An Introduction to Myofascial Pain Syndrome Content Definition

















- Slides: 75

An Introduction to Myofascial Pain Syndrome 神經內科 洪國華

Content • • Definition and examples Clinical characteristics Pathophysiology Clinical importance Diagnosis Treatment Perpetuating Factors

Myofascial Pain syndrome • General definition: A regional pain syndrome of any soft tissue origin • Specific definition: The sensory, motor and autonomic symptoms caused by myofascial trigger points

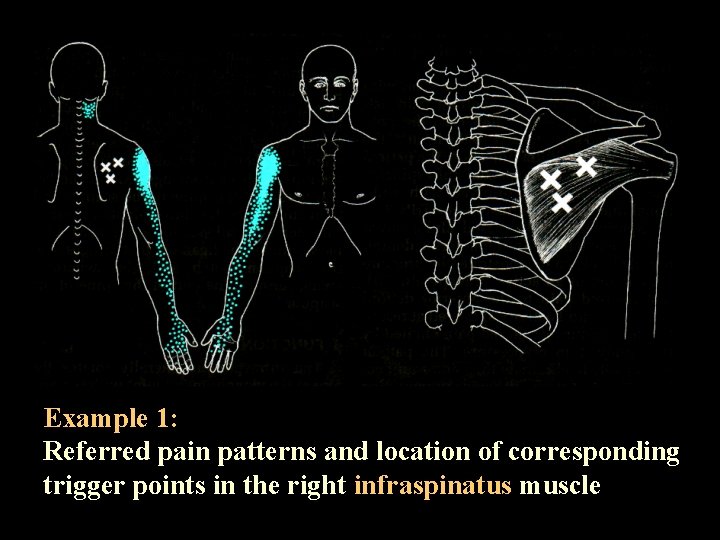
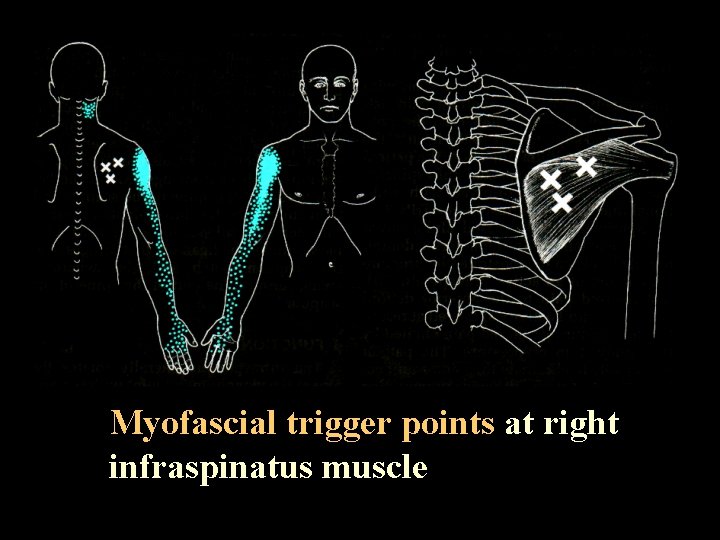
Example 1: Referred pain patterns and location of corresponding trigger points in the right infraspinatus muscle


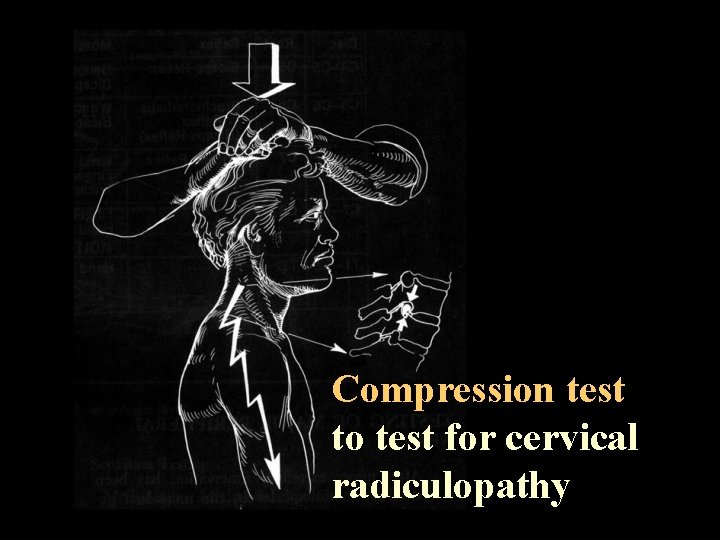
Compression test to test for cervical radiculopathy

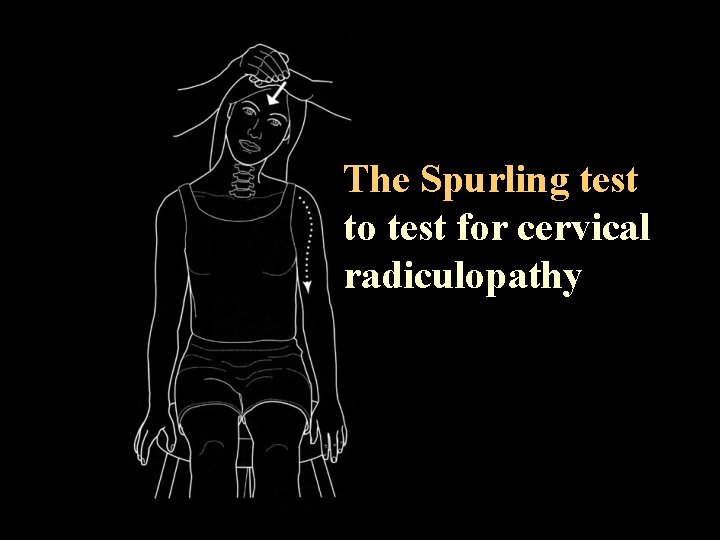
The Spurling test to test for cervical radiculopathy

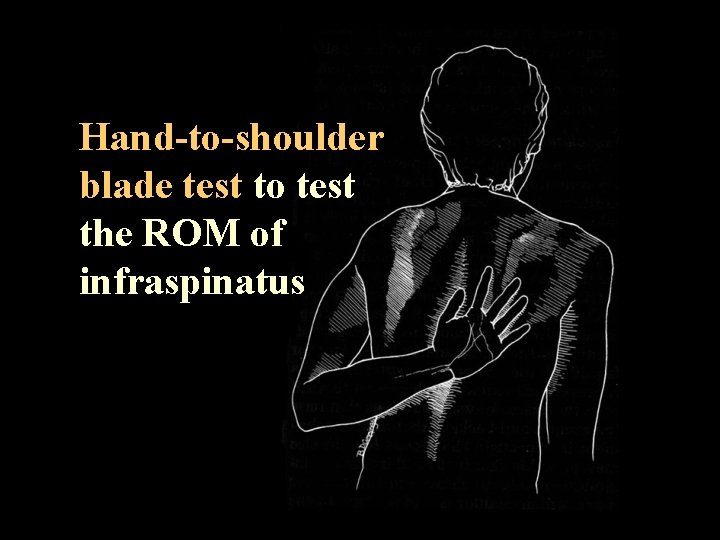
Hand-to-shoulder blade test to test the ROM of infraspinatus

Myofascial trigger points at right infraspinatus muscle

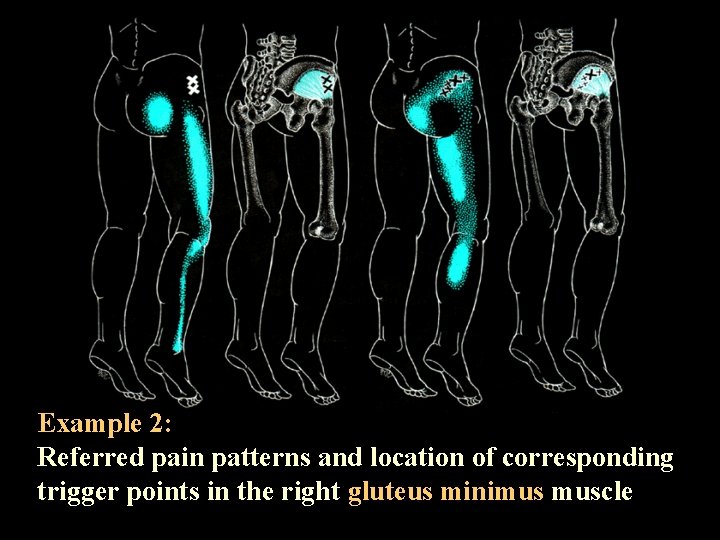
Example 2: Referred pain patterns and location of corresponding trigger points in the right gluteus minimus muscle


