An overview of Zimbabwe National Health Strategy 2016

An over-view of Zimbabwe National Health Strategy 2016 -2020 Tonderai Kadzere Deputy Director, Policy and Planning

Everyone is needed!!! The 58: 65 equation
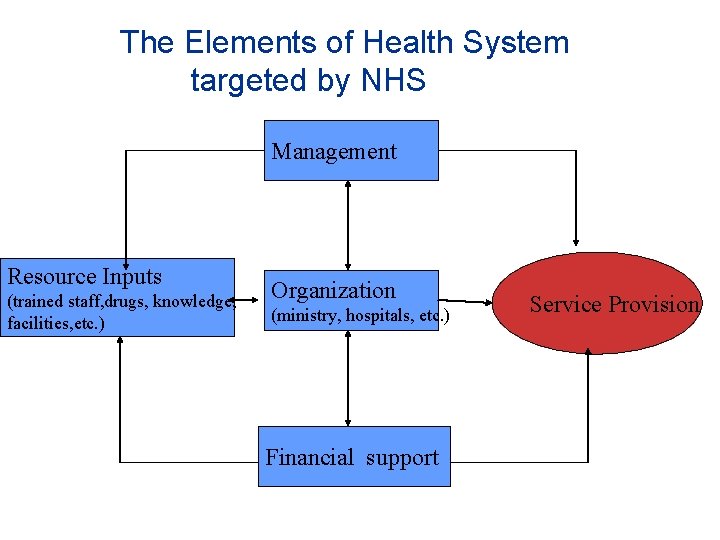
The Elements of Health System targeted by NHS Management Resource Inputs (trained staff, drugs, knowledge, facilities, etc. ) Organization (ministry, hospitals, etc. ) Financial support Service Provision

The NHS Objective: Universal Health Coverage þ All people have access to needed services þ Without the risk of financial ruin linked to paying for care Universal Health Coverage: • coverage with needed health services (of good quality); • coverage with financial risk protection • for all
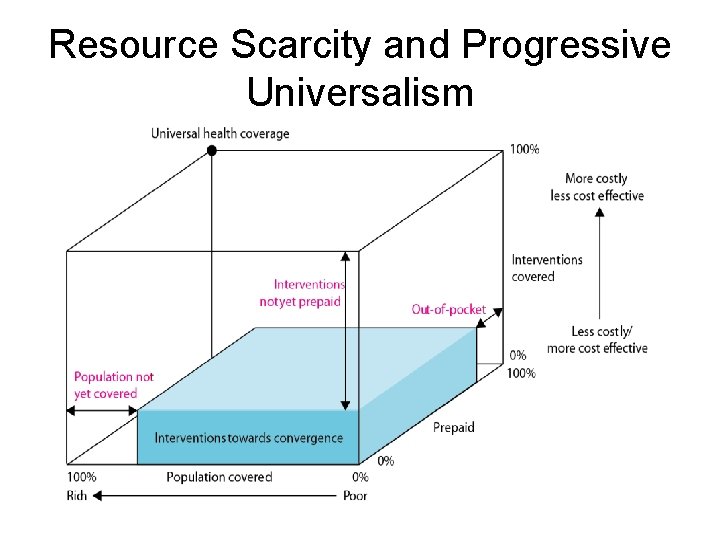
Resource Scarcity and Progressive Universalism

NHS: Key Results Areas 1. Strengthening priority programmes 2. Improving service delivery platforms or entities, and 3. Improving the enabling environment for service delivery

Principles and Values Underpinning the Ministry of Health and Child Care’s vision and mission are the following values: – Equity in health status and health care – Gender equality – Essential quality services – Cost effectiveness – Efficiency – Appropriateness – Social solidarity – Affordability – Client and provider satisfaction – Transparency and accountability – Ownership and partnership in health and; – Continuous Monitoring and evaluation.

The NHS 2016 -2010 –Dismissing the notion of telling the same story differently

Priority 1: Communicable Diseases Goals Objectives Strategies Goal 1: To reduce malaria incidence from 39/1000 in 2014 to 5/1000 in 2020 and malaria deaths to near zero by 2020 1. 1. To maintain universal access of the population at risk to effective and appropriate malaria prevention interventions by 2020 Improve Vector control through Indoor Residual Spraying (IRS) and use of Long Lasting Insecticide Treated Nets (LLIN) Larval source management, personal protection 1. 2. To ensure prompt and appropriate management of all malaria cases by 2020 Strengthening Case management (diagnostic, medicines, supportive care) at all levels Improved surveillance systems, monitoring, evaluation and research Increase the number of districts in pre-elimination phase (increasing surveillance) 1. 3 To enhance Pre elimination activities
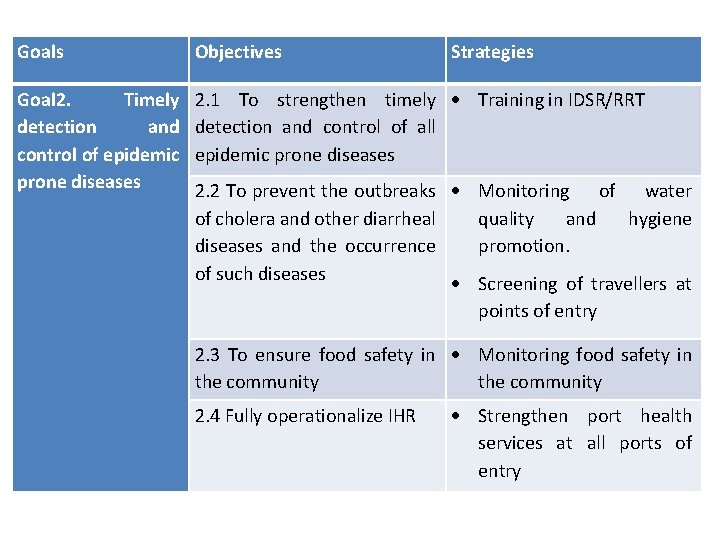
Goals Objectives Strategies Goal 2. Timely detection and control of epidemic prone diseases 2. 1 To strengthen timely Training in IDSR/RRT detection and control of all epidemic prone diseases 2. 2 To prevent the outbreaks Monitoring of water of cholera and other diarrheal quality and hygiene diseases and the occurrence promotion. of such diseases Screening of travellers at points of entry 2. 3 To ensure food safety in Monitoring food safety in the community 2. 4 Fully operationalize IHR Strengthen port health services at all ports of entry
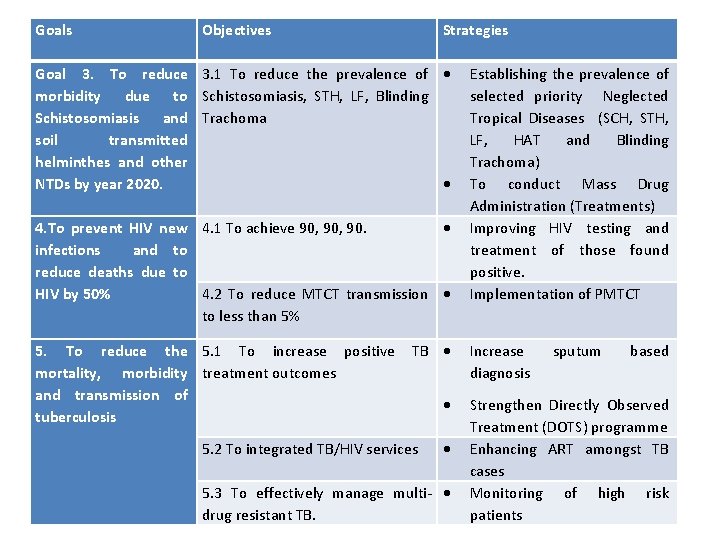
Goals Objectives Strategies Goal 3. To reduce morbidity due to Schistosomiasis and soil transmitted helminthes and other NTDs by year 2020. 3. 1 To reduce the prevalence of Schistosomiasis, STH, LF, Blinding Trachoma 4. To prevent HIV new 4. 1 To achieve 90, 90. infections and to reduce deaths due to HIV by 50% 4. 2 To reduce MTCT transmission to less than 5% 5. To reduce the 5. 1 To increase positive TB mortality, morbidity treatment outcomes and transmission of tuberculosis 5. 2 To integrated TB/HIV services 5. 3 To effectively manage multi- drug resistant TB. Establishing the prevalence of selected priority Neglected Tropical Diseases (SCH, STH, LF, HAT and Blinding Trachoma) To conduct Mass Drug Administration (Treatments) Improving HIV testing and treatment of those found positive. Implementation of PMTCT Increase diagnosis sputum based Strengthen Directly Observed Treatment (DOTS) programme Enhancing ART amongst TB cases Monitoring of high risk patients
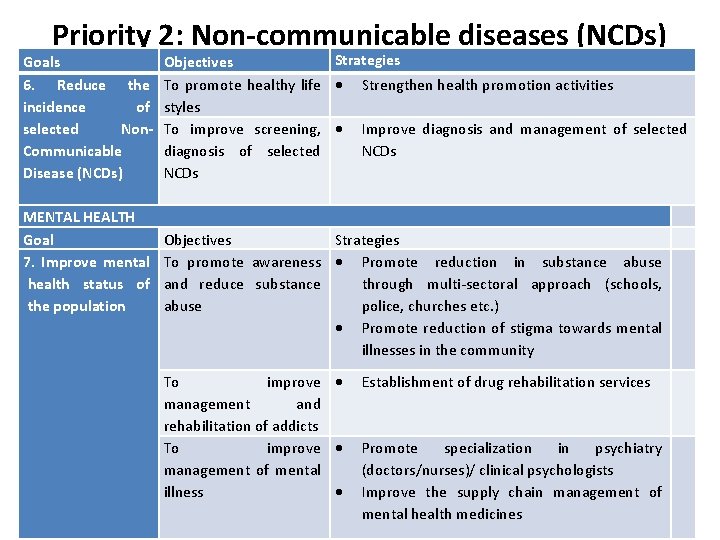
Priority 2: Non-communicable diseases (NCDs) Goals 6. Reduce the incidence of selected Non. Communicable Disease (NCDs) MENTAL HEALTH Goal 7. Improve mental health status of the population Strategies Objectives To promote healthy life Strengthen health promotion activities styles To improve screening, Improve diagnosis and management of selected diagnosis of selected NCDs Objectives Strategies To promote awareness Promote reduction in substance abuse and reduce substance through multi-sectoral approach (schools, abuse police, churches etc. ) Promote reduction of stigma towards mental illnesses in the community To improve management and rehabilitation of addicts To improve management of mental illness Establishment of drug rehabilitation services Promote specialization in psychiatry (doctors/nurses)/ clinical psychologists Improve the supply chain management of mental health medicines
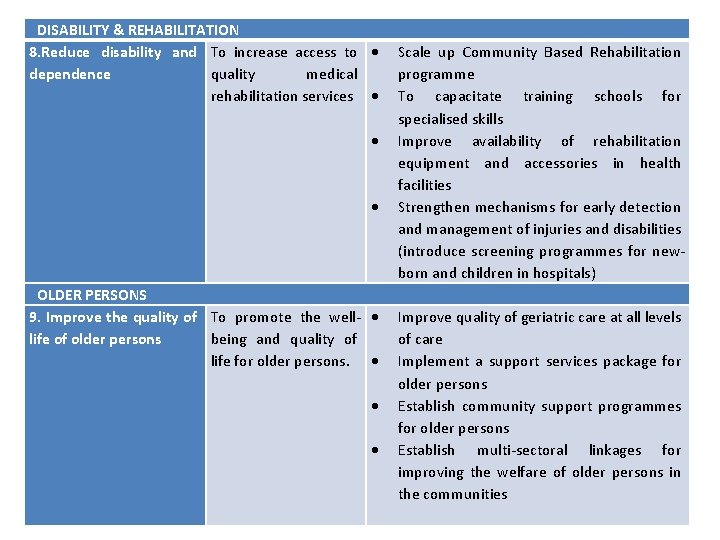
DISABILITY & REHABILITATION 8. Reduce disability and To increase access to dependence quality medical rehabilitation services Scale up Community Based Rehabilitation programme To capacitate training schools for specialised skills Improve availability of rehabilitation equipment and accessories in health facilities Strengthen mechanisms for early detection and management of injuries and disabilities (introduce screening programmes for newborn and children in hospitals) OLDER PERSONS 9. Improve the quality of To promote the well- life of older persons being and quality of life for older persons. Improve quality of geriatric care at all levels of care Implement a support services package for older persons Establish community support programmes for older persons Establish multi-sectoral linkages for improving the welfare of older persons in the communities

