ANATOMY OF TRACHEOBRONCHIAL TREE AND PULMONARY VENTILATION Presented

ANATOMY OF TRACHEOBRONCHIAL TREE AND PULMONARY VENTILATION Presented by Dr. Sunil Kumar Arora 1

Organs of the Respiratory System A. The organs of the respiratory tract can be divided into two groups: 1. Upper Airways 2. Lower airways 2

Upper Airways • Nose • Paranasal sinuses • Pharynx 3

Lower Airway Begins with true vocal cords and extends to alveoli • • • Larynx Trachea Main stem bronchi Segmental bronchi Subsegmental bronchi • Bronchioles • Terminal bronchioles • Respiratory bronchioles • Alveolar ducts • Alveolar sacs • alveoli 4
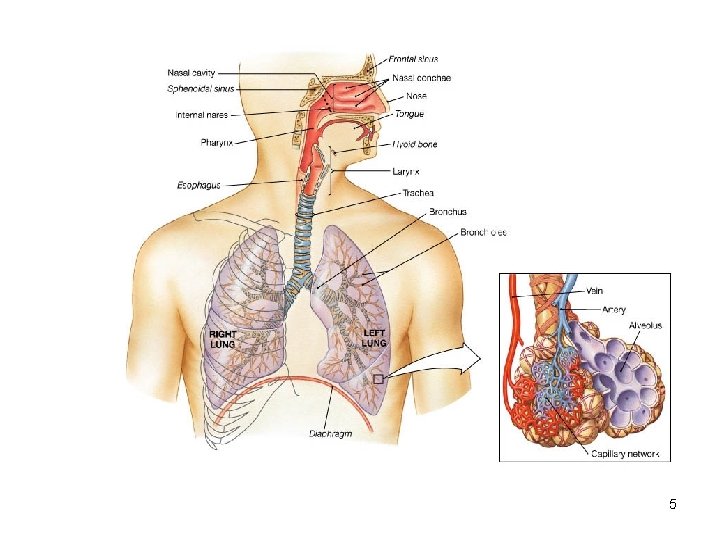
5

Organization and Functions of the Respiratory System • Conducting portion transports air. - includes the nose, nasal cavity, pharynx, larynx, trachea, and progressively smaller airways, from the primary bronchi to the terminal bronchioles • Respiratory portion carries out gas exchange. - composed of small airways called respiratory bronchioles and alveolar ducts as well as air sacs called alveoli 6

Tracheobronchial Tree • A highly branched system of air-conducting passages that originate from the trachea and progressively branch into narrower tubes as they diverge throughout the lungs before terminating in terminal bronchioles. • Series branching airways commonly referred to as “generations” or of “orders” The first generation or order is zero (0), the trachea itself 7

Trachea • A flexible tube of 10 -12 cm length and 1. 5 -2. 5 cm width also called windpipe. Extends to second rib anteriorly and T 4 -T 5 posteriorly. • Extends through the mediastinum and lies anterior to the esophagus and inferior to the larynx. • Anterior and lateral walls of the trachea supported by 15 to 20 Cshaped tracheal cartilages. • Cartilage rings reinforce and provide rigidity to the tracheal wall to ensure that the trachea remains open at all times • Posterior part of tube lined by trachealis muscle. 8

Tracheal lining • Pseudostratified columnar epithelium with cilia; goblet cells, serous cells, and specialized submucosal bronchial glands • 200+ cilia per cell, 5 -7 microns long • Beat cephalid (head) toward oropharynx 9

Primary bronchus • At the level of the sternal angle, the trachea bifurcates into two smaller tubes, called the right and left primary bronchi. • Each primary bronchus projects laterally toward each lung. • The most inferior tracheal cartilage separates the primary bronchi at their origin and forms an internal ridge called the carina. 10

Main Stem Bronchi • Right bronchus – – Wider More vertical 5 cm shorter Supported by C shaped cartilages – 20 -30 degree angle – First generation • Left bronchus – – Narrower More angular Longer Supported by C shaped cartilages – 40 -60 degree angle – First generation • Foreign particles are more likely to lodge in the right primary bronchus. 11

Bronchial tree • The primary bronchi enter the hilus of each lung together with the pulmonary vessels, lymphatic vessels, and nerves. • Each primary bronchus branches into several secondary bronchi (or lobar bronchi). • The left lung has two secondary bronchi. The right lung has three secondary bronchi. • They further divide into tertiary bronchi. • Each tertiary bronchus is called a segmental bronchus because it supplies a part of the lung called a bronchopulmonary segment. 12

Lobar Bronchi • R main stem divides into: – Upper lobar bronchus – Middle lobar bronchus – Lower lobar bronchus • L main stem divides into: – Upper lobar bronchus – Lower lobar bronchus 13