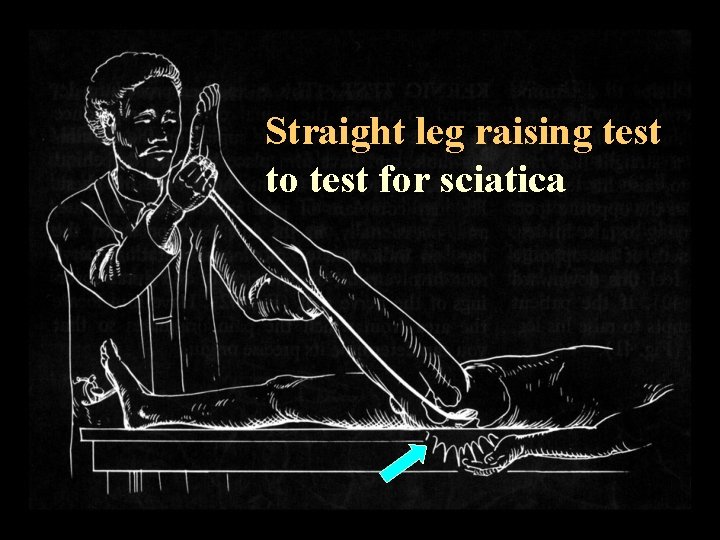
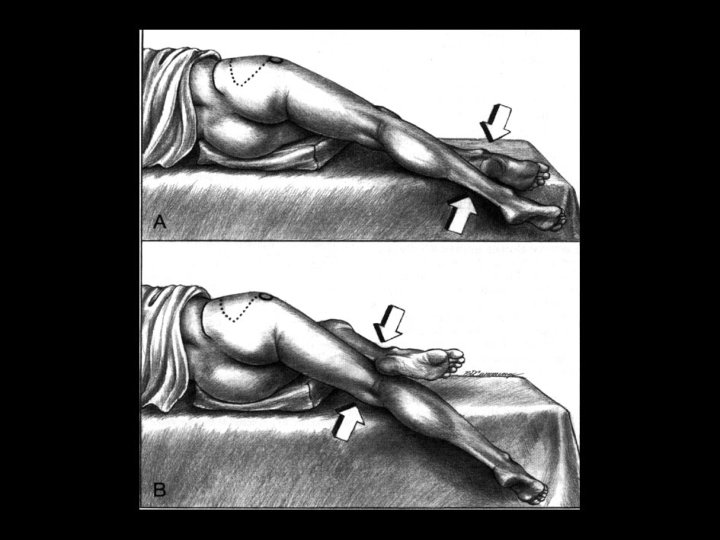
Straight leg raising test to test for sciatica


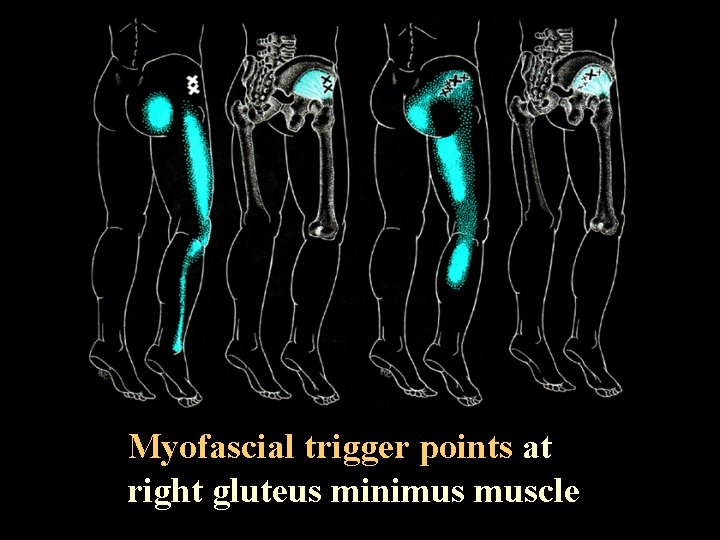
Myofascial trigger points at right gluteus minimus muscle

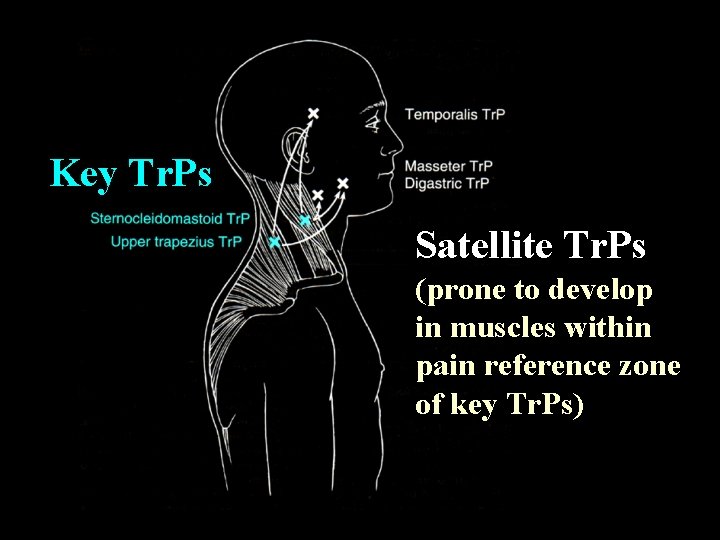
Categories of Trigger Points • Active Tr. Ps produce a familiar symptom when the Tr. P is digitally compressed • Latent Tr. Ps produce characteristics of a Tr. P but no spontaneous pain • An active key Tr. P in one muscle can induce an active satellite Tr. P in another muscle

Key Tr. Ps Satellite Tr. Ps (prone to develop in muscles within pain reference zone of key Tr. Ps)

Pain Complaint • Poorly localized, regional, aching pain in subcutaneous tissues, including muscles and joints • More likely to develop in sedentary workers who are prone to intermittent orgies of vigorous physical activity

Neurologic dysfunction • Sensory: Numbness or paresthesia • Proprioception: Imbalance, dizziness • Autonomic: Abnormal sweating, pilomotor activities • Motor: Spasm, weakness, loss of coordination and decreased work tolerance • Sleep disturbance

