AN AMERICAN APPROACH VISION REHABILITATION FOLLOWING ACQUIRED BRAIN

AN AMERICAN APPROACH: VISION REHABILITATION FOLLOWING ACQUIRED BRAIN INJURY AND STROKE – LESSONS FROM US VETERANS AND TROOPS Gregory L. Goodrich, Ph. D. Western Blind Rehabilitation Center & Psychology Service Supervisory Research Psychologist VA Palo Alto Health Care System

GOD MORGEN It’s a pleasure to be here! The top ten best places to be born in 2013: 1. Switzerland 2. Australia 3. Norway 4. Sweden 5. Denmark 6. Singapore 7. New Zealand 8. Netherlands 9. Canada 10. Hong Kong

DISCLAIMERS & ACKNOWLEDGMENTS I have no financial interest in any product discussed The views expressed are my own and do not necessarily reflect those of the Department of Veterans Affairs or the Palo Alto Health Care System My research colleagues Jennine Kirby, O. D. Heidi Flyg, O. D. Karen Brahm, O. D. Gary Martinsen, O. D. Glenn Cockerham, O. D.

BACKGROUND The Department of Veterans Affairs (VA) is a federal program serving veterans 22. 2 million veterans (Denmark ~5. 5 million) Serves 36% of all veterans 55% of 1. 5 million Iraq and Afghanistan veterans receive VA services; 94% outpatient & 6% hospitalized) Total 152 US population ~ 313 million (EU ~ 503, 679, 730) medical centers, over 1100 clinics 13 Blind Rehabilitation Centers, 54 Low Vision Clinics Currently serve veterans from WWII, Korea, Vietnam, Gulf War, and wars in Afghanistan and Iraq as well as peacetime intervals

OUTLINE Brief history of how I got here What do traumatic brain injury and stroke have in common (and differences)? Review of our research on TBI and vision loss Studies of vision loss/dysfunction Inpatient Outpatient Mechanism of injury Rehabilitation What we know and don’t know Summary

HOW I GOT HERE Most of my career in low vision research (reading, mobility, technology, etc. ) 2003 WBRC admitted first military patient with TBI-related vision loss Not a happy story We learned that individuals with TBI-related vision loss didn’t fit well into “traditional” low vision rehabilitation This led to research to characterize the vision injury and co-existing conditions Which, in turn, led to clinical rehabilitation programs
VISION LOSS – STROKE & TRAUMA Stroke Binocular/oculomotor problems Visual field loss Visual acuity loss (rare) Visual processing Light sensitivity Co-morbid loss (paresis, paralysis, cognitive, emotional, etc. ) Trauma Binocular/oculomotor problems Visual field loss Visual acuity loss (rare) Visual processing Light sensitivity Co-morbid loss (paresis, paralysis, cognitive, emotional, etc. )

Danish OTHER COMMONALITIES English In brain injury from both stroke and trauma vision loss/dysfunction are frequently undiagnosed Vision rehabilitation is usually one of numerous types of rehabilitation needed by the patient Vision loss/dysfunction degrades education, vocation and quality of life Caregivers play an important role in recovery We know much less than we would like! Similarities aside “the devil may be in the details”

SOME DIFFERENCES Stroke often occurs to specific brain areas Traumatic brain injury may lack this specificity Some differences in co-morbidities Post traumatic stress disorder (PTSD) May reflect that PTSD is not assessed in civilian settings Dual sensory impairment (DSI): hearing & vision (blast) Severity may be assessed on different scales Glasgow Coma Scale vs NIH Stroke Severity Commonalities and differences in visual loss/dysfunction between stroke- and traumarelated injury have not been well studied

SEVERITY OF BRAIN INJURY ~85% of TBIs are mild ~15% of TBIs are moderate/severe/penetrating In our studies severity of TBI does not correlate with severity of vision loss/dysfunction, but m. TBI generally associated with binocular/occulomotor dysfunction in outpatients Inpatients exhibit vision loss and binocular/ occulomotor dysfunction

EPIDEMIOLOGY: UNITED STATES Traumatic Brain Injury http: //www. cdc. gov/traumaticbraininjury/statistics. html Incidence = 1. 7 million/yr. (not treated hence not reported = ? ? ? ) 1. 365 million treated; 275, 000 hospitalized Cost = $76. 5 billion/yr. Causes Falls ~ 523, 000 Stuck by/against (sports, accidents, etc. ) ~ 271, 000 Motor Vehicle Accident ~ 218, 000 Assault ~ 148, 000 Other/Unknown ~202, 000 Aquired brain injury: stroke/anoxia/tumor/etc. http: //www. cdc. gov/mmwr/preview/mmwrhtml/mm 5619 a 2. htm Stroke ~ 795, 000/yr. Cost ~ $62. 7 Billion/yr.

