ANC The way to go Prof Elsayed Elbadawy

ANC: The way to go Prof. Elsayed Elbadawy Awad Professor of OB&Gyn Head of main U/S unit El-Shatby Maternity University hospital Alexandria University

Definition • An antenatal visit is defined as an intentional encounter between a pregnant woman and a health care provider to assess and improve maternal and fetal well-being throughout pregnancy and prior to labor

• Antenatal Care (ANC) means “care before birth”, and includes education, counseling, screening and treatment to monitor and to promote the well-being of the mother and fetus.

History revisited • The rationale for the 'traditional' schedule developed in the UK during the 1920 s is based on theory that regular visits with predefined content enable midwives and doctors to detect conditions in mother and baby that may threaten their health

Origin of ANC • Prenatal care started in Edinburgh at the turn of the 20 thcentury, but clinics for the checking of apparently well pregnant women were rare before the first world war. • During the 1920 s a few midwifery departments of hospitals and interested general practitioners saw women at intervals to check their urine for protein. Janet Campbell

Global or local ANC? • ANC is a right for any pregnant woman. • The package of interventions included in routine ANC should be based on : effectiveness, local epidemiology of specific diseases local priorities and resources; and the preferences and values of recipients.

Traditional schedule • The 'traditional' number of antenatal visits is approximately 14, based on early presentation and a schedule of four weekly visits until 28 weeks gestation, then fortnightly visits until 36 weeks gestation, followed by weekly visits until birth.

Objectives of ANC • Promote and maintain the physical, mental and social health of mother and baby by providing education on nutrition, personal hygiene and birthing process • Detect and manage complications during pregnancy, whether medical, surgical or obstetrical • Help prepare mother to breastfeed successfully, experience normal puerperium, and take good care of the child physically, psychologically and socially

National status: the bad news • Every year, 529 000 women and 5. 7 million newborns die, almost all in the developing world • More than 70% of maternal deaths are due to haemorrhage, obstructed labour, eclampsia, sepsis and unsafe abortion • Maternal mortality in Egypt is double that of Jordan & Malysia, 4 times that of KSA and 18 times that of Kuwait & 28 times that of UAE
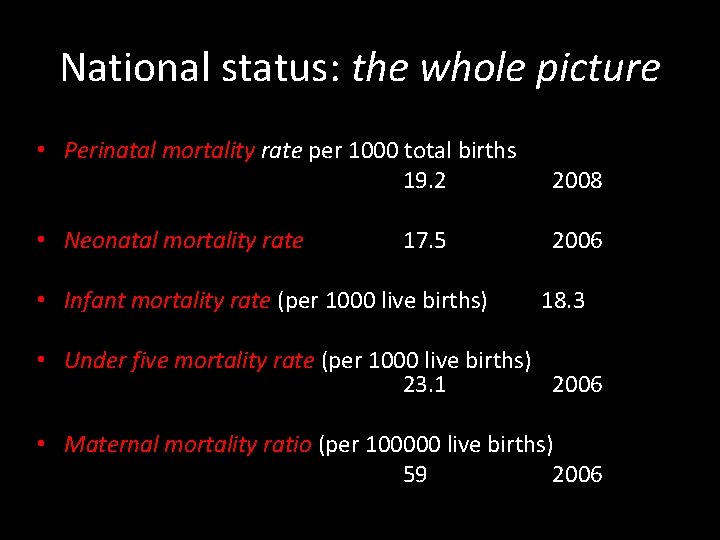
National status: the whole picture • Perinatal mortality rate per 1000 total births 19. 2 2008 • Neonatal mortality rate 17. 5 2006 • Infant mortality rate (per 1000 live births) 18. 3 • Under five mortality rate (per 1000 live births) 23. 1 2006 • Maternal mortality ratio (per 100000 live births) 59 2006

National status: the good news Coverage with primary health care services indicators (WHO Stats) • Population with access to local health services, total 100% 2008 • Population with access to local health services, urban 100% 2008 • Population with access to local health services, rural 100% 2008 • Contraceptive prevalence 60% 2008 • Antenatal care coverage 60% 2008 • Births attended by skilled health personnel 81 % 2008

National status: More good news • National maternal mortality ratio in Egypt halved between 1992– 93 and 2000 • MMR in Egypt has dropped from 184/100, 000 live births in 1993 to 59 in 2008 {WHO report 2009)