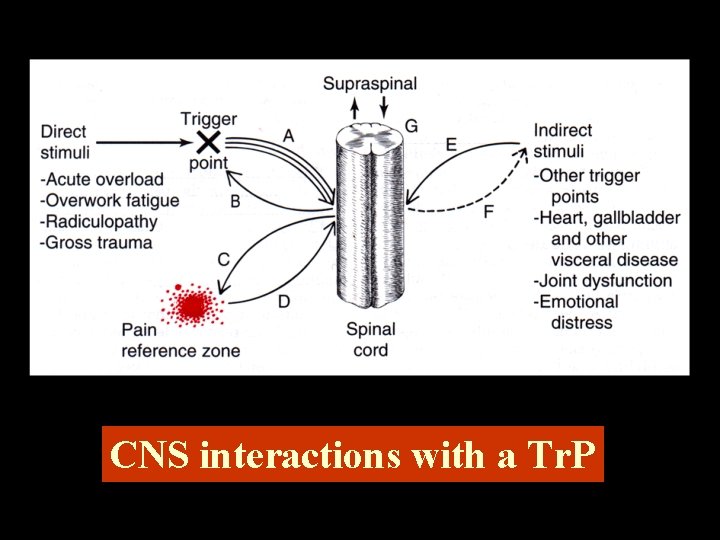
CNS interactions with a Tr. P

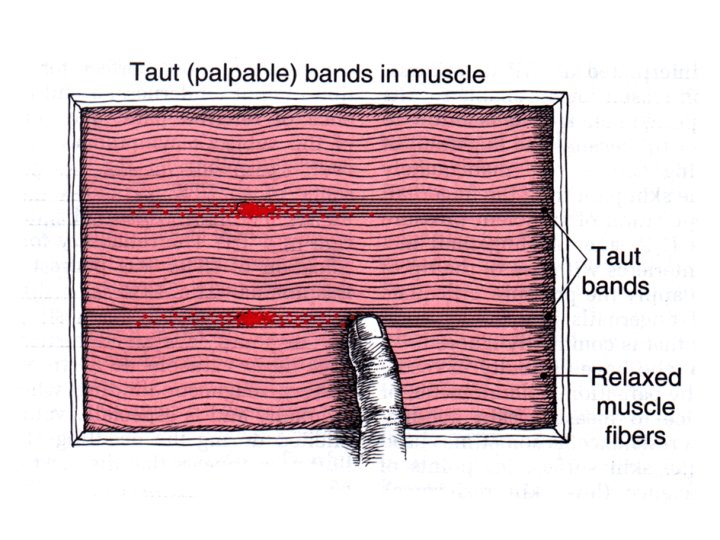
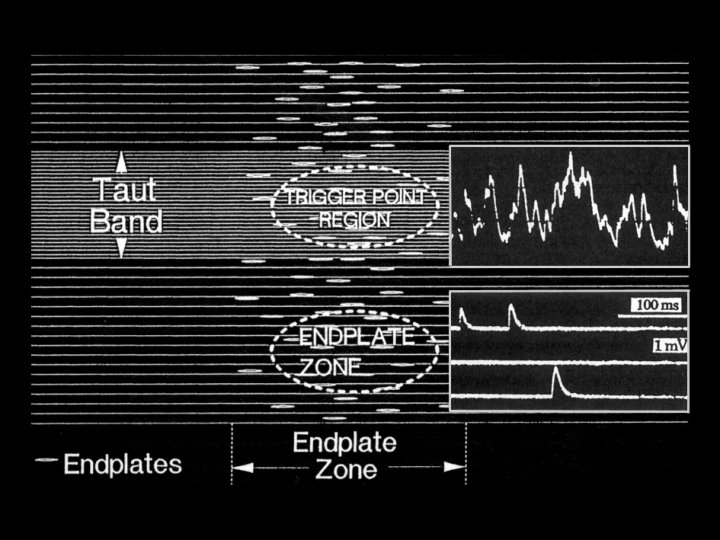
Physical Findings • • • Taut band tender nodule Recognition of familiar symptoms Referred sensory symptoms Local twitch response Limited range of movement





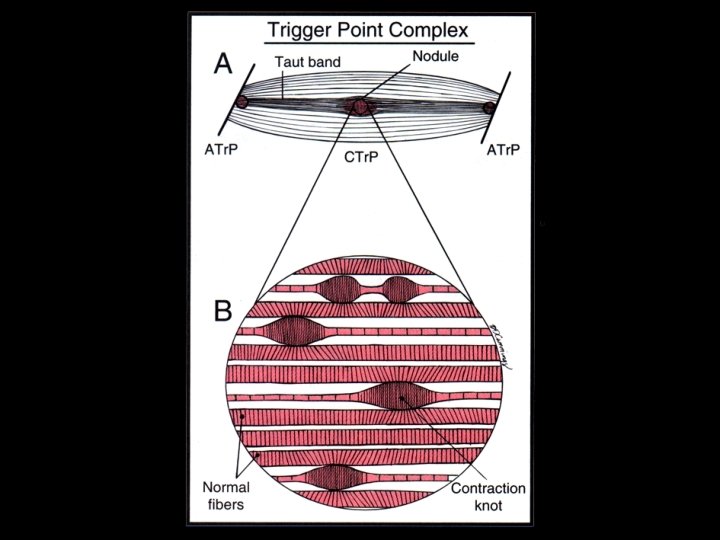
Central Vs Attachment Tr. Ps




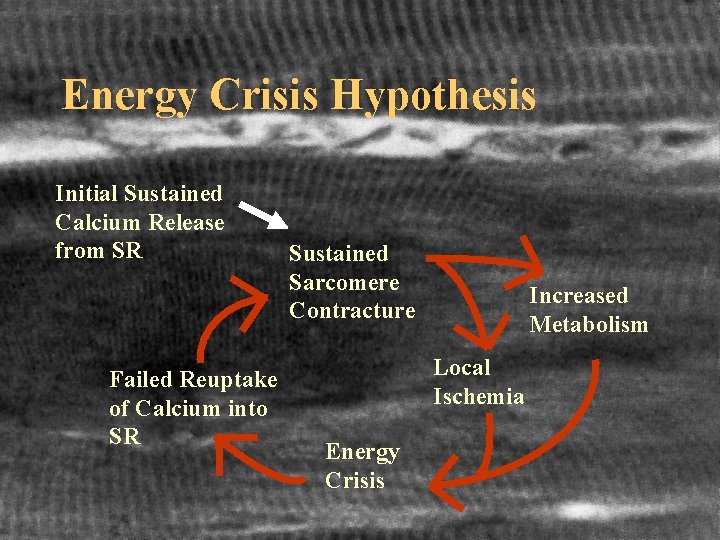
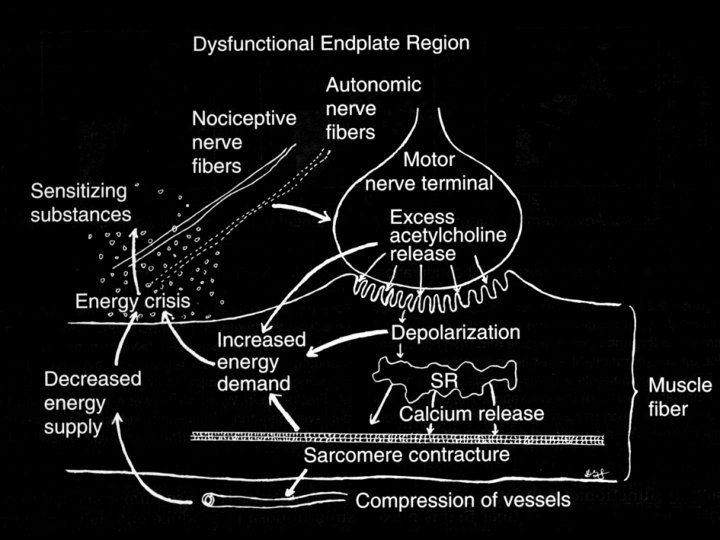
Energy Crisis Hypothesis Initial Sustained Calcium Release from SR Failed Reuptake of Calcium into SR Sustained Sarcomere Contracture Increased Metabolism Local Ischemia Energy Crisis


Prevalence of Trigger Point Pain

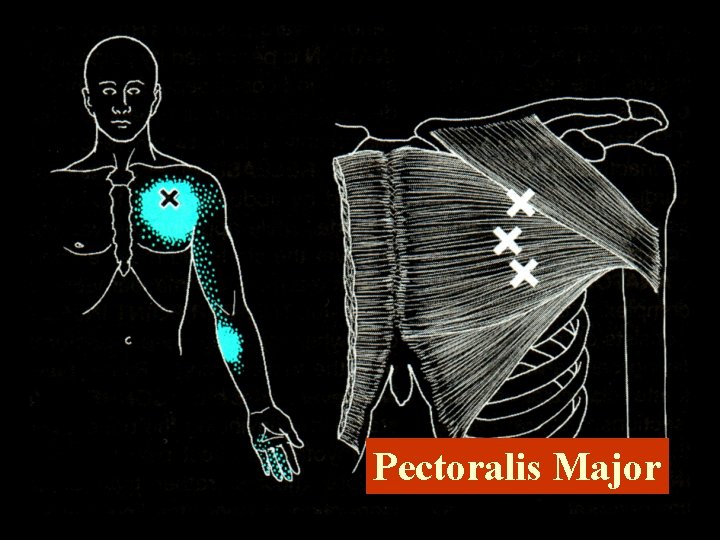
Pectoralis Major

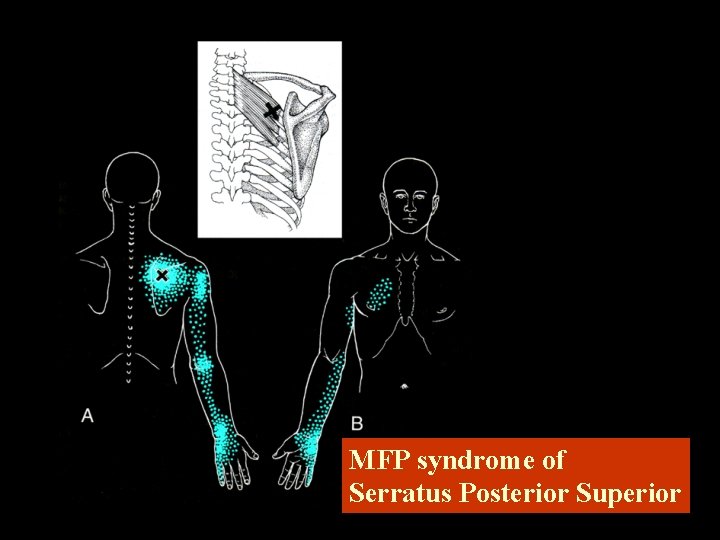
MFP syndrome of Serratus Posterior Superior

