Anatomy of the Skin Rich Callahan MSPA PAC











- Slides: 12

Anatomy of the Skin Rich Callahan MSPA, PA-C ICM I Summer 2009

Before Pathophysiology Comes Anatomy • One of the keys to your knowledge of skin disease is understanding the anatomy of the skin and the particular way a given skin disease affects it. • Anatomy of skin also important during dermatologic procedures like skin biopsy, excisions and ED&C.

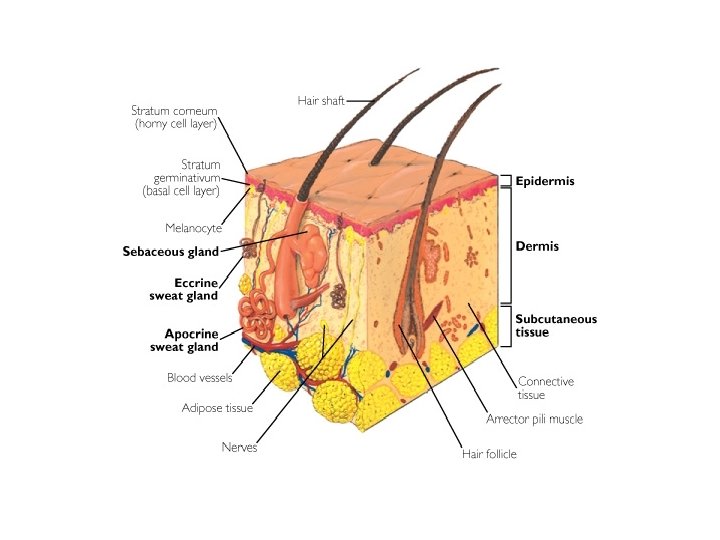
Skin Anatomy – Basic Overview • Skin essentially composed of 3 layers: epidermis, dermis and subcutis (subcutaneous tissue. ) • Epidermis is outermost layer – primarily functional and protective. Subdivided into five layers which migrate upwards and whose purpose is ultimately to form the end layer, or stratum corneum – the outer layer of dead cells that protects us from our environment. Process is called keratinization.

The first function of skin is physical protection from the environment. Protection From: • UV radiation • Physical trauma • Liquids (there is a reason we’re waterproof) • Dehydration • Sudden temperature shifts • Microbes First line of defense is the stratum corneum, which is primarily composed of laminated keratin.

Definition of Keratin (From Taber’s Medical Dictionary) • “A family of durable protein polymers that are found only in epithelial cells. They provide structural strength to skin, hair and nails. The fibrous protein is produced by keratinocytes. ” • Thoroughly understanding the process of keratinization which takes place in the epidermis will unlock answers for many skin diseases because so many of them are disorders of it.

Keratin • Comes from the Greek word “keras” for horn. • The outer layer of epidermis, the stratum corneum, gets its name from the Latin word for horn. • My first question was: Where were the people who make up these names seeing a horn?

Perhaps it is because the phenomenon of cutaneous horn is the most overt keratinizing process • Multiple underlying pathologies can cause a cutaneous horn: • Verruca vulgaris (common wart) • Actinic Keratosis (AK) • Squamous Cell Carcinoma (SCC) • Seborrheic Keratosis (SK) • Psoriasis • Sometimes no underlying pathology is found

Layers of the Epidermis: From Inside to Outside Basal (bottom) layer: A single layer of cells arranged like columns – which divide and turn into the… • Spinous layer (stratum spinosum)whose cells, keratinocytes, begin to form keratin, an insoluble protein critical in later stages. • Granular layer (str. Granulosum) is where cells flatten out and stretch into the • Stratum lucidum and eventually die to form the • Stratum corneum. Old school dermatologists called this the “horny layer” (heh, heh. ) Composed of laminated keratin.

The “Horny Layer” huh? That term has largely been dropped in dermatology but is getting plenty of utilization elsewhere…

Dermis – Divided into 2 layers from top to bottom • Superficial layer is the papillary dermis, a thin layer primarily of collagen fibers. • Arranged in domeshaped inclusions jutting into base of, and feeding small blood vessels into, the epidermis above. • Deep layer is Reticular dermis – composed of thickly layered collagen fibers. • Contains numerous small vessels, cutaneous nerves and apocrine glands.

Subcutis – The Deepest Layer of skin (AKA superficial fascia or hypodermis) • A layer of fat loosely marbled with connective tissue and the deeper parts of apocrine glands. • Important route for small to medium-sized blood vessels, sensory and autonomic nerves, lymphatics. • Deep to this is the deep fascia then skeletal muscle.
