Anesthesia for Post Tonsillectomy and Adenoidectomy Hemorrhage Robin

Anesthesia for Post. Tonsillectomy and Adenoidectomy Hemorrhage Robin G. Cox, MBBS, MRCP(UK), FRCA, FRCPC Professor of Anesthesiology University of Calgary Alberta Canada Updated 4/2017

Disclosure • No conflicts of interest to declare

Objectives To describe the epidemiology of posttonsillectomy and adenoidectomy hemorrhage in children To discuss the causes of post-tonsillectomy and adenoidectomy hemorrhage in children To formulate a plan for anesthesia management of the child with a post-tonsillectomy and adenoidectomy hemorrhage: Preoperative assessment and optimization Intraoperative management Postoperative management

Epidemiology of Post-Tonsillectomy Hemorrhage in Children • National Prospective Tonsillectomy Audit • 277 UK hospitals • 33, 921 patients undergoing tonsillectomy • 21, 060 were < 16 years of age • Overall hemorrhage rate 3. 5 %: • Primary (< 24 hrs postoperatively) • Secondary (> 24 hrs postoperatively) • Both • Return to O. R. in 0. 93 % (Lowe, Laryngoscope 2007) 0. 55 % 3. 0 % 0. 07 %

Epidemiology of Post. Adenoidectomy Hemorrhage • Surgical Instrument Surveillance Programme (Wales) • 5, 588 patients undergoing adenoidectomy: • 4, 225 with tonsillectomy (median age 6. 1 yr) • 1, 363 sole procedure (median age 6. 3 yr) • Return to O. R. for adenoid bleeding in 22 (0. 4 %) • All cases of adenoid bleeding occurred within 24 hrs, unlike tonsillectomy, which more often presents with secondary hemorrhage (Tomkinson, Laryngoscope 2012)

Mortality after Tonsillectomy and Adenoidectomy • Mortality fortunately rare, but it still occurs: • 1: 7, 000 – 1: 170, 000 • 32 deaths reviewed (31 tonsil; 1 adenoid) • Mortality more common in secondary hemorrhage • Aberrant course of internal carotid artery a rare factor • Deaths commonly related to airway obstruction and aspiration of blood • Rigid instruments for endoscopy and suction may have prevented death in some of these patients (Windfuhr, ORL 2013 & Otolaryngol Head Neck Surg 2009)

Aberrant Internal Carotid Artery - risk of 1° Hemorrhage Straight Curved Kinked May be close to tonsil bed (Paulsen, J Anat 2000) Coiled

Risk Factors for Hemorrhage • Older aged patients • In some studies: • • • Males Recurrent tonsillitis and peritonsillar abscess Inadequate hemostasis (primary) Excessive use of electrosurgery/coblation (secondary) Use of NSAIDs • Underlying coagulopathy is a very rare cause • Use of Dexamethasone is NOT a risk factor (Tomkinson, Sarny, Laryngoscope 2011; Mowatt, Clin Otolaryng 2006; Baugh, Otolaryngol Head Neck Surg 2010; Geva, Otolaryngol Head Neck Surg 2011)

Risk Factors for Hemorrhage: Effect of Age • Tonsillectomy or adenotonsillectomy most commonly performed in first decade of life • Patients ≥ 12 years of age are 1. 5 times more likely to experience early postoperative hemorrhage requiring surgery than those < 12 years of age • Patients ≥ 12 years of age are 3. 3 times more likely to experience late postoperative hemorrhage requiring surgery than those < 12 years of age (Tomkinson, Laryngoscope 2011)

Risk Factors for Hemorrhage: Effect of NSAIDs Ketorolac RCT 1996 INCREASED RISK Systematic Review 2003 AMBIGUOUS Meta-analysis 2003 INCREASED RISK Cochrane Review 2005 NO INCREASED RISK (Splinter, Can J Anes 1996; Møiniche, Anesth Analg 2003; Marret, Anesthesiology 2003; Cardwell, Cochrane Collaboration 2005)

Methods to Reduce Risk • Effective methods: • Screening for bleeding disorders in the history • Surgical technique avoiding excessive cautery • Avoiding surgery on acutely inflamed tonsils • Ineffective: • Routine preoperative screening for coagulopathy • Routine use of antibiotics (Lowe, Laryngoscope 2007)

Methods to Reduce Risk: Role of Tranexamic Acid? • Tranexamic Acid (TXA), a fibrinolytic agent, has been shown effective in reducing blood loss in cardiac and orthopedic surgery. • Systematic review and meta-analysis suggests that TXA may reduce the amount of blood loss during tonsillectomy, but not the incidence of postoperative hemorrhage. • Larger, more rigorous, studies are required to evaluate the possible role of TXA in the prevention of postoperative hemorrhage. (Robb, J Laryngol Otol 2014)

