AND ITS MANAGEMENT DR ASIFA SIRAJ CONSULTANT GYNAEOBG

AND ITS MANAGEMENT DR ASIFA SIRAJ CONSULTANT GYNAE/OBG MH RAWALPINDI
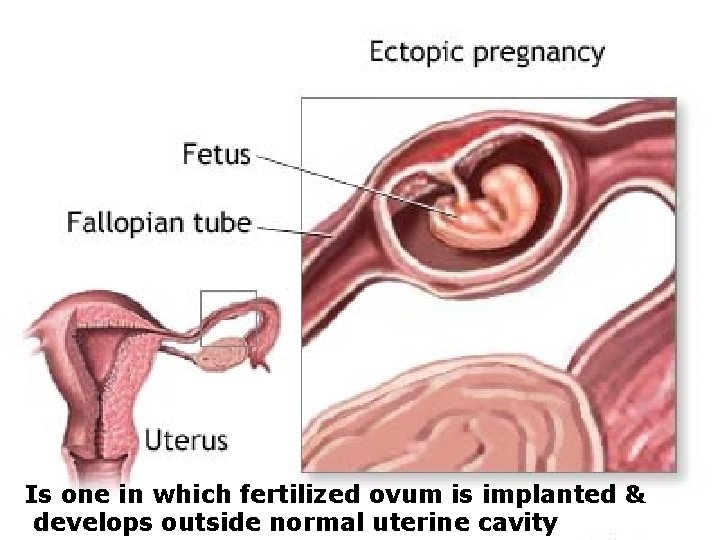
Is one in which fertilized ovum is implanted & develops outside normal uterine cavity

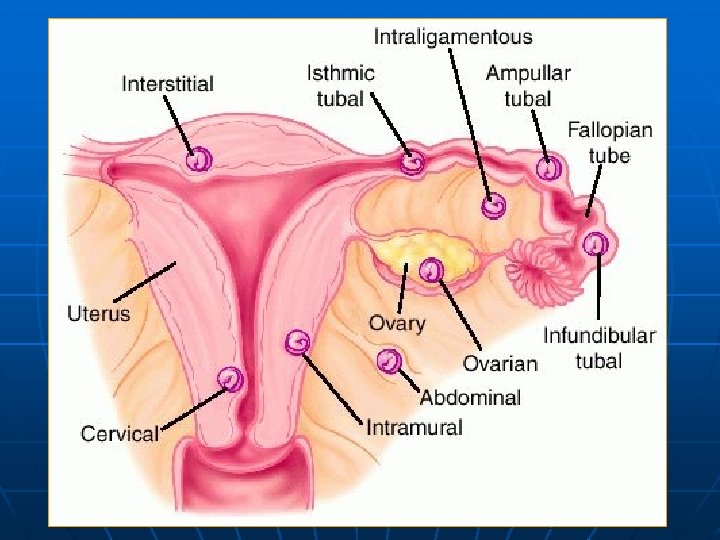
IMPLANTATIONS SITES EXTRAUTERINE TUBAL 97% OVARIAN (1: 40, 000) -Ampulla 80% -Isthmus 12% -Infundibulum 6% -Interstitial 2% UTERINE -CERVICAL (1: 18, 000) -ANGULAR -CORNUAL ABDOMINAL (1: 10, 000) PRIMARY SECONDARY Intraperitoneal Extraperitoneal Broad Ligament (rare)

INCIDENCE Increased due to PID, use of IUCD, Tubal surgeries, and Assisted reproductive techniques (ART). Ranges from 1: 25 to 1: 250 Average range is 1 in 100 normal pregnencies. Late marriages and late child bearing -> 2% ART -> 5% ETIOLOGY: *Pelvic Inflammatory disease (6 -10 times) Chlamydia trachomatis is most common