Priority 3: Reproductive, Maternal, Newborn, Child Health & Adolescents Goals Objectives Strategies 10 Reduce maternal To increase early and mortality ratio from continuous utilization of 614 to 300 by 2020 ANC services Advocacy and Communication for maternal health services RBF- pay for service conditional to quality of service (incentivizing VHW/PCN based on referrals) To set up focused quality improvement systems To increase the consistent provision of quality ANC services Strengthen on the job training, support and supervision and mentorship Institute client feedback mechanisms Further decentralization of services including infrastructure, health posts and community and supplies
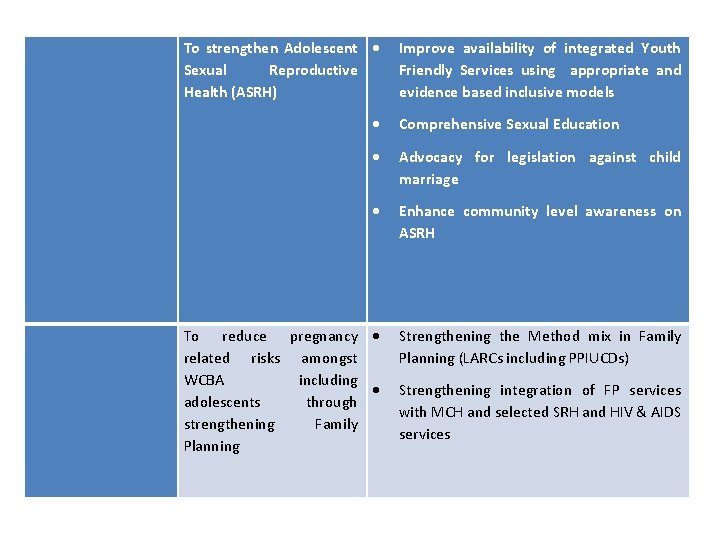
To strengthen Adolescent Sexual Reproductive Health (ASRH) Improve availability of integrated Youth Friendly Services using appropriate and evidence based inclusive models Comprehensive Sexual Education Advocacy for legislation against child marriage Enhance community level awareness on ASRH To reduce pregnancy related risks amongst WCBA including adolescents through strengthening Family Planning Strengthening the Method mix in Family Planning (LARCs including PPIUCDs) Strengthening integration of FP services with MCH and selected SRH and HIV & AIDS services
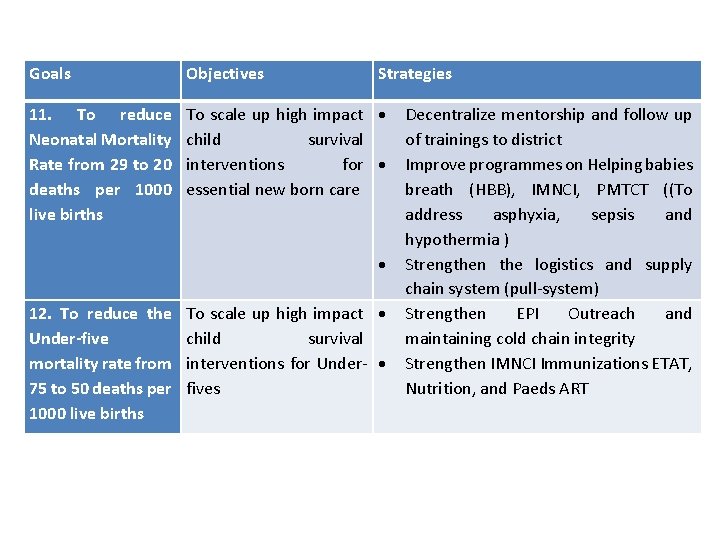
Goals Objectives 11. To reduce Neonatal Mortality Rate from 29 to 20 deaths per 1000 live births To scale up high impact child survival interventions for essential new born care 12. To reduce the Under-five mortality rate from 75 to 50 deaths per 1000 live births Strategies To scale up high impact child survival interventions for Under- fives Decentralize mentorship and follow up of trainings to district Improve programmes on Helping babies breath (HBB), IMNCI, PMTCT ((To address asphyxia, sepsis and hypothermia ) Strengthen the logistics and supply chain system (pull-system) Strengthen EPI Outreach and maintaining cold chain integrity Strengthen IMNCI Immunizations ETAT, Nutrition, and Paeds ART
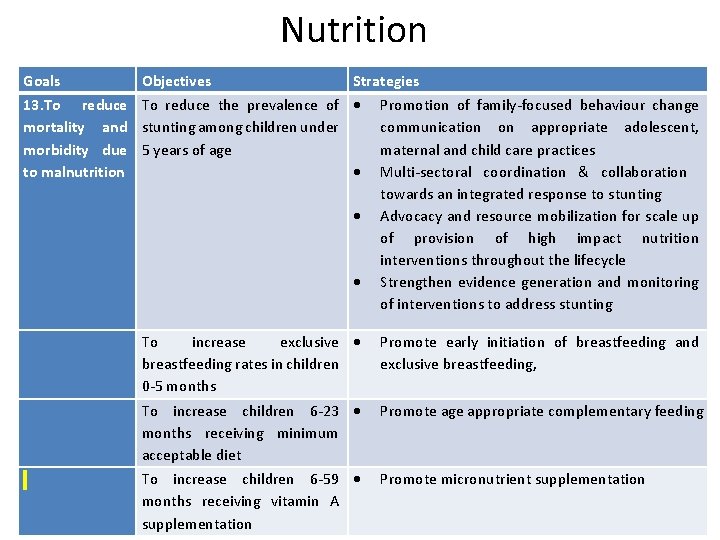
Nutrition Goals Objectives Strategies 13. To reduce mortality and morbidity due to malnutrition To reduce the prevalence of stunting among children under 5 years of age Promotion of family-focused behaviour change communication on appropriate adolescent, maternal and child care practices Multi-sectoral coordination & collaboration towards an integrated response to stunting Advocacy and resource mobilization for scale up of provision of high impact nutrition interventions throughout the lifecycle Strengthen evidence generation and monitoring of interventions to address stunting To increase exclusive breastfeeding rates in children 0 -5 months Promote early initiation of breastfeeding and exclusive breastfeeding, To increase children 6 -23 months receiving minimum acceptable diet Promote age appropriate complementary feeding To increase children 6 -59 months receiving vitamin A supplementation Promote micronutrient supplementation
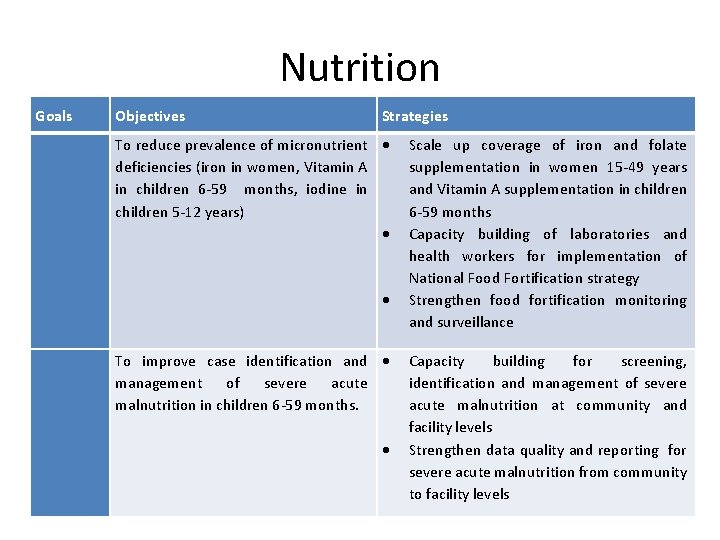
Nutrition Goals Objectives Strategies To reduce prevalence of micronutrient deficiencies (iron in women, Vitamin A in children 6 -59 months, iodine in children 5 -12 years) To improve case identification and management of severe acute malnutrition in children 6 -59 months. Scale up coverage of iron and folate supplementation in women 15 -49 years and Vitamin A supplementation in children 6 -59 months Capacity building of laboratories and health workers for implementation of National Food Fortification strategy Strengthen food fortification monitoring and surveillance Capacity building for screening, identification and management of severe acute malnutrition at community and facility levels Strengthen data quality and reporting for severe acute malnutrition from community to facility levels
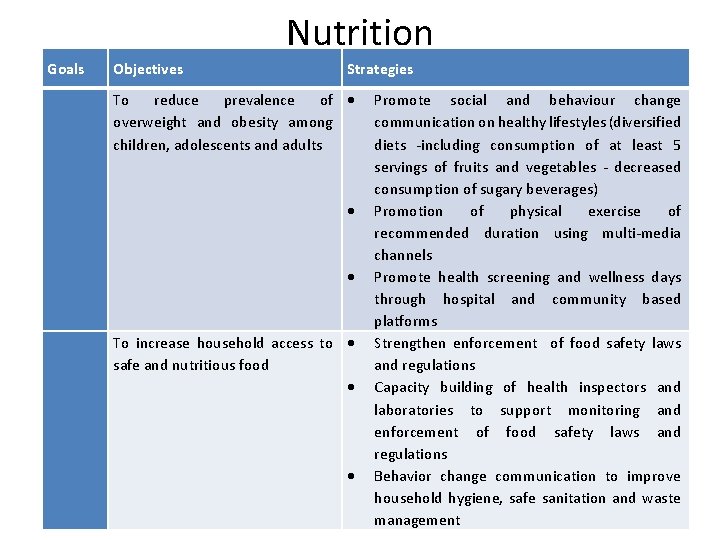