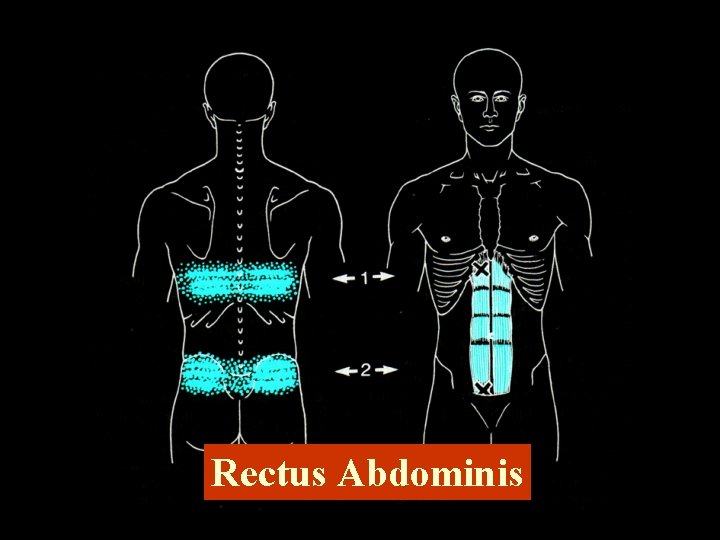
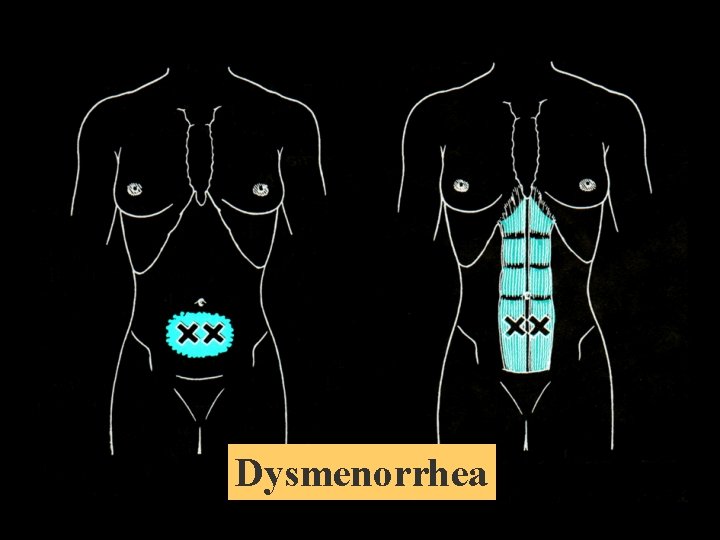
Rectus Abdominis

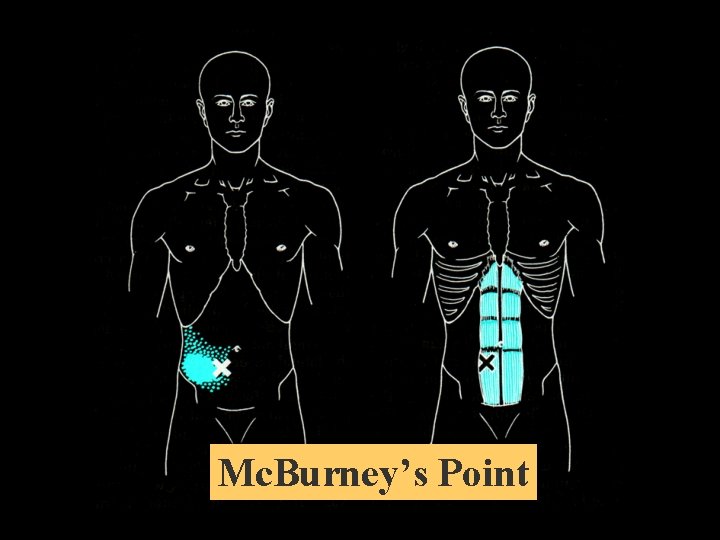
Mc. Burney’s Point

Dysmenorrhea

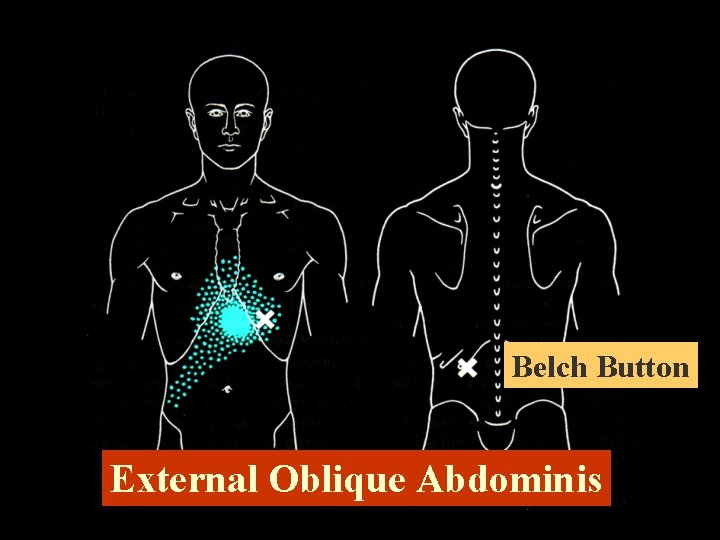
Belch Button External Oblique Abdominis

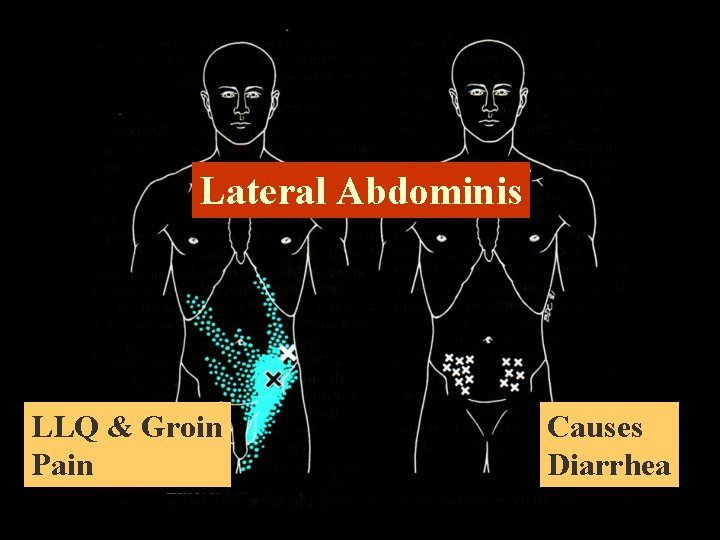
Lateral Abdominis LLQ & Groin Pain Causes Diarrhea

