Anesthesia in Electrophysiology 2016 Mark S Weiss MD


















- Slides: 27

Anesthesia in Electrophysiology © 2016 Mark S Weiss, MD Department of Anesthesiology and Critical Care

Goals of an EP lab w Diagnostic • Conduction studies / Arrhythmia induction • Device interrogation w Therapeutic • Tachyarrhythmia treatment • Ablation • Device implantation 2

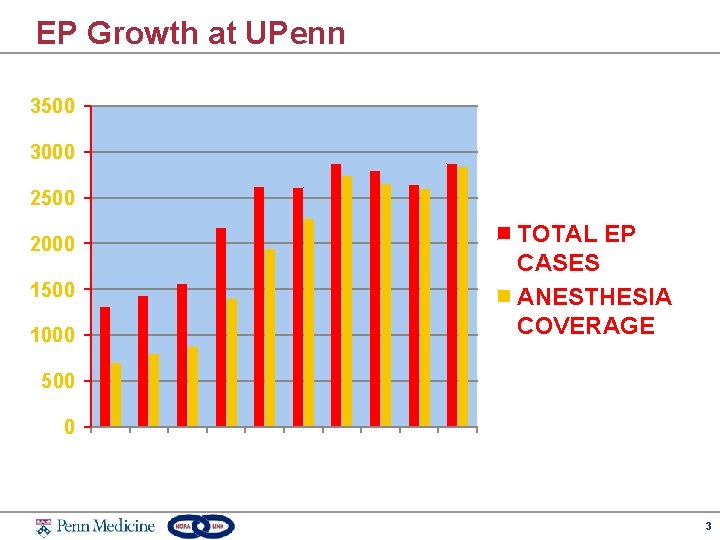
EP Growth at UPenn 3500 3000 2500 2000 1500 1000 TOTAL EP CASES ANESTHESIA COVERAGE 500 0 3

Communication disconnect Anesthesia’s view Control Room’s view 4

Preoperative Evaluation w Airway • challenges can be amplified in NORA environments w Allergies • Shellfish -> Contrast Dye • Fish -> Protamine • Antibiotics -> surgical site infection prevention protocols w Cardiac • Ejection Fraction – selecting pressor agents/anesthetic agents • Congestive heart failure – tolerance of supine position • Pulmonary HTN – sedation induced hypercarbia and hypoxia w Pulmonary • OSA/Morbid obesity - requirement for CPAP w Gastrointestinal • GERD – increased importance with sedation 5

Preanesthetic Preparation w w w w Machine –positive pressure ventilation Suction – sometimes shared with proceduralist Monitors – basic ASA and others as needed Airway IV –Sedation and TIVA common Drugs – resuscitation drugs Special equipment – jet ventilator, esophageal temperature probes, warming/cooling devices 6