Nutrition Goals Objectives Strategies To reduce prevalence of overweight and obesity among children, adolescents and adults To increase household access to safe and nutritious food Promote social and behaviour change communication on healthy lifestyles (diversified diets -including consumption of at least 5 servings of fruits and vegetables - decreased consumption of sugary beverages) Promotion of physical exercise of recommended duration using multi-media channels Promote health screening and wellness days through hospital and community based platforms Strengthen enforcement of food safety laws and regulations Capacity building of health inspectors and laboratories to support monitoring and enforcement of food safety laws and regulations Behavior change communication to improve household hygiene, safe sanitation and waste management
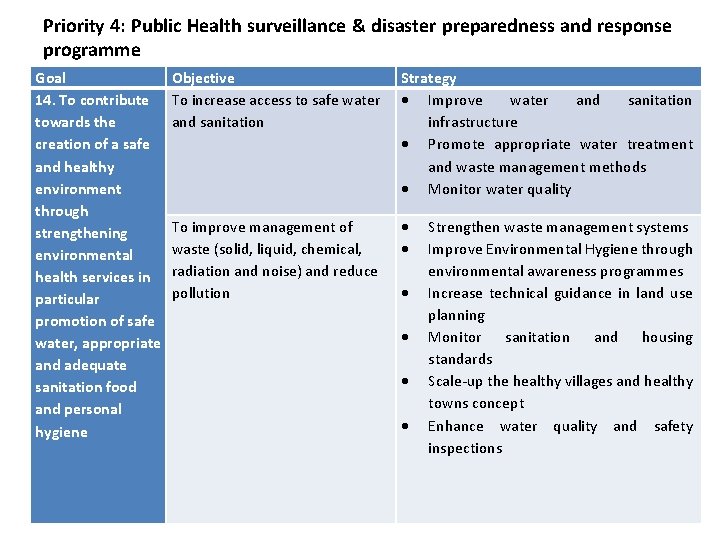
Priority 4: Public Health surveillance & disaster preparedness and response programme Goal 14. To contribute towards the creation of a safe and healthy environment through strengthening environmental health services in particular promotion of safe water, appropriate and adequate sanitation food and personal hygiene Objective To increase access to safe water and sanitation Strategy Improve water and sanitation infrastructure Promote appropriate water treatment and waste management methods Monitor water quality To improve management of waste (solid, liquid, chemical, radiation and noise) and reduce pollution Strengthen waste management systems Improve Environmental Hygiene through environmental awareness programmes Increase technical guidance in land use planning Monitor sanitation and housing standards Scale-up the healthy villages and healthy towns concept Enhance water quality and safety inspections
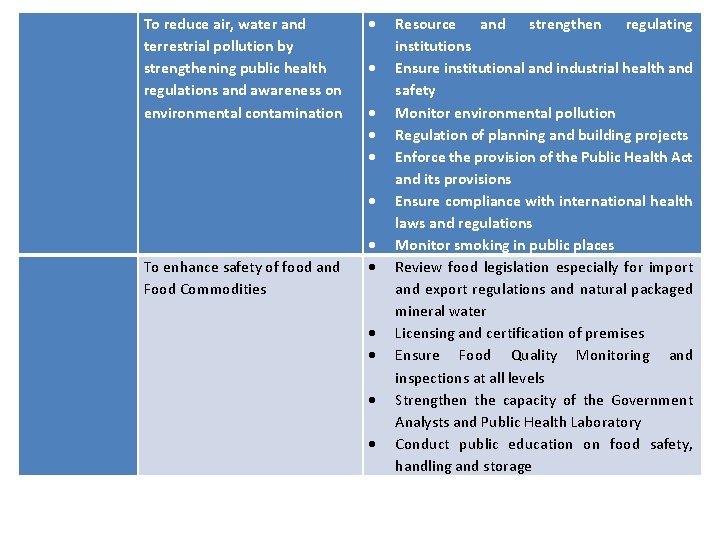