EPIDEMIOLOGY: EUROPE Traumatic Incidence Brain Injury = 1. 6 million/yr. Ribbers, G. M. Int Encyl Rehab (http: //cirrie. buffalo. edu/encyclopedia/en/) 18% of US incidence (reporting or just less accident prone? ) Cost = € 2. 9 billion/yr. Causes similar to US data Aquired brain injury: stroke/anoxia/tumor/etc. (http: //www. escardio. org/communities/EHRA/publications/papers-interest/Documents/ehra-stroke-report-recommend-document. pdf) Stroke ~ 2 million/yr. Cost ~ € 38 Billion/yr.

VISUAL CHANGES FOLLOWING TBI Visual Acuity Interestingly, visual acuity is not often impacted (~3% - 14% in inpatients; ~1% – 2% in outpatients) may be most affected by non-blast injury or more severe level of injury Blast events result in enucleation (18%) or blindness (6%) in polytrauma patients Visual acuity often considered “gold standard” of visual function – “status”may hinder identification of patients with visual abnormalities

VISUAL CHANGES FOLLOWING TBI Visual Field 14% - 33% found in our studies of polytrauma patients Hemianopia most common field loss usually homonimous but may be bitemporal Monocular or binocular Quadrant loss or field constriction
VISUAL CHANGES FOLLOWING TBI Binocular/Oculomotor Accommodation Vergence Strabismus Pursuits Fixation Dysfunctions

BINOCULAR/OCULOMOTOR DYSFUNCTION Very good documentation that dysfunctions negatively affect quality of life, for example, Reading Mobility & Driving Mckenna, K. et al, 2005, Brain Inj Recovery and reintegration Babbage, D. , Neuropsych, 2009 Visual Processing Hatt, S. J Ophthal, 2007; Chen, S. Top Stroke Rehab, 2009; DVBIC, July 2, 2009 Communication and social interaction Schuett, S. Neuropsychologia, 2008 Saunders, et al, JRRD, 2012 Quality of life Cockerham, NEJM, 2009

VA/DOD TBI & VISION LITERATURE Goodrich, et al. JRRD, 2007 Lew, et al. JRRD, 2007 Stelmack, et al. Optom, 2009 Cockerham, et al. JRRD, 2010 Lew, et al. (DSI) Neuro. Rehab, 2010 Cockerham, et al. NEJM, 2011 (occult eye injury) Dougherty, et al. Brain Inj, 2011 Capo’-Aponte, et al. Mil Med, 2012 Goodrich, et al. Opt Vis Sci 2013, (in press) Goodrich, et al. JRRD, 2013 (in press)
OUTPATIENT STUDIES (BRAHM, ET AL. OVS 2009; GOODRICH, ET AL. OVS (IN PRESS)) The following slides summarize our studies on VA outpatients Majority diagnosed with m. TBI Majority male ~95% Mean age ~ 29 years Served in Afghanistan and/or Iraq The data presented will address mechanism of injury (blast vs other trauma such as motor vehicle accidents, falls, assault, etc. )

