Anesthetic Considerations for Chemo Patients Brett Cavanaugh RNAI

Anesthetic Considerations for Chemo Patients Brett Cavanaugh, RNAI Sacred Heart Medical Center/ Gonzaga University 1

Case n n n 47 yo male, 65 kg Surgery: Wide local incision of squamous cell carcinoma of the lower lip History: n n n Atenolol Cisplatin 5 -flurouracil Bleomycin Pre-op n n n HTN Chews tobacco – 30 yrs Medications: n n n VSS: BP 130/88, HR 72, RR 16, Sp. O 2 96% Lungs CTA Heart tones normal Airway: MP 1 , TM 3, MO 3 Labs: CBC & Lytes WNL Chest x-ray, EKG normal Echo: EF 57% 2

Intra-op n Induction: n n n Maintenance: n n n Propofol/Fentanyl/Vecuronium Nasally intubated, atraumatic Isoflurane/N 2 O/Fentanyl/Vecuronium Fi. O 2 <30% Emergence: n n n Reversal with neostigmine/glycopyrrolate Immediately, Pt’s sats decreased to 89% on 100% Fi. O 2 Copious frothy sputum from ETT, bilat rales n n Pulm Edema --Lasix 40 mg IV Sats increased to 95% and Pt was taken to ICU intubated 3

Background n In 2005, cancer was the most common cause of death from disease in the USA, causing over 500, 000 fatalities n At present, 50% are cured of cancer n n Chemotherapy is the best approach to eradication of malignant cells n n Chemotherapy cures 10 -15% Total cell-kill Combination chemotherapy allows the largest possible doses by using different mechanisms, not sharing toxic effects 4

The Cell Cycle n Malignant cells go through normal mitosis, but synthesize DNA and divide at a faster rate n Most chemo drugs exert antineoplastic effects during DNA synthesis (S-phase) or mitosis n n Cell Cycle Specific (CCS) drugs Other chemo drugs sterilize tumor cells whether they are cycling or resting in the Go compartment n Cell Cycle Non-Specific (CCNS) 5

Classification of Chemotherapeutic Agents 6

Antimetabolites n MOA: Inhibition of DNA or RNA synthesis n Methotrexate: Folic acid analog (antagonist) n n n 5 -Fluorouracil: Pyrimidine analog (prodrug) n n n Acute Lymphoblastic Leukemia GI tract, myelosuppression and hepatic dysfunction Breast and GI carcinomas, and skin cancer Ulcerations of GI tract, myelosuppression Mecaptopurine: Purine analog (prodrug) n n Acute leukemia in children GI tract, gradual myelosuppression and jaundice 7

Antitumor Antibiotic Cell-cycle Specific n Bleomycin: Causes fragmentation of DNA n n n Clinical uses: Hodgkin’s and non-Hodgkin’s lymphomas, testicular cancer, and squamous cell carcinoma mucocutaneous reactions, exacerbation of rheumatoid arthritis and pulmonary toxicity Pulmonary Toxicity (PT) n n n 5 -10% develop PT 1 -2% of all patients die from PT Higher risk for ARDS due to free radicals from hyperoxygenation, which destroy alveolar lining Signs/Symptoms: Cough, dyspnea, basilar rales, developing into interstitial pneumonitis and fibrosis. Increased A-a gradient and decreased diffusion capacity Recommendation: Keep Fi. O 2 below 30% 8

Epipodophyllotoxins n Derived from mayapple root extract (podophyllotoxin) n n Etoposide: germ cell cancer, small cell and non-small cell lung cancer, Hodgkin’s/non. Hodgkin’s and gastric cancer n n Blocks cell division by damaging DNA strands, causing breakage alopecia and myelosuppression Tenoposide: acute lymphoblastic leukemia n similar to above 9