*Contraceptive Faliure Cu. T -4% Progestasart -17% Minipills -4 -10% Norplant -30% *Tubal sterilization faliure -40% Depends on sterilization technique and age of the patient Bipolar Cauterisation -65% Unipolar Cautery -17% Silicon rubber band -29% Interval Salpingectomy -43% Postpartum Salpingectomy -20%

*Reversal of sterilisation - Depends on method of sterilization, Site of tubal occlusion, residual tubal length. - Reanastomosis of cauterised tube -15% - Reversal of Pomeroy’s - < 3% *Tubal reconstructive surgery (4 -5 times) *Assisted Reproductive technique - Ovulation induction, IVF-ET and GIFT (4 -7%) - Risk of heterotopic pregnancy(1%) *Previous Ectopic Pregnancy - 7 -15% chances of repeat ectopic pregnancy - If first pregnancy is ectopic then 30% chance of repeat ectopic

*Developmental defects of tube elongation, diverticulum, accessory ostia, intamural polyp, entrap the ovum on its way. *Other Risk factors - Age 35 -45 yrs - Previous induced abortion - Previous pelvic surgeries - Cigarette smoking - DES Exposure in Utero

- Infertility Salpingitis Isthmica Nodosa Genital Tuberculosis Fundal Fibroid & Adenomyosis of tube Transperitoneal migration of ovum Iffy hypothesis – “Theory of reflux” menstural fluid throw the fertilised ovum into the tube Factors facilitating nidation of ovum in tube: - Premature degeneration of zona pellucida Increased decidual reaction Tubal endometriosis

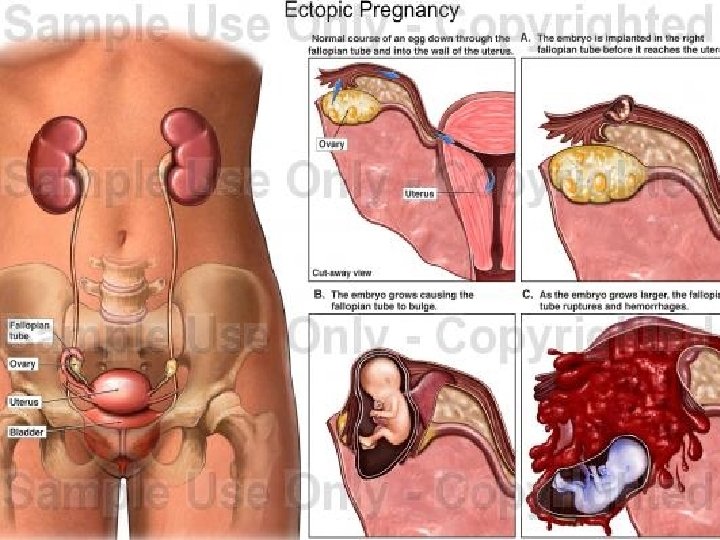
MODE OF TERMINATION 1. Tubal mole Complete absorption Abortion 2. Tubal Abortion (18 -20%) 3. Tubal Rupture Pelvic haematocele Complete Pelvic haematocele Incomplete Diffuse Intraperitoneal haemorrhage Roof Floor Diffuse Intraperitoneal haemorrhage Intraligamentary haematoma (Isthmic – 6 -8 wks, Ampullary – 8 -12 wks, Interstitial -4 months) 4. Tubal Perforation Roof Secondary Abdominal pregnancy Floor Secondary Intraligamentary pregnancy 5. Continuation of Pregnancy rarest

CLINICAL APPROACH n n n Dignosis can be done by history, detail examination and judicious use of investigation. H/o past PID, tubal surgery, current contraceptive measures should be asked Wide spectrum of clinical presentation from asymtomatic pt to others with acute abdomen and in shock.