OUTPATIENT POPULATION Polytrauma Referred Networks Site (outpatient clinic) to clinic if answered yes to any one question 1. Have you ever been in a blast/explosion (or close proximity), vehicular crash, or fall? (79% blast, 21% other) 2. Have you ever been rendered unconscious? (50%) 3. Have you ever had head trauma (98%) Visual status pre-injury unknown
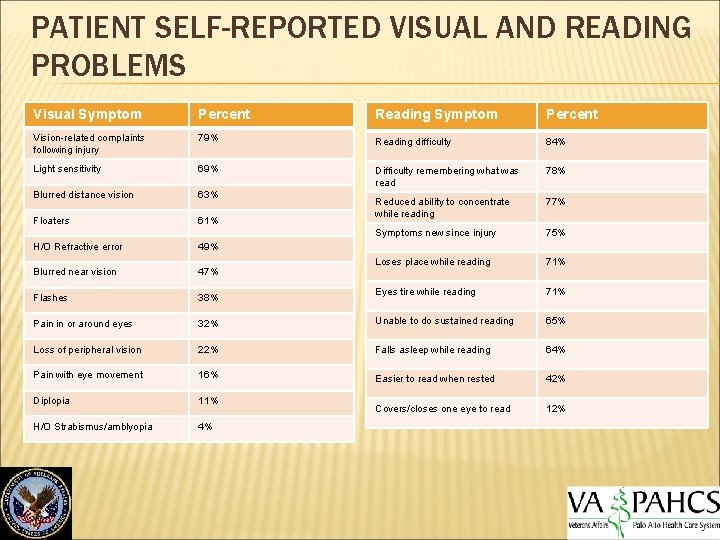
PATIENT SELF-REPORTED VISUAL AND READING PROBLEMS Visual Symptom Percent Reading Symptom Percent Vision-related complaints following injury 79% Reading difficulty 84% Light sensitivity 69% Difficulty remembering what was read 78% Blurred distance vision 63% 77% Floaters 61% Reduced ability to concentrate while reading Symptoms new since injury 75% H/O Refractive error 49% Blurred near vision 47% Loses place while reading 71% Flashes 38% Eyes tire while reading 71% Pain in or around eyes 32% Unable to do sustained reading 65% Loss of peripheral vision 22% Falls asleep while reading 64% Pain with eye movement 16% Easier to read when rested 42% Diplopia 11% Covers/closes one eye to read 12% H/O Strabismus/amblyopia 4%

EXAMPLE OF EFFECTS OF DYSFUNCTION Alphabet Pencils Read 1 st letter on left pencil then first on left pencil second on first pencil then second on left pencil, etc.

SPONTANEOUS RECOVERY? Findings from studies of military/veteran and civilian populations following TBI suggests spontaneous recovery may occur in accommodation, strabismus and pursuits/saccades, to a lesser degree in convergence. Self-reported and measured reading difficulties may persist Limitations of these conclusions is that we don’t know the visual status of patients prior to injury and that the comparison study (Capo-Aponte) was 3 a controlled study with small N 5 Study/ 1 2 4 Goodrich Brahm Stelmack Ciuffreda Capo-Aponte Reading* 61% 87% 50% - 65% Convergence 30% 48% 28% 42% 55% Accommodation 22% 49% 47% 41% 65% Strabismus - 7% 8% 25% 0% Pursuits/Saccades 20% 23% 6% 39% 60% Deficit *includes both symptoms and measured deficits 1. Goodrich GL et al. JRRD. 2007; 44: 929 -36. 2. Brahm KD et al. Optom Vis Sci 2009; 86: 817 -25. 3. Stelmack JA et al. Optometry 2009; 80: 419 -24. 4. Ciuffreda KJ et al. Optometry 2007; 78: 155 -61. 5. Capo-Aponte JE et al. Mil Med 2012; 177: 804 -13.

MECHANISM OF INJURY The question of mechanism of injury is an over-arching one for us since blast significantly differs from other mechanisms of injury primarily from the primary blast wave (over-pressure wave) and likelihood of injury due to burns and injury from projectiles/shrapnel (including infection risk)

MECHANISM OF INJURY In civilians: motor vehicle accidents, falls, assaults, struck by/against, other most frequent causes In military personnel: blast event, motor vehicle accident, falls, assaults, gunshot, struck by/against, other There is some evidence that traumatic brain injury due to a blast event differs from other causes. Blast events are also associated with higher rates of eye injury and loss of one or both eyes which is consistent with our findings. Svetlov, S, et al. (2009) J Neurotrauma; Hurley, R. et al (2006), NEJM

VISION LOSS/DYSFUNCTION IN POLYTRAUMA Polytrauma ~ multiple, simultaneously occurring injuries usually involving TBI Populations studied were inpatients of a polytrauma rehabilitation center outpatients with diagnosed mild traumatic brain injury (m. TBI) or Most common injury: blast-related (~50%) Median age ~ 29 years (range 19 to 59) ~95% male

VISION EXAMINATION Comprehensive Eye/Vision Examination (now mandated by VA for all Polytrauma Rehabilitation Center patients) Patient history Visual acuity (ETDRS, Feinbloom Number Chart)* Visual field (Goldman, Arc Perimeter, Tangent Screen, Confrontation)* Binocular/occulomotor Fixation, Reading accommodation, vergence, saccades, etc. ability assessed * Test selection determined by pt. capacity (i. e. , mobile, bed-ridden, etc. )

