Andropause Hormone Balance for Men Rebecca L Glaser

Andropause Hormone Balance for Men Rebecca L. Glaser M. D. , FACS

Andropause n n n Testosterone levels begin to decline in some men as early as 35 years of age, typically age 50 Gradual onset Deterioration of the mental and physical condition Testosterone therapy has been used for over 60 years Diet and lifestyle are extremely important to hormone balance Every person is a unique individual

Testosterone Anabolic hormone that improves muscle mass and bone density n Improves mental sharpness, concentration, and memory n Increases energy level n Improves flexibility and mobility n Prevents aches and pains n Increases sex drive and libido n

Testosterone (cont. ) Normal levels are protective against Alzheimer’s dementia, Parkinson’s disease, & cognitive decline n Protects against diabetes n Protects against abdominal obesity n Antidepressant n Protects against bone loss n Prevents inflammatory conditions n

Testosterone and the Heart Muscle building hormone n A low testosterone is a risk factor for CHF n Prevents CAD (heart disease) n Dilates coronary arteries n Helps maintain healthy cholesterol levels n As testosterone declines BP rises n

Testosterone n Does not cause prostate cancer n n n Low testosterone levels correlate with more aggressive disease and worse outcomes May stimulate an undiagnosed cancer Does not cause liver failure n (17α) Methyltestosterone (synthetic) n n n Orally effective Hepatotoxic, jaundice, cysts, hepatocellular adenomas Increased LDL, suppressed HDL, Increased risk HD Moralis 01: Algarte-Genin 04: Imamoto 04: Gooren 04: Slater 00

DHEA ( dehydroepiandrosterone) Precursor hormone for both testosterone and the estrogens n Low levels have been associated with depression, autoimmune diseases, and other chronic diseases (heart disease & diabetes) n Low levels and high levels have been associated with breast cancer n

Estradiol/Testosterone is converted to estradiol (estrone) by aromatase (enzyme) n As men age the ratio of estradiol to testosterone increases n Elevated estradiol/testosterone increases the risk of BPH and prostate cancer n It is not only the decline in testosterone but also the increase in estradiol that cause the symptoms of Andropause n

Symptoms of Andropause Mental fatigue, feeling burned out, inability to concentrate, insomnia n Decreased mental sharpness n Increased forgetfulness n Depression, irritability, anger, anxiety n Physical fatigue, tiredness in the afternoon n Aches, joint and muscle pain n Decreased muscle mass n

Symptoms of Andropause n n n n cont. Shortness of breath with activities Development of chest pain, dx. of heart disease, blockage of arteries, rising BP Swelling of ankles, varicose veins Lightheadedness, dizzy spells Increased sweating, hot flashes Rising blood sugar, worsening diabetes Incontinence Erectile dysfunction and decreased libido

Factors that Contribute to Testosterone Deficiency Mumps n Alcohol, stress, obesity n Drugs that affect the liver n NSAIDs (ibuprofen), Tylenol, ASA n Statins (cholesterol lowering drugs) n Many heart and BP medications n Antidepressants n H 2 blockers n Chemotherapy n

Raise Testosterone Naturally Exercise, weight loss, eliminating processed foods (lowers insulin levels), reducing stress, and limiting alcohol will raise testosterone levels n Fruits, vegetables, nuts, seeds, and fiber will offer protection to the prostate gland n

Supplements Raise testosterone and protect prostate n n n n n Zinc 25 -50 mg, Vitamin C (1000 mg) Chrysin (with piperine), flavones, Rx. arimidex Saw Palmetto 350 mg, Nettle Root Vitamin E (400 mg), B Complex (folate, B 6, B 12) Magnesium 500 mg Omega 3 Fatty Acids (flaxseed, fish oil) Whole soy foods 2 -3 times weekly Pygeum, pumpkin seed, lycopene I 3 C (Indole-3 -carbinol) www. hormonebalance. org …Topics…Prostate Protection