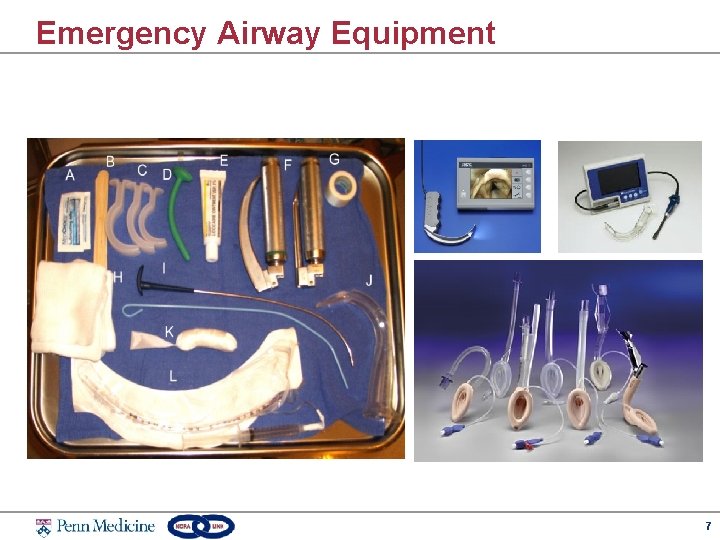
Emergency Airway Equipment 7

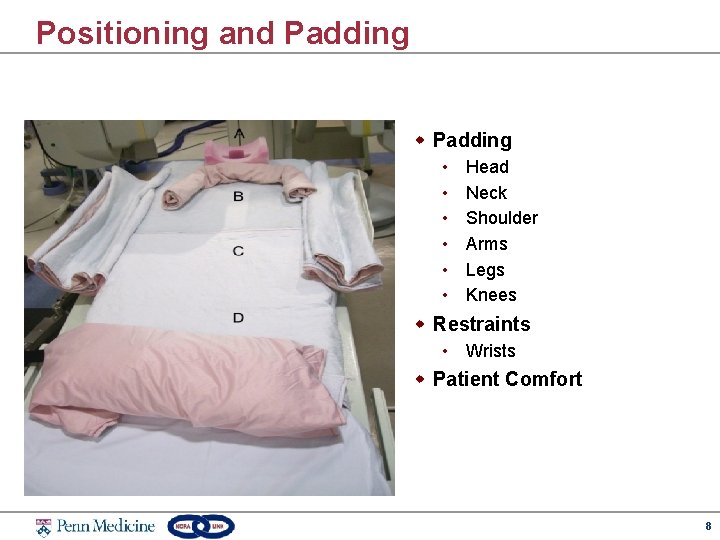
Positioning and Padding w Padding • • • Head Neck Shoulder Arms Legs Knees w Restraints • Wrists w Patient Comfort 8

Continuum of sedation Mild Sedation Moderate Deep Anesthesia (General) Procedure Length Cardioversion (CVN) 15 minutes Noninvasive Programmed Stimulation (NIPS) 30 minutes Defibrillator Threshold testing (DFT) 15 minutes Pacemaker +/- Generator Change 1 -6 hours Lead extraction +/- Laser 3 -6 hours SVT/WPW radiofrequency ablation 2 -4 hours AFib radiofrequency ablation 6 -12 hours Ventricular radiofrequency ablation 6 -12 hours 9

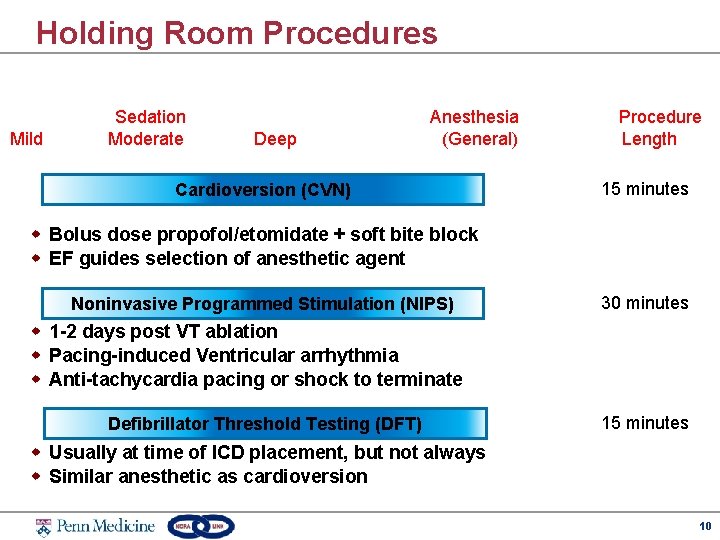
Holding Room Procedures Mild Sedation Moderate Deep Anesthesia (General) Cardioversion (CVN) Procedure Length 15 minutes w Bolus dose propofol/etomidate + soft bite block w EF guides selection of anesthetic agent Noninvasive Programmed Stimulation (NIPS) 30 minutes w 1 -2 days post VT ablation w Pacing-induced Ventricular arrhythmia w Anti-tachycardia pacing or shock to terminate Defibrillator Threshold Testing (DFT) 15 minutes w Usually at time of ICD placement, but not always w Similar anesthetic as cardioversion 10

Device Placement Mild Sedation Moderate Deep Anesthesia (General) Pacemaker +/- Generator Change Procedure Length 1 -6 hours w Device Placement – Pectoral vs. Subcutaneous • Symptomatic Bradycardia: Pacemaker • Tachyarrhythmia: ICD • Cardiac resynchronization therapy (CRT): Bi. V-ICD w Generator Change • Shorter procedure • May require DFT 11