To reduce air, water and terrestrial pollution by strengthening public health regulations and awareness on environmental contamination To enhance safety of food and Food Commodities Resource and strengthen regulating institutions Ensure institutional and industrial health and safety Monitor environmental pollution Regulation of planning and building projects Enforce the provision of the Public Health Act and its provisions Ensure compliance with international health laws and regulations Monitor smoking in public places Review food legislation especially for import and export regulations and natural packaged mineral water Licensing and certification of premises Ensure Food Quality Monitoring and inspections at all levels Strengthen the capacity of the Government Analysts and Public Health Laboratory Conduct public education on food safety, handling and storage
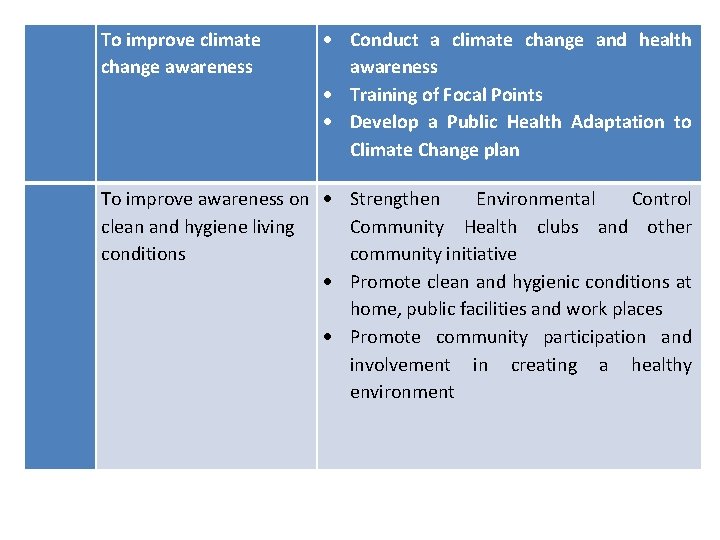
To improve climate change awareness Conduct a climate change and health awareness Training of Focal Points Develop a Public Health Adaptation to Climate Change plan To improve awareness on Strengthen Environmental Control clean and hygiene living Community Health clubs and other conditions community initiative Promote clean and hygienic conditions at home, public facilities and work places Promote community participation and involvement in creating a healthy environment

Service Delivery Platforms/Entities
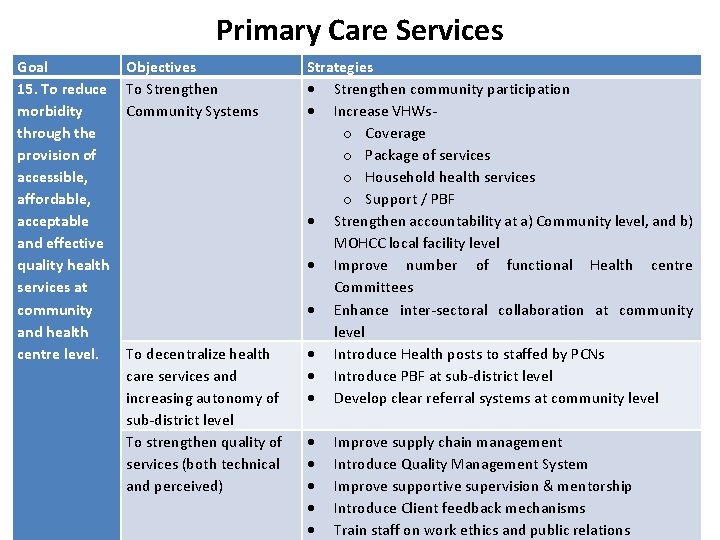
Primary Care Services Goal 15. To reduce morbidity through the provision of accessible, affordable, acceptable and effective quality health services at community and health centre level. Objectives To Strengthen Community Systems To decentralize health care services and increasing autonomy of sub-district level To strengthen quality of services (both technical and perceived) Strategies Strengthen community participation Increase VHWso Coverage o Package of services o Household health services o Support / PBF Strengthen accountability at a) Community level, and b) MOHCC local facility level Improve number of functional Health centre Committees Enhance inter-sectoral collaboration at community level Introduce Health posts to staffed by PCNs Introduce PBF at sub-district level Develop clear referral systems at community level Improve supply chain management Introduce Quality Management System Improve supportive supervision & mentorship Introduce Client feedback mechanisms Train staff on work ethics and public relations
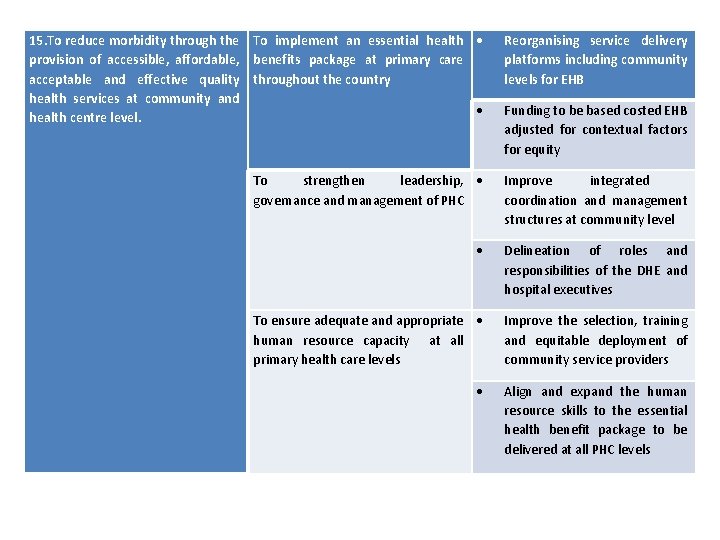
15. To reduce morbidity through the To implement an essential health provision of accessible, affordable, benefits package at primary care acceptable and effective quality throughout the country health services at community and health centre level. Reorganising service delivery platforms including community levels for EHB Funding to be based costed EHB adjusted for contextual factors for equity To strengthen leadership, governance and management of PHC Improve integrated coordination and management structures at community level Delineation of roles and responsibilities of the DHE and hospital executives To ensure adequate and appropriate human resource capacity at all primary health care levels Improve the selection, training and equitable deployment of community service providers Align and expand the human resource skills to the essential health benefit package to be delivered at all PHC levels
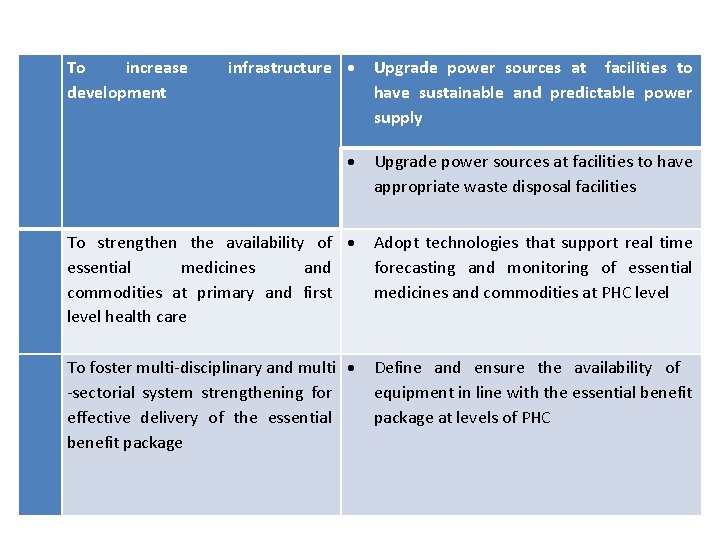
infrastructure Upgrade power sources at facilities to have sustainable and predictable power supply Upgrade power sources at facilities to have appropriate waste disposal facilities To strengthen the availability of essential medicines and commodities at primary and first level health care Adopt technologies that support real time forecasting and monitoring of essential medicines and commodities at PHC level To foster multi-disciplinary and multi -sectorial system strengthening for effective delivery of the essential benefit package Define and ensure the availability of equipment in line with the essential benefit package at levels of PHC To increase development
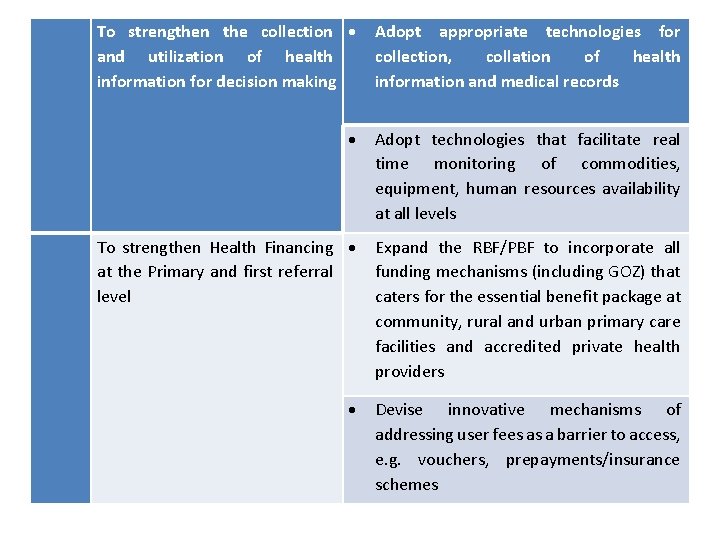
To strengthen the collection and utilization of health information for decision making Adopt appropriate technologies for collection, collation of health information and medical records Adopt technologies that facilitate real time monitoring of commodities, equipment, human resources availability at all levels To strengthen Health Financing at the Primary and first referral level Expand the RBF/PBF to incorporate all funding mechanisms (including GOZ) that caters for the essential benefit package at community, rural and urban primary care facilities and accredited private health providers Devise innovative mechanisms of addressing user fees as a barrier to access, e. g. vouchers, prepayments/insurance schemes