ACUTE ECTOPIC PREGNANCY n Classical triad is present in 50% of pt with rupture ectopic. - PAIN: - most constant feature in 95% pt - variable in severity and nature - AMENORRHOEA: - 60 -80% of pt - there may be delayed period or slight spotting at the time of expected menses. - VAGINAL BLEEDING: - scanty dark brown n Feeling of nausea, vomiting, fainting attack, syncope attack(10%) due to reflex vasomotor disturbance.

n n O/E: - patient is restless in agony, looks blanched, pale, sweating with cold clammy skin. Features of shock, tachycardia, hypotension. P/A: - abdomen tense, tender mostly in lower abdomen shifting dullness, rigidity may be present. P/S: - minimal bleeding may be present P/V: - uterus may be bulky, deviated to opposite side, fornix is tender, excitation pain on movement of cervix. POD may be full, uterus floats as if in water.

CHRONIC ECTOPIC PREGNANCY n n n It can be diagnosed by high clinical suspicion. Patient had previous attack of acute pain from which she has recovered. She may have amenorrhoea, vaginal bleeding with dull pain in abdomen, and with bladder and bowel complaints like dysuria, frequency or retention of urine, rectal tenesmus.

n n O/E: - patient look ill, varying degree of pallor, slightly raised temperature. Features of shock are absent. P/A: - Tenderness and muscle guard on the lower abdomen. A mass may be felt, irregular and tender. P/V: - Vaginal mucosa pale, uterus may be normal in size or bulky, ill defined boggy tender mass may be felt in one of the fornix. P/R: - Corrobarate the pelvic findings.

UNRUPTURED ECTOPIC n High degree of suspicion & ectopic conscious clinician can diagnose. n Diagnosed accidentally in Laparoscopy or Laparotomy C/F – delayed period, spotting with discomfort in lower abdomen. P/A – tenderness in lower abdomen P/V – should be done gently uterus is normal size, firm small tender mass may be felt in the fornix

DIAGNOSIS n Patient with acute ectopic can be diagnosed clinically. n Blood should be drawn for Hb gm%, blood grouping and cross matching, DC and TWBC, BT, CT. n Should be catheterized to know urine output. Bed side test: 1. Urine pregnancy test: - positive in 95% cases. ELISA is sensitive to 10 -50 ml. U/ml of β h. CG and can be detected on 24 th day after LMP.

2. Culdocentesis: - (70 -90%) - Can be done with 16 -18 G lumbar puncture needle through posterior fornix into POD. - Positive tap is 0. 5 ml of non clotting blood. n Other Investigations: 1. Ultra Sonographya) Transvaginal Sonography (TVS): is more sensitive -It detect intrauterine gestational sac at 4 -5 wks and at S-β h. CG level as low as 1500 IU/L.

b) Color Doppler Sonography(TV-CDS): - Improve the accuracy. - Identify the placental shape (ring-of-fire pattern) and blood flow outside the uterine cavity. c) Transabdominal Sonography: - can identify gestational sac at 5 -6 wks - S-β h. CG level at which intrauterine gestational sac is seen by TAS is 6500 IU/L.

USG PICTURE 1. ‘Bagel’ sign – Hyperechoic ring around gestational sac in adnexal region 2. ‘Blob’ sign – Seen as small inconglomerate mass next to ovary with no evidence of sac or embryo. 3. Adnexal sac with fetal pole and cardiac activity is most specific. 4. Corpus luteum is useful guide when looking for EP as present in 85% cases in Ipsilateral ovary.
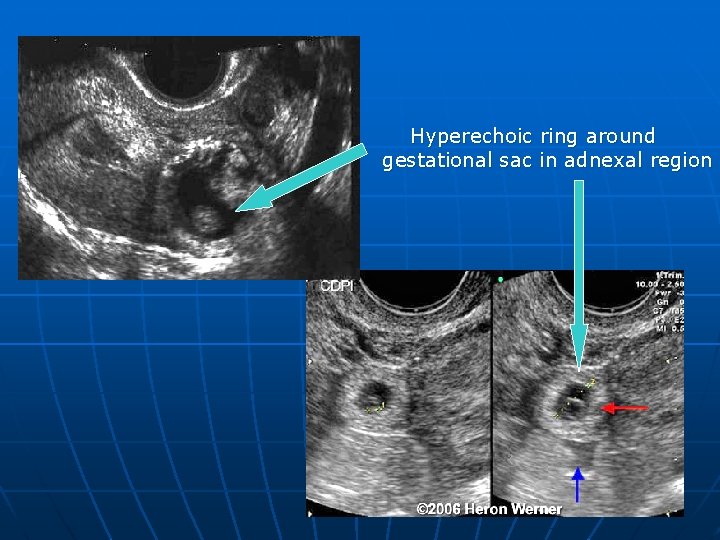
Hyperechoic ring around gestational sac in adnexal region