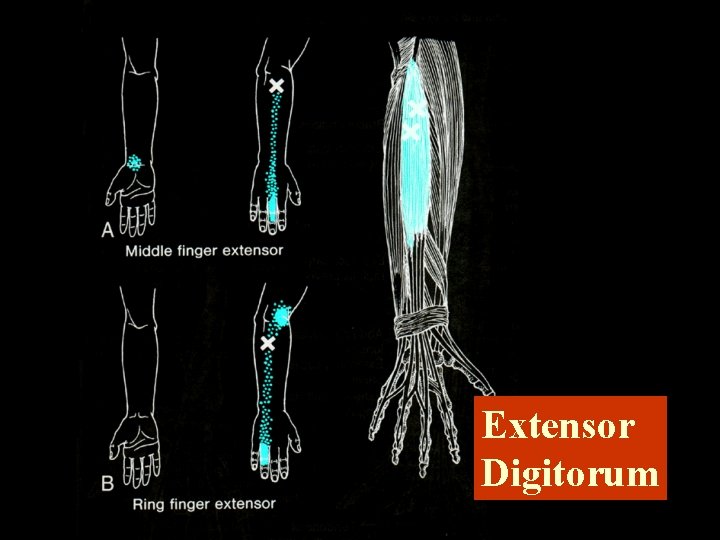
Extensor Digitorum

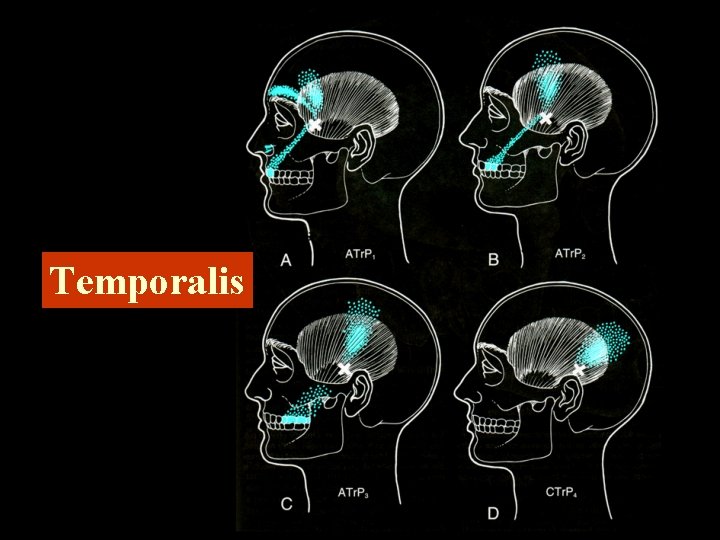
Temporalis

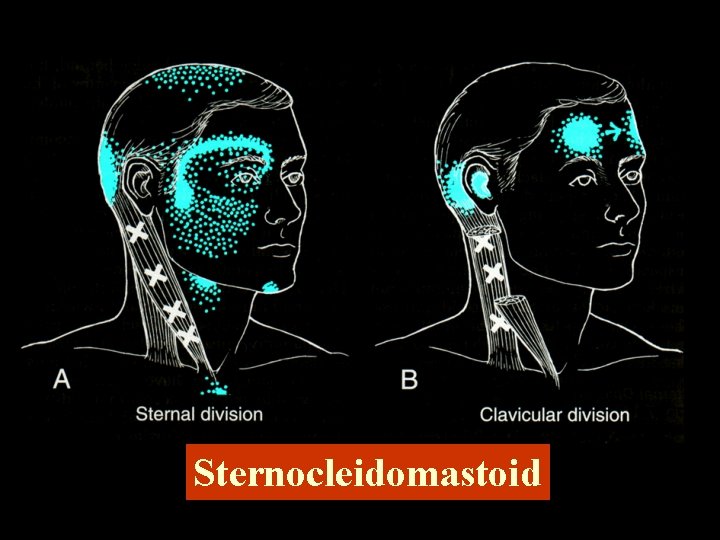
Sternocleidomastoid

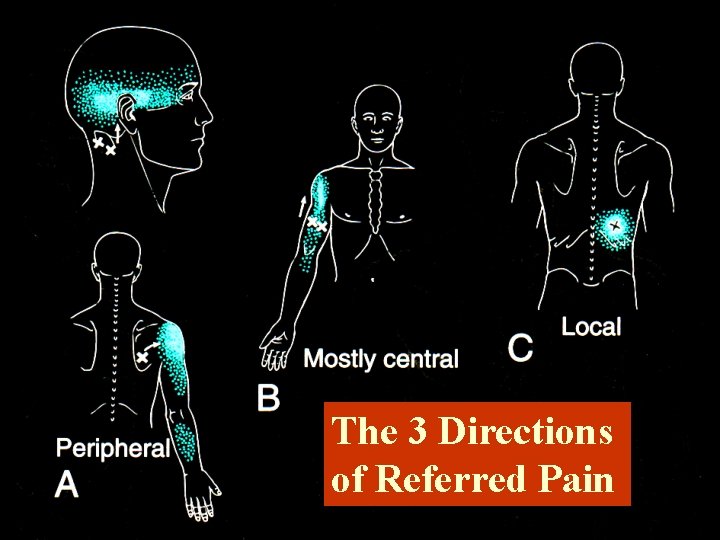
The 3 Directions of Referred Pain

Referred Pain • Referred at least partly in peripheral direction is most common (85% of patterns) • 48% referred only in direction of periphery • 20% both central & peripheral referral • 17% both local & peripheral referral • 10% only a local pattern • 5% refer only in a central direction

Criteria for Identifying a Tr. P Essential Criteria • Taut band palpable • Exquisite spot tenderness of a nodule in a taut band • Patient’s recognition of current pain by pressure on the trigger point • Painful limit to full stretch range of motion

Criteria for Identifying a Tr. P Confirmatory Observations • Visual or tactile identification of local twitch response (LTR) • Imaging of a local twitch response induced by needle penetration of tender nodule • Pain or altered sensation (in the distribution expected) on compression of tender nodule • EMG demonstration of spontaneous electrical activity

Trigger Point Release • Spray and Stretch • Voluntary Contraction and Released Methods • Trigger Point Pressure Release • Deep Stroking Massage

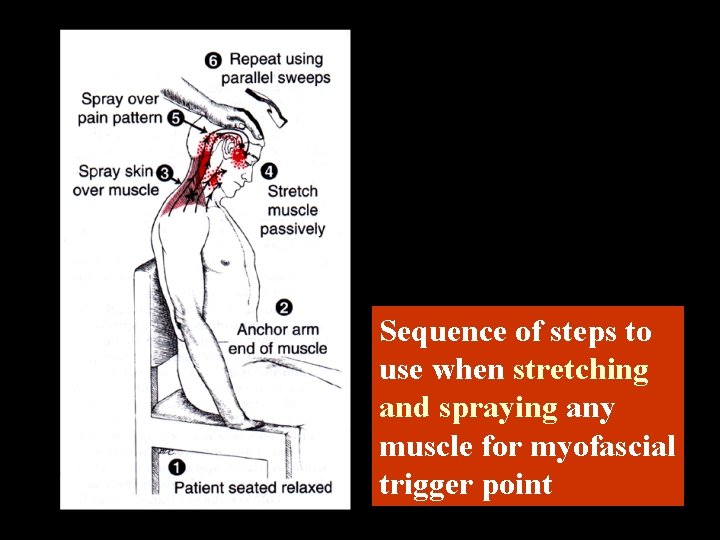
Sequence of steps to use when stretching and spraying any muscle for myofascial trigger point

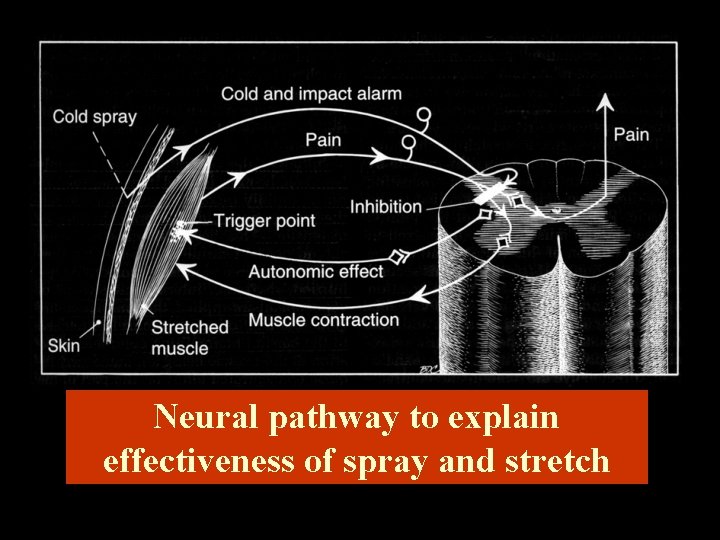
Neural pathway to explain effectiveness of spray and stretch