INPATIENT SYMPTOMS AND FINDINGS 75% self-reported visual symptoms 84% self-reported reading difficulties 59% Light sensitivity Optometric Over-all findings - Dysfunctions 70% presented with one or more findings 46% Convergence 25% Pursuit and/or saccadic 21% Accommodation 11% strabismus 5% fixation or nystagmus

MORE ABOUT “LIGHT SENSITIVITY” Reported by 59% of patients More common in m. TBI Most commonly reported by patients with PTSD Statistical analysis concludes that “light sensitivity” is due to PTSD not visual condition Important in that it suggests that not all visual symptoms generated by vision change Need to ensure we “sort out” visual from non-
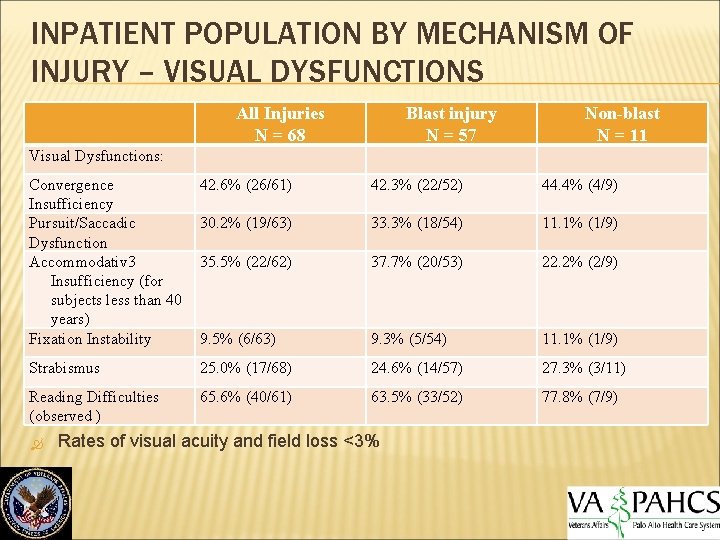
INPATIENT POPULATION BY MECHANISM OF INJURY – VISUAL DYSFUNCTIONS All Injuries N = 68 Blast injury N = 57 Non-blast N = 11 Visual Dysfunctions: Convergence Insufficiency Pursuit/Saccadic Dysfunction Accommodativ 3 Insufficiency (for subjects less than 40 years) Fixation Instability 42. 6% (26/61) 42. 3% (22/52) 44. 4% (4/9) 30. 2% (19/63) 33. 3% (18/54) 11. 1% (1/9) 35. 5% (22/62) 37. 7% (20/53) 22. 2% (2/9) 9. 5% (6/63) 9. 3% (5/54) 11. 1% (1/9) Strabismus 25. 0% (17/68) 24. 6% (14/57) 27. 3% (3/11) Reading Difficulties (observed ) 65. 6% (40/61) 63. 5% (33/52) 77. 8% (7/9) Rates of visual acuity and field loss <3%
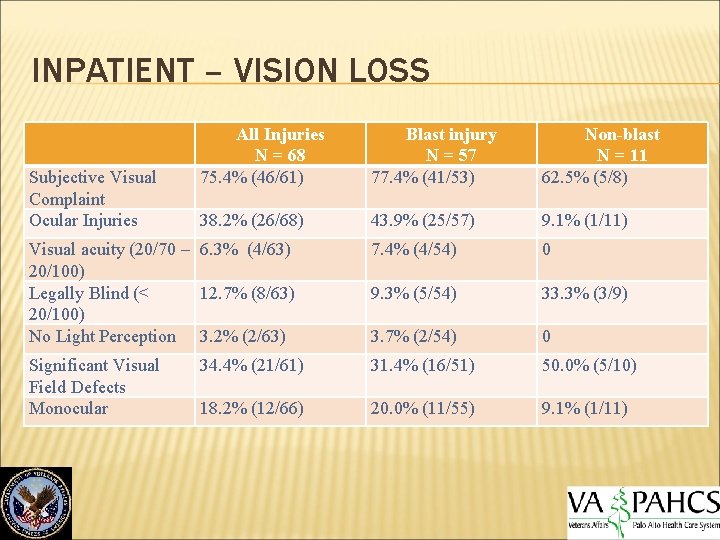
INPATIENT – VISION LOSS All Injuries N = 68 75. 4% (46/61) Blast injury N = 57 77. 4% (41/53) Non-blast N = 11 62. 5% (5/8) 38. 2% (26/68) 43. 9% (25/57) 9. 1% (1/11) Visual acuity (20/70 – 6. 3% (4/63) 20/100) Legally Blind (< 12. 7% (8/63) 20/100) No Light Perception 3. 2% (2/63) 7. 4% (4/54) 0 9. 3% (5/54) 33. 3% (3/9) 3. 7% (2/54) 0 Significant Visual Field Defects Monocular 34. 4% (21/61) 31. 4% (16/51) 50. 0% (5/10) 18. 2% (12/66) 20. 0% (11/55) 9. 1% (1/11) Subjective Visual Complaint Ocular Injuries