CO RELATION BETWEEN USG & HCG S h. CG > 6500 IU/L Sac visible by TAS Viable Intrauterine pregnancy Sac not visible S-h. CG < 6500 IU/L sac not visible - Normal pregnancy at early wks -Abnormal IU pregnancy Ectopic or Non viable -Recent abortion -Ectopic pregnancy -Non pregnant pt

2. β-HCG Assaya) Single β-HCG: little value b) Serial β-HCG: is required when result of initial USG is confusing. - When h. CG level < 2000 IU/L doubling time help to predict viable Vs nonviable pregnancy. -Rise of β-HCG <66% in 48 hrs indicate ectopic pregnancy or nonviable intrauterine pregnancy. Biochemical pregnancy is applied to those women who have two β-HCG values >10 IU/L

3. Serum Progesterone – - level >25 ngm/ml is suggestive of normal intrauterine pregnancy. - level <15 ngm/ml is suggestive of ectopic pregnancy. - level <5 ngm/ml indicates nonviable pregnancy, irrespective of its location. 4. Diagnostic Laparoscopy (Gold standard)– - Can be done only when patient is haemodynamically stable. -It confirms the diagnosis and removal of ectopic mass can be done at the same time.

5. Dilatation & Curettage – - Is recommended in suspected case of incomplete abortion vs ectopic pregnancy. - Identification of decidua without chorionic villi is suggestive of extra uterine pregnancy. - “Arias-Stella” endometrial reaction is suggestive but not diagnostic of ectopic pregnancy. 6. Other hormonal Tests – - Placenta protein (PP 14) decrease in EP - PAPPA (Pregnancy Associated Plasma Protein A), PAPPC (schwangerchaft protein 1) has low value in EP - CA-125, Maternal serum creatine kinase, Maternal serum AFP elevated in ectopic pregnancy.

SUSPECTED ECTOPIC PREGNANCY Urine Pregnancy test positive Transvaginal USG IU sac Quantitative S-h. CG + S progesterone < 66% rise in 48 hr or S progesterone < 5 -10 ng/ml D&C Villi present Incomplete abortion Villi absent Laparoscopy No IU sac >66% rise in 48 hr or S progesterone > 5 -10 ng/ml Repeat S-h. CG in 48 hrs till USG discrimination zone No sac IU sac Continue to monitor

DIFFERENTIAL DIAGNOSIS D/D of Acute Ectopic 1. 2. 3. 4. 5. 6. 7. 8. 9. Rupture corpus luteum of pregnancy Rupture of chocolate cyst Twisted ovarian cyst Torsion / degeneration of pedunculated fibroid Incomplete abortion Acute Appendicitis Perforated peptic ulcer Renal colic Splenic rupture

D/D OF CHRONIC (SUB ACUTE) ECTOPIC 1. Pelvic abscess 2. Pyosalpinx 3. Subserous uterine fibroid 4. Salpingintis 5. Retroverted gravid uterus 6. Appendicular lump

MANAGEMENT Expectant management Local (USG or Laparoscopic) salpingocentesis - Medical management Surgical management Radical Systemic Conservative Salpingectomy Methotrexate Potassium chloride Prostagladin(PGF 2α) Hypersmolar glucose Actinomycin D Mifepristone -Salpingostomy -Salpingotomy - Segmental resection -Milking or fimbrial expression