National Objectives • Reduce maternal & perinatal mortality and morbidity • Screen for endemic and common clinical conditions • Teaching mothers healthy practices about pregnancy and child birth • Establish a nationwide system of referrals to ensure best management for at risk patients
• The current challenge is to find out which type of care (value or quality ) and in what quantity (visits ) is considered sufficient to ensure good quality of care for low-risk pregnant women. • Only interventions of proven effectiveness, for which benefits largely overcome possible harms, and those acceptable to pregnant women and their families, should be offered

Examples of “ineffective” ANC interventions • Iron supplementation (may have unpleasant maternal side effects) • � Vitamin B 6 (pyridoxine) to control nausea • Pelvimetry ( increases the chances of caesarean section • � Uterine Doppler ultrasound for prediction of pre-eclampsia • Routine third-trimester ultrasound

Tailored ANC • Differences in epidemiology of given conditions, investment priorities, cultural and social values preclude implementation of a homogeneous imported ANC package. • However, in countries with scarce resources, attention should be primarily focused on a limited set of essential interventions that are effective in reducing relevant adverse outcomes for mothers and babies.

The way to go: Reduced number of visits • Lowering the number of routine prenatal visits does not jeopardize health outcomes for pregnancy women or their babies, but may reduce women's satisfaction with care. • A model with a reduced number of antenatal visits, with or without goal-oriented components, could be introduced into clinical practice without risk to mother or baby, but some degree of dissatisfaction by the mother could be expected. Lower costs can be achieved. “WHO systematic review of randomised controlled trials of routine antenatal care. ” The Lancet 2001; 357(9268): 1565 -70

Structured antenatal care: suggested schedule for improving quality

Booking visit • Timing 2 -3 weeks following +ve pregnancy test • Objectives – Confirm IUGS – Confirm fetal viability & twining – Order investigations • Tools

Initial Prenatal Visit • Confirmation of pregnancy • History – – – medical history psychosocial history family history surgical history genetic-familial history of both patient and spouse – reproductive history • • • menstrual history contraceptive history gynecologic history obstetrical history sexual history – medications/exposures since LMP • • alcohol smoking social drugs medications

• Perform physical examination – vital signs – head-to-toe exam – pelvimetry • measurement of the diagonal conjugate from the posterior inferior edge of the symphysis pubis to the sacral promontory - normally >12. 5 cm =>estimates the inlet • the transverse diameter of the midpelvis includes evaluation of the ischial spines (sharp or blunt and degree of prominence) and of the anteroposterior diameter by the shape of the sacrum (curved or flat). The ischial tuberosities should be >8 cm apart.

• Objectives of investigations requested : Screening and detection of common and endemic conditions: – Anemia – Blood group& Rh – Rubella status – HBV &HCV – Bacteriuria – Chronic illnesses

• Facilitate patient education – give handouts – answer questions – instruct about danger signals • • vaginal bleeding persistent vomiting chills or fever dysuria abdominal pain or uterine cramping swelling of the face or fingers cerebral or visual disturbances – dizziness – mental confusion – spots before the eyes

headaches that do not respond to simple remedies oliguria leakage of fluid from the vagina marked decrease in intensity or frequency of fetal movements • signs of preterm labor • • – uterine contractions – pelvic pressure – change in vaginal discharge – information about prenatal classes – choices in infant feeding • Schedule follow-up visits – discuss importance of prenatal care – discuss schedule of follow-up visits

Educating our patients • • • Plan of care Nutrition & weight gain Exercise Early warning signs Common discomforts Breastfeeding Sex Tobacco/alcohol/drugs Domestic violence Hot tubs & saunas
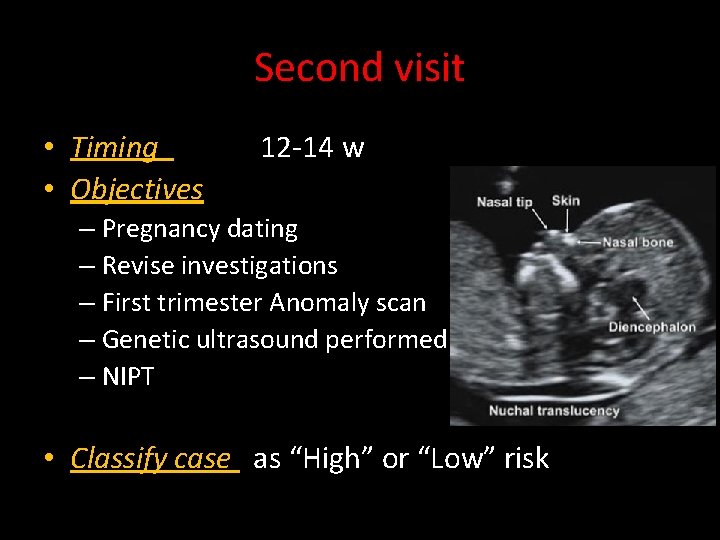
Second visit • Timing 12 -14 w • Objectives – Pregnancy dating – Revise investigations – First trimester Anomaly scan – Genetic ultrasound performed – NIPT • Classify case as “High” or “Low” risk