Segmental Bronchi 3 rd generation • R lobar divides into – Segmental bronchi – 10 segments on right • L lobar divides into – Segmental bronchi – 8 segments on left 14

Subsegmental Bronchi • • 4 th to 9 th generations Progressively smaller airways 1 -4 mm diameter At 1 mm diameter connective tissue sheath disappears 15

Noncartilagenous Airways Bronchioles – 10 -th to 15 th generation – Cartilage is absent – Lamina propria is directly connected with lung parenchyma – Surrounded by spiral muscle fibers – Epithelial cells are cuboidal – Less goblet cells and cilia – With no cartilage, airway remains open due to pressure gradients 16

Terminal Bronchioles • 16 th to 19 th generation • Average diameter is 0. 5 mm • Cilia and mucous glands begin to disappear totally • End of the conducting airway • Canals of Lambert-interconnect this generation, provide collateral ventilation 17

Respiratory Bronchioles, Alveolar Ducts, and Alveoli • Lungs contain small saccular outpocketings called alveoli. • They have a thin wall specialized to promote diffusion of gases between the alveolus and the blood in the pulmonary capillaries. • Gas exchange can take place in the respiratory bronchioles and alveolar ducts as well as in the alveoli, each lung contains approximately 300 to 400 million alveoli. • The spongy nature of the lung is due to the packing of millions of alveoli together. 18
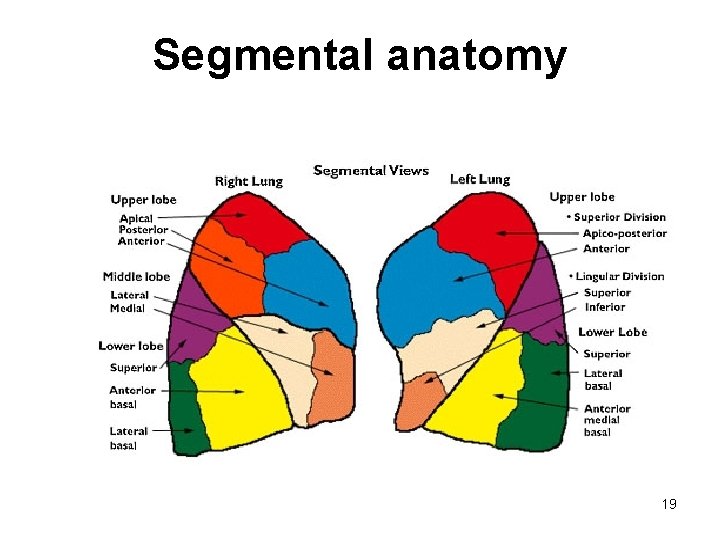
Segmental anatomy 19
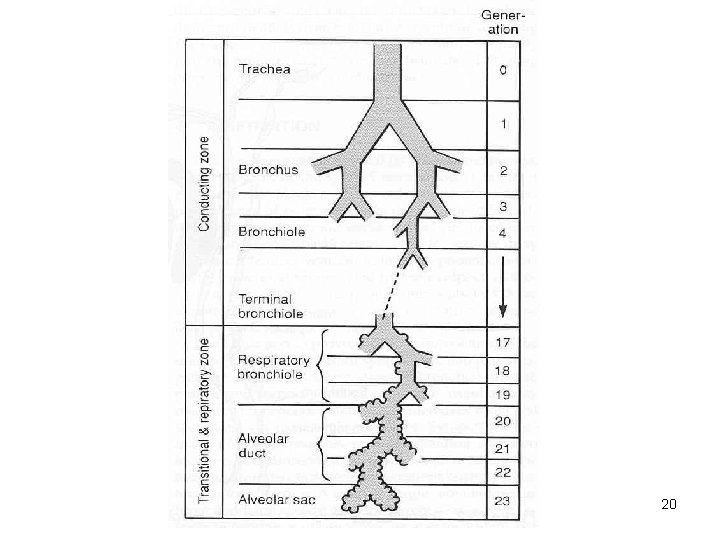
20

Gas exchange zone • Respiratory bronchioles • Acinus • Alveolar Ducts, sacs, alveoli 21

Functional Units of Gas Exchange • Three generations of respiratory bronchioles • Three generations of alveolar ducts • 15 -20 clusters--sacs 22

Acinus or Lobule • Each acinus (unit) is approximately 3. 5 mm in diameter • Each contains about 2000 aveloli • There approximately 130, 000 primary lobules in the lung 23

Anatomic Arrangement of Alveoli • 85 -95% of alveoli covered by small pulmonary capillaires • The cross-sectional area or surface area is approximately 70 m 2 • Total of about 300 million alveoli in 2 lungs 24