Trigger Point Release • Spray and Stretch • Voluntary Contraction and Released Methods • Trigger Point Pressure Release • Deep Stroking Massage

Accessory Techniques • • • Phased Respiration Directed Eye Movement Biofeedback Heat and Cold Iontophoresis and Phonophoresis

Modalities • Therapeutic Ultrasound • High Voltage (and High Frequency) Galvanic Stimulation

Pain Relief • Transcutaneous Electric Nerve Stimulation • Drug Therapy – Pain Killer – Muscle Relaxants – Sleep

Trouble-making Drugs • Caffeine – Small to moderate amounts of caffeine may help to minimize Tr. Ps – Excessive intake of caffeine ( > 2 or 3 cups/bottles/cans of coffee and/or cola) is likely to aggravate Tr. P activity • Alcohol reduces absorption of folic acid • Tobacco increases the need for vitamin C

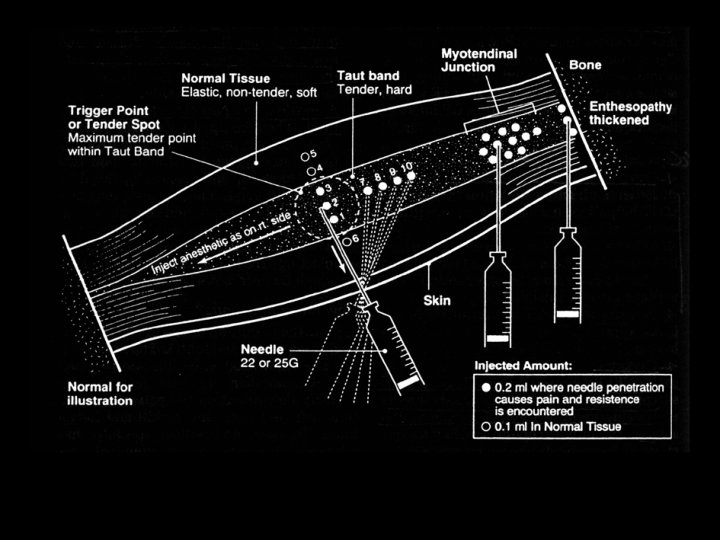
Trigger Point Injection • Local anesthetic with or WITHOUT corticosteroid • Dry needling – Within 2 - 8 hours, 42% of lidocaine-injected patients and 100% of dry-needled patients developed local soreness • Botulinum toxin A

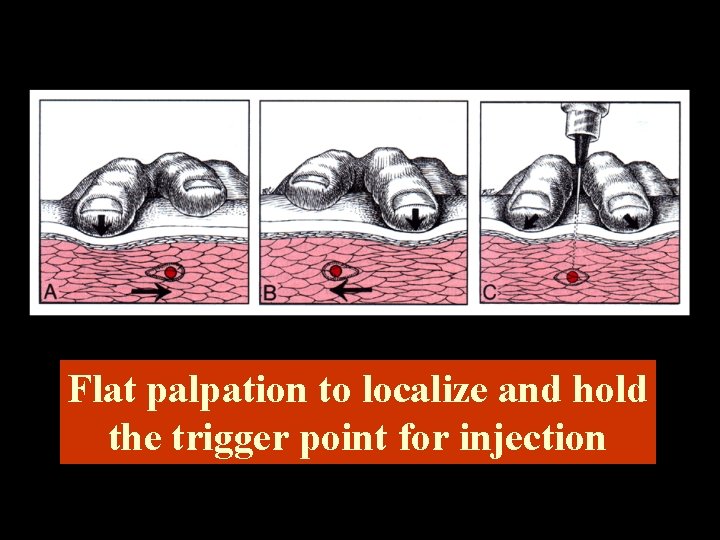
Flat palpation to localize and hold the trigger point for injection

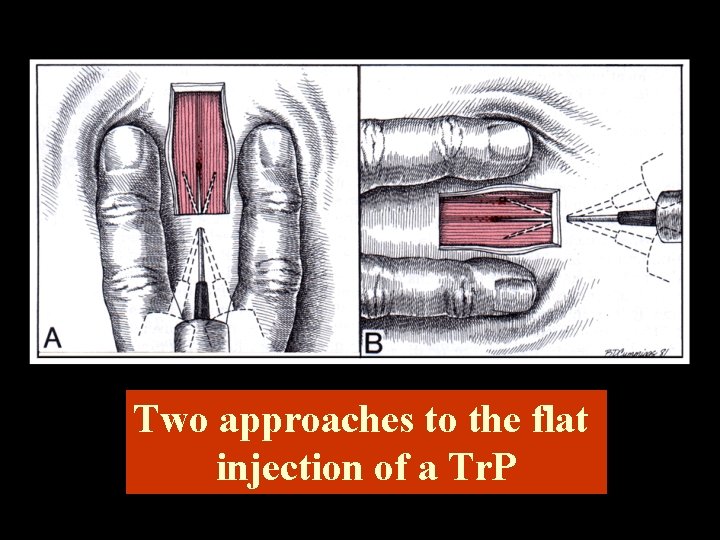
Two approaches to the flat injection of a Tr. P

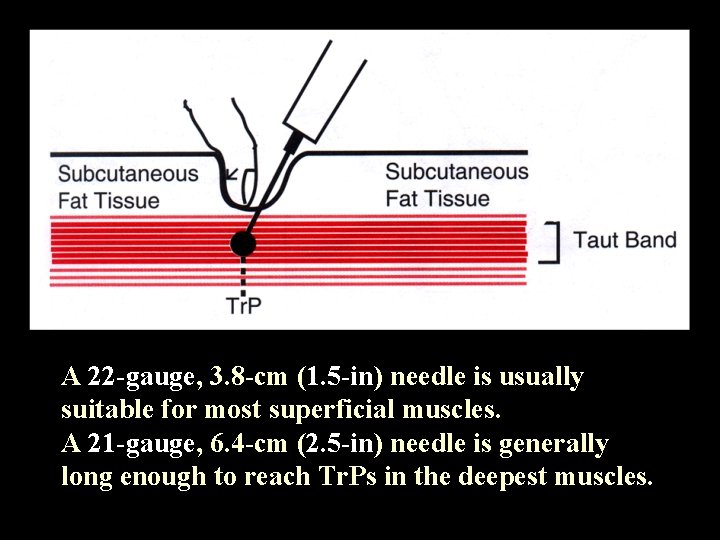
A 22 -gauge, 3. 8 -cm (1. 5 -in) needle is usually suitable for most superficial muscles. A 21 -gauge, 6. 4 -cm (2. 5 -in) needle is generally long enough to reach Tr. Ps in the deepest muscles.


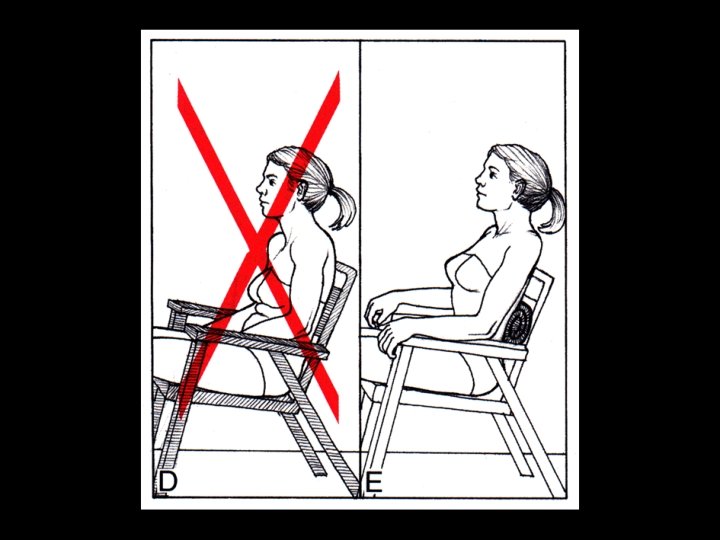
Appropriate Activities • Strenuous activities should be avoided for at least 2 or 3 days if soreness develops • Use muscles in gentle, normal way through their full range of motion • Avoid placing muscles in fixed, shortened position for long time • Any activity that produces pain for more than a few seconds should be avoided