EXPECTANT MANAGEMENT CRITERIA: 1. Haemodynamically stable 2. Haemoperitoneum < 50 ml 3. Adnexal mass of < 3. 5 cm without heart beat. 4. Initial β HCG <1000 IU/L and falling in titre SUCCESS RATE - Upto 60% PROTOCOL: - Hospitalization with strict monitoring of clinical symptom - Daily Hb estimation - Serum β HCG monitoring 3 -4 days until it is <10 IU/L - TVS to be done twice a week.

MEDICAL MANAGEMENT Surgery is the mainstay of T/t worldwide Medical M/m may be tried in selected cases CANDIDATES FOR METHOTREXATE (MTX) Ø Unruptured sac < 4 cm without cardiac activity or < 3. 5 cm with cardiac activity Ø S-h. CG < 10, 000 IU/L Ø Persistant Ectopic after conservative surgery PHYSICIAN CHECK LIST Ø CBC, LFT, RFT, S-h. CG Ø Transvaginal USG within 48 hrs Ø Obtain informed consent Ø Anti-D Ig if pt is Rh negative Ø Follow up on day 1, 4 and 7.

MEDICAL MANAGEMENT Methotrexate (Systemically – IM, IV, Oral) Single dose (recent) 50 mg/m 2 IM -D 1 – β-HCG, CBC, LFT, RFT -D 4 - β-HCG -D 7 - β-HCG, CBC, LFT, RFT Multiple dose (in the past) MTX 1 mg/kg IM on D 1, 3, 5, 7 + Citrovorum 0. 1 mg/kg on D 2, 4, 6, 8 • Weekly β-HCG till negative titre • If β-HCG decrease is < 15% D 4 – D 7 then repeat the MTX dose • If decline is > 15% then weekly measure β-HCG until level is < 15 IU/L.

SURGICALLY ADMINISTERED MEDICAL Tt (SAM) By Salpingocentesis, MTX (1 mg/kg), KCL, PGF 2α, Hyperosmolar glucose, mifepristone, Anti h. CG Ab is injected into sac by transvaginally under USG guidance, Laparoscopy, transcervical tubal cannulization Advantage of local MTX : - Increase tissue concentration at local site - Decrease systemic side effects - Decrease hospitalization - Greater preservation of fertility Follow up: - Serum β HCG twice weekly till < 10 IU/L - TVS weekly for 4 -6 weeks - HCG after 6 months for tubal patency

INSTRUCTION TO THE PATIENTS Ø Ø Ø If T/t on outpatient basis rapid transportation should be available Refrain from alcohol, sunlight, multivitamins with folic acid, and sexual intercourse until S-h. CG is negative. Report immediately when vaginal bleeding, abdominal pain, dizziness, syncope (mild pain is common called separation pain or resolution pain) Failure of medical therapy require retreatment Chance of tubal rupture in 5 -10 % require emergency Laparotomy.