Device Removal Mild Sedation Moderate Deep Anesthesia (General) Lead extraction +/- Laser Procedure Length 3 -6 hours w Indications • System infection • Lead malfunction (fracture/failure/erosion) w Considerations • Leads > 1 year old can have adhesions – May lead to cardiac/vascular avulsion or injury • Blood / Rapid infuser availability • Cardiac surgery backup • May have to be done in main OR 12

Radiofrequency ablation (RFA) Mild Sedation Moderate Deep Anesthesia (General) Procedure Length SVT/WPW radiofrequency ablation 2 -4 hours AFib radiofrequency ablation 6 -12 hours Ventricular radiofrequency ablation 6 -12 hours 13

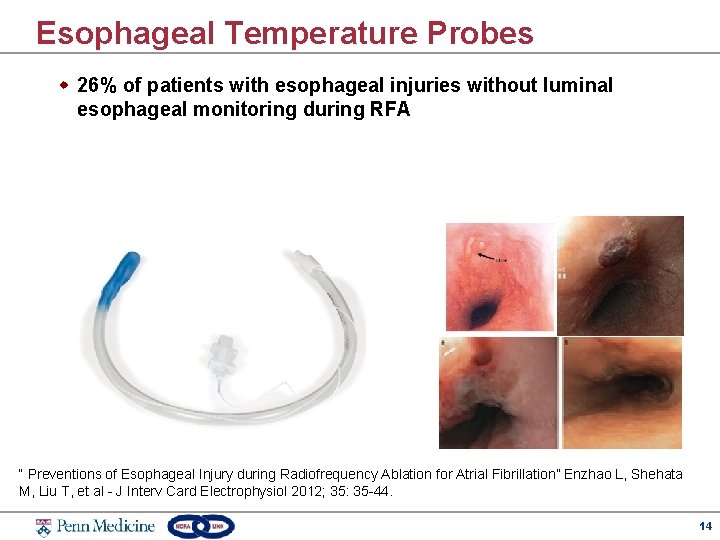
Esophageal Temperature Probes w 26% of patients with esophageal injuries without luminal esophageal monitoring during RFA “ Preventions of Esophageal Injury during Radiofrequency Ablation for Atrial Fibrillation” Enzhao L, Shehata M, Liu T, et al - J Interv Card Electrophysiol 2012; 35: 35 -44. 14

High Frequency Jet Ventilation (HFJV) w Increases efficiency/efficacy by decreasing respiratory motion artifacts w Requires GA with ETT and TIVA 15

SVT and Afib ablation Mild Sedation Moderate Deep Anesthesia (General) SVT/WPW radiofrequency ablation Procedure Length 2 -4 hours w Deep sedation suppresses autonomic system w Light sedation (remi) +/- short acting bolus (propofol) w Avoid long-acting sedatives like benzodiazepines AFib radiofrequency ablation 6 -12 hours w GETA + Arterial line + foley catheter w Consider HFJV 16

PVC and Vfib ablation Mild Sedation Moderate Deep Anesthesia (General) Ventricular radiofrequency ablation w w w Procedure Length 6 -12 hours Deep sedation suppresses autonomic system Usually have low EF ( < 10%) Light narcotic sedation used (remifentanil infusion) Mental status during V-tach assesses need for defibrillation If GETA, cerebral oximetry used to guide decision 17