Hospital Services GOAL Objectives Strategies 16 To ensure access and provision of complementary package of emergency and ambulatory curative services To ensure efficient and effective leadership and corporate governance in district hospitals To improve generation, mobilization and allocation of resources at hospitals To increase the availability of medicines and health commodities in hospitals Monitoring of hospital boards according to corporate governance principles Establish Quality Management System Ensure efficient equitable allocation of available resources Ensure efficient collection of funds owed Improve resource mobilization at hospital level Utilize HMTCs and VEN system for prioritization on procurement of medicines and health commodities. Allocate and ring-fence funding for blood and payment to NBSZ Capacitate Nat. Pharm with skills for hospital pooled procurement
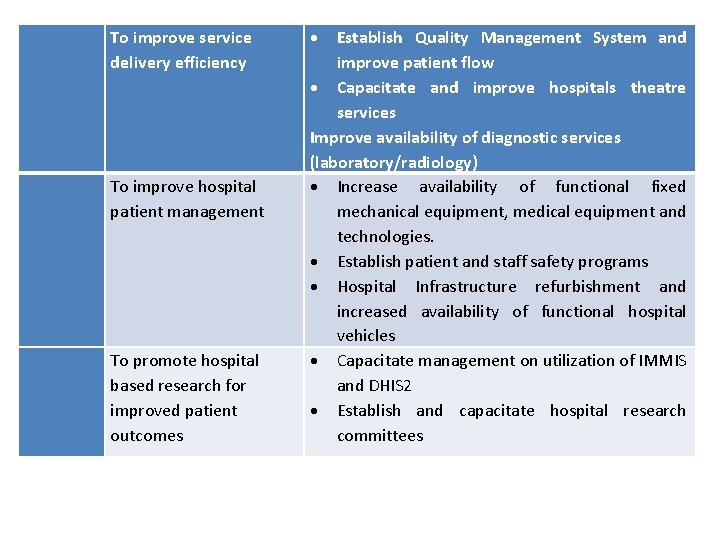
To improve service delivery efficiency To improve hospital patient management To promote hospital based research for improved patient outcomes Establish Quality Management System and improve patient flow Capacitate and improve hospitals theatre services Improve availability of diagnostic services (laboratory/radiology) Increase availability of functional fixed mechanical equipment, medical equipment and technologies. Establish patient and staff safety programs Hospital Infrastructure refurbishment and increased availability of functional hospital vehicles Capacitate management on utilization of IMMIS and DHIS 2 Establish and capacitate hospital research committees
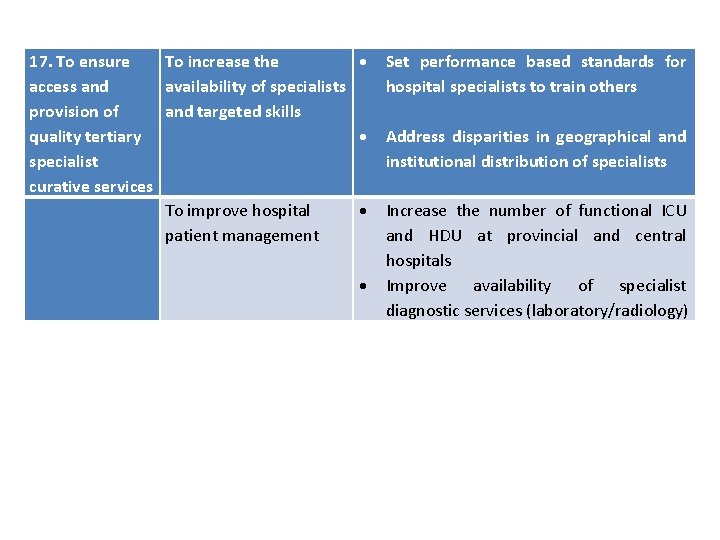
17. To ensure access and provision of quality tertiary specialist curative services To increase the Set performance based standards for availability of specialists hospital specialists to train others and targeted skills Address disparities in geographical and institutional distribution of specialists To improve hospital patient management Increase the number of functional ICU and HDU at provincial and central hospitals Improve availability of specialist diagnostic services (laboratory/radiology)

Enabling Environment for Service Delivery
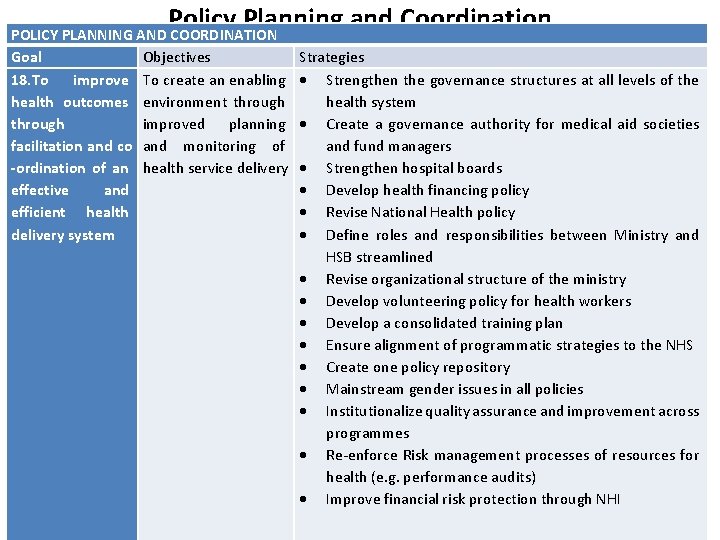
Policy Planning and Coordination POLICY PLANNING AND COORDINATION Goal Objectives 18. To improve To create an enabling health outcomes environment through improved planning facilitation and co and monitoring of -ordination of an health service delivery effective and efficient health delivery system Strategies Strengthen the governance structures at all levels of the health system Create a governance authority for medical aid societies and fund managers Strengthen hospital boards Develop health financing policy Revise National Health policy Define roles and responsibilities between Ministry and HSB streamlined Revise organizational structure of the ministry Develop volunteering policy for health workers Develop a consolidated training plan Ensure alignment of programmatic strategies to the NHS Create one policy repository Mainstream gender issues in all policies Institutionalize quality assurance and improvement across programmes Re-enforce Risk management processes of resources for health (e. g. performance audits) Improve financial risk protection through NHI
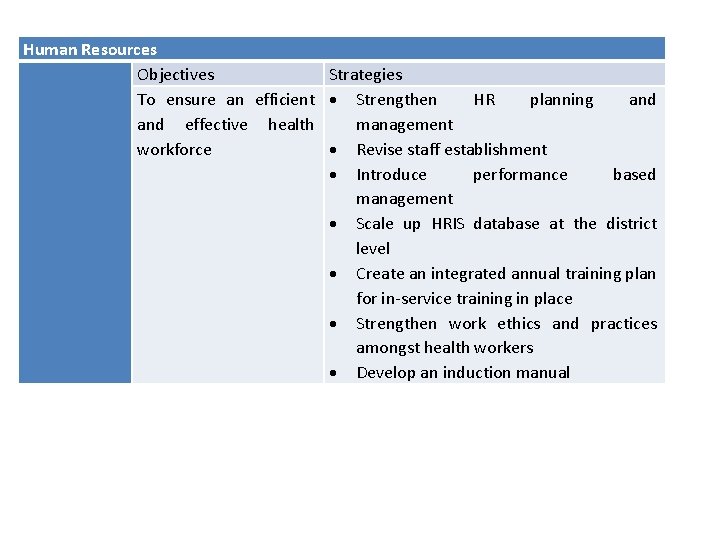
Human Resources Objectives Strategies To ensure an efficient Strengthen HR planning and effective health management workforce Revise staff establishment Introduce performance based management Scale up HRIS database at the district level Create an integrated annual training plan for in-service training in place Strengthen work ethics and practices amongst health workers Develop an induction manual