Cells in Alveolus Type I cells : 95% of Alveoler surface, Major site of gas exchange Type II cells : or Septal cells secrete surfactant, About 5% of Alveoler surface. Alveolar macrophages-Plays role in defence mechenism. 25
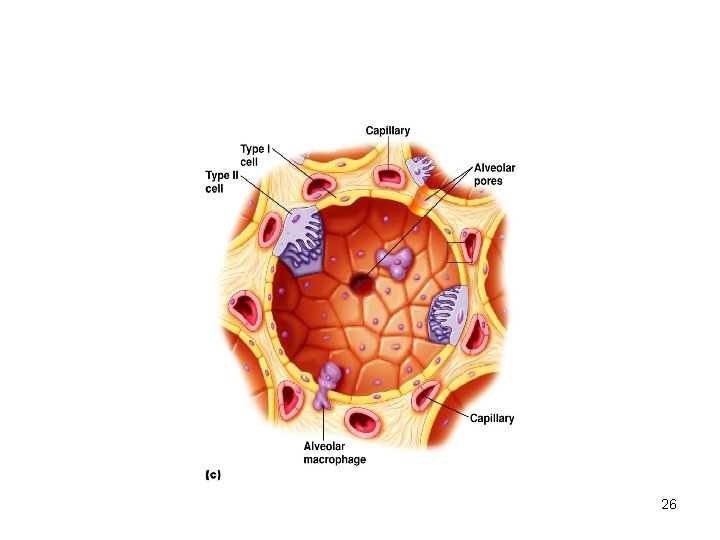
26

Surfactant Is a substance produce by type II alveolar epithelial cells (~ 5% of the surface area of the alveoli) which reduce the surface tension of the fluid in the inner surface of the alveoli it is a mixture of phospholipids, proteins, and ions, the most important component is phospholipid dipalmitoyl phosphatidylcholine which is responsible for reducing the surface tension. 27
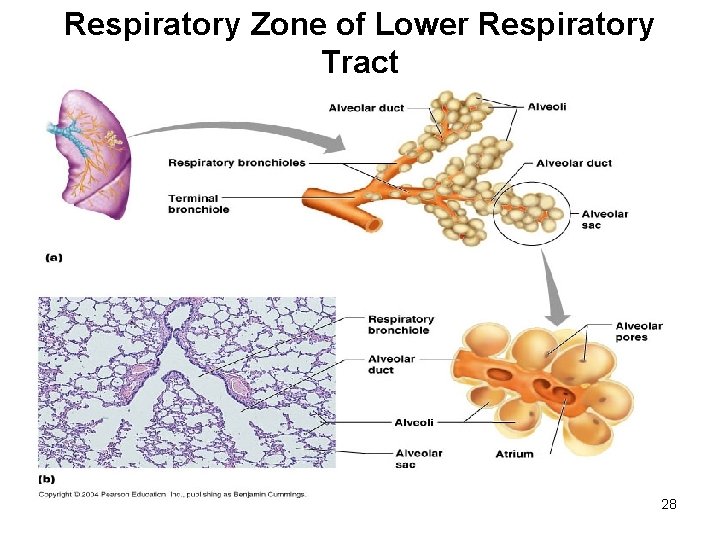
Respiratory Zone of Lower Respiratory Tract 28