Progesterone Levels decline after 60 n Protects the prostate gland lowers PSA n Inhibits aromatase and 5 alpha reductase, raising testosterone levels n Antagonizes the stimulatory effect of estrogen on the prostate gland n Stimulates p 53 (antitumor antigen) n

Hormone Testing n Saliva, Urine, Blood n www. hormonebalance. org n Featured reference sites n n Hormone Testing Bio-available (free) testosterone Saliva n 24 hour Urine n Free testosterone in blood (vs. total Testosterone) n

Testing n n Saliva: Profile I (estradiol, DHEA-S, progesterone, testosterone, and cortisol) 24 hour Urine Blood : Testosterone , free testosterone (non-SHBG bound), estradiol, estrone, and PSA Blood : Thyroid Panel (T 4, free T 3, TSH), IGF-1 ZRT laboratory www. salivatest. com 503 -466 -2445 Rhein Consulting (Urine Testing) www. rheinlabs. com 503 -292 -1988

Options for HRT n Testosterone (bio-identical) n n n Oral capsule (40 -120 mg) Sublingual tablet or lozenge (5 -10 mg) TDD (Patch 5 mg-10 mg) Skin Cream/Gel (Patented 50 -100 mg/5 gm) (Compounded 20 -100 mg/gm) Injections (T cypionate 100 -200 mg IM) Pellets (four 200 mg. /4 -6 months) DHEA 25 -50 mg/day n Progesterone (5 -10 mg/d) n men

Oral Testosterone n n Testosterone is absorbed well from the gut but is metabolized and inactivated in the liver ‘Micronized in oil’ shifts the absorption to the lymphatics and thus to the systemic circulation via the thoracic duct to the subclavian vein Testosterone undecanoate (esterified) also attempts to shift absorption to the lymphatics Alkylated testosterones (methyltestosterone) are metabolized more slowly but cause problems with lipid metabolism and liver toxicity

Sublingual Testosterone Lozenge/Tablet n n n Avoids intestinal absorption and hepatic inactivation Dose is 5 -10 mg. three times daily Serum levels peak in 30 minutes and return to baseline in 4 -6 hours n n Increase in serum estradiol and DHT Patented 30 mg buccal mucoadhesive system applied twice daily Avoid swallowing saliva Variability in absorption

Transdermal Testosterone (TDD) Patches n Patented Products 1990’s Testoderm scrotal patch (4 to 6 mg/d), rapid absorption, applied daily, elevated DHT n Andropatch Applied daily n Androderm Applied daily, rotating sites, delivers 5 mg T/d n n Alcohol base to enhance absorption n n Skin irritation (50%) or contact dermatitis (12%) Problems with hair and sweating

Percutaneous Testosterone Creams and Gels n Base Natural Cream n Non alcoholic gel n Hydro-alcoholic gel (9 -14% bioavailable) n Andro. Gel, Testim, Testogel n Dose 50 -100 mg (delivers 5 -10 mg of Testosterone) n Can combine testosterone with progesterone 5 -10 mg n Apply cream/gel to inner arms, abdomen, chest, neck n Rotate sites, rub vigorously, wash hands if handling infant n Variability in absorption n Swerdloff 00: Wang 01: Mc. Nicholas 03: Gooren 04: Ebert 05: Meikle 04: Rolf 02: Nieschlag 04:

Testosterone Injections n n n Widely used in Europe, low cost, consistent absorption Well tolerated, intramuscular injection Esterification of the 17β –hydroxyl group n n Lipid soluble Depot Hydrolyzed in vivo to release Testosterone Long acting esters n n n Testosterone Cypionate (every 2 weeks, weekly) Testosterone Propionate (every 2 weeks) Testosterone Undecanoate (every 12 weeks)