Finance and Administration To implement accountable, effective and transparent management systems at all levels of the health sector Ensure alignment of Mo. HCC financial management system to the PFM Act and its regulations Strengthen coordination of development partners funding Introduce PBB across districts Safeguard and ensure optimum use of resources through audits Introduce a resource allocation formula Introduce compulsory maintenance plans and budgets for equipment and infrastructure Conduct NHA studies Continuous resource mobilization for the health sector
Monitoring and Evaluation To enhance performance and accountability Provincial Administration To ensure effective policy implementation at provincial level Institutionalize an Framework for the NHS M&E Strengthen coordination between National and provincial level Clearly define roles and activities between provincial and national supervision teams Ensure integrated supportive supervisions per district Strengthen provincial health team review meetings Strengthen monitoring and evaluation of RBM
Multi-Sectoral Partnerships 19. To To strengthen intergovernmental collaboration with local and international partners Support existing national and sub-national structures for inter-governmental interactions Creating a framework for funding health and health related activities across ministries Mainstream “health-in-all” policies across sector ministries Harmonisation of health services at local government level Improved funding for local government health services To improve public-private sector collaborations in funding and provision of health services Develop a policy on public/private partnerships Develop appropriate regulations to facilitate private sector involvement in providing services for public purpose
To enhance collaboration with development partners To strengthen community participation Strengthen existing platforms for donor coordination Develop guidelines for partner involvement in health development Develop a policy and strategy for community participation and involvement Empowering health workers with tools for effective community engagement Strengthen existing local structures for community involvement Empower communities through implementation of Patient Charter Create multi-channels and opportunities community participation at all levels for

Research and Development Goals 20. Conduct scientific research that promotes evidenced based decision making and policy development. Objectives Strategies To establish an essential national Conduct consultative process for health research agenda for the establishing a national health country research agenda To develop human capacity for health research development Research capacity building at all levels (national, provincial, district and community levels) To promote getting research into policy, practice and product Convening results sharing fora or mechanisms at various levels To conduct research (including surveys) on priority health issues Research approval system informed by national health priorities Collaborative projects with other institutions and investigators including practitioners Promoting research excellence (MRCZ, ZIPHA, etc. )
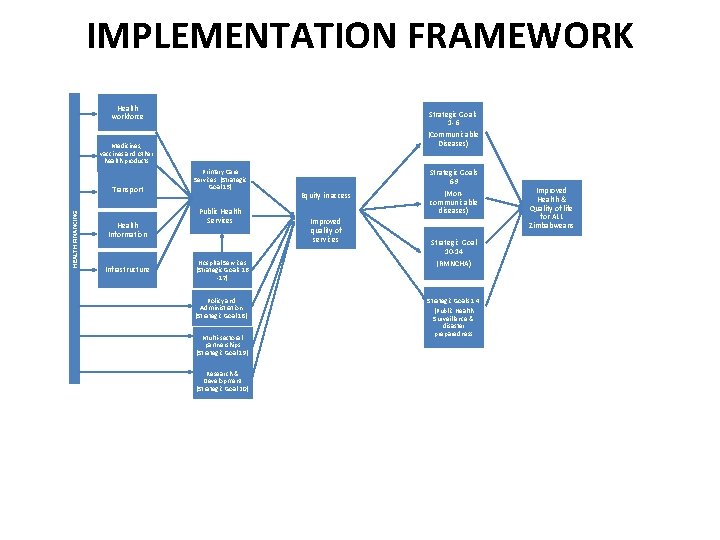
IMPLEMENTATION FRAMEWORK Health workforce Strategic Goals 1 -6 (Communicable Diseases) Medicines, vaccines and other health products HEALTH FINANCING Transport Health Information Infrastructure Primary Care Services (Strategic Goal 15) Public Health Services Hospital Services (Strategic Goals 16 -17) Policy and Administration (Strategic Goal 18) Multi-sectoral partnerships (Strategic Goal 19) Research & Development (Strategic Goal 20) Strategic Goals 6 -9 Equity in access Improved quality of services (Moncommunicable diseases) Strategic Goal 10 -14 (RMNCHA) Strategic Goals 1 4 (Public Health Surveillance & disaster preparedness Improved Health & Quality of life for ALL Zimbabweans

NHS COSTED
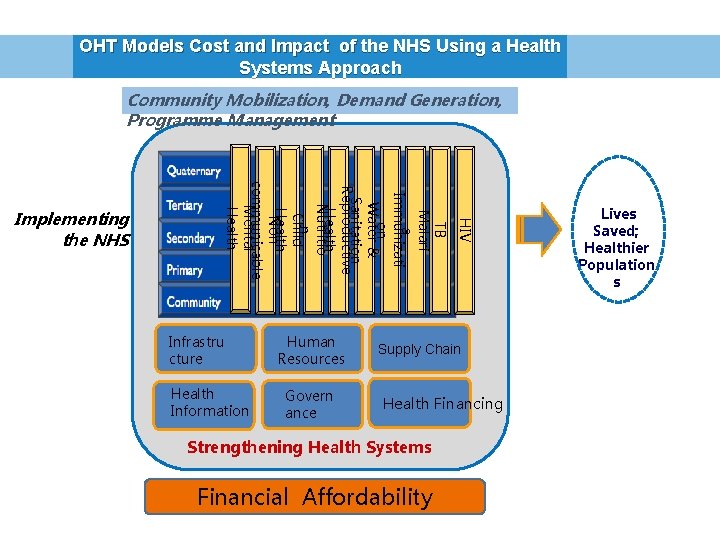
OHT Models Cost and Impact of the NHS Using a Health Systems Approach Community Mobilization, Demand Generation, Programme Management Infrastru cture Health Information Human Resources Govern ance HIV TB Malari a Immunizati on Water & Sanitation Reproductive Health Nutritio n Child Health Non communicable Mental Health Implementing the NHS Supply Chain Health Financing Strengthening Health Systems Financial Affordability Lives Saved; Healthier Population s

NHS Services and System Components Costed by the One Health Tool Disease Programme • • RMNCHA Immunization Malaria TB HIV/AIDS Nutrition Environmental Health and WASH • Non-communicable diseases • Mental Health • Other Communicable Disease (Rabies, Anthrax, Other HSS Component Costed • Governance • HR (Admin and Service Delivery) • Logistics • Infrastructure include Blood Safety, Labs • Health Information System 4 2

