Anatomy Physiology Of Female Reproductive System Learning Objectives

Anatomy & Physiology Of Female Reproductive System

Learning Objectives l Define the terms listed. l Identify the female external reproductive organs. l Explain the structure of the bony pelvis. l Explain the functions and structures of pelvic floor.

Introduction

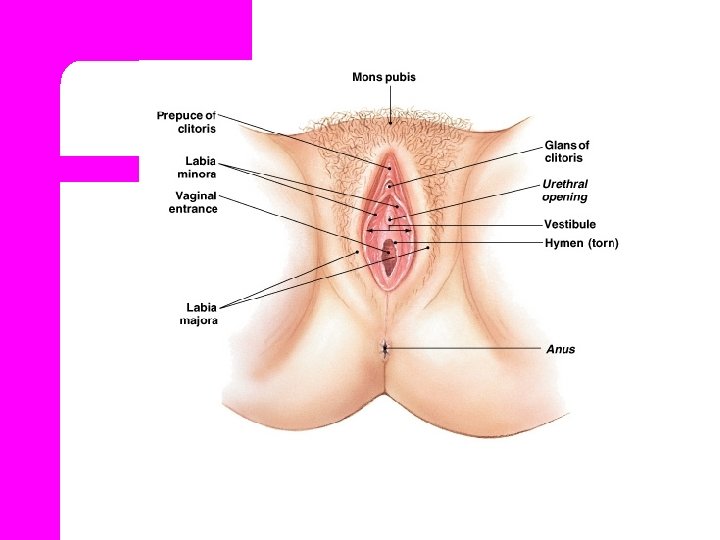
External Female Structures l. Collectively, the external female reproductive organs are called the Vulva.

External Female Structures l Mons Pubis. l Labia Majora l Labia Minora. l Clitoris. l Vestibule. l Perineum

Mons Pubis Is rounded, soft fullness of subcutaneous fatty tissue, prominence over the symphysis pubis that forms the anterior border of the external reproductive organs. It is covered with varying amounts of pubic hair.

Labia Majora & Minora l The labia Majora are two rounded, fleshy folds of tissue that extended from the mons pubis to the perineum. l It is protect the labia minora, urinary meatus and vaginal introitus.

Labia Minora l It is located between the labia majora, are narrow. l The lateral and anterior aspects are usually pigmented. l The inner surfaces are similar to vaginal mucosa, pink and mois. l Their rich vascularity.

Clitoris. l The term clitoris comes from a Greek word meaning key. l Erectile organ. l It’s rich vascular, highly sensitive to temperature, touch, and pressure sensation

Vestibule. l Is oval-shaped area formed between the labia minora, clitoris, and fourchette. l Vestibule contains the external urethral meatus, vaginal introitus, and Bartholins glands.

Perineum l Is the most posterior part of the external female reproductive organs. l It extends from fourchette anteriorly to the anus posteriorly. l And is composed of fibrous and muscular tissues that support pelvic structures.

Internal Female Structures l. Vagina l. Uterus l. Fallopian l. Ovaries tubes
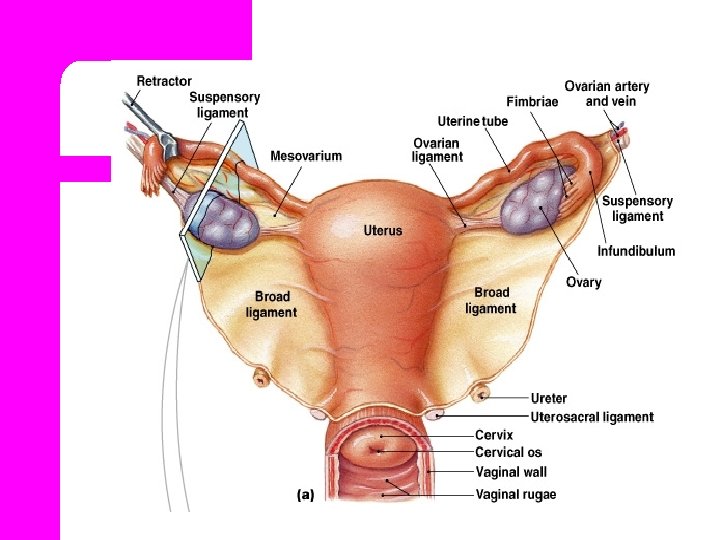