Taxanes n Alkaloid esters derived from the Pacific and European yew n n Paclitaxel: broad range of solid tumors and Kaposi’s sarcoma n n Mitotic spindle poison GI, Sensory neuropathy, myelosuppression Doxetaxel: second line therapy in advance or refractory cancer of solid tumors n Neurotoxicity, fluid retention, neutropenia 10
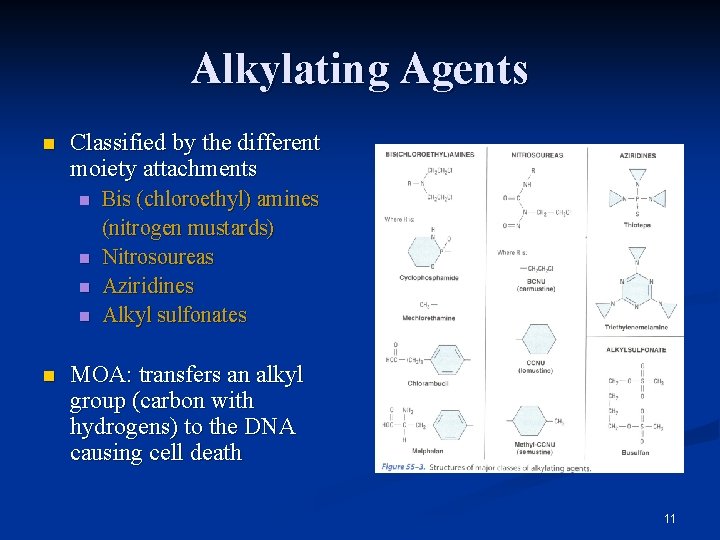
Alkylating Agents n Classified by the different moiety attachments n n n Bis (chloroethyl) amines (nitrogen mustards) Nitrosoureas Aziridines Alkyl sulfonates MOA: transfers an alkyl group (carbon with hydrogens) to the DNA causing cell death 11

Alkylating Agents Nitrogen Mustard n Mechlorethamine: Hodgkin’s disease in combination with other chemo drugs n GI, myelosuppression, herpes zoster Nitrourea n Streptozosin: pancreatic cancer n 70% produce renal or hepatic injury Aziridines n Thiotepa: ovarian/bladder/breast cancer n Myelosuppression Alkylsulfonate n Busulfan: chronic granulocytic leukemia n Myelosuppression with an increase in thrombocytopenia 12

Anthracyclines n Antibiotics isolated from Streptomyces n Not only prevent DNA/RNA replication, but also promote free radicals and cell destruction n Daunorubicin: acute lymphocytic and granulocytic leukemia, and wide range of solid tumors n Doxorubicin: metastatic adenocarcinoma and thyroid carcinoma, bladder and lung cancer. n Side effects: acutely: conduction problems, myocarditis, and pericarditis; chronically: dilated cardiomyopathy and CHF. n Myelosuppression with an increase in neutropenia 13

Antitumor Antibiotics Cell-cycle non-specific n Derived from Streptomyces n n Inhibits DNA/RNA synthesis Dactinomycin: pediatric tumors; Wilms’ tumor (nephroblastoma), rhabdomyosarcoma, Ewing’s sarcoma (rare bone/soft tissue tumor) n n GI, alopecia and myelosuppression Mitomycin: squamous cell cancers n Myelosuppression 14

Platinum Analogs n Inorganic metal complex n n Cisplatin: broad range of solid tumors n n Thought to have cytotoxic effects similar to alkylating agents Nephrotoxicity, ototoxicity, peripheral sensory neuropthy Carboplatin (second generation): Same spectrum as cisplatin n Less nephrotoxic, myelosuppression 15

Conclusion n There a variety of chemotherapeutic drugs targeted either at CCS or CCNS n Wide range of toxicities n Evaluate CBC, lytes, renal function, and ECG n Doxo/Daunorubicin = cardiotoxicity n Bleomycin = pulmonary toxicity n Cisplatin = Nephrotoxic n Wise Words: “When in doubt, Palm it out” - B. Engel, CRNA 16

Bibliography n n Katsung, B. Basic and Clinical Pharmacology. 2007, 10 th Ed. Pp 878 -898. Stoelting, R. Pharmacology and Physiology in Anesthetic Practice. 1987, 2 nd Ed. Pp 504 -520. Mathes, D. Bleomycin and Hyperoxia Exposure in the Operating Room, Anesthesia and Analgesia, 1995; 81: 624 -629. S. Prakash, H. Suri, G. Usha & A. R. Gogia : Bleomycin Induced Pulmonary Toxicity: A Case Report. The Internet Journal of Anesthesiology. 2008; 16: 1 17
- Slides: 17