Respiratory Membrane Diffusion of gases occurs through Respiratory mambrane. • • • squamous cells of alveoli. basement membrane of capillaries simple squamous cells of capillaries about. 5 μ in thickness 29
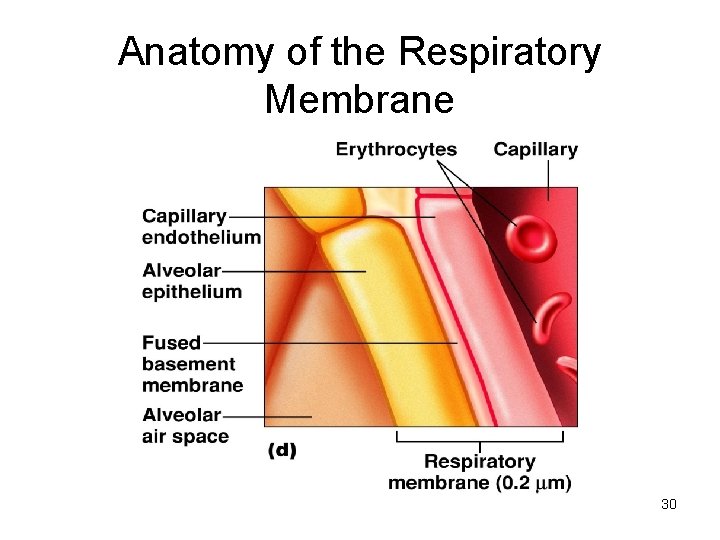
Anatomy of the Respiratory Membrane 30
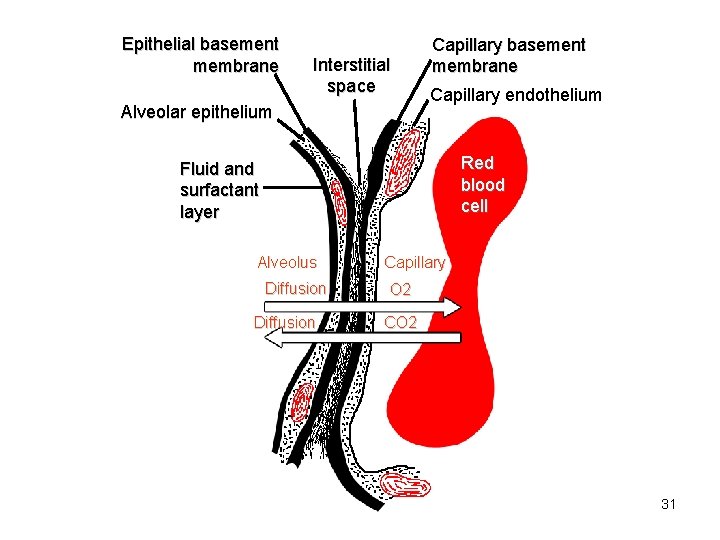
Epithelial basement membrane Interstitial space Alveolar epithelium Capillary basement membrane Capillary endothelium Red blood cell Fluid and surfactant layer Alveolus Diffusion Capillary O 2 CO 2 31

Intersitium/interstial space • Surround, supports, and shapes the alveoli and capillaries • Composed of a gel like substance and collagen fibers • Contains tight space and loose space areas 32

Factors that affect the rate of gas diffusion through the respiratory membrane 1. The thickness of the respiratory membrane is inversely proportional to the rate of diffusion through the membrane. 2. Surface area of the membrane. 33

3. The diffusion rate of the specific gas. Diffusion coefficient for the transfer of each gas through the respiratory membrane depends on its solubility in the membrane and inversely on the square root of its molecular weight. CO 2 diffuses 20 times as rapidly as O 2. 4. The pressure difference between the two sides of the membrane (between the alveoli and in the blood). 34

Pores of Kohn • Small holes in the walls of adjoining alveoli (alveaolar septa) • Between 3 to 13 µ in diameter • Formation of pores may be due to: – Desquamation due to disease – Normal degeneration due to aging – Movement of macrophages leaving holes 35

Blood supply of Lungs • Bronchial circulation – bronchial arteries supply oxygenated blood to lungs, bronchial veins carry away deoxygenated blood from lung tissue. • Pulmonary circulation • Response of two systems to hypoxia – pulmonary vessels undergo vasoconstriction, bronchial vessels like all other systemic vessels undergo vasodilation 36

Bronchial Blood Supply • Bronchial arteries – Arise from thoracic aorta(Anatomic variation is there), usually there are 1 artery for Rt lung and 2 arteries for Lt Lung. – Bronchial arteries run along with the branching bronchi and supply lung tissue except the alveoli. – Much of the blood supplied by Bronchial arteries is Returned via Pulmonary veins rather than bronchial veins. 37

Bronchial arteries • Also nourish – Mediastinal lymph nodes – Pulmonary nerves – Some muscular pulmonary arteries and veins – Portions of the esophagus – Visceral pleura 38

Bronchial venous system • Approx. 1/3 blood returns to right heart – Azygous vien – Hemiazygous vein – Intercostal veins – This blood comes form the first two or three generations of bronchi 39

Bronchial venous return • 2/3 of blood flowing to terminal bronchioles drains into pulmonary circulation via “bronchopulmonary anastomoses” • Then flows to left atrium via pulmonary veins • Contributes to “venous admixture” or “anatomic shunt” (1 -2% of C. O. ) 40
Pulmonary Vascular System • The second source of blood to the lungs • Primary purpose is to deliver blood to lungs for gas exchange • Also delivers nutrients to cells distal to terminal bronchioles • Composed of arteries, arterioles, capllaries, venules, and veins 41

• Pulmonary Trunk arises from the infundibulum of Rt ventricle and divide into Rt and Lt branches. Which carry deoxygenated blood. • Pulmonary arteries branch profusely along with the bronchi leading to capillary network sorrunding the alveoli. • 4 Pulmonary veins(2 from each Lung) form post alveoli to carry oxygenated blood to the Lt Atrium 42