Perpetuating Factors • • • Mechanical stress Nutritional Inadequacies Metabolic Factors Psychological Factors Chronic infection Other factors (e. g. Allergic Rhinitis, Dysomnia, Nerve impingement)






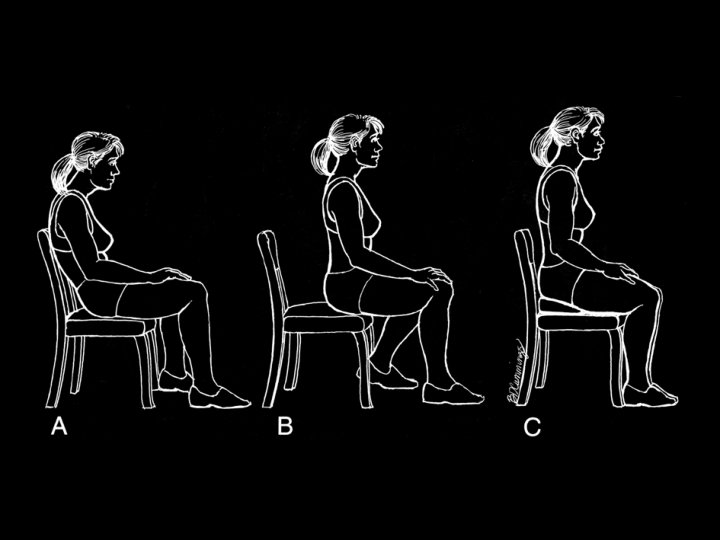
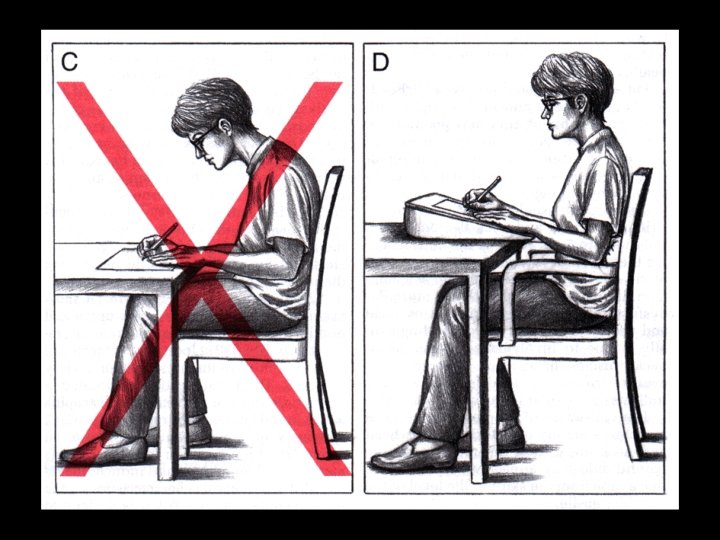
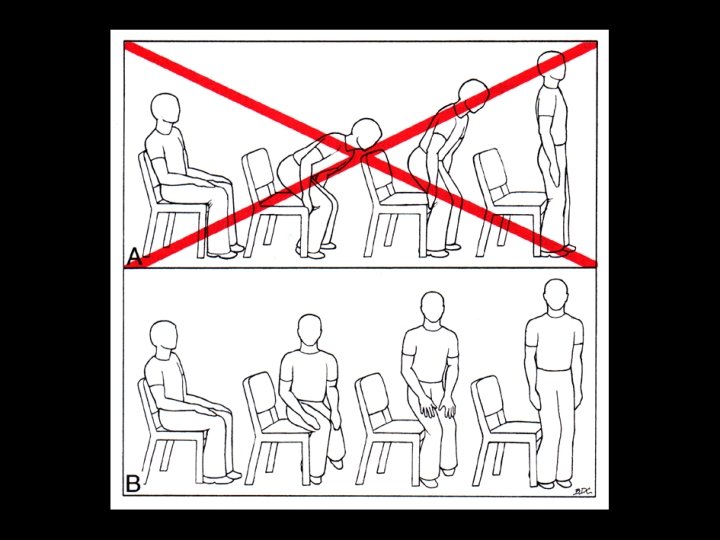
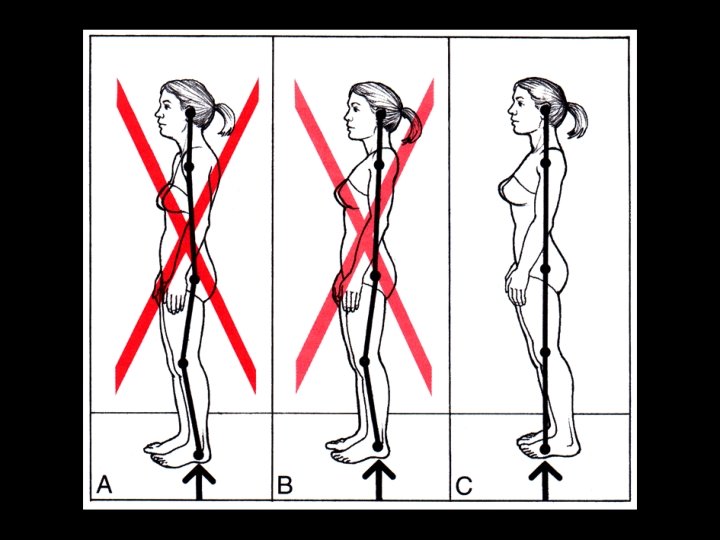
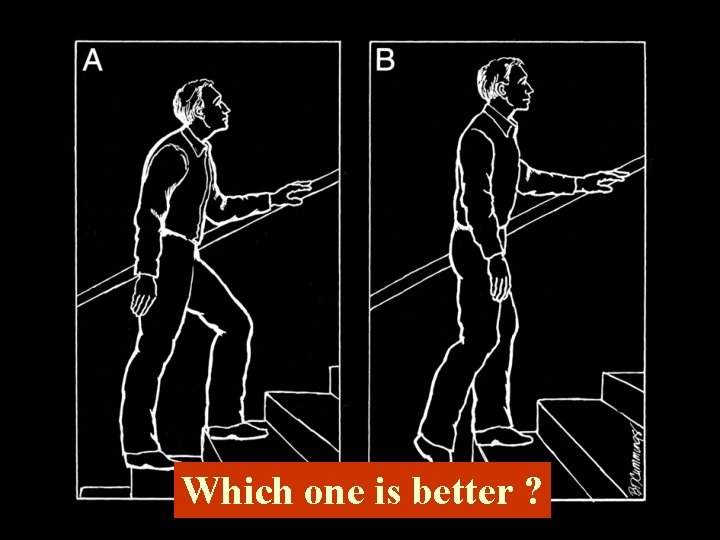
Which one is better ?

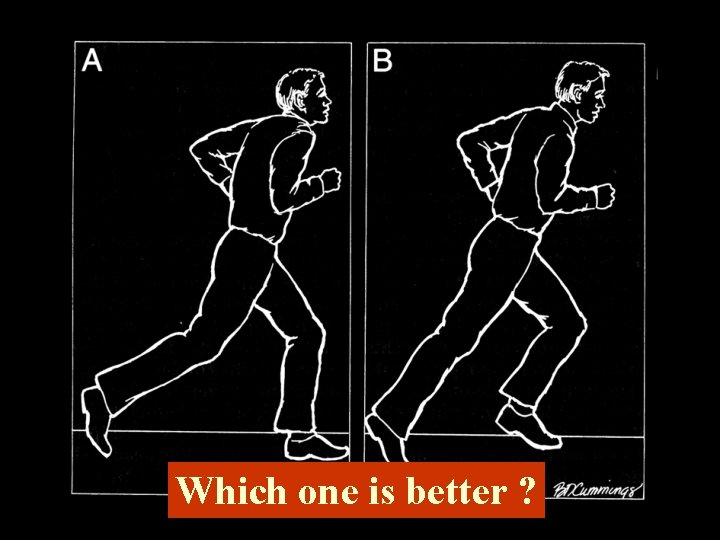
Which one is better ?