3 NHS scenarios NHS 1: "Baseline" Maintain 2015 coverage levels for all health interventions • No change in health service and health system coverage • No change in investments • Flat-lined coverage of health services • No capital investments (e. g. construction of additional health facilities NHS 2: "High Impact interventions" Reduce mortality associated with the 20 established leading causes within limits of the proposed financial space • Scale-up of reproductive and MCH, Malaria, HIV, Nutrition and NCDs interventions with emphasis on lower levels of care • Shift provision of preventive services at the primary health level • Infrastructure improvements at the primary level only • Investments to improve availability and security of medicines and supplies • Capacitation of skilled Human Resources NHS 3: "Optimal scenario" Scale up optimally most health service interventions • Health service and health system investments implemented as planned • All proposed Infrastructure (construction and renovation of health facilities at all the levels) incorporated • All planned HR improvements factored into this model (facilities and admin staff recruitments and training)
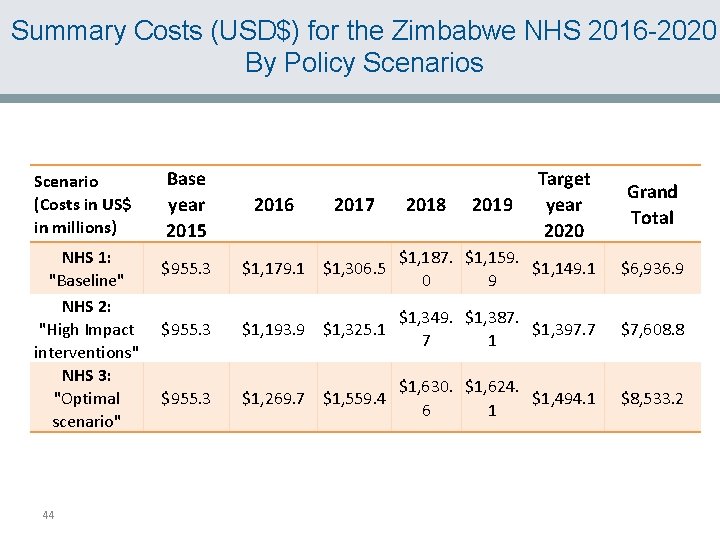
Summary Costs (USD$) for the Zimbabwe NHS 2016 -2020 By Policy Scenarios Scenario (Costs in US$ in millions) NHS 1: "Baseline" NHS 2: "High Impact interventions" NHS 3: "Optimal scenario" 44 Base year 2015 2016 2017 2018 2019 Target year 2020 Grand Total $955. 3 $1, 179. 1 $1, 306. 5 $1, 187. $1, 159. $1, 149. 1 0 9 $6, 936. 9 $955. 3 $1, 193. 9 $1, 325. 1 $1, 349. $1, 387. $1, 397. 7 7 1 $7, 608. 8 $955. 3 $1, 269. 7 $1, 559. 4 $1, 630. $1, 624. $1, 494. 1 6 1 $8, 533. 2
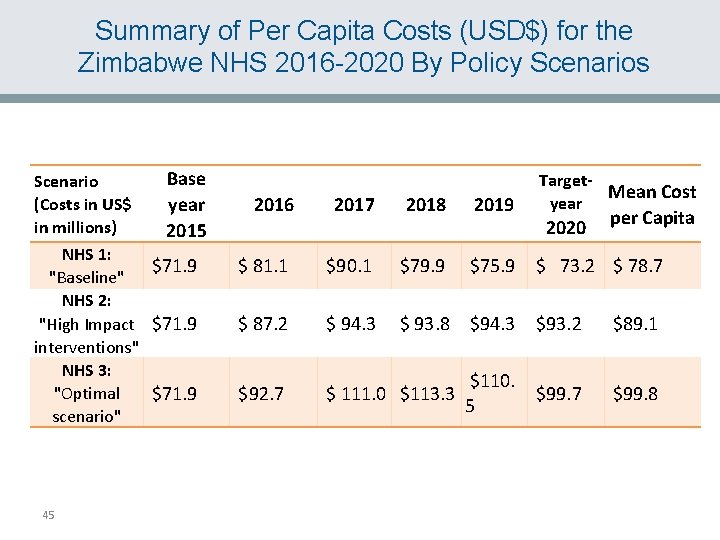
Summary of Per Capita Costs (USD$) for the Zimbabwe NHS 2016 -2020 By Policy Scenarios Base Scenario (Costs in US$ year in millions) 2015 NHS 1: $71. 9 "Baseline" NHS 2: "High Impact $71. 9 interventions" NHS 3: "Optimal $71. 9 scenario" 45 2016 2017 2018 2019 Target. Mean Cost year 2020 per Capita $ 81. 1 $90. 1 $79. 9 $75. 9 $ 73. 2 $ 78. 7 $ 87. 2 $ 94. 3 $ 93. 8 $94. 3 $93. 2 $89. 1 $92. 7 $ 111. 0 $113. 3 $110. $99. 7 5 $99. 8
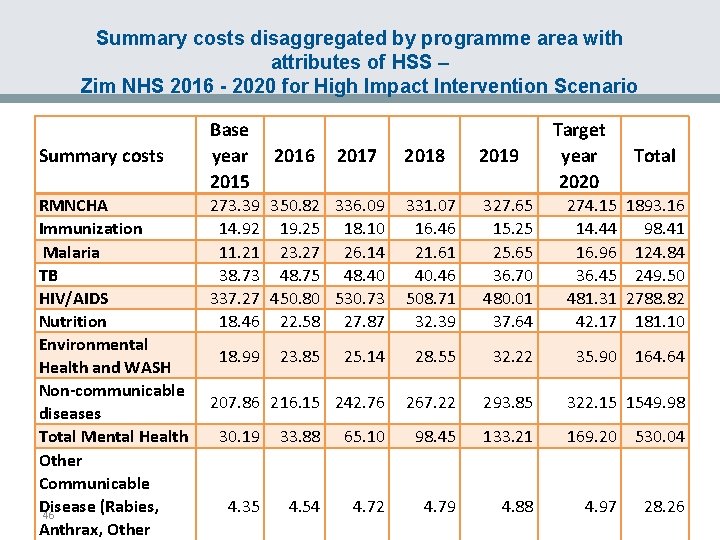
Summary costs disaggregated by programme area with attributes of HSS – Zim NHS 2016 - 2020 for High Impact Intervention Scenario Summary costs RMNCHA Immunization Malaria TB HIV/AIDS Nutrition Environmental Health and WASH Non-communicable diseases Total Mental Health Other Communicable Disease (Rabies, 46 Anthrax, Other Base year 2015 2016 2017 Target year 2020 2018 2019 331. 07 16. 46 21. 61 40. 46 508. 71 32. 39 327. 65 15. 25 25. 65 36. 70 480. 01 37. 64 25. 14 28. 55 32. 22 35. 90 164. 64 207. 86 216. 15 242. 76 267. 22 293. 85 322. 15 1549. 98 169. 20 530. 04 273. 39 350. 82 336. 09 14. 92 19. 25 18. 10 11. 21 23. 27 26. 14 38. 73 48. 75 48. 40 337. 27 450. 80 530. 73 18. 46 22. 58 27. 87 18. 99 23. 85 30. 19 33. 88 65. 10 98. 45 133. 21 4. 35 4. 54 4. 72 4. 79 4. 88 274. 15 14. 44 16. 96 36. 45 481. 31 42. 17 4. 97 Total 1893. 16 98. 41 124. 84 249. 50 2788. 82 181. 10 28. 26
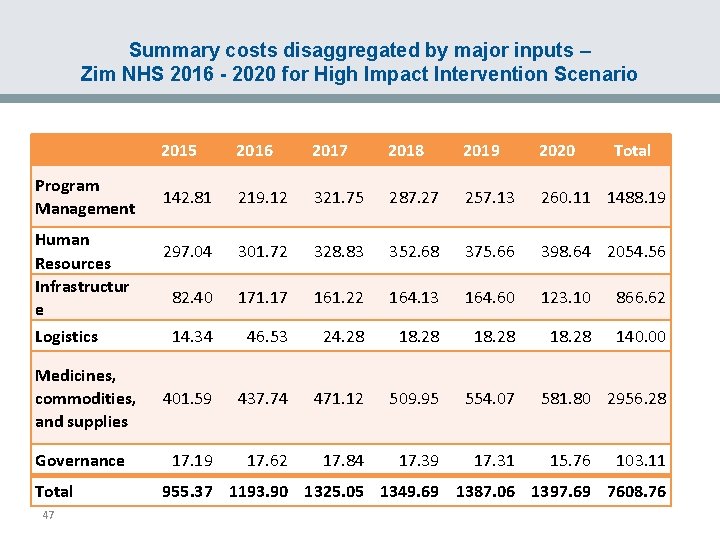
Summary costs disaggregated by major inputs – Zim NHS 2016 - 2020 for High Impact Intervention Scenario 2015 2016 2017 2018 2019 2020 Program Management 142. 81 219. 12 321. 75 287. 27 257. 13 260. 11 1488. 19 297. 04 301. 72 328. 83 352. 68 375. 66 398. 64 2054. 56 82. 40 171. 17 161. 22 164. 13 164. 60 123. 10 866. 62 14. 34 46. 53 24. 28 18. 28 140. 00 401. 59 437. 74 471. 12 509. 95 554. 07 17. 19 17. 62 17. 84 17. 39 17. 31 Human Resources Infrastructur e Logistics Medicines, commodities, and supplies Governance Total 47 Total 581. 80 2956. 28 15. 76 103. 11 955. 37 1193. 90 1325. 05 1349. 69 1387. 06 1397. 69 7608. 76