Pulmonary Capillaries • Walls are less than 0. 1µ thick • Total external thickness is about 10µ • Selective permeability to water, electrolytes, sugars • Produce and destroy biologically active substances 43

Nerve Supply • Lung and Pleura are innervated by Anterior and posterior pulmonary plexuses • They are mixed plexuses containing vagal(Parasympethatic) and sympathetic fibers. • Vagus Nerve(Parasympathetic)— Bronchoconstriction, vasodilatation and Secretomotor • Sympathetic Fibres— Bronchodilator, vasocostrictor and inhibitor to the glands of bronchial tree. 44
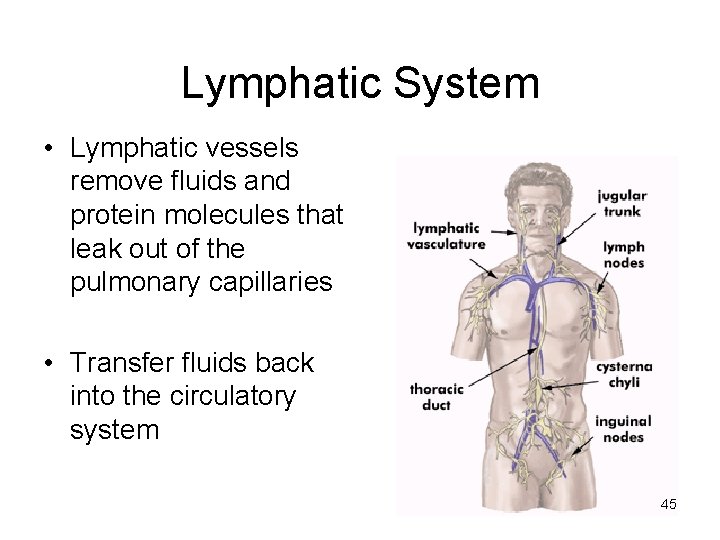
Lymphatic System • Lymphatic vessels remove fluids and protein molecules that leak out of the pulmonary capillaries • Transfer fluids back into the circulatory system 45

Lymphatic Drainage of Lungs • There are 2 sets of Lymphatics, both of which drain into the Bronchopulmonary nodes. • Superficial vessels drain the peripheral lung tissue lying beneth the pulmonary pleura • Deep lymphatics drain the bronchial tree, the pulmonary vessels and connective tissue septa and then run towards the hilum. 46

• Lymphatic vessels of upper lobe end up in superior tracheobronchial node and from lower lobe enters the inferior tracheobronchial nodes. • The tracheobronchial and bronchopulmonary nodes end in the bronchomediastinal lymph trunk • This trunk reaches the thoracic duct on the left and Rt lymphatic duct on the Rt side. 47

Respiratory events • Pulmonary ventilation = exchange of gases between lungs and atmosphere • External respiration = exchange of gases between alveoli and pulmonary capillaries • Internal respiration = exchange of gases between systemic capillaries and tissue cells 48

Breathing • Breathing (pulmonary ventilation). consists of two cyclic phases: • inhalation, also called inspiration - draws gases into the lungs. • exhalation, also called expiration - forces gases out of the lungs. 49
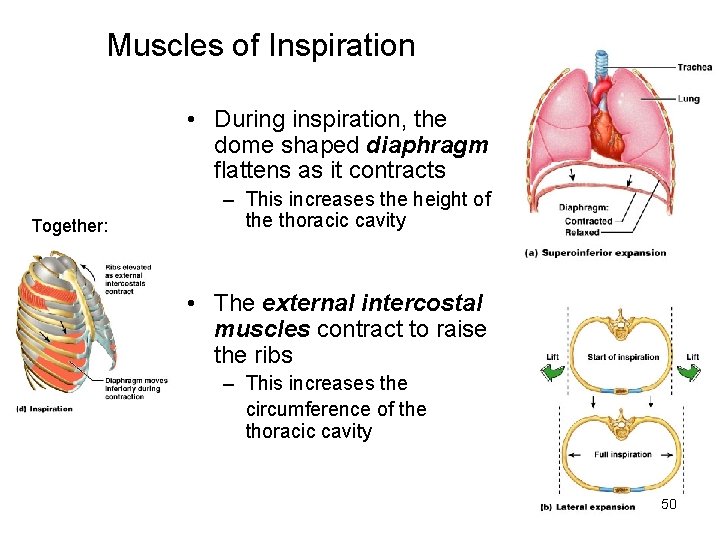
Muscles of Inspiration • During inspiration, the dome shaped diaphragm flattens as it contracts Together: – This increases the height of the thoracic cavity • The external intercostal muscles contract to raise the ribs – This increases the circumference of the thoracic cavity 50