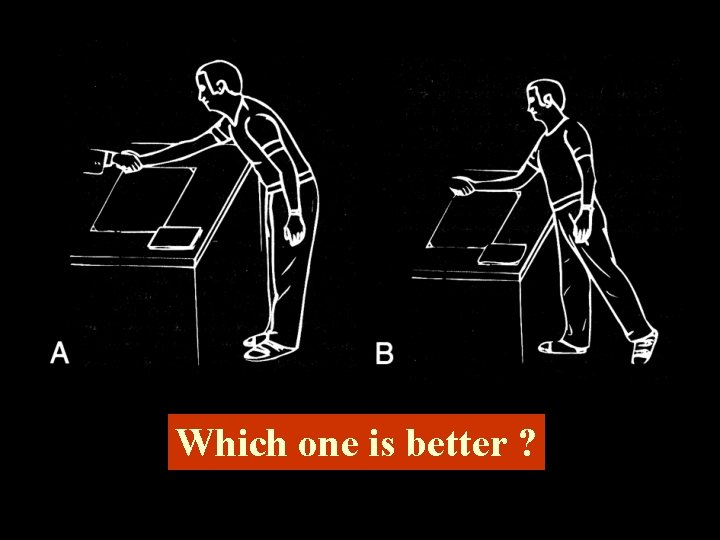
Which one is better ?

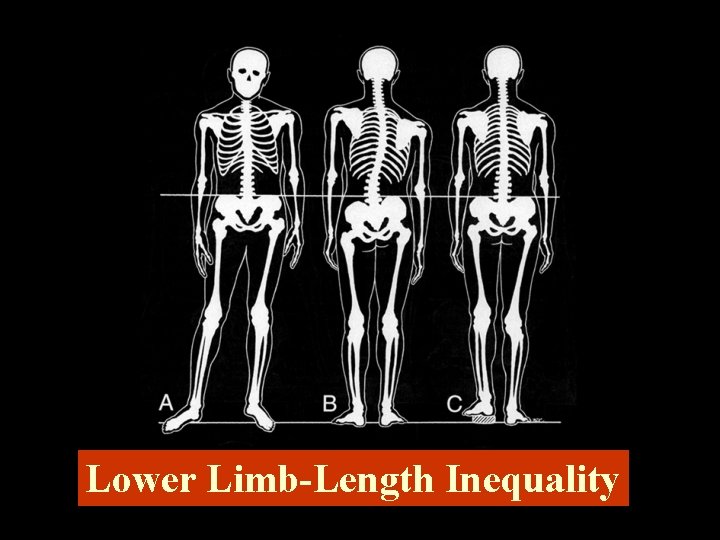
Structural Inadequacies • Lower Limb-length Inequality • Small Hemipelvis • Short Upper Arms

Lower Limb-Length Inequality

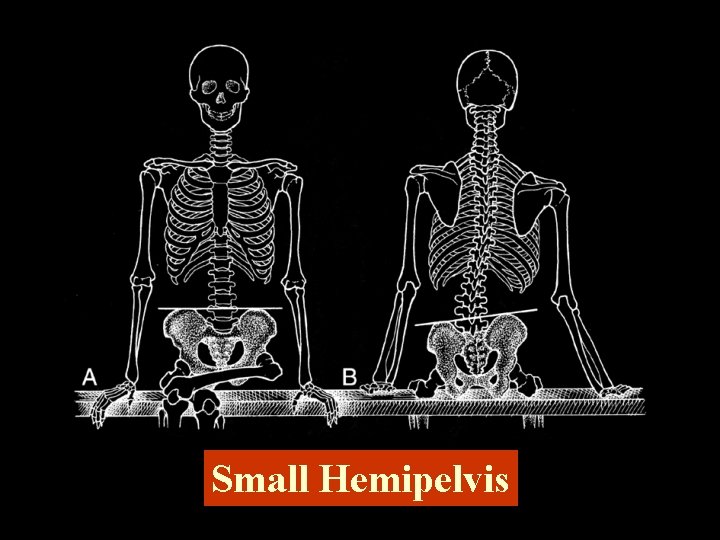
Small Hemipelvis

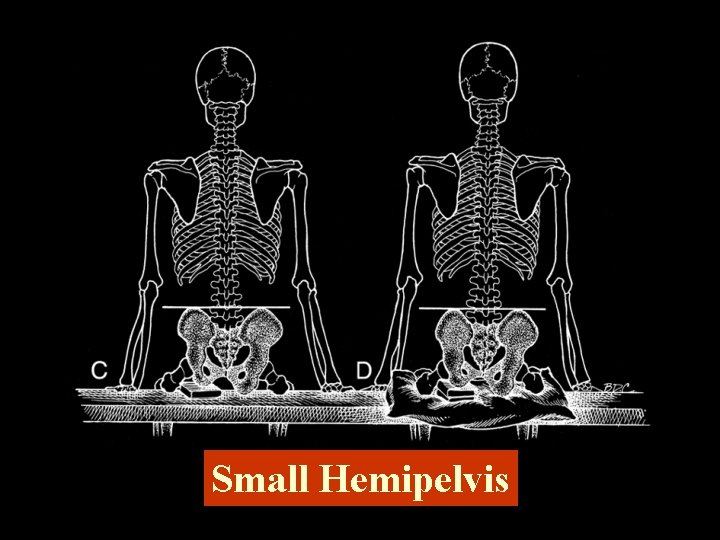
Small Hemipelvis

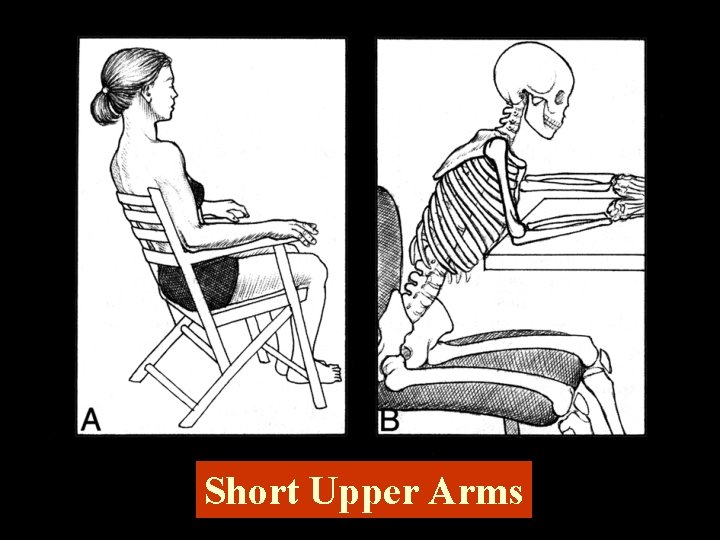
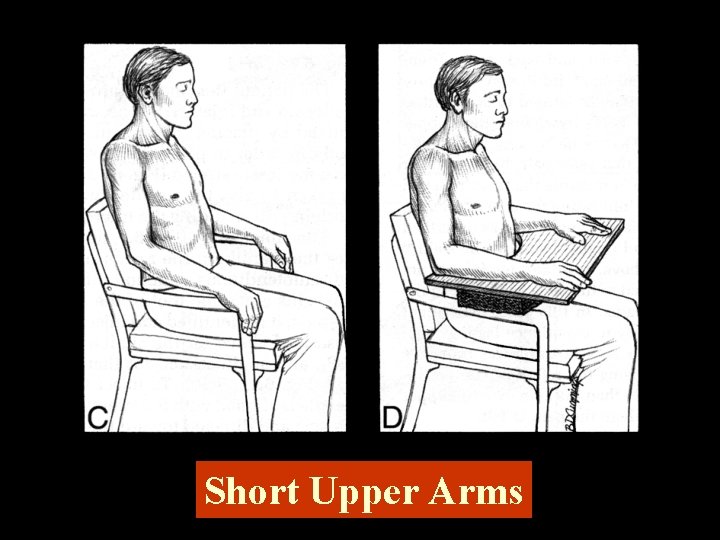
Short Upper Arms

Short Upper Arms

Conclusion • Myofascial trigger points (Tr. Ps) are extremely common and become a painful part of nearly everyone’s life at one time or another • Try to seek for Tr. P in any cases of pain and dysfunction