MANAGEMENT OF RUPTURED ECTOPIC PRINCIPLE: Resuscitation and Laparotomy ANTI SHOCK TREATEMENT: - IV line made patent, crystalloid is started - Blood sample for Hb, blood grouping & cross matching, BT, CT - Folley’s catheterization done - Colloids for volume replacement LAPAROTOMY: Principle is ‘Quick in and Quick out’ - Rapid exploration of abdominal cavity is done - Salpingectomy is the definitive surgery (sent for HP study) - Blood transfusion to be given - Autotransfusion only when donated blood not available.
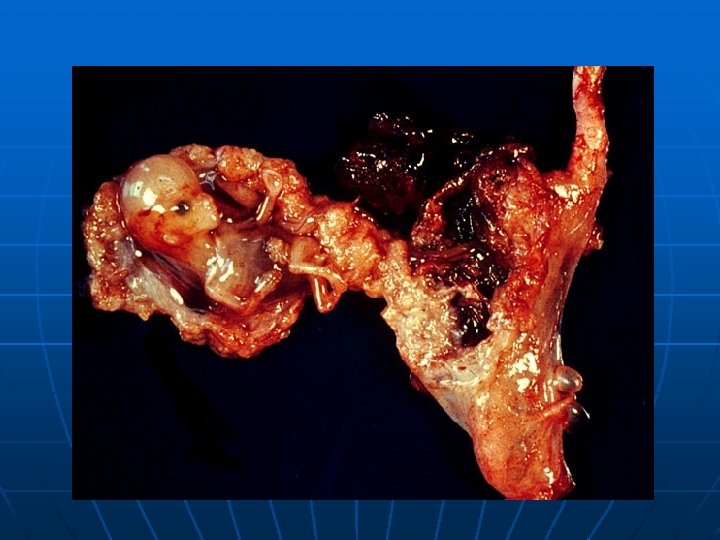

MANAGEMENT OF UNRUPTURED ECTOPIC Conservative Surgery Can be done Laparoscopically or by microsurgical laparotomy INDICATION: - Patient desires future fertility - Contralateral tube is damaged or surgically removed previously CHOICE OF TECHNIQUE: depends on - Location and size of gestational sac - Condition of tubes - Accessibility

VARIOUS CONSERVATIVE SURGERIES 1. Linear Salpingostomy: - Indicated in unruptured ectopic <2 cm in ampullary region. - Linear incision given on antimesentric border over the site and product removed by fingers, scalpel handle or gentle suction and irrigation. - Incision line kept open (heals by secondary intention) 2. Linear Salpingotomy : - Incision line is closed in two layers with 7 -0 interrupted vicryl sutures. 3. Segmental Resection & Anastomosis: - Indicated in unruptured isthmic pregnancy - End to end anastomosis is done immediately or at later date

4. Milking or fimbrial Expression: - This is ideal in distal ampullary or infundibular pregnancy. - It has got increased risk of persistent ectopic pregnancy. ADVANTAGES OF LAPAROSCOPY - It helps in diagnosis, evaluation, and treatment. - Diagnose other causes of infertility. - Decreased hospitalization, operative time, recovery period, analgesic requirement. Follow up after conservative surgery - With weekly Serum β HCG titre till it is negative. - If titre increases methotrexate can be given.

DEBATABLE ISSUES ? Salpingectomy Vs Salpingostomy ? Laparotomy Vs Laparoscopy ? Reproductive outcome ? Risk of Recurrent Ectopic

Salpingectomy Vs Salpingostomy - If future fertility is a consideration the factors to be taken into account are status of Ipsilateral tube, Contralateral tube, other pelvic pathology. - Report shows there is no significant difference in subsequent reproductive outcome with regard to IU pregnancy or recurrent Ectopic. - Linear Salpingostomy is currently procedure of choice, when pt has unruptured Ectopic and wishes to retain her potential for future fertility. - In pt with only one tube, conservative surgery may be appropriate but only when pt is aware and accept the risk involved.

Laparotomy Vs Laparoscopy - Laparoscopy is reserved for pt who are hemodynamically stable. - Ruptured Ectopic does not necessarily require Laparotomy, but if large clots are present Laparotomy should be considered. Reproductive outcome Is similar in pt treated with either Laparoscopy or Laparotomy. Identical rates of 40% of IUP, around 12% risk of recurrent pregnancy with either radical or conservative pregnancy.

