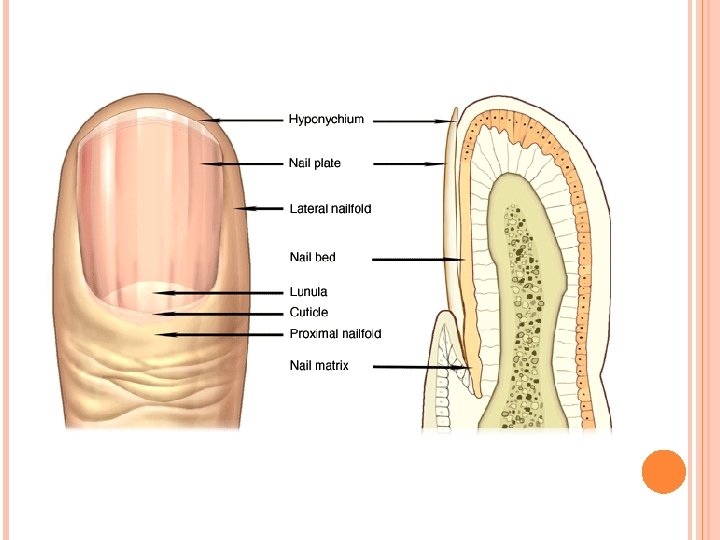
Nails VII. Nails (located on distal phalanx of each finger and toe): 1. Nails are hard keratinized plates that rest on the nail bed of the epidermis. 2. At the proximal end, each is covered by a fold of epidermis, called the cuticle or eponychium, which corresponds to the stratum corneum. The cuticle overlies the crescent-shaped whitish lunula. 3. At the distal (free) edge, each is underlain by the hyponychium, which is also composed ofstratum corneum. 4. Nails grow as the result of mitoses of cells in the matrix of the nail root.

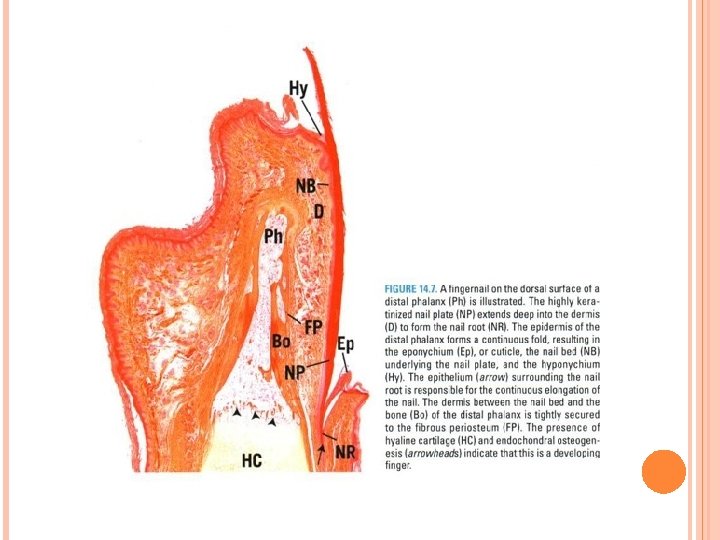
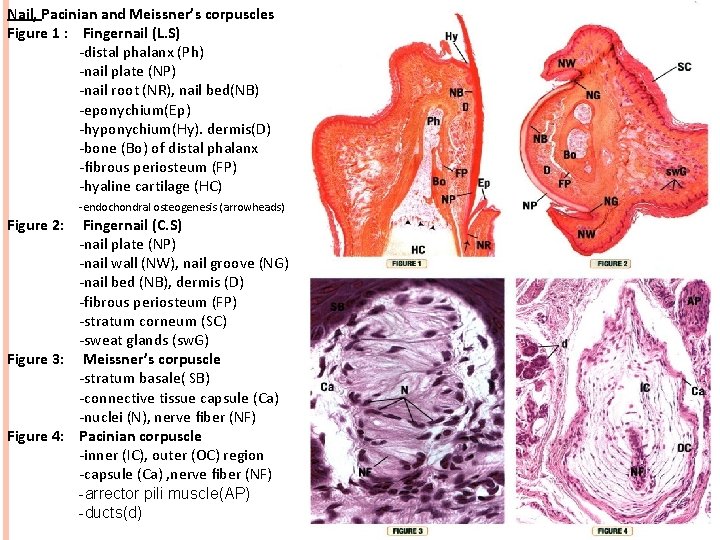
Nail, Pacinian and Meissner’s corpuscles Figure 1 : Fingernail (L. S) -distal phalanx (Ph) -nail plate (NP) -nail root (NR), nail bed(NB) -eponychium(Ep) -hyponychium(Hy). dermis(D) -bone (Bo) of distal phalanx -fibrous periosteum (FP) -hyaline cartilage (HC) -endochondral osteogenesis (arrowheads) Figure 2: Fingernail (C. S) -nail plate (NP) -nail wall (NW), nail groove (NG) -nail bed (NB), dermis (D) -fibrous periosteum (FP) -stratum corneum (SC) -sweat glands (sw. G) Figure 3: Meissner’s corpuscle -stratum basale( SB) -connective tissue capsule (Ca) -nuclei (N), nerve fiber (NF) Figure 4: Pacinian corpuscle -inner (IC), outer (OC) region -capsule (Ca) , nerve fiber (NF) -arrector pili muscle(AP) -ducts(d)
- Slides: 45