VISION & WAR – NUMBERS AND COST FROM AFGHANISTAN & IRAQ Numbers 244, 217 and cost TBIs as of May 16, 2012 http: //www. health. mil/Libraries/TBI-Numbers-Current-Reports/dod-tbi-worldwide-2000 -2012 Q 1 -as-of-120516. pdf 187, 539 mild; 56, 678 moderate, severe, penetrating Causes: blast, MVA, fall, assault, gunshot, etc. Cost from 2000 to 2010 yearly cost = $2. 3 billion for military eye injuries including TBI NAEVR Report, K. Frick, Ph. D Professor, Johns Hopkins Bloomberg School of Public Health, May 2012 54, 291 service members had some degree of visual impairment Total cost to military, VA, & society over remainder of service members lifetime = $24. 3 Billion

REHABILITATION – FIELD LOSS Area contains a good deal of controversy regarding effectiveness of interventions Prisms Vision Restoration Therapy Vision Rehabilitation Therapy Scanning NVT Training Scanning Therapy

PRISMS Prisms relocate image from affected field to intact field Training requirements extensive Fixation spot (minimize eye movement) and presentation of image in intact field Training in office/outdoors (weekly visits up to a period of weeks) Patient “success” – 27% to 81% (Bowers, et al, Arch Ophthal, 2008) Patient “discontinuance” a concern

VISION RESTORATION THERAPY Nova Vision Therapy (NVT) Based on concept of brain plasticity Initial office visit with computer assessment Home training In home computer Two 30 minute sessions per week for 3 to 6 months Weekly “results” uploaded to NVT computer and a new training program download to patient computer based upon prior week’s performance Some literature suggests a small 3 to 5 degree improvement while other reports little improvement

NVT SCANNING THERAPY NVT Systems Computer assessment on scanning bar Computer suggests initial training program Additional training components include paper and pencil tests, indoor/outdoor mobility lessons Assessment of both static (NVT scanning bar) and dynamic training (Mobility Assessment Course) Little formal study of effectiveness

WHAT DOES THE LITERATURE TELL US? Review articles Riggs, et al. Am J Phys Med Rehabil, 2007 Pelak, et al. Curr Treat Options Neurol. 2007 Conclude that scanning training is currently the most promising option for rehabilitation of field losses such as hemianopia Both reviews highlight the need for controlled trials to determine rehabilitation potential

SUMMARY - 1 Casualties for the wars in Afghanistan and Iraq have highlighted vision loss/dysfunction following TBI and the need for: Better access to care, and Additional research to understand the loss/dysfunction and to improve rehabilitation In TBI the mechanism of injury does not change the resulting visual loss/dysfunction

SUMMARY - 2 All forms of brain injury (e. g. trauma, stroke) may involve visual loss or dysfunction Estimates of the number of people affected represent a “best guess” Vision not routinely assessed in most settings dealing with brain injury thus it is likely that current estimates under-report Cost estimates based on incidence suggest that society pays a very heavy price

SUMMARY - 3 Additional research is needed to understand the effects of trauma to the brain on the visual system and how these interactions affect the “whole” individual And, we lack “gold standards” for rehabilitation therapies for the visual deficits caused by brain injury Other than that we’re good

THANK YOU I look forward to learning more at this conference My contact address: Gregory. Goodrich@va. gov

The 11 th International Conference 31 March – 3 on Low Vision April 2014 Advancing research • Upgrading practice • Improving participation www. vision 2014. org
- Slides: 41