PERSISTENT ECTOPIC PREGNANACY Defined as continued growth of trophoblastic tissue after conservative treatment (3 – 20 % incidence) Risk Factor: 1. Early ectopic pregnancy (< 6 wks amenorrhoea) 2. Smaller size < 2 cm (Incomplete removal) 3. Preoperative high serum β HCG (> 3, 000 IU/L) 4. Decrease in postoperative Day 1 titre is < 50% of preoperative level, is predictor of persistent EP. Treatment surgery Total or partial salpingectomy Medical (selected Asymptomatic pt) MTX + Leukovorin

OVARIAN ECTOPIC PREGNANCY Incidence: 1: 40, 000 Risk factor: - IUCD - Endometriosis on surface of ovary Course: C/F are same as tubal pregnancy ruptures within 2 -3 wks Diagnosis: On Laparotomy Spiegelberg’s Criteria 1. Ipsilateral tube is intact and separate from sac 2. Sac occupies the position of the ovary 3. Connected to uterus by ovarian ligament 4. Ovarian tissue found on its wall on HP study M/M Ruptured Laparotomy Oophorectomy Unruptured Ovarian wedge resection Ovarian Cystectomy

ABDOMINAL PREGNANCY Incidence: Rarest MMR : 7 -8 times > tubal ectopic 90 times > Intrauterine pregnancy H/O : - Irregular bleeding, spotting - Nausea, vomiting, flatulence, constipation, diarrhoea, abdominal pain. - Fetal movement may be painful and high in the abdomen O/E : - Abnormal fetal position, easy in palpating fetal parts. - uterus palpated separate from sac - no uterine contraction after oxytocin infusion

Diagnosis: Confirmed by USG, CT scan, MRI, Radiography TYPE Primary Studiford’s criteria 1. Both tubes and ovaries normal 2. Absence of Uteroperitonal fistula Secondary Conceptus escapes out through a rent from primary site 3. Pregnancy related to Peritoneal Intraperitoneal surface & young enough to rule out possibility of secondary implantation Extraperitoneal Broad ligament

FATE OF SECONDARY ABDOMINAL PREGNANCY : 1. Death of ovum – complete absorption 2. Placental separation – massive intraperitoneal haemorrhage 3. Infection – fistulous communication with intestine, bladder, vagina, or umbilicus 4. Fetus dies (majority) – mummification, adipocere formation, or calcified to lithopaedion 5. Rarely – continue to term (malformation) M/M: - Urgent Laparatomy irrespective of period of gestation - Ideal to remove entire sac fetus, placenta, membrane - Placenta may be left if attached to vital organs, get absorbed by aseptic autolysis

CERVICAL PREGNANCY Implantation occurs in cervical canal at or below internal Os. Incidence: 1 in 18, 000 RISK FACTORS : - Previous induced abortion - Previous caesarean delivery - Asherman’s syndrome - IVF - DES exposure - Leiomyoma

Diagnosis: CLINICAL CRITERIA: Paulman & Mc. Ellin 1. Uterine bleeding, no cramping, following amenorrhoea 2. Cervix > Corpus, soft consistency 3. POC confined to endocervix 4. Internal Os is closed 5. External Os is partially opened USG CRITERIA: American Journal of O&G 1. Echo-free uterine cavity/ pseudo-gestational sac 2. Decidual reaction 3. Hourglass uterus with ballooned cervical canal 4. Gestational sac in endocervix 5. Closed internal Os 6. Placental tissue in Cx canal