Inspiration continued • Intercostals keep the thorax stiff so sides don’t collapse in with change of diaphragm • During deep or forced inspiration, additional muscles are recruited: – – – Scalenes Sternocleidomastoid Pectoralis minor Quadratus lumborum on 12 th rib Erector spinae (some of these “accessory muscles” of ventilation are visible to an observer; it usually tells you that there is respiratory distress – working hard to breathe) 51
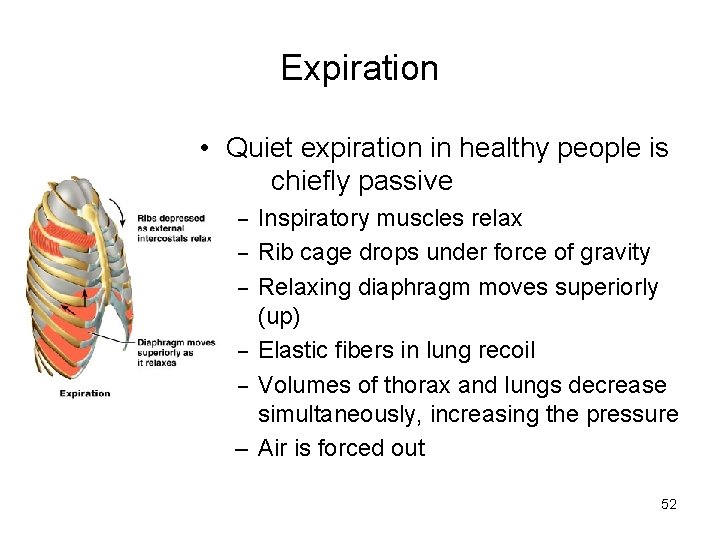
Expiration • Quiet expiration in healthy people is chiefly passive – Inspiratory muscles relax – Rib cage drops under force of gravity – Relaxing diaphragm moves superiorly (up) – Elastic fibers in lung recoil – Volumes of thorax and lungs decrease simultaneously, increasing the pressure – Air is forced out 52

Expiration continued • Forced expiration is active – Contraction of abdominal wall muscles • Oblique and transversus predominantly – Increases intra-abdominal pressure forcing the diaphragm superiorly – Depressing the rib cage, decreases thoracic volume • Some help from internal intercostals and latissimus dorsi (try this on yourself to feel the different muscles acting) 53
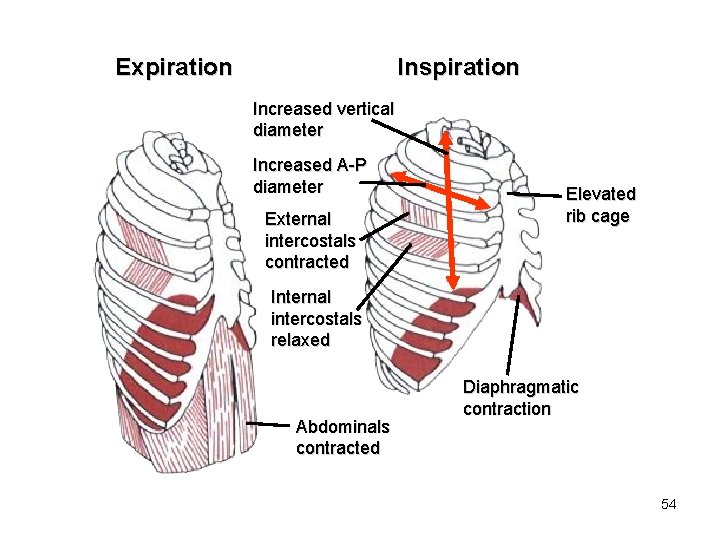
Expiration Inspiration Increased vertical diameter Increased A-P diameter External intercostals contracted Elevated rib cage Internal intercostals relaxed Abdominals contracted Diaphragmatic contraction 54
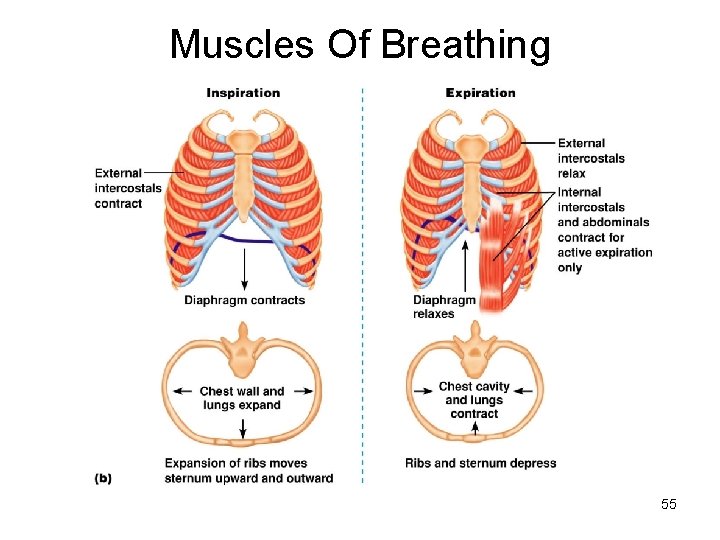
Muscles Of Breathing 55