Summary of findings on costing of the Zimbabwe National Health Strategy 2016 -2020 • The preferred scenario (Scenario 2), with an estimated mean cost-per capita of $89 over the entire period is also expected to have the following impact in 2020: • Decline in infant mortality from 45 per live births 1000 (2015) to 31 per 1000 live births in 2020 • Decline in child mortality from 70 per 1000 (2015) to 55 per 1000 in 2020 • Decline in maternal mortality ratio from 514 per 100, 000 live births (2015) to 327 per 100, 000 live births in 2020 • 101, 645 life years gained by ART and PMTCT interventions by 2020 48
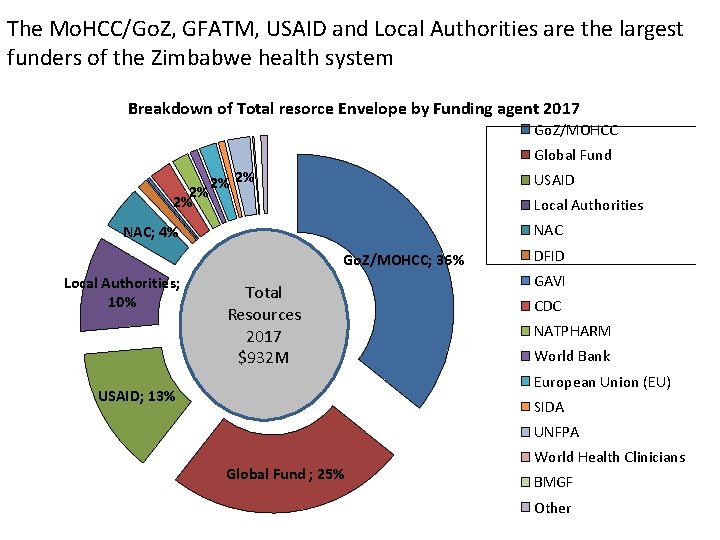
The Mo. HCC/Go. Z, GFATM, USAID and Local Authorities are the largest funders of the Zimbabwe health system Breakdown of Total resorce Envelope by Funding agent 2017 Go. Z/MOHCC Global Fund NA USAID Local Authorities NAC; 4% , TF , 2% GAVI 2% C, CD 4% 2% 2% Local Authorities; 10% Go. Z/MOHCC; 36% Total Resources $932 M 2017 $932 M DFID GAVI CDC NATPHARM World Bank European Union (EU) USAID; 13% SIDA UNFPA Global Fund ; 25% World Health Clinicians BMGF Other
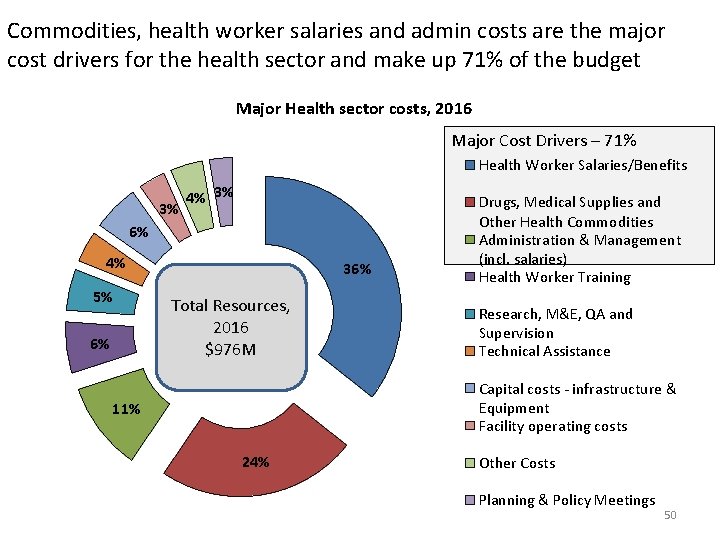
Commodities, health worker salaries and admin costs are the major cost drivers for the health sector and make up 71% of the budget Major Health sector costs, 2016 Major Cost Drivers – 71% Health Worker Salaries/Benefits 3% 4% 3% 6% 4% 5% 6% 36% Total Resources, 2016 $976 M Drugs, Medical Supplies and Other Health Commodities Administration & Management (incl. salaries) Health Worker Training Research, M&E, QA and Supervision Technical Assistance Capital costs - infrastructure & Equipment Facility operating costs 11% 24% Other Costs Planning & Policy Meetings 50
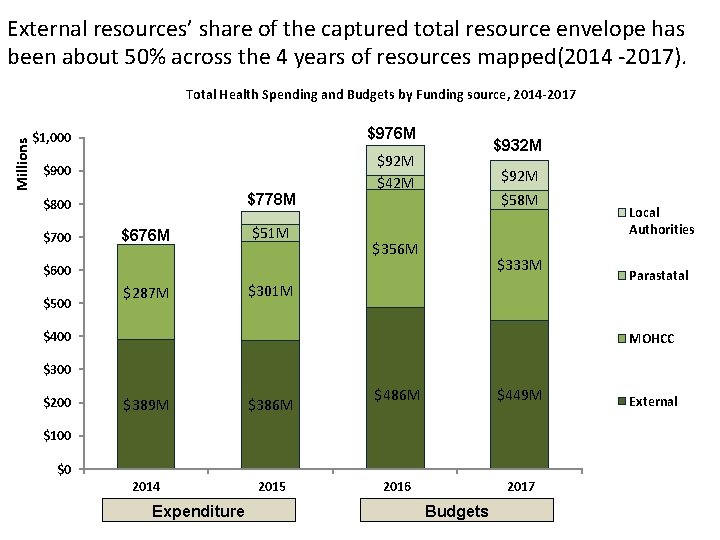
External resources’ share of the captured total resource envelope has been about 50% across the 4 years of resources mapped(2014 -2017). Millions Total Health Spending and Budgets by Funding source, 2014 -2017 $1, 000 $976 M $900 $92 M $42 M $778 M $800 $700 $676 M $51 M $932 M $92 M $58 M $356 M $333 M $600 $500 $287 M $301 M $400 Local Authorities Parastatal MOHCC $300 $200 $389 M $386 M 2014 2015 $486 M $449 M 2016 2017 $100 $0 Expenditure Budgets External
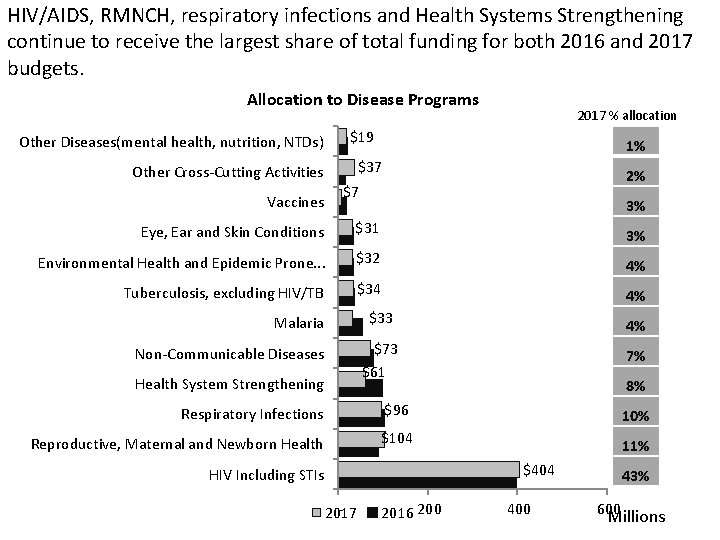
HIV/AIDS, RMNCH, respiratory infections and Health Systems Strengthening continue to receive the largest share of total funding for both 2016 and 2017 budgets. Allocation to Disease Programs 2017 % allocation $19 Other Diseases(mental health, nutrition, NTDs) 1% $37 Other Cross-Cutting Activities 2% $7 Vaccines 3% Eye, Ear and Skin Conditions $31 Environmental Health and Epidemic Prone. . . $32 4% Tuberculosis, excluding HIV/TB $34 4% 3% $33 Malaria 4% $73 $61 Non-Communicable Diseases Health System Strengthening Respiratory Infections $96 Reproductive, Maternal and Newborn Health $104 7% 8% 10% 11% $404 HIV Including STIs 2017 2016 200 400 43% 600 Millions
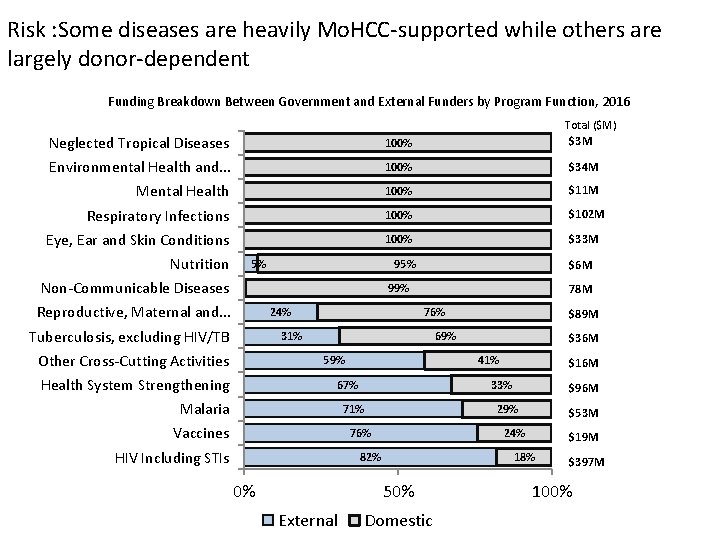
Risk : Some diseases are heavily Mo. HCC-supported while others are largely donor-dependent Funding Breakdown Between Government and External Funders by Program Function, 2016 Total ($M) $3 M Neglected Tropical Diseases 100% Environmental Health and. . . 100% $34 M Mental Health 100% $11 M Respiratory Infections 100% $102 M Eye, Ear and Skin Conditions 100% $33 M Nutrition 5% 95% Non-Communicable Diseases $6 M 99% Reproductive, Maternal and. . . 24% Tuberculosis, excluding HIV/TB 78 M 76% 31% Other Cross-Cutting Activities 69% 59% Health System Strengthening $89 M 41% 67% Malaria $19 M 18% 50% External $53 M 24% 82% 0% $96 M 29% 76% HIV Including STIs $16 M 33% 71% Vaccines $36 M Domestic $397 M 100%

HFP • National Health Financing Policy/Strategy • Innovative financing • Health in All Policies

Thank you
- Slides: 55