Management of Post. Tonsillectomy Hemorrhage • Non-operative (73%): • Observation • Packs, epinephrine, cautery (in older cooperative children) • Operative (27%): • Cautery • Ligation of bleeding points • Rarely more invasive measures (embolization, ligation of external carotid artery) (Lowe, Laryngoscope 2007)

Post-Tonsillectomy Hemorrhage Preoperative Management • Assessment: • Must be a rapid evaluation, combined with resuscitation as required • Remember routine preoperative questions • Review clinical course following surgery, estimate degree of bleeding (however blood loss may be hidden) • Review anesthesia record of tonsillectomy, including postoperative medications • Focus on airway, vital signs and cardiovascular status

Preoperative Management • Initial Resuscitation: • Apply oxygen and obtain intravenous access • Bolus with Normal Saline or Ringers Lactate – 10 ml/kg repeated as required • Send blood for CBC, coagulation studies, and blood typing and screen, crossmatch as required • [Hb] may not be reliable in assessing degree of hemorrhage • Transfuse for [Hb] < 70 - 80 g/L • In major hemorrhage, order FFP and platelets; consider tranexamic acid

Preoperative Management • Continuing Resuscitation: • Evaluate response to fluid bolus • Vital signs • Capillary refill • Mental status • Remember that surgical control of the bleeding is part of the resuscitation • It may not be possible to achieve perfect vital signs before induction of anesthesia

Intraoperative Management: Induction • Airway – could it be difficult? • Hemodynamic State – hypovolemia, overt or hidden? • Full Stomach – must be assumed… • Previous Sedation – particularly if anesthesia that day

A Safe Method of Induction • Adequate assistance and surgeon in the O. R. • Two suction devices to hand turned on to maximum (Yankauer) • Rapid sequence induction with preoxygenation and cricoid pressure • Induction agent: • Choice of agent and dose according to hemodynamic status – always assume there is major blood loss • Muscle relaxant: • Succinylcholine unless contraindicated

A Safe Method of Induction • As soon as succinylcholine takes effect, perform direct laryngoscopy, suction pharynx, and intubate with oral RAE tube. Glide. Scope as backup, if available • Consider cuffed tube • Suction ETT if any possibility of tracheal aspiration of blood • Recheck vital signs and continue volume loading as required • Allow the surgeon to proceed as soon as possible

Induction Methods • 475 children who underwent surgery for posttonsillectomy hemorrhage were retrospectively reviewed • Induction types were: • • • 84. 4% RSI 5. 5% modified RSI 3. 2% mask inhalation 0. 2% tracheostomy 6. 1% unspecified (Fields, Pediatric Anesthesia 2010)

Induction Methods • Muscle relaxants used were: • 88% succinylcholine • 8% nondepolarizing muscle relaxant • 3% no muscle relaxant, or unrecorded • Atropine was used in 21. 9% (atropine or glycopyrrolate) • Cricoid pressure recorded in 90% • Only 2/475 patients encountered a difficult intubation, requiring a second attempt. (Fields, Pediatric Anesthesia 2010)
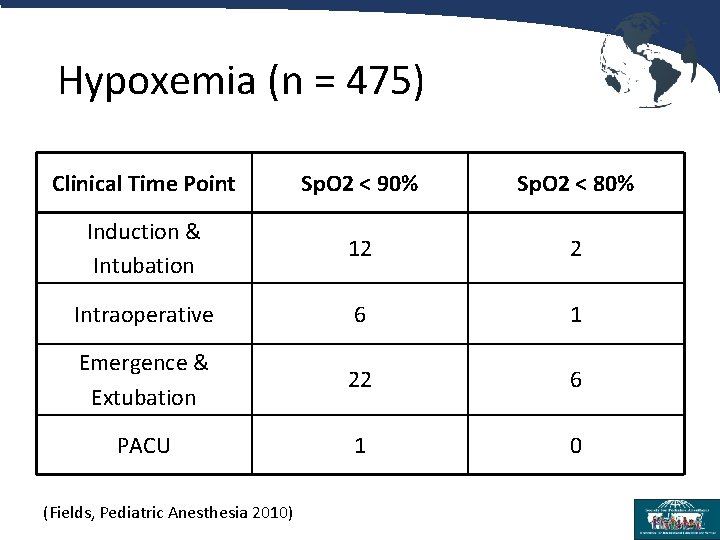
Hypoxemia (n = 475) Clinical Time Point Sp. O 2 < 90% Sp. O 2 < 80% Induction & Intubation 12 2 Intraoperative 6 1 Emergence & Extubation 22 6 PACU 1 0 (Fields, Pediatric Anesthesia 2010)

Anesthetic Technique (cont. ) • Continuing resuscitation with fluid/blood products • Coagulopathies are rare unless massive transfusion • Caution with volatile agents (hypovolemia) • Opiate dose reduced, particularly in primary hemorrhage – may have opiates on board • Empty stomach with large-bore tube under direct vision • Antiemetics - Dexamethasone/Ondansetron • Awake extubation