Boyle’s Law • The pressure of a gas decreases if the volume of the container increases, and vice versa. • When the volume of the thoracic cavity increases even slightly during inhalation, the intrapulmonary pressure decreases slightly, and air flows into the lungs through the conducting airways. Air flows into the lungs from a region of higher pressure (the atmosphere)into a region of lower pressure (the intrapulmonary region). • When the volume of the thoracic cavity decreases during exhalation, the intrapulmonary pressure increases and forces air out of the lungs into the atmosphere. 56

Alveolar pressure: – is the pressure inside the lung alveoli During inspiration: – 1 cm of H 2 O (this slight negative pressure is enough to move about 0. 5 liter of air into the lungs in the first 2 second of inspiration) During expiration: it rises to about +1 cm of H 2 O (this forces 0. 5 liter of inspired air out of the lungs during the 2 to 3 seconds of expiration 57

Compliance of the lungs Definition: the extent to which the lungs expand for each unit increase in transpulmonary pressure (difference between intraalveolar pressure and intra-pleural pressure) ~ 200 ml/cm of H 2 O (each time, the transpulmonary pressure increase by 1 cm of H 2 O, the lungs expand 200 ml) 58
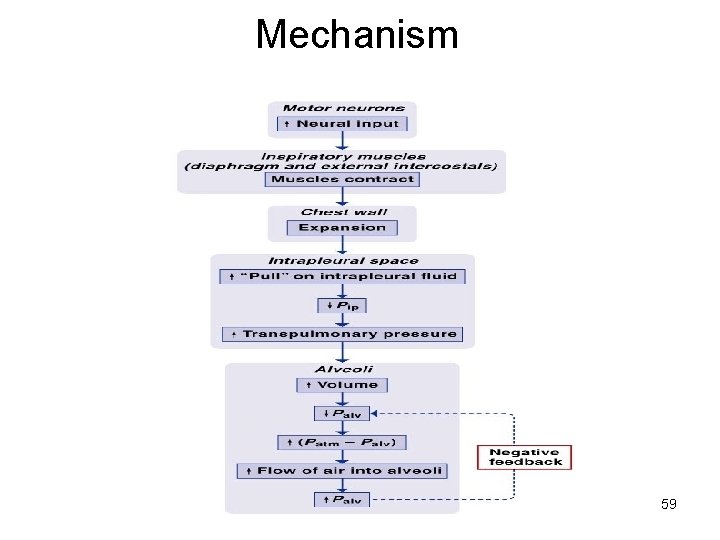
Mechanism 59

Respiratory Values • A normal adult averages 12 breathes per minute = respiratory rate(RR) • Respiratory volumes – determined by using a spirometer 60

LUNG VOLUMES • TIDAL VOLUME (TV): Volume inspired or expired with each normalハbreath. = 500 ml • INSPIRATORY RESERVE VOLUME (IRV): Maximum volume that can be inspired over the inspiration of a tidal volume/normal breath. Used during exercise/exertion. =3100 ml • EXPIRATRY RESERVE VOLUME (ERV): Maximal volume that can be expired after the expiration of a tidal volume/normal breath. = 1200 ml • RESIDUAL VOLUME (RV): Volume that remains in the lungs after a maximal expiration. ハ CANNOT be measured by spirometry. = 1200 ml • RESPIRATORY MINUTE VOLUME : Amount of air inspired per minute. e. g. 500 ml x 12 = 6 Ltr. • Dead Space : Portion of each Tidal volume that does not take part in gas exchange (150 ml). 61