Fallopian tubes l The two tubes extended from the cornu of the uterus to the ovary. l It runs in the upper free border of the broad ligament. l Length 8 to 14 cm average 10 cm l Its divided into 4 parts.
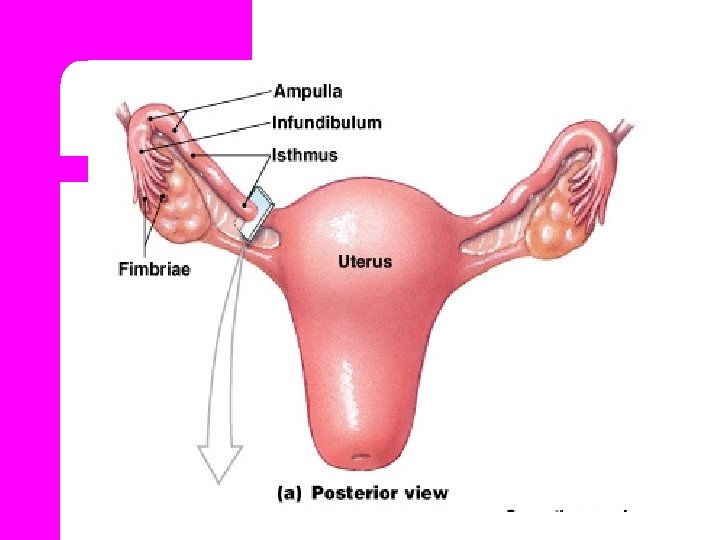

1. Interstitial part l Which runs into uterine cavity, passes through the myometrium between the fundus and body of the uterus. About 1 -2 cm in length.

2. Isthmus l. Which is the narrow part of the tube adjacent to the uterus. l. Straight and cord like , about 2 – 3 cm in length.

3. Ampulla l. Which is the wider part about 5 cm in length. l. Fertilization ampulla. occurs in the

4. Infundibulum l It is funnel or trumpet shaped. l Fimbriae are fingerlike processes, one of these is longer than the other and adherent to the ovary. l The fimbriae become swollen almost erectile at ovulation.

Functions l Gamete transport (ovum pickup, ovum transport, sperm transport). l Final maturation of gamete post ovulate oocyte maturation, sperm capicitation.

l Fluid environment for early embryonic development. l Transport of fertilized and unfertilized ovum to the uterus.

Ovaries l Oval solid structure, 1. 5 cm in thickness, 2. 5 cm in width and 3. 5 cm in length respectively. Each weights about 4– 8 gm. l Ovary is located on each side of the uterus, below and behind the uterine tubes

Structure of the ovaries l. Cortex l. Medulla l. Hilum
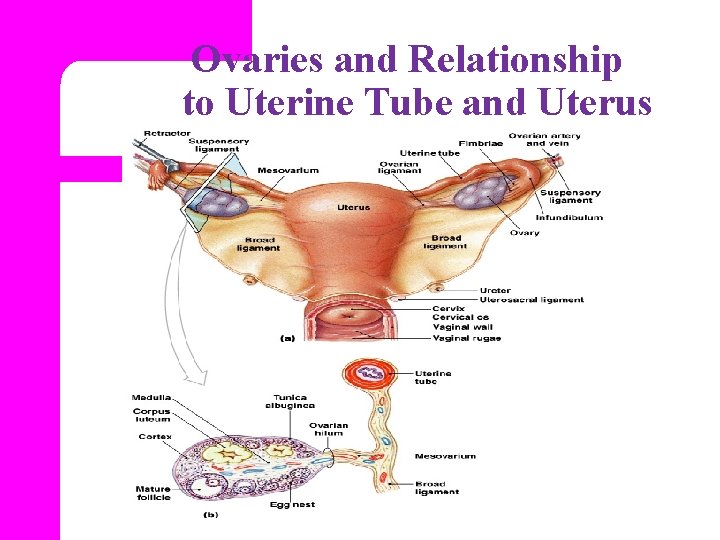
Ovaries and Relationship to Uterine Tube and Uterus Figure 28– 14

Function of the ovary l Secrete estrogen & progesterone. l Production of ova

Uterus l The uterus is a hollow, pear shaped muscular organ. l The uterus measures about 7. 5 X 2. 5 cm and weight about 50 – 60 gm.

l Its normal position is anteverted (rotated forward and slightly antiflexed (flexed forward) l The uterus divided into three parts

1. Body of the uterus l The upper part is the corpus, or body of the uterus l The fundus is the part of the body or corpus above the area where the fallopian tubes enter the uterus. l Length about 5 cm.

2. Isthmus l. A narrower transition zone. l Is between the corpus of the uterus and cervix. l During late pregnancy, the isthmus elongates and is known as the lower uterine segment.

3. Cervix l The lowermost position of the uterus “neck”. l The length of the cervix is about 2. 5 t 0 3 cm.

l The os, is the opening in the cervix that runs between the uterus and vagina. l The upper part of the cervix is marked by internal os and the lower cervix is marked by the external os.