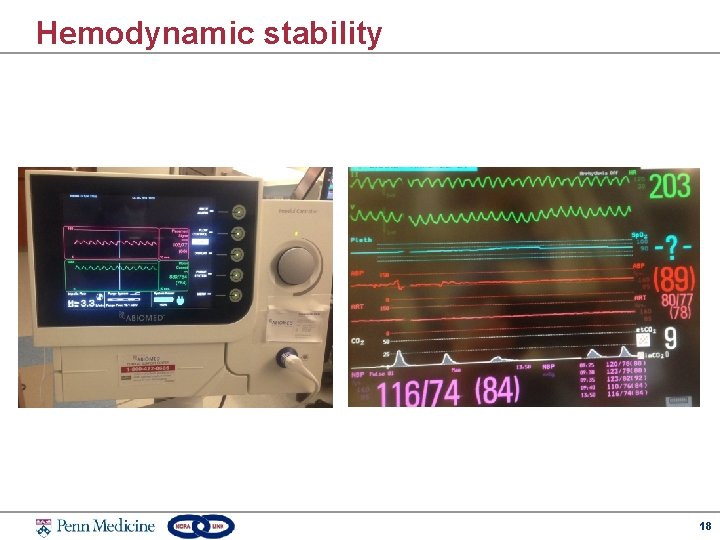
Hemodynamic stability 18

Isoproterenol (Isuprel) w Basic concepts • • • Nonspecific beta agonist Positive chronotropic, dromotropic, and inotropic effects Used to induce ventricular arrhythmias Beta 2 -mediated hypotension Can cause an increase in the MAC requirement 19

Isoproterenol challenge w Requires invasive blood pressure monitoring w Increased MAC requirement • If under GETA: – Remi > 0. 15 mcg/kg/min and propofol > 80 mcg/kg/min – Or as required by patient w Ensure adequate IV flow rate w Keep SBP > 140 prior to isoproterenol challenge • Provides buffer for isoproterenol-induced hypotension w Listen for subtle heart rate increase • Pre-emptive management is key • Increase phenylephrine ; high individual variability, but increase by 50100 mcg/kg/min 20

Isoproterenol challenge - cont w Isoproterenol challenge doses • 6 -> 12 -> 20 -> 30 -> 40 mcg/min w Decrease systolic goals at higher isoproterenol doses • SBP 110 -120 for isoproterenol doses 20 -40 mcg/min • Isoproterenol metabolized faster than phenylephrine and abrupt challenge end can lead to rebound hypertensive crisis w At end of isoproterenol challenge • Stop phenylephrine infusion • Return IV flow rate to initial settings • As blood pressure decreases, restart phenylephrine. at pre-challenge rates 21

Isoproterenol challenge - sedation w Patient may not be able to tolerate GETA • “too sick” w Isoproterenol challenge doses • 3 - 12 mcg/min w Less hypotension • Can usually react to change as opposed to pre-empt • Moderation in reaction to changes w Consider Epinephrine infusions • Pt may have Low EF 22

Hemodynamic changes w Infusions: • phenylephrine • epinephrine w Volume status: • Ablation catheter can deliver >3 L of fluid • The patient may require diuresis w Labile hemodynamics • May be due to the electrophysiologist • Communication is key 23

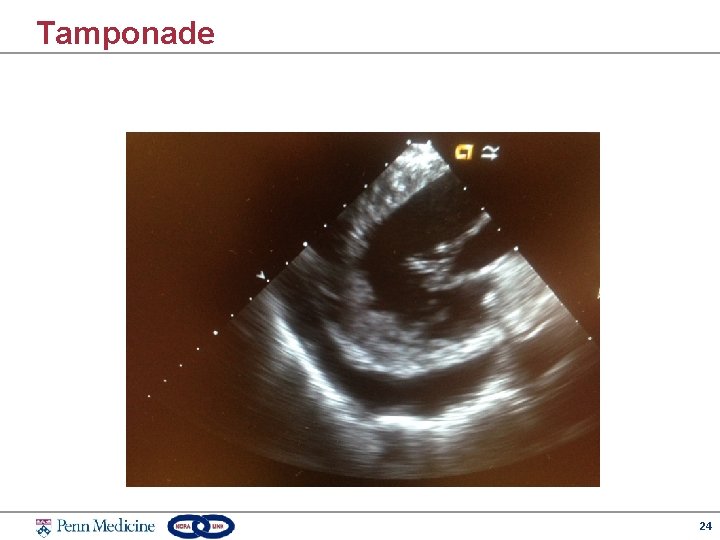
Tamponade 24

Postoperative Pain management w Pain generators • Back pain/Extremity pain for laying supine for prolonged period • Foley catheter • Intravascular Catheters in groin, need to hold pressure w Typical Pain medications: • Ketorolac typically given (avoid in renal impairment) • Morphine/Dilaudid to be considered w Ondansetron for PONV 25

Tips for success w Communication w Understanding procedures and their effects on hemodynamics as much as possible w Preparation and ensuring proper positioning, line set up w Comfort in a NORA setting 26

27