LUNG CAPACITIES • INSPIRATORY CAPACITY ( IC): Volume of maximal inspiration: IRV + TV = 3600 ml • FUNCTIONAL RESIDUAL CAPACITY (FRC): Volume of gas remaining in lung after normal expiration, cannot be measured by spirometry because it includes residual volume: ERV + RV = 2400 ml • VITAL CAPACITY (VC): Volume of maximal inspiration and expiration: IRV + TV + ERV = IC + ERV = 4800 ml • TOTAL LUNG CAPACITY (TLC): The volume of the lung after maximal inspiration. ハ The sum of all four lung volumes, cannot be measured by spirometry because it includes residual volume: IRV+ TV + ERV + RV = IC + FRC = 6000 ml 62
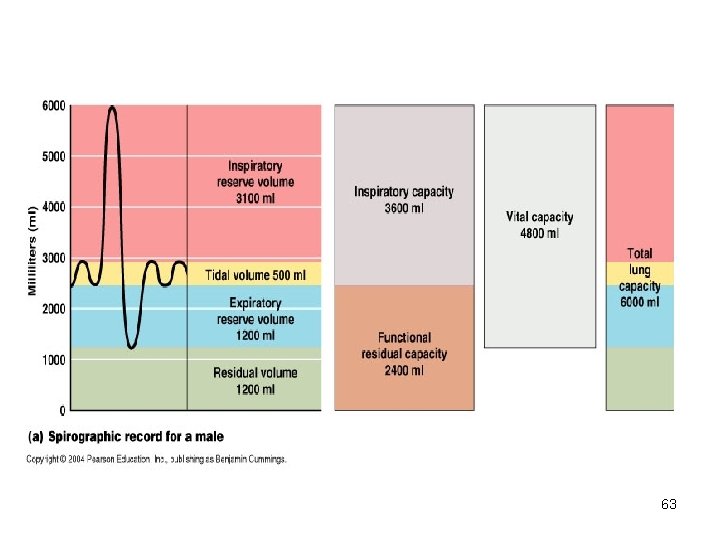
63
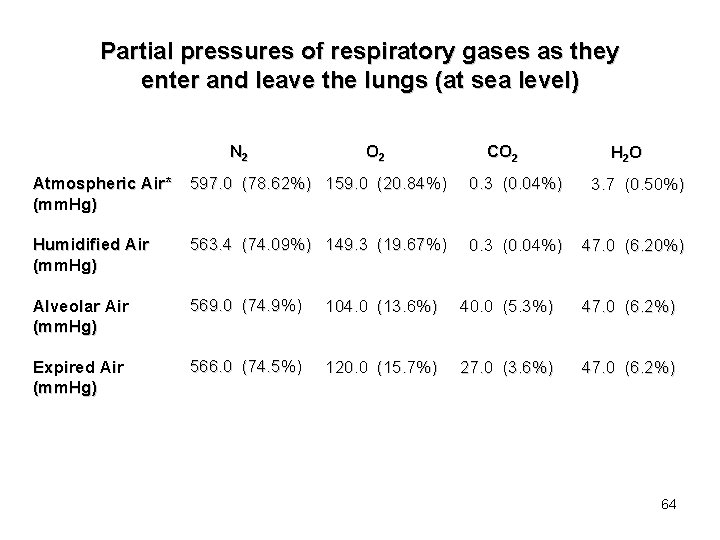
Partial pressures of respiratory gases as they enter and leave the lungs (at sea level) N 2 O 2 CO 2 H 2 O Atmospheric Air* (mm. Hg) 597. 0 (78. 62%) 159. 0 (20. 84%) 0. 3 (0. 04%) 3. 7 (0. 50%) Humidified Air (mm. Hg) 563. 4 (74. 09%) 149. 3 (19. 67%) 0. 3 (0. 04%) 47. 0 (6. 20%) Alveolar Air (mm. Hg) 569. 0 (74. 9%) 104. 0 (13. 6%) 40. 0 (5. 3%) 47. 0 (6. 2%) Expired Air (mm. Hg) 566. 0 (74. 5%) 120. 0 (15. 7%) 27. 0 (3. 6%) 47. 0 (6. 2%) 64

The rate at which alveolar air is renewed by atmospheric air: The amount of air remaining in the lungs at the end of normal expiration ~ 2300 ml (FRC). Only 350 ml of air is brought into the alveoli with each breath. Therefore, the amount of alveolar air is replaced by new atmospheric air with each breath is only 1/7 th of the total. This slow replacement of alveolar air is important in preventing sudden changes in gaseous concentrations in the blood. 65

Ventilation-perfusion ratio (V/Q) It is the ratio of alveolar ventilation to pulmonary blood flow per minute. The alveolar ventilation at rest (4. 2 L/min) and is calculated as: Alveolar ventilation = respiratory rate x (tidal volume – dead space air). The pulmonary blood flow is equal to right ventricular output per minute (5 L/min). This value is an average value across the lung. At the apex, V/Q ratio = 3. At the base, V/Q ratio = 0. 6. So the apex is more ventilated than perfused, and the base is more perfused than ventilated. During exercise, the V/Q ratio becomes more homogenous among different parts of the lung. 66

- Slides: 67