HISTOPATHOLOGIC CRITERIA: Rubin’s 1. Cervical glands present opposite to placenta 2. Placental attachment to the cervix must be below the entrance of uterine vessels. 3. Fetal element absent from corpus uteri. D/d : - Carcinoma Cx - Cervical submucous fibroid - Trophoblastic tumour - Placenta previa
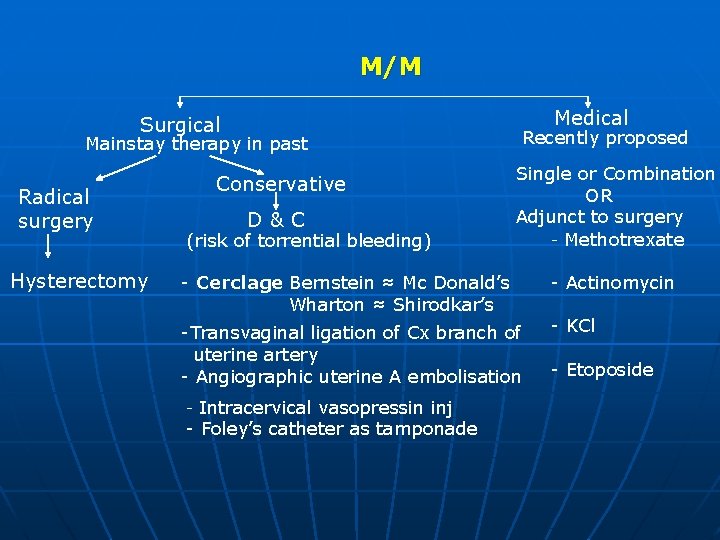
M/M Medical Surgical Mainstay therapy in past Radical surgery Hysterectomy Conservative D&C (risk of torrential bleeding) Recently proposed Single or Combination OR Adjunct to surgery - Methotrexate - Cerclage Bernstein ≈ Mc Donald’s Wharton ≈ Shirodkar’s -Transvaginal ligation of Cx branch of uterine artery - Angiographic uterine A embolisation - Intracervical vasopressin inj - Foley’s catheter as tamponade - Actinomycin - KCl - Etoposide

CORNUAL PREGNANCY SITE: Implantation occurs in rudimentary horn of Bicornuate uterus COURSE : Rupture of horn occurs by 12 – 20 wks D/D : 1. Interstitial tubal pregnancy 2. Painful leiomyoma along with pregnancy 3. Ovarian tumor with pregnancy 4. Asymmetrical enlargement of uterus. Implantation into cornu of normal uterus is sometime called Angular pregnancy. TREATEMENT: - Affected cornu with pregnancy is removed - Hysterectomy - Hysteroscopically guided suction curettage if communication with Cx is patent

HETEROTYPIC PREGNANCY Co-existing intrauterine and extra uterine pregnancies Incidence: 1 : 30, 000 With ART – 1: 7000 With ovulation induction – 1: 900 More likely: a) Ass. reproductive technique b) Rising HCG titre after D & C c) More than 1 corpus luteum at laparotomy M/M : Depends on the site. Ectopic site may be removed with continuation of IU pregnancy (Rh Immunoglobulin: dose of 50 μ gm is sufficient to prevent sensitization. )

INTERSTITAL PREGNANCY (2%) It ruptures late at 3 -4 months gestation. Fatal rupture – severe bleeding as both uterine & ovarian artery supply. Early & Unruptured – Local or IM MTX with followup Cornual resection by Laparotomy may be done. There is high risk of uterine rupture in subsequent pregnancy. Rupture – Hysterectomy is indicated

CAESAREAN SCAR ECTOPIC PREGNANCY Ø Ø Recently reported USG slows on empty uterine cavity and gestational sac attached low to the lower segment caesarean scar. C/F : similar to threatened or inevitable abortion Diagnosis : Doppler imaging confirms T/t : Methotrexate injection Hysterectomy in a multiparous women. In young pt resection & suturing of scar may be done (high risk of rupture).

OTHER RARE TYPES 1. 2. 3. 4. 5. 6. Multiple Ectopic pregnancy Pregnancy after hysterectomy Primary splenic pregnancy Primary hepatic pregnancy Rectroperitoneal pregnancy Diaphragmatic pregnancy MORTALITY : In general population is 10 -15% mainly due to haemorrhage.

CONCLUSION Ø Ø Ectopic pregnancy can be diagnosed early (before it ruptures) with recent advances in Immunoassay to detect S-h. CG , high resolution USG, and dignostic Laparoscopy. There has been shift in the M/m from ablative surgery to conservative fertility preserving therapy Laparotomy should be done when in doubt Surgeon should not be ashamed of having negative abdominal exploration, rather to be disgraced for the mistake in diagnosis with the eventual fatality.

- Slides: 60