Layers of the uterus Perimetrium. l Myometrium. l Endometrium. l
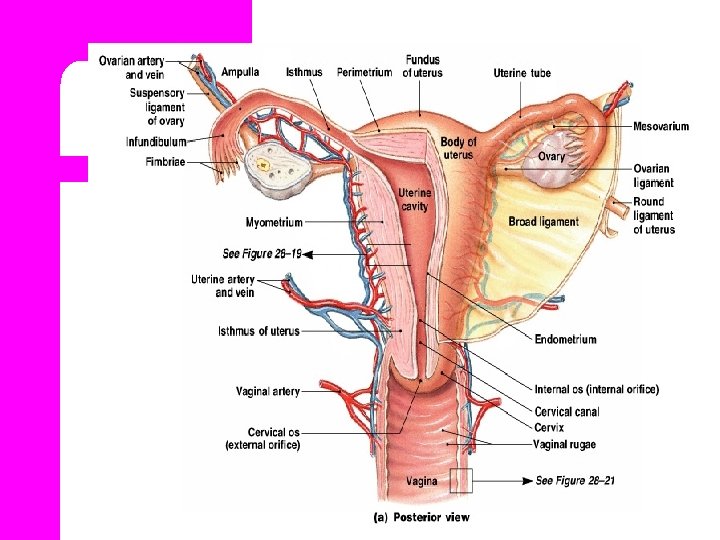

1. Perimetrium l Is the outer peritoneal layer of serous membrane that covers most of the uterus.

l Laterally, the perimetrium is continuous with the broad ligaments on either side of the uterus.

2. Myometrium l Is the middle layer of thick muscle. l Most of the muscle fibers are concentrated in the upper uterus, and their number diminishes progressively toward the cervix.

l. The myometrium contains three types of smooth muscle fiber

Longitudinal fibers (outer layer) l Which are found mostly in the fundus and are designed to expel the fetus efficiently toward the pelvic outlet during birth.

Middle layer figure-8 fibers l. These fiber contract after birth to compress the blood vessels that pass between them to limit blood loss.

Inner layer circular fibers l Which form constrictions where the fallopian tubes enter the uterus and surround the internal os l Circular fibers prevent reflux of menstrual blood and tissue into the fallopian tubes.

l Promote normal implantation of the fertilized ovum by controlling its entry into the uterus. l And retain the fetus until the appropriate time of birth.

3. Endometrium l Is the inner layer of the uterus. l It is responsive to the cyclic variations of estrogen and progesterone during the female reproductive cycle every month.

l The two or three layers of the endometrium are: *Compact layer *The basal layer *The functional or Sponge layer this layer is shed during each menstrual period and after child birth in the lochia

The Function of the uterus l Menstruation ----the uterus sloughs off the endometrium. l Pregnancy ---the uterus support fetus and allows the fetus to grow.

l Labor and birth---the uterine muscles contract and the cervix dilates during labor to expel the fetus

Vagina l It is an elastic fibro-muscular tube and membranous tissue about 8 to 10 cm long. l Lying between the bladder anteriorly and the rectum posteriorly.

l The vagina connects the uterus above with the vestibule below. l The upper end is blind and called the vaginal vault.

l The vaginal lining has multiple folds, or rugae and muscle layer. These folds allow the vagina to stretch considerably during childbirth.

l. The reaction of the vagina is acidic, the p. H is 4. 5 that protects the vagina against infection.

Functions of the vagina l To allow discharge of the menstrual flow. l As the female organs of coitus. l To allow passage of the fetus from the uterus.

Support structures l. The bony pelvis support and protects the lower abdominal and internal reproductive organs.

l Muscle, Joints and ligaments provide added support for internal organs of the pelvis against the downward force of gravity and the increases in intra-abdominal pressure

Bony Pelvis l Bony Pelvis Is Composed of 4 bones: 1. Two hip bones. 2. Sacrum. 3. Coccyx.

1. Two hip bones. l Each or hip bone is composed of three bones: *Ilium *Ischium *Pubis

*Ilium l It is the flared out part. l The greater part of its inner aspect is smooth and concave, forming the iliac fossa. l The upper border of the ilium is called iliac crest

*Ischium l It is the thick lower part. l It has a large prominence known as the ischial tuberosity on which the body rests while sitting.

l. Behind and little above the tuberosity is an inward projection the ischial spine.

2. Sacrum l Is a wedge shaped bone consisting of five vertebrae. l The anterior surface of the sacrum is concave l The upper border of the first sacral vertebra known as the sacral promontory

3. Coccyx. Consists of four vertebrae forming a small triangular bone. l

- Slides: 61