Recovery Period • Close monitoring for recurrent bleeding, hemodynamic instability, airway obstruction • Repeat hematology/coagulation studies as required • Caution with sedative agents • Surgeons may consider antibiotics in secondary hemorrhage

Special Situations: Induction if MH Susceptible • Can proceed with RSI using large dose of rocuronium (1. 2 mg/kg) • Consider remifentanil (1 -2 µg/kg) as an alternative to rocuronium, but be prepared to treat bradycardia • Ketamine, nitrous oxide both safe • Maintain with TIVA • Extubate awake

Special Situations: Previously Difficult Airway • E. G. Pierre-Robin Sequence • Although spontaneous ventilation may be preferred until the airway is secure, the classic inhalational induction, in the head down lateral position, still carries the risks of aspiration and hypotension • Glide. Scope may be very effective and provide a better view than fiberoptic techniques (blood) • Surgeon skilled at rigid bronchoscopy and surgical airways immediately available

Conclusions • Prevention includes evaluating for bleeding diathesis by history and investigation if indicated, avoidance of excessive use of cautery/coblation, and avoiding operating on acutely inflamed tonsils • Perioperative management is focused on timely resuscitation, an anesthetic technique that captures the airway rapidly, continued resuscitation, and very close postoperative monitoring • With this approach, morbidity and mortality should be very rare

References 1. Lowe D, van der Meulen J, Cromwell D, Lewsey J, Copley L, Browne J, Yung M, Brown P. Key messages from the National Prospective Tonsillectomy Audit. Laryngoscope 2007; 117: 717 -24. 2. Tomkinson A, Harrison W, Owens D, Fishpool S, Temple M. Postoperative hemorrhage following adenoidectomy. Laryngoscope 2012; 122: 1246 -53. 3. Windfuhr JP. Serious complications following tonsillectomy: how frequent are they really? ORL 2013; 75: 166 -73. 4. Windfuhr JP, Schloendorff G, Sesterhenn AM, Prescher A, Kremer B. A devastating outcome after adenoidectomy and tonsillectomy: ideas for improved prevention and management. Otolaryngol Head Neck Surg 2009; 140: 191 -6.

References 5. Paulsen F. Curving and looping of the internal carotid artery in relation to the pharynx: frequency, embryology and clinical implications. J Anat 2000; 197: 373 -81. 6. Mowatt G, Cook JA, Fraser C, Mc. Kerrow WS, Burr JM. Systematic review of the safety of electrosurgery for tonsillectomy. Clin Otolaryngol 2006; 31: 95 -102. 7. Tomkinson A, Harrison W, Owens D, Harris S, Mc. Clure V, Temple M. Risk factors for postoperative hemorrhage following tonsillectomy. Laryngoscope 2011; 121: 279 -88. 8. Sarny S, Ossimitz G, Habermann W, Stammberger H. Hemorrhage following tonsil surgery: a multicenter prospective study. Laryngoscope 2011; 121: 2553 -60.

References 9. Baugh RF et al, American Academy of Otolaryngology. Head and Neck Surgery Foundation. Clinical practice guideline: tonsillectomy in children. Otolaryngol Head Neck Surg 2011; 144 (1 Suppl): S 1 -30. 10. Geva A, Brigger MT. Dexamethasone and Tonsillectomy Bleeding: a meta-analysis. Otolaryngol Head Neck Surg 2011; 144: 838 -43. 11. Splinter WM, Rhine EJ, Roberts DW, Reid CW, Mac. Neill HB. Preoperative ketorolac increases bleeding after tonsillectomy in children. Can J Anaesth 1996; 43: 560 -3. 12. Møiniche S, Rømsing J, Dahl JB, Tramèr MR. Nonsteroidal antiinflammatory drugs and the risk of operative site bleeding after tonsillectomy: a quantitative systematic review. Anesth Analg 2003; 96: 68 -77.

References 13. Marret E, Flahault A, Samama CM, Bonnet F. Effects of postoperative, nonsteroidal, antiinflammatory drugs on bleeding risk after tonsillectomy: meta-analysis of randomized, controlled trials. Anesthesiology 2003; 98: 1497 -502. 14. Cardwell M, Siviter G, Smith A. Non-steroidal antiinflammatory drugs and perioperative bleeding in paediatric tonsillectomy. Cochrane Database Syst Rev 2005 Apr 18; (2): CD 003591. 15. Robb PJ. Tranexamic Acid – a useful drug in ENT surgery? J Laryngol Otol 2014; 128: 574 -9. 16. Fields RG, Gencorelli FJ, Litman RS. Anesthetic management of the pediatric bleeding tonsil. Pediatr Anaesth 201 o; 11: 982 -6.
- Slides: 31