Subsequent Prenatal Visits • measure: – weight – BP • evaluate urine for: – – – blood protein ketones nitrites glucose assess fetal movement determine fundal height assess fetal heart tones assess fetal position evaluate any patient complaints • answer questions appropriately • • •
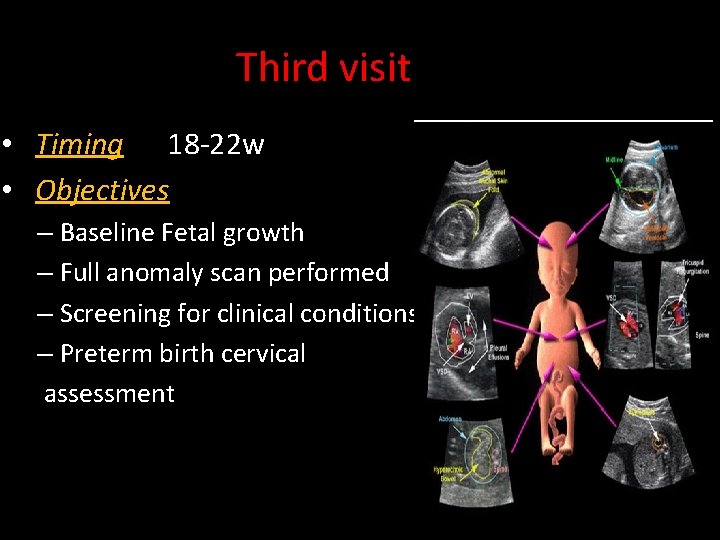
Third visit • Timing 18 -22 w • Objectives – Baseline Fetal growth – Full anomaly scan performed – Screening for clinical conditions – Preterm birth cervical assessment

Fourth visit • Timing 26 -30 w • Objectives – Monitor fetal growth – Detection of placenta previa&accreta – Maternal well-being – Screen for GDM, anemia and Asymptomatic bacteriuria
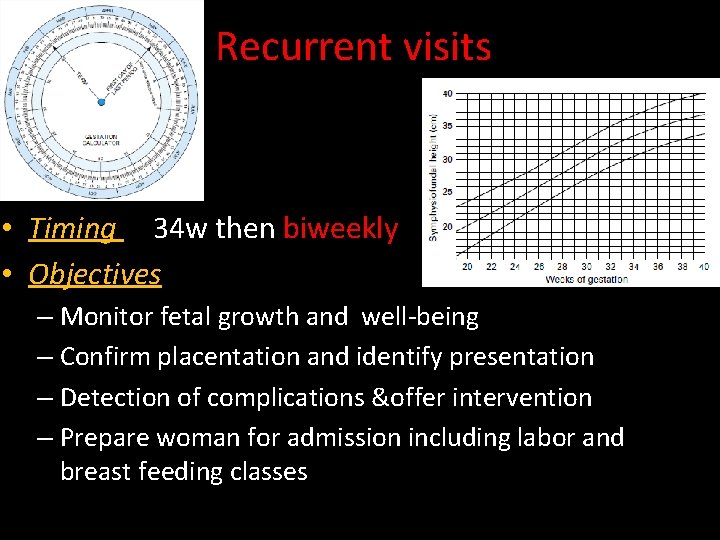
Recurrent visits • Timing 34 w then biweekly • Objectives – Monitor fetal growth and well-being – Confirm placentation and identify presentation – Detection of complications &offer intervention – Prepare woman for admission including labor and breast feeding classes

Take Home Message Define national objectives Set National priorities Reducing No. of visits will not affect outcome Improving Quality per visit will improve outcome • Screening versus early detection of complications is still debatabale • •

THANK YOU

The 3 Centre Collaboration concurs with the RCOG recommendations of: • “A schedule of antenatal appointments should be determined by the function of the appointments. • For a woman who is nulliparous with an uncomplicated pregnancy, a schedule of ten appointments should be adequate. • For a woman who is parous with an uncomplicated pregnancy, a schedule of seven appointments should be adequate. ”
- Slides: 34