Testosterone Pellets n n n n Have been used since 1940 Implanted in the subcutaneous tissue of the lower abdominal wall Requires a minor procedure 3 -6 200 mg pellets provide a physiologic dose of testosterone for 4 -6 months Effective form of therapy with complete bioavailability No elevation of DHT or estradiol Transient accelerated release rate 1 -2 d only Extrusion 5%, minor bleeding 2%, infection <1%

Compounding Pharmacy Oral Capsules n Sublingual lozenges or tablets n Creams and Gels n Pellets n Injectable testosterone esters n n www. hormonebalance. org n n Topics…Compounding Pharmacies Featured Reference Sites…Find a compounding pharmacy
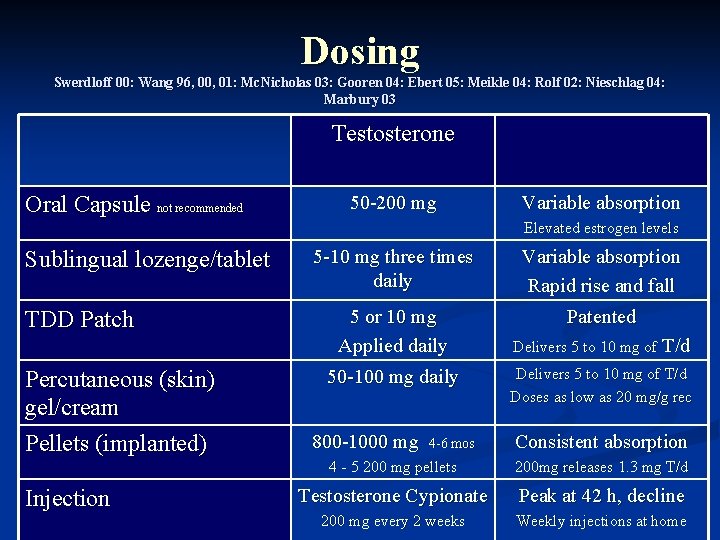
Dosing Swerdloff 00: Wang 96, 00, 01: Mc. Nicholas 03: Gooren 04: Ebert 05: Meikle 04: Rolf 02: Nieschlag 04: Marbury 03 Testosterone Oral Capsule not recommended Sublingual lozenge/tablet TDD Patch Percutaneous (skin) gel/cream Pellets (implanted) Injection 50 -200 mg Variable absorption Elevated estrogen levels 5 -10 mg three times daily Variable absorption Rapid rise and fall 5 or 10 mg Applied daily Patented 50 -100 mg daily 800 -1000 mg 4 -6 mos Delivers 5 to 10 mg of T/d Doses as low as 20 mg/g rec Consistent absorption 4 - 5 200 mg pellets 200 mg releases 1. 3 mg T/d Testosterone Cypionate Peak at 42 h, decline 200 mg every 2 weeks Weekly injections at home

Cost Patented Androgel $235. 00/mo. n USP Testosterone Gel $30. 00 -$45. 00/mo. n USP Testosterone SL lozenge (5 -10 mg. ) two or three times daily $30. 00 -$45. 00/mo. n Pellets 200 mg pellets implanted/6 mos $365 n n Injection $30 twice monthly or at home

BHRT and the Prostate PSA (<2. 6) & digital rectal exam prior to starting therapy n PSA at 3, 6, and 12 mos. following initiation of testosterone therapy n If PSA > 4. 0 prostate biopsy n FU estradiol, estrone, free testosterone, and testosterone levels at 3 months n Testosterone does not cause prostate cancer but may stimulate an existing cancer n

Conclusion n BALANCE n Individual n Levels n Biologically Identical Hormones n Disease Prevention n Active Participant

Recommended Reading www. lef. org Testosterone Protocol n www. salivatest. com n The Testosterone Syndrome Shippen/Fryer n The Hormone Solution Thierry Hertoghe n Adrenal Fatigue James Wilson n The Miracle of Natural Hormones Brownstein n
- Slides: 29